21 July 2021: Clinical Research
Comparison of Intra-Abdominal Pressure Measurements in Critically Ill Patients Using Intravesical Normal Saline at 15°C, 25°C, and 35°C
Jianfeng Zou1ABD*, Lili Zheng2EG, Weizheng Shuai1DE, Qi Li1CD, Qian Wang1BE, Zhicheng Zhang1DE, Dawei Li1BDDOI: 10.12659/MSM.932804
Med Sci Monit 2021; 27:e932804
Abstract
BACKGROUND: The incidence of intra-abdominal hypertension (IAH) and abdominal compartment syndrome (ACS) in intensive care units is high. Dynamic monitoring of intra-abdominal pressure (IAP) is important to treat patients with these conditions. The World Society of Abdominal Compartment Syndrome revised IAP measurement and treatment guidelines in 2013. IAP is measured by instilling ≤25 mL of sterile saline into the bladder, but there is no requirement for the saline to be at a specific temperature. Many doctors presume that using cold saline will trigger bladder muscle spasms, resulting in measurement error. In the present study, we investigated the effect of body-temperature saline on IAP measurements.
MATERIAL AND METHODS: A single-center study was conducted in 12 patients with IAH over a 2-year period. IAP was measured via the bladder with instillation of sterile saline at temperatures of 35°C, 25°C, and 15°C. We analyzed the data using R software, version 4.1.0. Paired t tests were used for comparisons between groups. A Spearman rank correlation analysis was performed to compare groups. Analysis results were plotted using the R packages ggplot2, ggpubr, and BlandAltmanLeh. P<0.05 was considered statistically significant.
RESULTS: There was a significant difference in IAP measurement between the 15°C and 35°C groups (t=-2.55, P=0.027). There was no significant difference between the 25°C and 35°C groups (t=0.73, P=0.48). Bland-Altman analysis showed that IAP was consistent in the 25°C and 35°C groups.
CONCLUSIONS: Although it is preferable to measure IAP with saline at body temperature (35°C), a temperature >25°C is associated with accurate results. Using saline at <15°C should be avoided.
Keywords: Compartment Syndromes, intra-abdominal hypertension, Muscular Diseases, Body Temperature, Critical Care, Critical Illness, saline solution, Temperature
Background
Intra-abdominal pressure (IAP) is approximately 5 to 7 mmHg in critically ill adults. A persistent increase in IAP in critically ill patients in the Intensive Care Unit (ICU) – resulting from acute respiratory failure, gastrointestinal dysfunction, abdominal and pelvic hemorrhage, effusion, intensive fluid resuscitation, and/or septic shock – can lead to intra-abdominal hypertension (IAH) or abdominal compartment syndrome (ACS) [1]. IAH is defined as a sustained or repeated pathological increase in IAP to ≥12 mmHg. ACS is defined as a sustained IAP >20 mmHg (with or without an abdominal perfusion pressure <60 mmHg) that is associated with new organ dysfunction/failure. IAH severity is defined as follows: grade I, 12 to 15 mmHg; grade II, 16 to 20 mmHg; grade III, 21 to 25 mmHg; and grade IV, >25 mmHg [2].
Attention increasingly is being paid to the incidence of IAH [3]. It reportedly occurs in 30% to 50% of critically ill patients and 8% to 15% subsequently develop ACS [4,5]. IAH can cause dysfunction in pulmonary, cardiovascular, renal, and gastrointestinal systems, which leads to a vicious cycle. If not effectively treated in a timely manner, IAH can cause multiple-organ dysfunction or death; diagnosing it is heavily dependent upon dynamic measurement of IAP. Early treatment can prevent deterioration, improve patient outcomes, and reduce mortality.
IAP monitoring has received increasing attention in patients who are at high risk and critically ill [5]. The World Society of the Abdominal Compartment Syndrome (WSACS) is dedicated to research about ACS. The organization revised its guidelines for ACS measurement and treatment in 2013, based on published clinical studies [6]. The current guidelines recommend placing the patient in the supine position, inserting a urethral catheter and emptying the bladder, connecting the catheter to the piezometer, injecting ≤25 mL of sterile saline into the urethral catheter, and setting the 0 point at the midaxillary line. IAP is the pressure measured at the end of expiration. The standard unit of measure is mmHg. However, there is no specific requirement for saline temperature. A common current practice is to measure bladder pressure using ≤25 mL of saline. In this context, we presumed that sufficient accuracy could be achieved using room-temperature saline. Measurement of IAP is fundamental to the diagnosis and treatment of IAH and ACS; therefore, we evaluated the effects of saline temperature on IAP measurement.
