06 May 2022: Clinical Research
COVID-19: Another Cause of Dental Anxiety?
Marija Nikolić1ABCDEF*, Aleksandar Mitić1ABE, Jelena Petrović2ABCD, Dragana Dimitrijević2ABCD, Jelena Popović1ABDE, Radomir Barac1ABE, Ana Todorović3ABEDOI: 10.12659/MSM.936535
Med Sci Monit 2022; 28:e936535
Abstract
BACKGROUND: Fear has always been closely linked to dentistry but it could be intensified by the objective risks imposed by the pandemic. The objective of this study was to determine the profile of the frightened dental patient during the COVID-19 pandemic and determine measures taken by dentists to reduce fear and increase security among their patients.
MATERIAL AND METHODS: An anonymous online survey was conducted between March 15 and April 15, 2021. The respondents were 2060 adult citizens of the Republic of Serbia. In addition to demographic data, data related to the COVID-19 pandemic, dental fear, and attitudes and fear of dental interventions during the ongoing pandemic were compiled. The data were analyzed using descriptive statistics: the chi-square test and Pearson’s coefficient.
RESULTS: Seventy percent of the respondents felt some level of fear of the ongoing pandemic, 50% felt fear of going to a dentist during the pandemic, 20% considered a dental office a hotspot for the transmission of SARS-CoV-2, and 43% would visit their dentist only in the case of emergency.
CONCLUSIONS: The COVID-19 pandemic has affected the attitudes and behavior of people pertaining to visits to dental offices. Identifying frightened patients and their opinions and fears at this challenging time would make it easier for dentists to include protocols in their everyday practice to increase a sense of security among their patients, such as implementing preventive measures in front of the patients, ensuring an empty waiting room, and providing telephone consultations.
Keywords: COVID-19, Dental Anxiety, Dentistry, Adult, Dentists, Humans, Pandemics, SARS-CoV-2, Surveys and Questionnaires
Background
Dentistry has always been related to anxiety and pain. Dental fear and anxiety are important characteristics that contribute to the avoidance of dental treatment [1,2]. Dental fear or anxiety affects approximately 36% of the population, of which approximately 12% have extreme fear [3,4].
While anxiety is a state that precedes facing a threatening stimulus, fear is a reaction that occurs when that stimulus is spotted and leads to a fight or flight response. Consequently, anxiety related to the idea of visiting a dentist for preventive care or dental procedures is called dental anxiety, and the reaction to threatening stimuli in the dental environment is called dental fear [5]. In dental practice, it is not necessary to separate these 2 terms, which in the broadest sense represent the fear of anything that has to do with dentistry. Therefore, it is convenient to use the umbrella term: dental fear and anxiety [6]. The overpowering and irrational fear of dentistry is also known as odontophobia, which leads to the complete avoidance of the dentist and is classified as a phobia in the Diagnostic and Statistical Manual of Mental Disorders-IV and the International Statistical Classification of Diseases and Related Health Problems [7].
The etiology of dental anxiety is multicausal and very complex. The etiological factors are mostly either endogenic, such as genetics, personality type, and intelligence or exogenic (or conditioning experience), such as role models, the media, and previous experience [6].
The emergence of the SARS-CoV-2 virus has changed the world, from individual lives to global functioning. Care for one’s own health and life and the lives of loved ones, fear of pandemic consequences, and daily disturbing images coming from around the globe have had an impact on mental health [8]. For a long time, this problem was not the focus of the scientific community, since the preservation of life came first. However, over time, studies emerged which confirm the negative impact of the pandemic on mental health [9,10]. If we could identify the concerns and fears of potential patients at this challenging time, we might be able to better meet their needs [10].
It is believed that a dental office, and dentistry as a high-risk profession, are hotspots for the transmission of contagious diseases [11,12]. It is not possible to completely exclude the risk of getting infected in a dental office [13]. A dental intervention precludes 2 basic recommendations for the prevention of the spread of COVID-19: social distancing and wearing protective masks. Direct contact with a patient is required (60 cm and less), and most interventions include the use of rotating instruments with the production of aerosol, which not only potentially endangers those present, but could contaminate surrounding surfaces [12,14]. The highly contagious nature of SARS-CoV-2 presents a risk for dental office employees and patients, especially because asymptomatic carriers can also transmit the virus [15]. Dentists have always taken care about the prevention of contagious diseases. However, in this new pandemic, the situation may require the implementation of additional preventive measures, especially since the SARS-CoV-2 virus has been around longer than expected [14].
