25 July 2021: Animal Study
Effects of Repetitive Transcranial Magnetic Stimulation (rTMS) and Treadmill Training on Recovery of Motor Function in a Rat Model of Partial Spinal Cord Injury
Pei Wang12CDE, Ruian Yin1B, Shuangyan Wang1BC, Ting Zhou3B, Yongjie Zhang4D, Ming Xiao5D, Hongxing Wang23AFG*, Guangxu Xu1AFGDOI: 10.12659/MSM.931601
Med Sci Monit 2021; 27:e931601
Abstract
BACKGROUND: This study aimed to investigate the effects of repetitive transcranial magnetic stimulation (rTMS) and treadmill training (TT) on motor function recovery in rats with partial spinal cord injury (SCI).
MATERIAL AND METHODS: Sixty rats with moderate partial SCI at the 9th thoracic vertebral level induced by a Louisville Injury System Apparatus impactor were randomly allocated to 5 groups: Sham surgery (Intact); Sham rTMS without TT (S-rTMS/Non-TT); Sham rTMS with TT (S-rTMS/TT); rTMS without TT (rTMS/Non-TT); and rTMS with TT (rTMS/TT). Interventions commenced 8 days after SCI and continued for 8 weeks. Outcomes studied were Basso, Beattie, and Bresnahan locomotor scale scores, grid walking test, and biochemical analysis of the brain-derived neurotrophic factor (BDNF), synapsin I (SYN), and postsynaptic density protein-95 (PSD-95) in the motor cortex and spinal cord.
RESULTS: The rTMS/TT contributed to greater Basso, Beattie, and Bresnahan scores compared with the S-rTMS/Non-TT (P<0.01), S-rTMS/TT (P<0.05), and rTMS/Non-TT (P<0.05), and showed obviously reduced numbers of foot drops compared with the S-rTMS/Non-TT (P<0.05). The rTMS/TT significantly increased the expressions of BDNF, SYN, and PSD-95 compared with the S-rTMS/Non-TT, both in the motor cortex (P<0.01, P<0.01, P<0.001, respectively) and spinal cord (P<0.001, P<0.01, P<0.05, respectively).
CONCLUSIONS: In a modified rat model of SCI, combined rTMS with TT improved motor function, indicating that this combined approach promoted adaptive neuroplasticity between the motor cortex and the spinal cord. A combined app roach to improving motor function following SCI requires further evaluation to determine the possible clinical applications.
Keywords: Neuronal Plasticity, Spinal Cord Injuries, Transcranial Magnetic Stimulation, Motor Activity, Physical Conditioning, Animal, Recovery of Function
Background
Spinal cord injury (SCI) is a neurological disorder caused by interruption of ascending and descending pathways that carry information between the brain and the spinal cord, leading to severe and permanent motor and sensory dysfunction [1–3]. After SCI, plastic changes occur in some neural circuits, not only in the spinal cord but also in cortical structures [3]. Unselective and maladaptive plasticity of the motor and sensory projection may induce further limitation of movement [4]. Promotion of motor function recovery is urgent and challenging for SCI patients [5]. Approaches based on drug administration or cell transplants are aimed at restoring sensorimotor function after SCI [6]. However, clinical conversions often fail due to adverse effects or lack of efficacy [6]. In contrast, noninvasive neurophysical therapy has shown the potential to improve motor function in patients with incomplete SCI [7]. A clinical practice guideline for SCI has suggested that rehabilitation can maximize neural function recovery [8].
Exercise training aimed at promoting motor function has been studied extensively with SCI patients and animal models [9]. The biological effects of exercise training mainly include preventing dendritic atrophy of motor neurons [10], inducing collateral sprouting of axons [11], reducing myelin loss [12], and promoting the expressions of neurotrophic factors [13]. Some studies reported that exercise training is beneficial to improve motor function after SCI [14–16]. However, the effectiveness of exercise training alone on the recovery of motor function is often limited [17–19] and additional intervention may be necessary to activate specific neural networks [1].
Repetitive transcranial magnetic stimulation (rTMS) is a noninvasive brain stimulation technique effected by transmitting bipolar magnetic pulses repeatedly on the cerebral cortex to generate induced current [17], modulating activity of cortical, subcortical, and the corticospinal pathways to improve function [20]. In general, low-frequency rTMS (≤1 Hz) inhibits cortical excitability, whereas high-frequency rTMS (≥5 Hz) increases cortical excitability and induces long-term potentiation, which contributes to the promotion of synaptic plasticity [1,21,22]. rTMS has been considered to be a promising tool for the treatment of somatomotor deficit after SCI [23,24]. However, some studies have shown that the effectiveness of rTMS is limited and variable, which may due to use of different stimulus parameters, number of sessions, targeted region, and the start time of use [20,25,26].
Recently, more and more researchers have realized that combination therapy is more beneficial to the regeneration and reconnection of neural circuits than monotherapy [17,27]. From the spinal to the motor cortex, combination therapy aims to promote plasticity at multiple levels of the neuraxis and may be the key to improve motor function after SCI [28]. In a clinical study, Benito et al [29] reported the combination of routine rehabilitation training and rTMS is beneficial to functional recovery, but the evaluation indexes are limited to the subjective function assessment scales, such as walking index for SCI, 10-meter walking test, and the lower-extremities motor score. The differences in biological effects between exercise training and rTMS at different levels of motor systems have not been studied, and their synergistic mechanism is still unclear. Thus, further studies in animal models of SCI are needed to explore the biological effects of exercise training and rTMS at different levels of motor systems. We proposed that significant motor function recovery following SCI may require the co-promotion of neuroplasticity both in the motor cortex and spinal cord through a combination therapy using rTMS and exercise training.
Therefore, this study aimed to investigate the effects of rTMS and exercise training on the recovery of motor function in a rat model of partial SCI. The training method was modified treadmill training (TT) to produce a standardized and consistent plantar stepping pattern because the pattern of plantar stepping helps activate motor function [30]. We conducted an animal experiment based on a rat model of partial SCI because rats have been identified to be the primary model to study the underlying mechanisms of function recovery after SCI [31]. We evaluated motor function by using the Basso, Beattie, and Bresnahan locomotor scale scores and the grid walking test. The Basso, Beattie, and Bresnahan scale is a universal, reliable, and valid measure of motor function recovery [32,33]. The grid walking test is valid and sensitive for sensorimotor coordination evaluation [34,35]. For motor cortical and spinal plasticity, we evaluated BDNF, synapsin I (SYN), and postsynaptic density protein-95 (PSD-95). BDNF modulates synaptic efficacy by altering release of presynaptic transmitter or increasing sensitivity of postsynaptic transmitters [36,37], thereby promoting neuroplasticity [38,39]. SYN is a presynaptic marker showing synaptic connectivity changes [40], and PSD-95 is a marker of postsynaptic remodeling [41].
Material and Methods
ANIMALS:
All procedures were conducted in accordance with the China Laboratory Animal Guidelines and followed the guidelines of the Institutional Animal Care and Use Committee of Nanjing Medical University. All procedures complied with animal protection, animal welfare, and ethical principles, and were approved by Institutional Animal Care and Use Committee of Nanjing Medical University, China (license no. IACUC-1901039).
Sixty female Sprague-Dawley rats (8–10 weeks, 200–220 g) were provided by the Animal Care Facility, Nanjing Medical University, China. The rats were housed in a temperature-controlled environment (22°C), with free access to food and water and a 12-h light/dark cycle.