Material and Methods
PATIENT POPULATION:
The present study was conducted in the Critical Care Medicine Department of the Sixth Medical Center, a tertiary hospital in Beijing, China. Our ICU has 14 beds and approximately 300 hospitalizations per year. Patients treated in the ICU in the past 2 years who were at high risk of IAH because of factors such as major abdominal surgery, severe trauma, and acute severe pancreatitis were included in the study. Patients were excluded if they had bladder lesions, contracture, trauma, neurogenic bladder, and other bladder-related issues. All patients enrolled in the study provided written informed consent. The protocol was approved by our institution’s Ethics Committee before the start of the study (approval number: HZKY-PJ-2021-16).
STUDY DESIGN:
Sterile normal saline was prepared and kept at constant temperatures of 35°C, 25°C, and 15°C using a heating bath (Model DK-8D, Qianjun, Shanghai, China). IAP was measured using the intravesical pressure method, as described by the WSACS [6]. First, the patient’s bladder was emptied. IAP measurements were recorded after installation of 25 mL of sterile saline into the bladder and with the patient in the supine position at end expiration and the transducer zeroed at the level of the midaxillary line. First, 35°C was used, then 25°C, and finally 15°C. It took about 10 s to infuse 25 mL of saline into the bladder and close the catheter. The IAP was read 10 s after the instillation. After each measurement, the patient’s bladder was emptied again [7]. Two colleagues read the IAP measurements independently and their readings were averaged and recorded as the final value. Before the study, these clinicians were well trained by the author in how to measure IAP.
STATISTICAL ANALYSIS:
All analyses were conducted with R software, version 4.1.0 (R Foundation for Statistical Computing, Vienna, Austria). Paired
Results
CLINICAL CHARACTERISTICS AND IAP MEASUREMENTS:
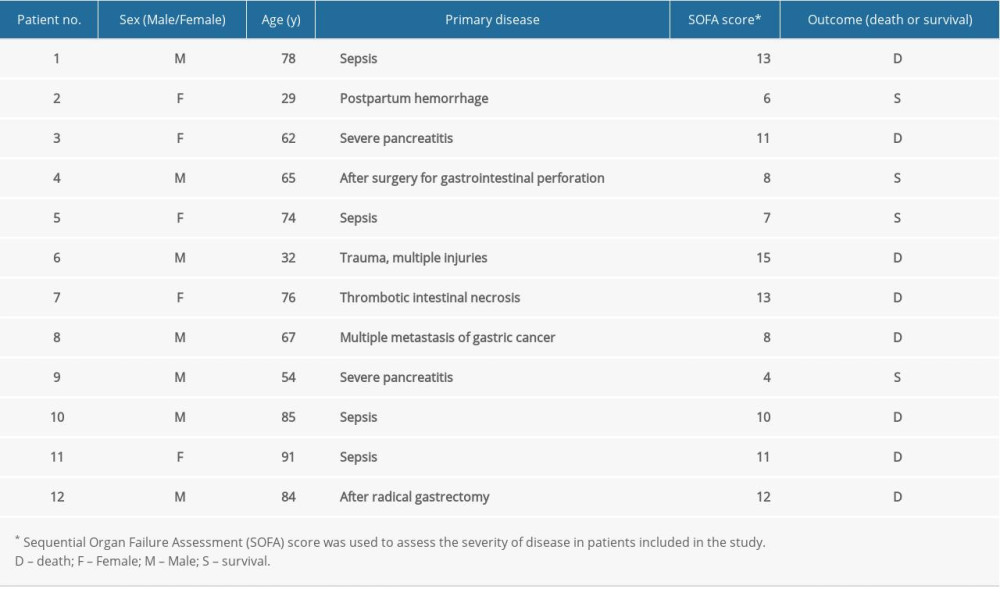
Twelve patients at high risk of IAH (8 men and 4 women; median age 66.4±18.9 years) who were admitted to our department from June 2017 to September 2019 were included in the present study. Their baseline clinical characteristics are shown in Table 1. Of the patients, 2 had severe pancreatitis, 4 had septic shock, 2 had postoperative abdominal infections, 1 had a metastatic tumor in the gastrointestinal tract, 1 had thrombotic intestinal necrosis, 1 had obstetric pathology, and 1 had trauma and multiple injuries with gastrointestinal perforation.