The duration of the pandemic has taught us to live with the virus, and dental care is available again, but the fear has not disappeared. The ever-present dental fear has been assigned a new exogenic etiological factor; namely, fear of contracting the SARS-CoV-2 virus in a dental office, which became a challenge for dentists and their patients.
The aims of this study were to determine the profile of the frightened dental patient during the COVID-19 pandemic and determine the measures which, when implemented by dentists, could decrease fear and increase a sense of security among their patients.
Material and Methods
STUDY DESIGN AND RESPONDENTS:
An online survey was conducted between March 15 and April 15, 2021. It was distributed via online channels and social media. The research included a sample of 2060 adult citizens from the Republic of Serbia (35% male, 65% female). The representative sample was calculated using a 95% confidence level and error margin of 3%. Available statistical data on the population from 2021 indicated that the representative sample size for the defined criteria was a minimum of 1067 respondents (data from the Statistical Office of the Republic of Serbia) [16].
ETHICS:
Participation in the survey was anonymous and voluntary, and the respondents could stop participating at any phase. They were informed about the study and gave their consent prior to the beginning of the survey. The study was conducted in accordance with the Helsinki Declaration and with previous approval from the Ethics Committee of the Faculty of Medicine-University of Niš, Serbia (approval no: 12-2213-2/3). The online study design was chosen owing to its simplicity and lack of social contact, which is recommended during a pandemic.
QUESTIONNAIRE:
The survey questions were designed based on the study objectives, according to the Stehr-Green steps for developing a questionnaire [17]. The expert assessment of the questionnaire was performed by 2 university professors from the relevant field of dentistry who were not involved in the study, and the evaluation of the question construction (eg, avoiding ambiguity and suggestibility) was conducted by 2 experienced experts in questionnaire construction. In accordance with their suggestions, and after a pilot study, a definitive version of the questionnaire was formed using the Google Forms platform. Reliability was determined based on the value of the Cronbach Alpha test, which was 0.801. Twenty closed-ended questions were grouped into 4 sections: section 1, demographic data (2 questions); section 2, COVID-19-related information (6 questions); section 3, fear of dental interventions unrelated to the pandemic (3 questions); and section 4, fear of dental interventions during the pandemic (9 questions).
The degree of determined fear is not a clinical assessment but an individual’s self-assessment that dictates a person’s fear-driven behavior, which is why it was considered more relevant to this study. The respondents rated fear of the dentist, fear of visiting the dentist in a pandemic, and fear of a pandemic using a 5-point Likert scale (0, I do not feel fear; 1, I am slightly scared; 2, I am quite scared; 3, I am very scared; 4, I am extremely scared).
The number of questions in the questionnaire was limited to 20, because owing to the set goals of the study (such as determining the profile of a frightened dental patient during a pandemic), the authors decided that the central data processing method should be a correlation analysis which, when working on a large number of questions, would provide a certain amount of data in the results that would exceed the amount of data that are usually presented in a single scientific paper. The questions are shown in Table 1.
STATISTICAL ANALYSIS:
The Statistical Package for the Social Sciences (SPSS, version 22.0) software was used for descriptive statistical analysis. The chi-square test was used to show statistical significance of the obtained data with the level of statistical significance set at
Results
Seventy percent of the respondents felt some level of fear of the COVID-19 pandemic. Most described the extent of this fear as mild (48%). Almost 60% of the respondents had not contracted COVID-19 up until the beginning of the survey, while others had had symptoms but had not been tested (14%) or had tested positive to the virus and recovered (26%). At the time of the survey, 31.5% of the respondents had been vaccinated. Most evaluated the epidemiological situation as unfavorable (74%) and had reduced their activities to a minimum (60%). Ten percent of the respondents avoided information about the pandemic because it upset them, while 20% tried to keep up with the current global information.
A total of 49.5% of respondents felt some level of dental fear. Most described the extent of that fear as mild (32.5%), then strong (5%) and extreme (2%). Only 8% of the respondents feared that they could contract a disease (other than COVID-19) during a dental intervention, but 27% experienced a distressing sense of powerlessness and lack of control in a dental office.
Approximately 20% of the respondents considered a dental office a hotspot for the transmission of COVID-19, while 43% of them would only go there in an emergency. Most (80%) would not cease ongoing treatment, irrespective of the COVID-19 pandemic.