Rats were randomly allocated to 5 groups (n=12 per group) with a computer-generated randomization algorithm: Sham surgery (Intact): rats underwent laminectomy without damaging the spinal cord; S-rTMS/Non-TT: Rats with induced SCI that performed sham rTMS without TT; S-rTMS/TT: Rats with SCI that performed TT with sham rTMS; rTMS/Non-TT: Rats with SCI that performed rTMS without TT; and rTMS/TT: Rats with SCI that performed TT immediately after the completion of rTMS.
SCI MODEL ESTABLISHMENT:
A moderate contusive SCI rat model was established with the Louisville Injury System Apparatus (LISA, University of Louisville, USA) impactor. To avoid damaging the respiratory center and urination center, leading to difficulties in postoperative care and high postoperative mortality, we set SCI at the ninth thoracic vertebra level. Surgical procedures followed previously published methods [42]. Briefly, rats were anesthetized via intraperitoneal injection of 10% chloral hydrate (3.5 mg/kg). Once the tail and paw withdrawal reflex disappeared, the back of the rat was shaved and disinfected. The skin and musculature were dissected to expose thoracic vertebrae, and the ninth thoracic vertebra was stabilized with a stabilization device. After that, vertebral laminectomy was performed to expose the spinal cord. Then, rats received a rapid strike via a tip (diameter=2.2 mm) driven with 138 Kpa (Figure 1A). The depth of penetration into the spinal cord was 1.2 mm. Finally, muscles and skin were sutured. Rats were placed on a heat-regulated mat until awake. The swing of the tail and paralyzed hind limbs were regarded as a sign of a successful model. The whole procedure was performed under aseptic conditions. Postoperative care was performed to empty bladders of all SCI rats at least twice a day until micturition control re-established.
TT: TT commenced 1 week after SCI. The instrument was provided by Indiana University School of Medicine, Indianapolis, USA. The partial body weight of rats was supported with a cloth harness [30], which was connected to a steel bridge. The 2 tracks slide back and forth alternately. Both hind paws wore boots that were immobilized on the pedals of 2 tracks and moved back and forth with the tracks. The pedals moved up and down to make the hind limbs of rats lift and fall in a standardized and consistent plantar stepping pattern. The tail was gently secured to the steel bridge to prevent it from interfering with the instrument (Figure 1B). The training schedule was 5 days per week, 10 min per day, for a total 8-week training period. Based on the situation of locomotion recovery, initial speed was 60 rpm (3.6 m/min) and gradually increased to 100 rpm (6 m/min) within the first training week and then was maintained at that speed until the end of the training period.
RTMS: rTMS commenced 1 week after surgery. Conscious rats were attached to a board with an elastic bandage to keep them stable, and their heads were fixed by pushpins placed around the head. An instrument (CCY-IA, Wuhan Yiruide medical Co., Hubei, China) with a 6-cm-diameter coil was used (Figure 1C). The stimulation site was located at the midline between the bregma and lambda, covering bilateral sensorimotor cortices [26]. The orientation of the coil was tangent to the skull. Stimulation parameters were as follows [23,43]: 10 Hz at 90% active motor threshold, 1000 pulses and a 25-s interval between each training. For sham rTMS [44], an inactive coil was placed where the active coil was normally placed, and the active coil was placed vertically above the inactive coil with parameters unchanged, so the rats could feel the same sounds and vibrations without being exposed to the magnetic field. The stimulation schedule was 5 days per week, 10 min per day, for a total 8-week period.
TISSUE COLLECTION:
After completing the final treatment and behavioral assessments, the rats of all groups were deeply anesthetized by 10% chloral hydrate. and then killed by transcardial perfusion with 0.9% saline, then 4% paraformaldehyde. Afterwards, the brain and the lumbar spinal cord (L2–4 level) were carefully separated and fixed in 4% paraformaldehyde overnight at 4°C. After gradient alcohol dehydration, the tissues were paraffin-embedded and sectioned serially to a thickness of 5 μm.
IMMUNOHISTOCHEMISTRY ASSAY:
As deparaffinization finished, slices were repaired with sodium citrate buffer (0.01 mol/L, pH 6.0). After peroxidase inactivation, phosphate-buffered saline washing and 10% goat serum blocking, sections were incubated overnight at 4°C with the following primary antibodies: rabbit anti- BDNF antibody (1: 800, Abcam, UK), anti-SYN antibody (1: 300, Abcam, UK), and anti- PSD-95 antibody (1: 200, Abcam, UK). Then, the tissues were incubated with horseradish peroxidase-conjugated goat anti-rabbit antibody (1: 300, Zhong Shan Jin Qiao, China) for 1 h at 37°C. 3,3′-diaminobenzidine-4 HCl/H2O2 (DAB, Vector Laboratories, Burlingame, CA, USA) was used for visualization. Hematoxylin was counterstained after BDNF and SYN staining. Images of the motor cortex and the ventral horn region of the lumbar spinal cord were obtained using an optical microscope at 200× and 400× view field by Leica Application Suite (Leica Microsystems, Wetzlar, Germany). Image J software (National Institutes of Health, Bethesda, Maryland, USA) was applied to analyze mean optical density values.
WESTERN BLOTTING:
Tissues in the motor cortex and the lumbar spinal cord (L2–4 level) of rats were selected. After homogenization and centrifugation, the supernatants were diluted with loading buffer. The protein samples were separated by 12% sodium dodecyl sulfate-polyacrylamide gel by electrophoresis (SDS-PAGE) and transferred on to polyvinylidene fluoride membranes (Millipore, USA). Then, the membranes were blocked with 5% milk solubilized in Tris-buffered saline with 0.1% Tween 20 at room temperature for 1 h. After that, the membranes were incubated with rabbit anti-BDNF antibody (1: 1000, Abcam, UK), anti-SYN antibody (1: 1000, Abcam, UK), anti- PSD-95 antibody (1: 1000, Abcam, UK), or glyceraldehyde phosphate dehydrogenase (GAPDH) (1: 1000, Proteintech, USA) overnight at 4°C. The next day, the membranes were incubated with horseradish peroxidase-conjugated goat anti-rabbit antibody (1: 2000, Zhong Shan Jin Qiao, China) for 1 h at room temperature. Reacting bands were visualized though enhanced chemiluminescence method. Image J software (National Institutes of Health, Bethesda, Maryland, USA) was applied for semi-quantitative analysis of the density of the immunoreactive bands.