ANALYSIS OF IAP USING SALINE AT DIFFERENT TEMPERATURES:
The results of the Spearman correlation analysis for IAP measurement with saline infusion between 15°C and 35°C were P<2.2e-16 and rho=0.958042. For the measurements made with the 25°C and 35°C infusions, the results were P<2.2e-16 and rho=0.986014. Both analyses showed a positive correlation between the saline temperatures and the IAP measurements (Figure 1A, 1B).
Figure 2A shows IAP measurements using saline at 35°C, 25°C, and 15°C. There was a significant difference between measurements using the 15°C and 35°C infusions (t=−2.55, P=0.027). Figure 2B shows that there was no significant difference between the 25°C and 35°C infusions (t=0.73, P=0.48).
Bland-Altman analysis showed a considerable difference between the groups with the 15°C and 35°C infusions (mean difference±SD, 0.625±1.661; Figure 3A). In contrast, there was a minimal difference between the 25°C and 35°C groups (mean difference±SD, 0.067±0.622; Figure 3B). These findings indicate that IAP measurements using saline at 25°C and 35°C are consistent, which suggests that either temperature is acceptable for clinical IAP measurement. However, the results differed when using saline at 15°C, which suggests that lower temperatures should be avoided.
Discussion
LIMITATIONS:
In the present study, modifying saline temperature by 10
Conclusions
Timely trans-bladder measurement of IAP is important for critically ill patients. Our study revealed that room-temperature saline (>25°C) can be used directly to measure IAP, without heating it to body temperature. Use of saline at temperatures <15°C should be avoid and it should be heated to 25°C to 35°C before infusion into the bladder.
Figures
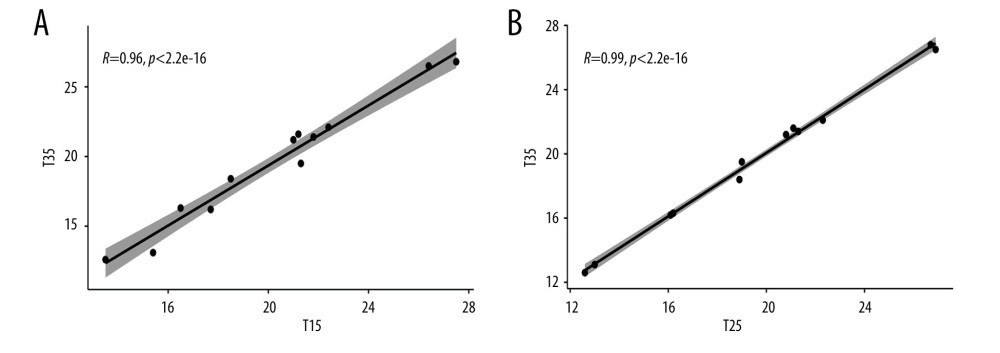 Figure 1. (A) Scatter plot of Spearman correlation between the 15°C and 35°C groups. P<2.2e-16, rho=0.958042. (B) Scatter plot for Spearman correlation between the 25°C (T25) and 35°C (T35) groups. P<2.2e-16, rho=0.986014. R – rho.