Most (70%) of the respondents felt safer when the dentist implemented preventive measures in their presence and 50% felt safer when there were no other patients in the waiting room. The possibility of telephone consultations during a pandemic was considered desirable by 76% of the respondents. Approximately 14% stated that a waiting room with chairs evenly spaced apart, containing disinfectant, and without the presence of other people or magazines seemed distressing. Irrespective of the beginning of mass vaccination and the fact that many people recovered from the virus, 26.5% of the respondents still did not feel safe in a dental office.
Statistical analyses showed that the responses which reflected fear of dental interventions during the pandemic (section 4 of the survey) differed based on demographic data (section 1), COVID-related information (section 2), and data regarding fear of dental interventions unrelated to COVID-19 (section 3).
The statistical analysis showed a statistically significant positive correlation between fear of COVID-19 and fear of going to a dental office during the COVID-19 pandemic (correlation coefficient=0.460
Discussion
STUDY LIMITATIONS:
An online study is recommended during a pandemic owing to the lack of social contact and simplicity. However, the required access to the internet is a possible reason why there were few elderly respondents (65+ years) in the studied population. The cross-sectional design of the study had its limitations since it was not possible to determine a cause-and-effect relationship. Although the size of the sample was representative, this was still a convenience sample with potential bias.
Collecting data such as whether someone had been vaccinated, had had the disease, kept activities to a minimum, and assessed the epidemiological situation were not in themselves the goal of the research because these data change from day to day and they can reflect the situation at only a given moment. These data were collected because they reflected the fear and discomfort of patients caused by the pandemic and were current regardless of the moment in time. The aim of the research was not to determine the proportion of people who were vaccinated or contracted the disease, but to determine the attitudes and behaviors of people who belong to these groups when it came to visiting the dentist in a pandemic.
To the best of our knowledge, this is the first study that deals with the fear of dentists during the pandemic in Serbia and that gives practical recommendations to dental professionals on how to behave to positively influence the fear of their patients. The length of the pandemic, with all the changes it has brought, such as the number of infected people, the availability of vaccines, and new strains of the virus, but also the habituation of people to the situation, imposes the need for further research.
Conclusions
One of the basic objectives of treating dental anxiety is to diminish or remove the cause of fear among patients so that they could be motivated for long-term repeat visits [5]. The pandemic as an exogenic factor cannot be removed, and therefore it is important to know the profile of the frightened dental patient during the pandemic, as well as what increases fear and what increases a sense of security. Our results showed that the individual most afraid of a dental intervention during the COVID-19 pandemic is an elderly adult who has not had the disease, is vaccinated, has reduced activities to a minimum, and is regularly informed about the current situation around the world. Implementing preventive measures in front of the patient, ensuring an empty waiting room, and enabling telephone consultations increase a sense of security. Knowing this, it is easier for dentists to identify a frightened patient and to implement certain protocols in their daily practice because they can view the dental intervention during the COVID-19 pandemic through the eyes of a frightened patient. In this way, dentists would give their patients’ fear as much importance as they do the success of the intervention.
Tables
Table 1. The questions included in the questionnaire. Table 2. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q12, Q14, Q15) and sections 1 and 2 (Q1, Q4, Q5, Q6, Q7, Q8).
Table 2. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q12, Q14, Q15) and sections 1 and 2 (Q1, Q4, Q5, Q6, Q7, Q8).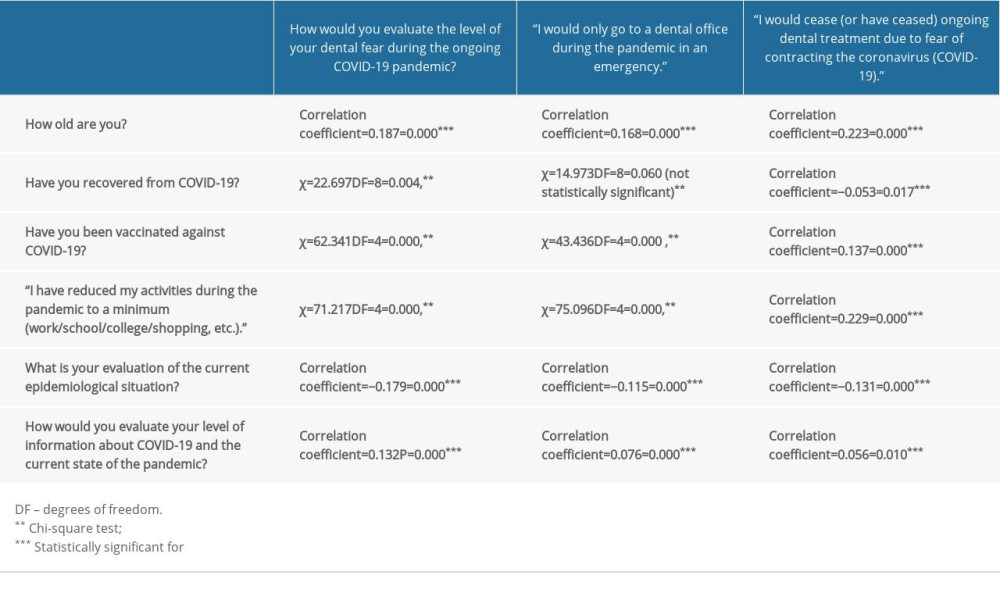 Table 3. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q16) and sections 1 and 2 (Q1, Q4, Q5, Q7, Q8).