STATISTICAL ANALYSIS:
Basso, Beattie, and Bresnahan scores were analyzed with repeated-measures analysis of variance, followed by Bonferroni-corrected post hoc tests. The remaining data were analyzed using one-way analysis of variance, followed by post hoc Tukey
Results
Motor Function Assessment
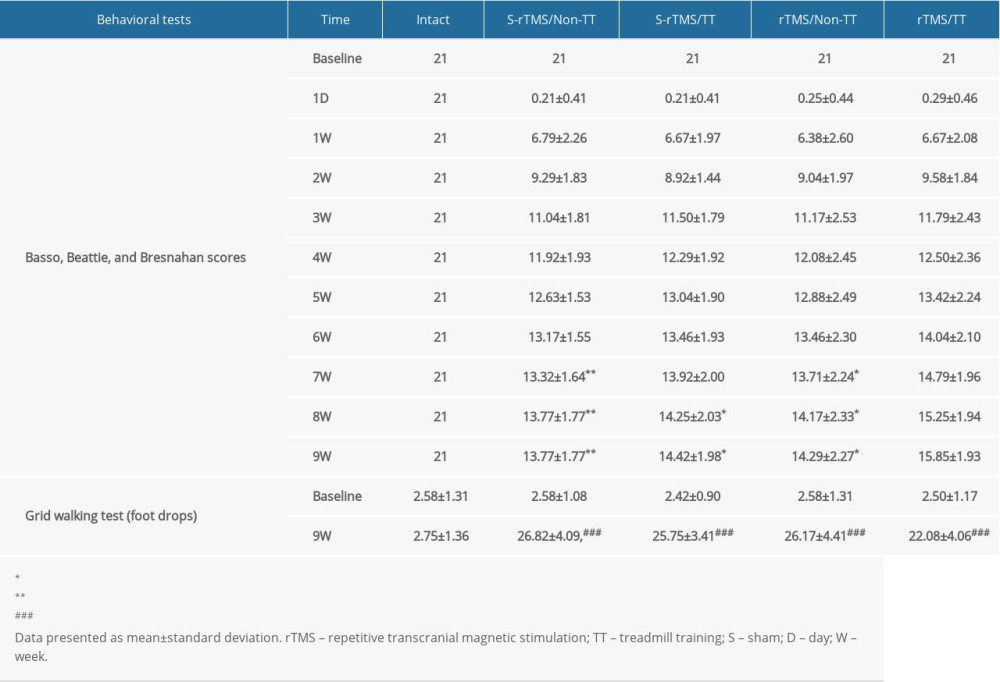
BASSO, BEATTIE, AND BRESNAHAN SCORES: At 1 week after injury, the scores in the S-rTMS/Non-TT, S-rTMS/TT, rTMS/Non-TT, and rTMS/TT groups were 6.79±2.26, 6.67±1.97, 6.38±2.60, and 6.67±2.08, respectively. No statistically significant difference was observed (P>0.05). From the seventh week to the ninth week after injury, the rTMS/TT group (7/8/9 weeks: 14.79±1.96, 15.25±1.94, 15.85±1.93) showed noticeably enhanced locomotion compared with the S-rTMS/Non-TT (7/8/9 weeks: 13.32±1.64, 13.77±1.77,13.77±1.77, and P<0.01) and rTMS/Non-TT (7/8/9 weeks: 13.71±2.24, 14.17±2.33, 14.29±2.27, and P<0.05) groups. At 8 weeks after injury, the rTMS/TT group showed significantly higher scores than the S-rTMS/TT group (8/9 weeks: 14.25±2.03,14.42±1.98, and P<0.05). No significant difference was observed among the S-rTMS/Non-TT, S-rTMS/TT, and rTMS/Non-TT rats (Figure 2A, Table 1).
GRID WALKING TEST: At 9 weeks after injury, the number of foot drops in the Intact, S-rTMS/Non-TT, S-rTMS/TT, rTMS/Non-TT, and rTMS/TT groups were 2.75±1.36, 26.82±4.09, 25.75±3.41, 26.17±4.41, and 22.08±4.06, respectively. The number of foot drops in the 4 groups of SCI rats were significantly higher than in the Intact rats (P<0.001). The rTMS/TT rats showed obviously reduced number of foot drops compared with the S-rTMS/Non-TT rats (P<0.05) (Figure 2B). However, there was no statistically significant difference among the S-rTMS/TT, rTMS/Non-TT, and S-rTMS/Non-TT groups.
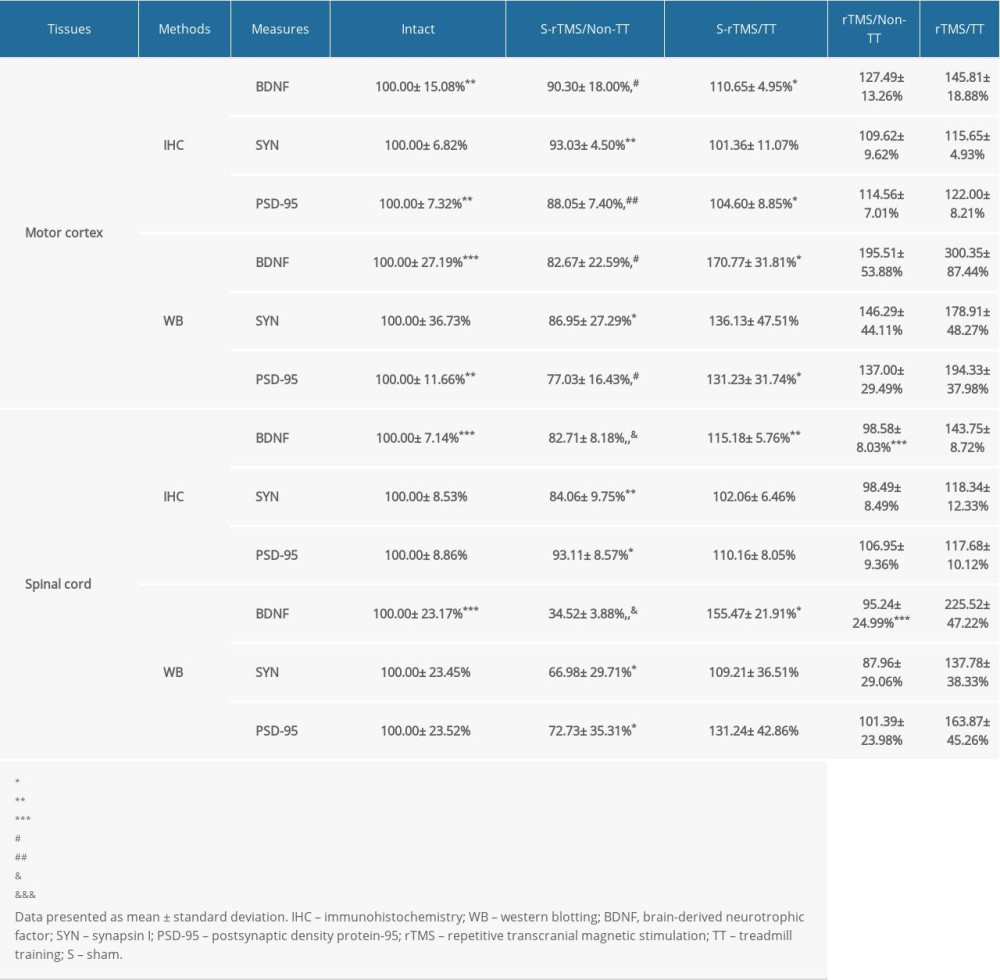
MOTOR CORTEX: In the 2 TT-treated groups, the relative densities of BDNF and PSD-95 were significantly higher in the rTMS/TT group (145.81±18.88% and 122.00±8.21%, respectively) compared with the S-rTMS/TT group (110.65±4.95%, 104.60±8.85%, and P<0.05, P<0.05, respectively, Figure 3B, 3D).
In the 2 Non-TT-treated groups, the relative densities of BDNF and PSD-95 were significantly higher in the rTMS/Non-TT group (127.49±13.26% and 114.56±7.01%) compared with the S-rTMS/Non-TT group (90.30±18.00%, 88.05±7.40%, and P<0.05, P<0.01, respectively, Figure 3B, 3D).
In 2 rTMS-treated groups, no significant difference was observed between the rTMS/TT and rTMS/Non-TT groups. In the 2 sham rTMS-treated groups, no significant difference was observed between the S-rTMS/TT and S-rTMS/Non-TT groups.
The relative densities of BDNF, SYN, and PSD-95 were far higher in the rTMS/TT group (145.81±18.88%, 115.65±4.93%, 122.00±8.21%) compared with the S-rTMS/Non-TT group (90.30±18.00%, 93.03±4.50%, 88.05±7.40%, and P<0.01, P<0.01, P<0.001, respectively, Figure 3A–3D, Table 2). There was no statistically significant difference between the S-rTMS/Non-TT and Intact group.