Figure 1. (A) Scatter plot of Spearman correlation between the 15°C and 35°C groups. P<2.2e-16, rho=0.958042. (B) Scatter plot for Spearman correlation between the 25°C (T25) and 35°C (T35) groups. P<2.2e-16, rho=0.986014. R – rho. 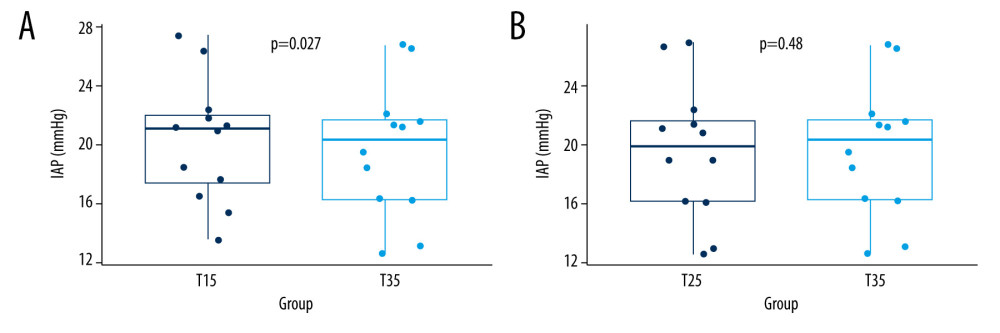 Figure 2. (A) Comparison of IAP measurements using saline at 15°C (T15) and 35°C (T35). A paired t test analysis showed a significant difference (t=−2.55, P=0.027). IAP – intra-abdominal pressure. (B) Comparison of IAP measurements using saline at 25°C (T25) and 35°C (T35). A paired t test analysis showed no significant difference (t=0.73, P=0.48). IAP – intra-abdominal pressure.
Figure 2. (A) Comparison of IAP measurements using saline at 15°C (T15) and 35°C (T35). A paired t test analysis showed a significant difference (t=−2.55, P=0.027). IAP – intra-abdominal pressure. (B) Comparison of IAP measurements using saline at 25°C (T25) and 35°C (T35). A paired t test analysis showed no significant difference (t=0.73, P=0.48). IAP – intra-abdominal pressure. 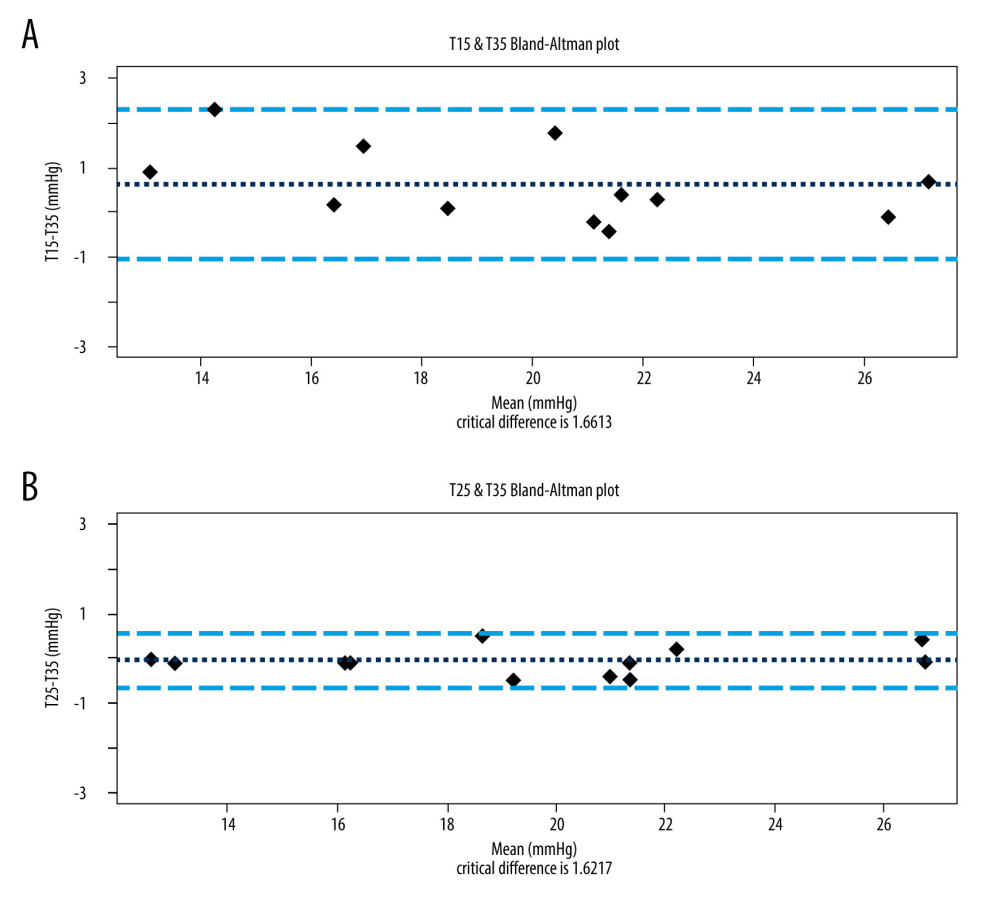 Figure 3. (A) Bland-Altman plot of IAP measurements using saline at 15°C (T15) and 35°C (T35). The upper line indicates 2.286, the mean of the middle line indicates 0.625, lower line indicates −1.036, and the mean difference±SD is 0.625±1.661. IAP – intra-abdominal pressure. (B) Bland-Altman plot of IAP measurements using saline at 25°C (T25) and 35°C (T35). The upper line indicates 0.555, the mean of the middle line indicates 0.067, the lower line indicates −0.688, and the mean difference±SD is 0.067±0.622. IAP – intra-abdominal pressure.