Table 3. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q16) and sections 1 and 2 (Q1, Q4, Q5, Q7, Q8).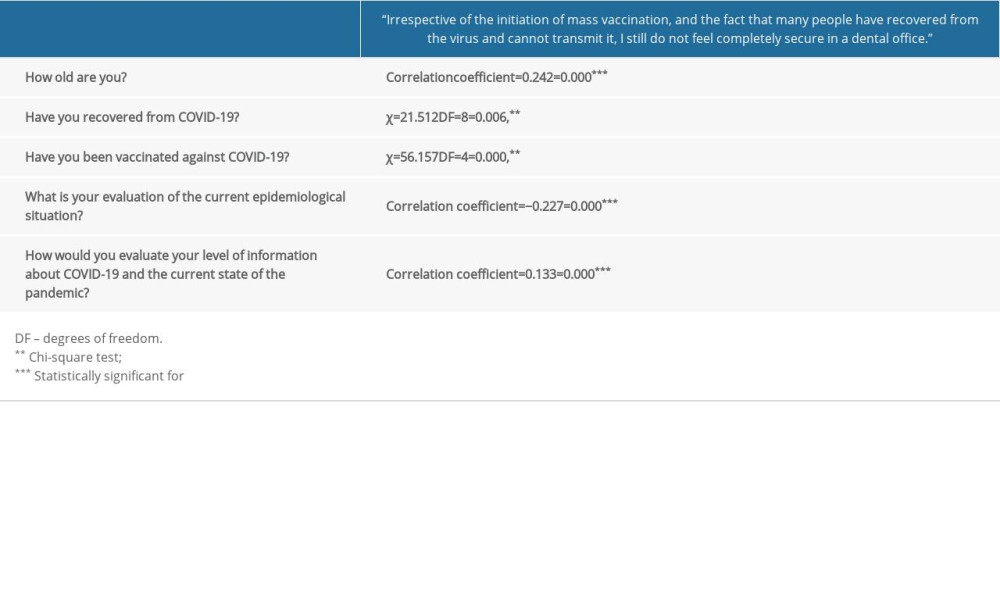 Table 4. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q13) and sections 2 and 3 (Q8, Q10, Q11).
Table 4. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q13) and sections 2 and 3 (Q8, Q10, Q11).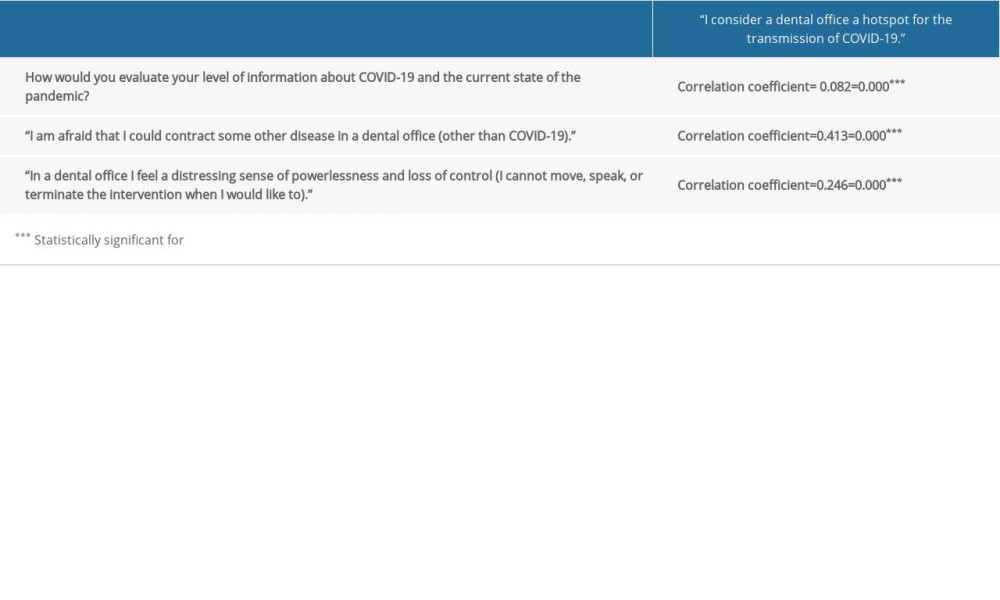 Table 5. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q18) and sections 1, 2 and 4 (Q1, Q4, Q5, Q6, Q12, Q14).