LUMBAR SPINAL CORD: Compared with the Intact group, the relative density of BDNF was significantly reduced in the S-rTMS/Non-TT group (82.71±8.18%, P<0.05, Figure 4B).
In the 2 TT-treated groups, the density of BDNF was significantly higher in the rTMS/TT group (143.75±8.72%) than that in the S-rTMS/TT group (115.18±5.76%, P<0.01, Figure 4B).
In the 2 Non-TT-treated groups, no significant difference was found between rTMS/Non-TT and S-rTMS/Non-TT.
In the 2 rTMS-treated groups, the density of BDNF was significantly higher in the rTMS/TT group (143.75±8.72%) compared with the rTMS/Non-TT (98.58±8.03%, P<0.001, Figure 4B).
In the 2 sham rTMS-treated groups, the S-rTMS/TT group had significantly higher BDNF density compared with the S-rTMS/Non-TT group (P<0.001, Figure 4B).
The rTMS/TT group (143.75±8.72%, 118.34±12.33%, 117.68±10.12%) had higher relative densities of BDNF, SYN, and PSD-95 compared with the S-rTMS/Non-TT group (82.71±8.18%, 84.06±9.75%, 93.11±8.57%, and P<0.001, P<0.01, P<0.05, respectively, Figure 4A–4D).
MOTOR CORTEX: In the 2 TT-treated groups, the expressions of BDNF and PSD-95 were significantly higher in the rTMS/TT group (300.35±87.44%, 194.33±37.98%) compared with the S-rTMS/TT group (170.77±31.81%, 131.23±31.74%, and P<0.05, P<0.05, respectively, Figure 5B, 5D). In the 2 Non-TT-treated groups, the rTMS/Non-TT group (195.51±53.88%, 137.00±29.49%) also had significantly higher expressions of BDNF and PSD-95 compared with the S-rTMS/Non-TT group (82.67±22.59%, 77.03±16.43%, and P<0.05, P<0.05, respectively, Figure 5B, 5D).
The expressions of BDNF, SYN, and PSD-95 were higher in the rTMS/TT group (300.35±87.44%, 178.91±48.27%, 194.33±37.98%) compared with the S-rTMS/Non-TT group (82.67±22.59%, 86.95±27.29%, 77.03±16.43%, and P<0.001, P<0.05, P<0.001, respectively, Figure 5A–5D). Taken together, these results further confirmed the results of immunohistochemistry analysis of the motor cortex.
LUMBAR SPINAL CORD: Compared with the Intact group, the BDNF expression was significantly reduced in the S-rTMS/Non-TT group (34.52±3.88%, P<0.05, Figure 6B). In the 2 TT-treated groups, the BDNF expression was significantly higher in the rTMS/TT group (225.52±47.22%) than that in the S-rTMS/TT group (155.47±21.91%, P<0.05, Figure 6B). In the 2 Non-TT-treated groups, no significant difference was found between rTMS/Non-TT and S-rTMS/Non-TT. In the 2 rTMS-treated groups, the BDNF expression was significantly higher in the rTMS/TT group compared with the rTMS/Non-TT (95.24±24.99%, P<0.001, Figure 6B). In 2 sham rTMS-treated groups, the S-rTMS/TT group had significantly higher BDNF expression compared with the S-rTMS/Non-TT group (P<0.001, Figure 6B). The rTMS/TT group (225.52±47.22%, 137.78±38.33%, 163.87±45.26%) had higher expressions of BDNF, SYN, and PSD-95 compared with the S-rTMS/Non-TT group (34.52±3.88%, 66.98±29.71%, 72.73±35.31%, and P<0.001, P<0.05, P<0.05, respectively, Figure 6A–6D). Taken together, these results further confirmed the results of immunohistochemistry analysis of the spinal cord.
Discussion
EFFECTS OF TT:
We found the effect of TT with sham rTMS on motor function recovery was limited. Nicola et al [18] also found no significant differences in Basso, Beattie, and Bresnahan scores between TT alone and non-trained SCI rats. Research on TT applied following SCI has often shown controversial results in motor function recovery [9]. Some studies found that TT alone improved motor function, but it often took considerable time and effort, such as multiple sessions per day [14] and longer duration (30 min) [15] and periods (more than 9 weeks) [19].
In the spinal cord, the BDNF expression was significantly reduced after SCI. We found TT alone reversed this change, enhancing BDNF expression, as reported previously [14,16].
BDNF acts as a mediator or instructor in inducing activity-dependent plasticity [45] by stimulating dendritic spines and regulating synapses [39,42]. As a crucial downstream effector for BDNF [46], SYN is phosphorylated by BDNF, which mediates synaptic vesicle circulation and neurotransmitter release [47]. PSD-95 facilitates downstream intracellular signaling and modulates receptor stability, thus contributing to synaptic plasticity [41,48–50]. In our study, the higher expressions of presynaptic and postsynaptic plasticity markers SYN and PSD-95 were not observed in the TT alone group. These results indicated that the activation of BDNF in the spinal cord induced by TT was still insufficient to extend to downstream effectors and failed to produce an important effect on synaptic plasticity, which may partially explain the limited motor function recovery.
In the motor cortex, we found that TT alone was not effective in increasing expressions of BDNF and synaptic plasticity markers. However, Ilha et al [51] showed that overground gait training was able to promote motor cortical plasticity. Similar repetitive motor training in our study seemed to train paralyzed limbs without the need for cortical relearning, such as step initiation and forward progression, thus improving the motor learning and control ability of the motor cortex and subsequently enhancing supraspinal drive to the spinal motor circuit, which may be an important way to promote motor function recovery after SCI [51].
EFFECTS OF RTMS:
In the motor cortex, we corroborated that the expressions of BDNF and PSD-95 were increased by rTMS. Recently, Fujiki et al [22] also found that high-frequency rTMS strongly activated molecular pathways critical for synaptic plasticity in the motor cortex of lightly anesthetized rats. It has been reported that synaptic remodeling in the motor cortex is a target to improve function recovery following SCI [28]. Hence, rTMS is an effective combined treatment to promote cortical plasticity, remedying some shortcomings of TT.
However, applying rTMS without TT was insufficient to promote spinal plasticity. It is known that the increase of BDNF has an activity-dependent property [52], and exercise is able to upregulate BDNF genes in the spinal cord [53]. It is reasonable to think that rTMS has limitations in the absence of TT.
We observed that applying rTMS alone did not lead to behavioral improvement in partial SCI rats. In a clinical study, rTMS also did not induce changes in sensory and motor function in patients with chronic SCI [25]. Krishnan et al [26] determined the effective time range for rTMS intervention in rats with incomplete SCI, and the results showed that rTMS performed 2 weeks after injury was not effective in improving motor function, but it was effective within 10 minutes. A meta-analysis showed that the efficacy of rTMS gradually decreased with the prolongation of disease duration [54]. These results indicate that the application of rTMS alone may have a limited time window, because a decrease in cortical spontaneous neuronal activity was observed within a few minutes after SCI [55], which was associated with poor recovery. Reducing and reversing the reduction of early cortical spontaneous activity as soon as possible plays a key role in the neurological recovery after SCI [26]. It is better to start using rTMS at a very early stage after SCI, at 2 days [23] or even 10 minutes after injury [26], which is difficult to carry out in clinical practice.