Figure 3. (A) Bland-Altman plot of IAP measurements using saline at 15°C (T15) and 35°C (T35). The upper line indicates 2.286, the mean of the middle line indicates 0.625, lower line indicates −1.036, and the mean difference±SD is 0.625±1.661. IAP – intra-abdominal pressure. (B) Bland-Altman plot of IAP measurements using saline at 25°C (T25) and 35°C (T35). The upper line indicates 0.555, the mean of the middle line indicates 0.067, the lower line indicates −0.688, and the mean difference±SD is 0.067±0.622. IAP – intra-abdominal pressure. References
1. Malbrain ML, Cheatham ML, Kirkpatrick A, Results from the International Conference of Experts on Intra-abdominal Hypertension and Abdominal Compartment Syndrome. I. Definitions: Intensive Care Med, 2006; 32(11); 1722-32
2. Sanchez NC, Tenofsky PL, Dort JM, What is normal intra-abdominal pressure?: Am Surg, 2001; 67(3); 243-48
3. Malbrain ML, Cheatham ML, Kirkpatrick A, Abdominal compartment syndrome: It’s time to pay attention!: Intensive Care Med, 2006; 32(11); 1912-14
4. Malbrain ML, Chiumello D, Pelosi P, Prevalence of intra-abdominal hypertension in critically ill patients: A multicentre epidemiological study: Intensive Care Med, 2004; 30(5); 822-29
5. Murphy PB, Parry NG, Sela N, Intra-abdominal hypertension is more common than previously thought: A prospective study in a mixed medical-surgical ICU: Crit Care Med, 2018; 46(6); 958-64
6. Kirkpatrick AW, Roberts DJ, De Waele J, Intra-abdominal hypertension and the abdominal compartment syndrome: Updated consensus definitions and clinical practice guidelines from the World Society of the Abdominal Compartment Syndrome: Intensive Care Med, 2013; 39(7); 1190-206
7. Chiumello D, Tallarini F, Chierichetti M, The effect of different volumes and temperatures of saline on the bladder pressure measurement in critically ill patients: Crit Care, 2007; 11(4); R82
8. Pereira BM, Abdominal compartment syndrome and intra-abdominal hypertension: Curr Opin Crit Care, 2019; 25(6); 688-96
9. Kirkpatrick AW, Sugrue M, McKee JL, Update from the Abdominal Compartment Society (WSACS) on intra-abdominal hypertension and abdominal compartment syndrome: Past, present, and future beyond Banff 2017: Anaesthesiol Intensive Ther, 2017; 49(2); 83-87
10. Sadeghi M, Kiani A, Sheikhy K, Abdominal compartment syndrome in critically ill patients: Open Access Maced J Med Sci, 2019; 7(7); 1097-102
11. Patel DM, Connor MJ, Intra-abdominal hypertension and abdominal compartment syndrome: An underappreciated cause of acute kidney injury: Adv Chronic Kidney Dis, 2016; 23(3); 160-66
12. Reintam Blaser A, Malbrain M, Regli A, Abdominal pressure and gastrointestinal function: An inseparable couple?: Anaesthesiol Intensive Ther, 2017; 49(2); 146-58
13. Kron IL, Harman PK, Nolan SP, The measurement of intra-abdominal pressure as a criterion for abdominal re-exploration: Ann Surg, 1984; 199(1); 28-30
14. Reintam Blaser A, Regli A, De Keulenaer B, Incidence, risk factors, and outcomes of intra-abdominal hypertension in critically ill patients – a prospective multicenter study (IROI Study): Crit Care Med, 2019; 47(4); 535-42
15. Maddison L, Starkopf J, Reintam Blaser A, Mild to moderate intra-abdominal hypertension: Does it matter?: World J Crit Care Med, 2016; 5(1); 96-102
16. Padar M, Reintam Blaser A, Talving P, abdominal compartment syndrome: Improving outcomes with a multidisciplinary approach – a narrative review: J Multidiscip Healthc, 2019; 12; 1061-74