Table 5. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q18) and sections 1, 2 and 4 (Q1, Q4, Q5, Q6, Q12, Q14). Table 6. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q17) and sections 2 and 3 (Q8, Q10, Q11).
Table 6. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q17) and sections 2 and 3 (Q8, Q10, Q11).
References
1. Pohjola V, Lahti S, Vehkalahti MM, Tolvanen MHH, Association between dental fear and dental attendance among adults in Finland: Acta Odontol Scand, 2007; 65(4); 224-30
2. Gatchell R, Ingersoll B, Bowman L, Robertson MWC, The prevalence of dental fear and avoidance: A recent survey study: J Am Dent Assoc, 1983; 107(4); 609-10
3. Hill KB, Chadwick B, Freeman R, Adult Dental Health Survey 2009: Relationships between dental attendance patterns, oral health behaviour and the current barriers to dental care: Br Dent J, 2013; 214(1); 25-32
4. Humphris GM, Dyer TA, Robinson PG, The modified dental anxiety scale: UK general public population norms in 2008 with further psychometrics and effects of age: BMC Oral Health, 2009; 9; 20
5. Appukuttan DP, Strategies to manage patients with dental anxiety and dental phobia: Literature review: Clin Cosmet Investig Dent, 2016; 8; 35-50
6. Beaton L, Freeman R, Humphris G, Why are people afraid of the dentist? Observations and explanations: Med Princ Pract, 2014; 23; 295-301
7. van Wijk AHJ, The Fear of Dental Pain questionnaire: Construction and validity: Eur J Oral Sci, 2003; 111(1); 12-18
8. Ornell F, Schuch JB, Sordi AO, Kessler FHP, ‘“Pandemic fear”’ and COVID-19: Mental health burden and strategies: Braz J Psychiatry, 2020; 42; 232-35
9. Bäuerle A, Teufel M, Musche V, Increased generalized anxiety, depression and distress during the COVID-19 pandemic: A cross-sectional study in Germany: J Public Heal (United Kingdom), 2020; 42(4); 672-78
10. Knipe D, Evans H, Marchant A, Mapping population mental health concerns related to COVID-19 and the consequences of physical distancing: A Google trends analysis: Wellcome Open Res, 2020; 5; 82
11. Gurzawska-Comis K, Becker K, Brunello G, Recommendations for dental care during COVID-19 pandemic: J Clin Med, 2020; 9(6); 1833
12. Kanathila H, Pangi A, Bharathi B, COVID-19 – threat to dentistry – how to overcome?: J Evol Med Dent Sci Sep 14, 2020; 9(37); 2746-50
13. Volgenant CMC, de Soet JJ, Cross-transmission in the Dental Office: Does This Make You Ill?: Curr Oral Heal Rep, 2018; 5(4); 221-28
14. Volgenant CMC, Persoon IF, de Ruijter RAG, de Soet JJ, Infection control in dental health care during and after the SARS-CoV-2 outbreak: Oral Dis, 2021; 27(3); 674-83
15. Ahmadi H, Ebrahimi A, Ghorbani F, The impact of COVID-19 pandemic on dental practice in Iran: a questionnaire-based report: BMC Oral Health, 2020; 20; 354
16. : Republički zavod za statistiku Srbije [Internet] Available from: [in Croatian]https://www.stat.gov.rs/sr-Latn/oblasti/stanovnistvo
17. Nardi MP, Developing a questionnaire: Doing Surv Res, 2020; 2(2); 80-121
18. Cotrin P, Peloso RM, Oliveira RC, Impact of coronavirus pandemic in appointments and anxiety/concerns of patients regarding orthodontic treatment: Orthod Craniofacial Res, 2020; 23(4); 455-61
19. Tunis TS, Ratson T, Matalon S, The impact of the COVID-19 pandemic on Israeli orthodontic practice: A clinic’s activity and patients’ attitudes: Int J Environ Res Public Health, 2022; 19(4); 1965
20. Alassiry AM, Hakami Z, The attitude, perception, and mental health of patients receiving orthodontic treatment during the COVID-19 pandemic in Saudi Arabia: Patient Prefer Adherence, 2022; 16(February); 363-72