EFFECTS OF COMBINATION THERAPY OF RTMS AND TT:
In our study, combination therapy achieved optimal locomotion recovery, with higher Basso, Beattie, and Bresnahan scores and fewer foot drops. Yang et al [17] reported the possible relationship between rTMS and exercise training in promoting motor function recovery as follows: exercise training can establish motor memory through repeated practice of specific movements, which is a form of use-dependent plasticity, and rTMS enhances the encoding of motor memory related with use-dependent plasticity in the motor cortex. We consider that rTMS excites the motor cortex and related subcortical structures inducing the activation of particular neural networks, but it does not lead to long-term motor behavior changes by itself. Then, TT provides correct motor guidance to make target behaviors correlate with activated networks, thus improving motor performance.
In addition, the combination therapy created a cumulative impact on increased BDNF expression in both the motor cortex and spinal cord. A recent study also showed that combined TT and injury site magnetic stimulation increased the BDNF expression following cervical SCI in rats [4]. These results raise the question as to whether the synergistic activation of BDNF is the key to the improvement of locomotion in combination therapy. Although there is no direct verification in this study, recent studies have identified that both rTMS and TT promote neurological recovery though the BDNF-TrkB signaling pathway [16,40].
We also found that combination therapy further increased the expressions of synaptic plasticity markers in the motor cortex and spinal cord, suggesting that the plastic changes were deeper in the combination therapy group than those in the single-therapy groups. We consider that there were interconnections between cortical and spinal motor systems, because plastic changes occurring at one level may be influenced and/or result in plasticity at other levels [56]. The adaptive plasticity occurring in a coordinated manner at different levels of the motor system is an important factor for promoting locomotion recovery after incomplete SCI.
LIMITATIONS:
The three-dimensional analysis of gait kinematics may be beneficial to observe the slight changes of hind-limb motor performance. Additionally, there are anatomical differences between rats and humans. The characteristics of pathophysiological changes and spontaneous function recovery are also different after SCI [31], so further evaluation may be needed to determine its possible clinical effects.
Conclusions
The present study demonstrated that combined treatment using rTMS with TT remarkably promoted motor function recovery in a modified rat model of SCI, which involved promoting neuroplasticity in a coordinated manner at the motor cortex and spinal cord levels. This combined approach to improving motor function following SCI requires further evaluation to determine the possible clinical applications.
Figures
 Figure 1. Interventions and measures. (A) Spinal cord injury model establishment. (B) Treadmill training. (C) Repetitive transcranial magnetic stimulation. (D) Basso, Beattie, and Bresnahan locomotor scale. (E) Grid walking test.
Figure 1. Interventions and measures. (A) Spinal cord injury model establishment. (B) Treadmill training. (C) Repetitive transcranial magnetic stimulation. (D) Basso, Beattie, and Bresnahan locomotor scale. (E) Grid walking test. 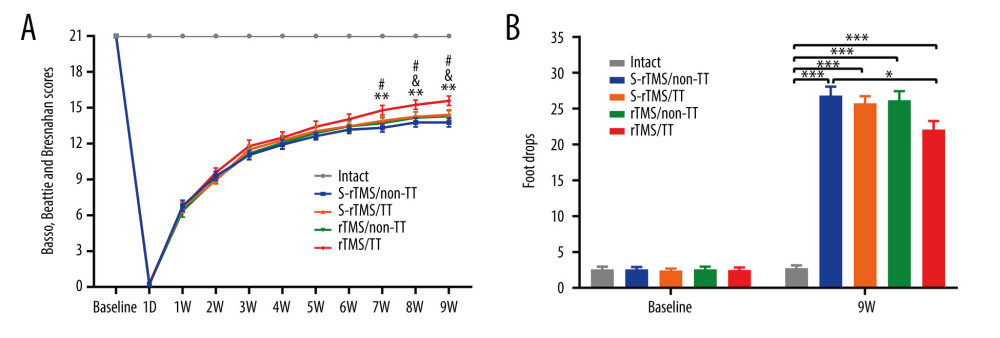 Figure 2. Motor function assessment. (A) Basso, Beattie, and Bresnahan scores. ** P<0.01, rTMS/TT vs S-rTMS/Non-TT; # P<0.05, rTMS/TT vs rTMS/Non-TT; & P<0.05, rTMS/TT vs S-rTMS/TT. (B) Grid walking test. The number of foot drops in each group. *** P<0.001, * P<0.05. Twelve rats in each group. At 8 weeks after injury, 1 rat in the S-rTMS/Non-TT group died of abdominal distention. Data presented as mean±standard error of mean. D – day; W,– week; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 2. Motor function assessment. (A) Basso, Beattie, and Bresnahan scores. ** P<0.01, rTMS/TT vs S-rTMS/Non-TT; # P<0.05, rTMS/TT vs rTMS/Non-TT; & P<0.05, rTMS/TT vs S-rTMS/TT. (B) Grid walking test. The number of foot drops in each group. *** P<0.001, * P<0.05. Twelve rats in each group. At 8 weeks after injury, 1 rat in the S-rTMS/Non-TT group died of abdominal distention. Data presented as mean±standard error of mean. D – day; W,– week; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. 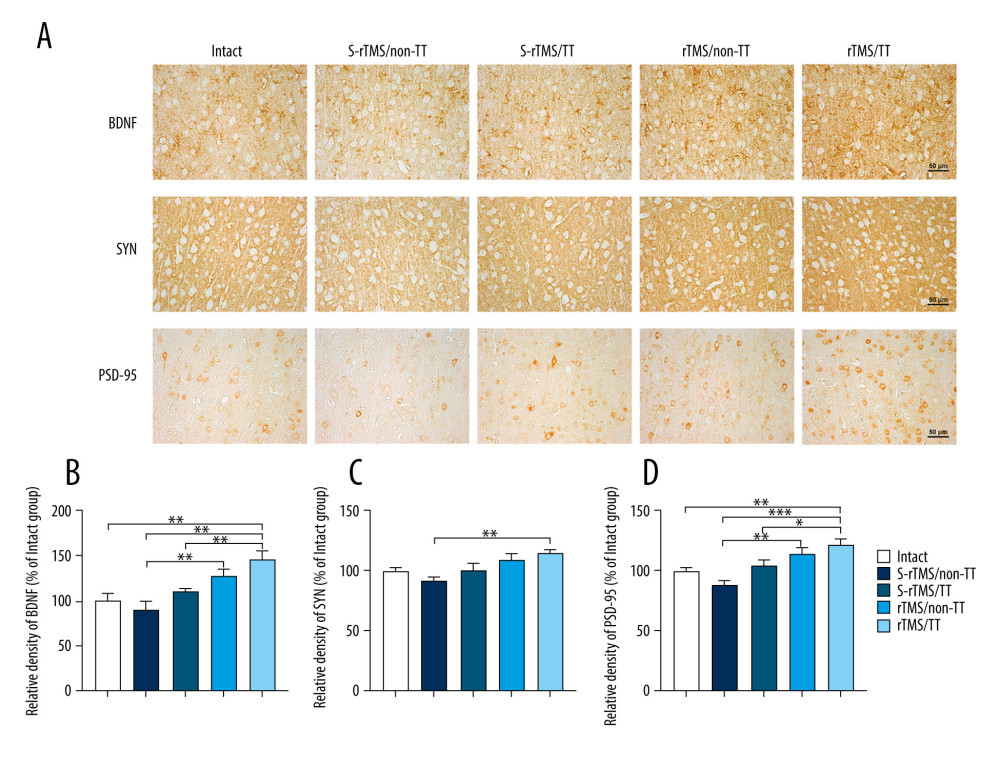 Figure 3. Immunohistochemistry analysis of motor cortex. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 50 μm. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 3. Immunohistochemistry analysis of motor cortex. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 50 μm. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. 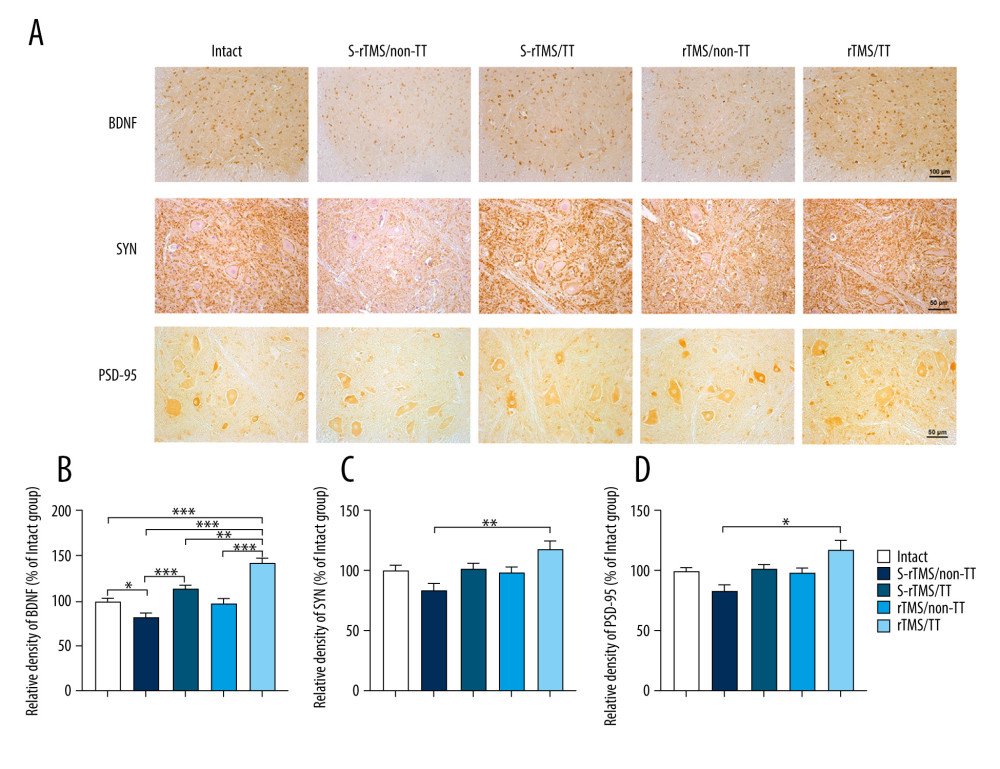 Figure 4. Immunohistochemistry analysis of spinal cord. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 100 μm in BDNF. 50 μm in SYN and PSD-95. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 4. Immunohistochemistry analysis of spinal cord. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 100 μm in BDNF. 50 μm in SYN and PSD-95. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. 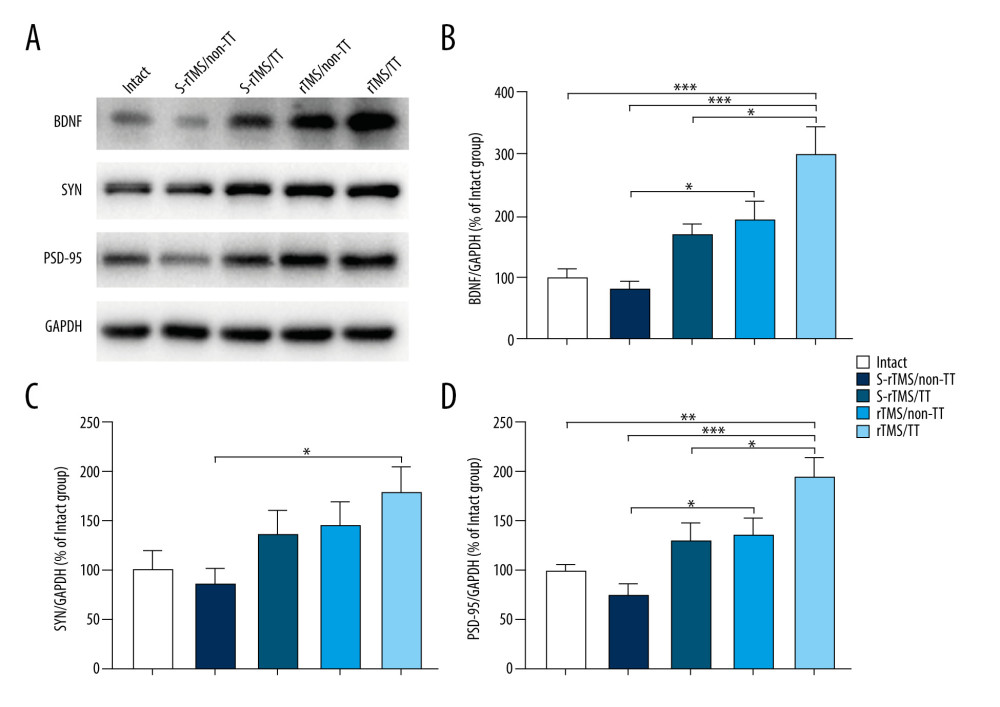 Figure 5. Western blotting analysis of motor cortex. (A) Western blotting representative bands of BDNF, SYN and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 5. Western blotting analysis of motor cortex. (A) Western blotting representative bands of BDNF, SYN and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. 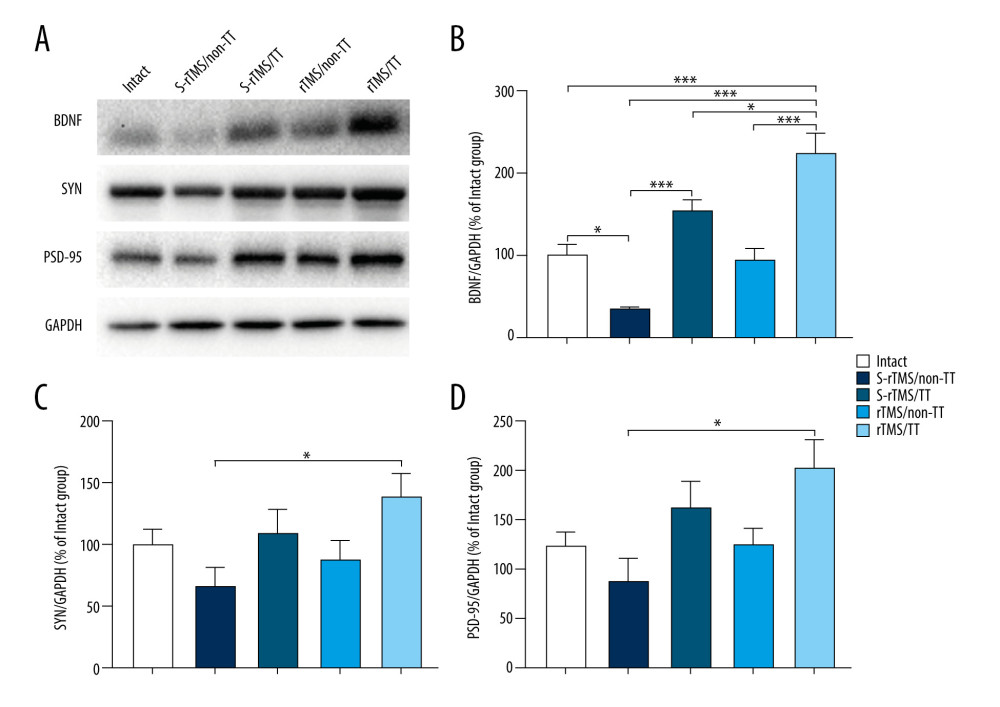 Figure 6. Western blotting analysis of spinal cord. (A) Western blotting representative bands of BDNF, SYN, and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 6. Western blotting analysis of spinal cord. (A) Western blotting representative bands of BDNF, SYN, and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. References
1. Zheng Y, Mao YR, Yuan TF, Multimodal treatment for spinal cord injury: A sword of neuroregeneration upon neuromodulation: Neural Regen Res, 2020; 15; 1437-50
2. Abel TE, Juan F, Fenrich KK, Eliciting inflammation enables successful rehabilitative training in chronic spinal cord injury: Brain, 2018; 141; 1946-62
3. Nardone R, Höller Y, Brigo F, Functional brain reorganization after spinal cord injury: Systematic review of animal and human studies: Brain Res, 2013; 1504; 58-73
4. Hou J, Nelson R, Mohammad N, Effect of simultaneous combined treadmill training and magnetic stimulation on spasticity and gait impairments following cervical spinal cord injury (C-SCI): J Neurotrauma, 2020; 37; 1999-2013
5. Kirshblum SC, Priebe MM, Ho CH, Spinal cord injury medicine. 3. Rehabilitation phase after acute spinal cord injury: Arch Phys Med Rehabil, 2007; 88; S62-70
6. Cote MP, Murray M, Lemay MA, Rehabilitation strategies after spinal cord injury: Inquiry into the mechanisms of success and failure: J Neurotrauma, 2017; 34; 1841-57
7. Kristina L, Anja S, Tobias H, Enhanced voluntary exercise improves functional recovery following spinal cord injury by impacting the local neuroglial injury response and supporting the rewiring of supraspinal circuits: J Neurotrauma, 2018; 35; 2904-15
8. Fehlings MG, Tetreault LA, Wilson JR, A clinical practice guideline for the management of acute spinal cord injury: Introduction, rationale, and scope: Global Spine J, 2017; 7; 84S-94S
9. Battistuzzo CR, Callister RJ, Callister R, Galea MP, A systematic review of exercise training to promote locomotor recovery in animal models of spinal cord injury: J Neurotrauma, 2012; 29; 1600-13
10. Gazula VR, Roberts M, Luzzio C, Effects of limb exercise after spinal cord injury on motor neuron dendrite structure: J Comp Neurol, 2004; 476; 130-45
11. Zhang W, Yang B, Weng H, Wheel running improves motor function and spinal cord plasticity in mice with genetic absence of the corticospinal tract: Front Cell Neurosci, 2019; 13; 106
12. Loy K, Schmalz A, Hoche T, Enhanced voluntary exercise improves functional recovery following spinal cord injury by impacting the local neuroglial injury response and supporting the rewiring of supraspinal circuits: J Neurotrauma, 2018; 35; 2904-15
13. Yu P, Zhang W, Liu Y, The effects and potential mechanisms of locomotor training on improvements of functional recovery after spinal cord injury: Int Rev Neurobiol, 2019; 147; 199-217
14. Wang H, Liu NK, Zhang YP, Treadmill training induced lumbar motoneuron dendritic plasticity and behavior recovery in adult rats after a thoracic contusive spinal cord injury: Exp Neurol, 2015; 271; 368-78
15. Multon S, Franzen R, Poirrier AL, The effect of treadmill training on motor recovery after a partial spinal cord compression-injury in the adult rat: J Neurotrauma, 2003; 20; 699-706
16. Li X, Wu Q, Xie C, Blocking of BDNF-TrkB signaling inhibits the promotion effect of neurological function recovery after treadmill training in rats with spinal cord injury: Spinal Cord, 2019; 57; 65-74
17. Yang YW, Pan WX, Xie Q, Combined effect of repetitive transcranial magnetic stimulation and physical exercise on cortical plasticity: Neural Regen Res, 2020; 15; 1986-94
18. Nicola FC, Rodrigues LP, Crestani T, Human dental pulp stem cells transplantation combined with treadmill training in rats after traumatic spinal cord injury: Braz J Med Biol Res, 2016; 49; e5319
19. Battistuzzo CR, Rank MM, Flynn JR, Gait recovery following spinal cord injury in mice: Limited effect of treadmill training: J Spinal Cord Med, 2016; 39; 335-43
20. Tazoe T, Perez MA, Effects of repetitive transcranial magnetic stimulation on recovery of function after spinal cord injury: Arch Phys Med Rehabil, 2015; 96; S145-55
21. Nardone R, Höller Y, Brigo F, Descending motor pathways and cortical physiology after spinal cord injury assessed by transcranial magnetic stimulation: A systematic review: Brain Res, 2015; 1619; 139-54