17. Brooks AJ, Simpson A, Delbridge M, Validation of direct intraabdominal pressure measurement using a continuous indwelling compartment pressure monitor: J Trauma, 2005; 58(4); 830-32
18. Pereira B, Dorigatti A, Melek M, Septic shock patients admitted to the intensive care unit with higher SOFA score tend to have higher incidence of abdominal compartment syndrome – a preliminary analysis: Anaesthesiol Intensive Ther, 2019; 51(5); 370-72
19. Lee AHH, Lee WS, Anderson D, Severe pancreatitis complicated by abdominal compartment syndrome managed with decompressive laparotomy: A case report: BMC Surg, 2019; 19(1); 113
20. Bland JM, Altman DG, Statistical methods for assessing agreement between two methods of clinical measurement: Lancet, 1986; 1(8476); 307-10
21. Rajasurya V, Surani S, Abdominal compartment syndrome: Often overlooked conditions in medical intensive care units: World J Gastroenterol, 2020; 26(3); 266-78
Figures
 Figure 1. (A) Scatter plot of Spearman correlation between the 15°C and 35°C groups. P<2.2e-16, rho=0.958042. (B) Scatter plot for Spearman correlation between the 25°C (T25) and 35°C (T35) groups. P<2.2e-16, rho=0.986014. R – rho.
Figure 1. (A) Scatter plot of Spearman correlation between the 15°C and 35°C groups. P<2.2e-16, rho=0.958042. (B) Scatter plot for Spearman correlation between the 25°C (T25) and 35°C (T35) groups. P<2.2e-16, rho=0.986014. R – rho. Figure 2. (A) Comparison of IAP measurements using saline at 15°C (T15) and 35°C (T35). A paired t test analysis showed a significant difference (t=−2.55, P=0.027). IAP – intra-abdominal pressure. (B) Comparison of IAP measurements using saline at 25°C (T25) and 35°C (T35). A paired t test analysis showed no significant difference (t=0.73, P=0.48). IAP – intra-abdominal pressure.
Figure 2. (A) Comparison of IAP measurements using saline at 15°C (T15) and 35°C (T35). A paired t test analysis showed a significant difference (t=−2.55, P=0.027). IAP – intra-abdominal pressure. (B) Comparison of IAP measurements using saline at 25°C (T25) and 35°C (T35). A paired t test analysis showed no significant difference (t=0.73, P=0.48). IAP – intra-abdominal pressure. Figure 3. (A) Bland-Altman plot of IAP measurements using saline at 15°C (T15) and 35°C (T35). The upper line indicates 2.286, the mean of the middle line indicates 0.625, lower line indicates −1.036, and the mean difference±SD is 0.625±1.661. IAP – intra-abdominal pressure. (B) Bland-Altman plot of IAP measurements using saline at 25°C (T25) and 35°C (T35). The upper line indicates 0.555, the mean of the middle line indicates 0.067, the lower line indicates −0.688, and the mean difference±SD is 0.067±0.622. IAP – intra-abdominal pressure.
Figure 3. (A) Bland-Altman plot of IAP measurements using saline at 15°C (T15) and 35°C (T35). The upper line indicates 2.286, the mean of the middle line indicates 0.625, lower line indicates −1.036, and the mean difference±SD is 0.625±1.661. IAP – intra-abdominal pressure. (B) Bland-Altman plot of IAP measurements using saline at 25°C (T25) and 35°C (T35). The upper line indicates 0.555, the mean of the middle line indicates 0.067, the lower line indicates −0.688, and the mean difference±SD is 0.067±0.622. IAP – intra-abdominal pressure. In Press
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952