21. Campagnaro R, Collet G, de O, de Andrade MP, COVID-19 pandemic and pediatric dentistry: Fear, eating habits and parent–s oral health perceptions: Child Youth Serv Rev, 2020; 118; 105469
22. Migas K, Marczak M, Kozłowski R, Impact of the COVID-19 pandemic on the dental preferences of patients in the private sector: Int J Environ Res Public Health, 2022; 19(4); 2183
23. Ciardo A, Simon MM, Sonnenschein SK, Impact of the COVID-19 pandemic on oral health and psychosocial factors: Sci Rep [Internet], 2022; 12(1); 1-12
24. Oshima K, Miura H, Tano R, Fukuda H, Factors associated with regular dental checkups ’ discontinuation during the COVID-19 pandemic: A nationwide cross-sectional web-based survey in Japan: Int J Environ Res Public Health, 2022; 19(5); 2917
25. Jum’ah AA, Elsalem L, Loch C, Perception of health and educational risks amongst dental students and educators in the era of COVID-19: Eur J Dent Educ, 2021; 25; 506-15
26. Jordan RE, Adab P, Cheng KK, COVID-19: Risk factors for severe disease and death: BMJ, 2020; 368; m1198
27. Cagetti MG, Cairoli JL, Senna A, Campus G, COVID-19 outbreak in North Italy: An overview on dentistry. A questionnaire survey: Int J Environ Res Public Health, 2020; 17(11); 3835
28. Lin CY, Broström A, Griffiths MD, Pakpour AH, Investigating mediated effects of fear of COVID-19 and COVID-19 misunderstanding in the association between problematic social media use, psychological distress, and insomnia: Internet Interv, 2020; 21; 100345
29. Patel M, Infection control in dentistry during COVID-19 pandemic: What has changed?: Heliyon, 2020; 10(6); E05402
30. Gambarini E, Galli M, di Nardo D, A survey on perceived COVID-19 risk in dentistry and the possible use of rapid tests: J Contemp Dent Pract, 2020; 21(7); 718-22
31. Giraudeau N, Bauer M, Tramini P, A national teledentistry study on the knowledge, attitudes, training and practices of private dentists: Digit Heal, 2022; 8 205520762210850
Tables
 Table 1. The questions included in the questionnaire.
Table 1. The questions included in the questionnaire. Table 2. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q12, Q14, Q15) and sections 1 and 2 (Q1, Q4, Q5, Q6, Q7, Q8).
Table 2. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q12, Q14, Q15) and sections 1 and 2 (Q1, Q4, Q5, Q6, Q7, Q8). Table 3. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q16) and sections 1 and 2 (Q1, Q4, Q5, Q7, Q8).
Table 3. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q16) and sections 1 and 2 (Q1, Q4, Q5, Q7, Q8). Table 4. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q13) and sections 2 and 3 (Q8, Q10, Q11).
Table 4. Correlation analysis. The correlation coefficients for the responses to the questions from section 4 (Q13) and sections 2 and 3 (Q8, Q10, Q11). Table 5. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q18) and sections 1, 2 and 4 (Q1, Q4, Q5, Q6, Q12, Q14).
Table 5. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q18) and sections 1, 2 and 4 (Q1, Q4, Q5, Q6, Q12, Q14). Table 6. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q17) and sections 2 and 3 (Q8, Q10, Q11).
Table 6. Correlation analysis. Correlation coefficients for the responses to the questions from section 4 (Q17) and sections 2 and 3 (Q8, Q10, Q11). In Press
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
11 Mar 2024 : Clinical Research
Comparison of Effects of Sugammadex and Neostigmine on Postoperative Neuromuscular Blockade Recovery in Pat...Med Sci Monit In Press; DOI: 10.12659/MSM.942773
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