22. Fujiki M, Yee KM, Steward O, Non-invasive high frequency repetitive transcranial Magnetic stimulation (hfrTMS) robustly activates molecular pathways implicated in neuronal growth and synaptic plasticity in select populations of neurons: Front Neurosci, 2020; 14; 558
23. Poirrier AL, Nyssen Y, Scholtes F, Repetitive transcranial magnetic stimulation improves open field locomotor recovery after low but not high thoracic spinal cord compression-injury in adult rats: J Neurosci Res, 2004; 75; 253-61
24. Awad BI, Carmody MA, Zhang X, Transcranial magnetic stimulation after spinal cord injury: World Neurosurg, 2015; 83; 232-35
25. Kuppuswamy A, Balasubramian AV, Maksimovic R, Action of 5 Hz repetitive transcranial magnetic stimulation on sensory, motor and autonomic function in human spinal cord injury: Clin Neurophysiol, 2011; 122; 2452-61
26. Krishnan VS, Shin SS, Belegu V, Multimodal evaluation of TMS-induced somatosensory plasticity and behavioral recovery in rats with contusion spinal cord injury: Front Neurosci, 2019; 13; 387
27. Xia Y, Chen D, Xia H, Serotonergic projections to lumbar levels and its plasticity following spinal cord injury: Neurosci Lett, 2017; 649; 70-77
28. Kim BG, Dai HN, McAtee M, Bregman BS, Modulation of dendritic spine remodeling in the motor cortex following spinal cord injury: Effects of environmental enrichment and combinatorial treatment with transplants and neurotrophin-3: J Comp Neurol, 2008; 508; 473-86
29. Benito J, Kumru H, Murillo N, Motor and gait improvement in patients with incomplete spinal cord injury induced by high-frequency repetitive transcranial magnetic stimulation: Top Spinal Cord Inj Rehabil, 2012; 18; 106-12
30. Hayashibe M, Homma T, Fujimoto K, Locomotor improvement of spinal cord-injured rats through treadmill training by forced plantar placement of hind paws: Spinal Cord, 2016; 54; 521-29
31. Filipp ME, Travis BJ, Henry SS, Differences in neuroplasticity after spinal cord injury in varying animal models and humans: Neural Regen Res, 2019; 14; 7-19
32. Basso DM, Beattie MS, Bresnahan JC, A sensitive and reliable locomotor rating scale for open field testing in rats: J Neurotrauma, 1995; 12; 1-21
33. Kjell J, Olson L, Rat models of spinal cord injury: From pathology to potential therapies: Dis Model Mech, 2016; 9; 1125-37
34. Grill R, Murai K, Blesch A, Cellular delivery of neurotrophin-3 promotes corticospinal axonal growth and partial functional recovery after spinal cord injury: J Neurosci, 1997; 17; 5560-72
35. Sandrow HR, Shumsky JS, Amin A, Houle JD, Aspiration of a cervical spinal contusion injury in preparation for delayed peripheral nerve grafting does not impair forelimb behavior or axon regeneration: Exp Neurol, 2008; 210; 489-500
36. Itami C, Kimura F, Kohno T, Brain-derived neurotrophic factor-dependent unmasking of “silent” synapses in the developing mouse barrel cortex: Proc Natl Acad Sci USA, 2003; 100; 13069-74
37. Edelmann E, Lessmann V, Brigadski T, Pre-and postsynaptic twists in BDNF secretion and action in synaptic plasticity: Neuropharmacology, 2014; 76; 610-27
38. Shen K, Cowan CW, Guidance molecules in synapse formation and plasticity: Cold Spring Harb Perspect Biol, 2010; 2; a001842
39. Cote MP, Azzam GA, Lemay MA, Activity-dependent increase in neurotrophic factors is associated with an enhanced modulation of spinal reflexes after spinal cord injury: J Neurotrauma, 2011; 28; 299-309
40. Macias M, Nowicka D, Czupryn A, Exercise-induced motor improvement after complete spinal cord transection and its relation to expression of brain-derived neurotrophic factor and presynaptic markers: BMC Neurosci, 2009; 10; 144
41. Okabe S, Kim HD, Miwa A, Kuriu T, Okado H, Continual remodeling of postsynaptic density and its regulation by synaptic activity: Nat Neurosci, 1999; 2; 804-11
42. Zhang YP, Burke DA, Shields LBE, Spinal cord contusion based on precise vertebral stabilization and tissue displacement measured by combined assessment to discriminate small functional differences: J Neurotrauma, 2008; 25; 1227-40
43. Guo M, Wu L, Song Z, Yang B, Enhancement of neural stem cell proliferation in rats with spinal cord injury by a combination of repetitive transcranial magnetic stimulation (rTMS) and human umbilical cord blood mesenchymal stem cells (hUCB-MSCs): Med Sci Monit, 2020; 26; e924445
44. Luo J, Zheng H, Zhang L, High-frequency repetitive transcranial magnetic stimulation (rTMS) improves functional recovery by enhancing neurogenesis and activating BDNF/TrkB signaling in ischemic rats: Int J Mol Sci, 2017; 18; 455
45. Colucci-D’Amato L, Speranza L, Volpicelli F, Neurotrophic factor BDNF, physiological functions and therapeutic potential in depression, neurodegeneration and brain cancer: Int J Mol Sci, 2020; 21; 7777
46. Jovanovich JN, Czernik AJ, Fienberg AA, Synapsins as mediators of BDNF-enhanced neurotransmitter release: Nat Neurosci, 2000; 3; 323-29
47. Lau BY, Foldes AE, Alieva NO, Increased synapsin expression and neurite sprouting in lamprey brain after spinal cord injury: Exp Neurol, 2011; 228; 283-93
48. Marrs GS, Green SH, Dailey ME, Rapid formation and remodeling of postsynaptic densities in developing dendrites: Nat Neurosci, 2001; 4; 1006-13
49. Zelano J, Berg A, Thams S, SynCAM1 expression correlates with restoration of central synapses on spinal motoneurons after two different models of peripheral nerve injury: J Comp Neurol, 2009; 517; 670-82
50. D’mello R, Marchand F, Pezet S, Perturbing PSD-95 interactions with NR2B-subtype receptors attenuates spinal nociceptive plasticity and neuropathic pain: Mol Ther, 2011; 19; 1780-92
51. Ilha J, Meireles A, de Freitas GR, Overground gait training promotes functional recovery and cortical neuroplasticity in an incomplete spinal cord injury model: Life Sci, 2019; 232; 116627
52. Lu B, BDNF and activity-dependent synaptic modulation: Learn Mem, 2003; 10; 86-98
53. Gómez-Pinilla F, Ying Z, Roy RR, Voluntary exercise induces a BDNF-mediated mechanism that promotes neuroplasticity: J Neurophysiol, 2002; 88; 2187-95
54. Zhang L, Xing G, Fan Y, Short- and long-term effects of repetitive transcranial magnetic stimulation on upper limb motor function after stroke: A systematic review and meta-analysis: Clin Rehabil, 2017; 31; 1137-53
55. Aguilar J, Humanes-Valera D, Alonso-Calviño E, Spinal cord injury immediately changes the state of the brain: J Neurosci, 2010; 30; 7528-37
56. Raineteau O, Schwab ME, Plasticity of motor systems after incomplete spinal cord injury: Nat Rev Neurosci, 2001; 2; 263-73
Figures
 Figure 1. Interventions and measures. (A) Spinal cord injury model establishment. (B) Treadmill training. (C) Repetitive transcranial magnetic stimulation. (D) Basso, Beattie, and Bresnahan locomotor scale. (E) Grid walking test.
Figure 1. Interventions and measures. (A) Spinal cord injury model establishment. (B) Treadmill training. (C) Repetitive transcranial magnetic stimulation. (D) Basso, Beattie, and Bresnahan locomotor scale. (E) Grid walking test. Figure 2. Motor function assessment. (A) Basso, Beattie, and Bresnahan scores. ** P<0.01, rTMS/TT vs S-rTMS/Non-TT; # P<0.05, rTMS/TT vs rTMS/Non-TT; & P<0.05, rTMS/TT vs S-rTMS/TT. (B) Grid walking test. The number of foot drops in each group. *** P<0.001, * P<0.05. Twelve rats in each group. At 8 weeks after injury, 1 rat in the S-rTMS/Non-TT group died of abdominal distention. Data presented as mean±standard error of mean. D – day; W,– week; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 2. Motor function assessment. (A) Basso, Beattie, and Bresnahan scores. ** P<0.01, rTMS/TT vs S-rTMS/Non-TT; # P<0.05, rTMS/TT vs rTMS/Non-TT; & P<0.05, rTMS/TT vs S-rTMS/TT. (B) Grid walking test. The number of foot drops in each group. *** P<0.001, * P<0.05. Twelve rats in each group. At 8 weeks after injury, 1 rat in the S-rTMS/Non-TT group died of abdominal distention. Data presented as mean±standard error of mean. D – day; W,– week; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. Figure 3. Immunohistochemistry analysis of motor cortex. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 50 μm. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 3. Immunohistochemistry analysis of motor cortex. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 50 μm. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. Figure 4. Immunohistochemistry analysis of spinal cord. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 100 μm in BDNF. 50 μm in SYN and PSD-95. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 4. Immunohistochemistry analysis of spinal cord. (A) Immunohistochemistry staining of BDNF, SYN and PSD-95. (B) Relative density of BDNF. (C) Relative density of SYN. (D) Relative density of PSD-95. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. Scale bar: 100 μm in BDNF. 50 μm in SYN and PSD-95. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. Figure 5. Western blotting analysis of motor cortex. (A) Western blotting representative bands of BDNF, SYN and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 5. Western blotting analysis of motor cortex. (A) Western blotting representative bands of BDNF, SYN and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. Figure 6. Western blotting analysis of spinal cord. (A) Western blotting representative bands of BDNF, SYN, and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham.
Figure 6. Western blotting analysis of spinal cord. (A) Western blotting representative bands of BDNF, SYN, and PSD-95. (B) Quantification of BDNF expression. (C) Quantification of SYN expression. (D) Quantification of PSD-95 expression. Data presented as mean±standard error of mean. * P<0.05, ** P<0.01, *** P<0.001. Four rats in each group. BDNF – brain-derived neurotrophic factor; SYN – synapsin I; PSD-95 – postsynaptic density protein-95; GAPDH – glyceraldehyde phosphate dehydrogenase; rTMS – repetitive transcranial magnetic stimulation; TT – treadmill training; S – sham. In Press
05 Mar 2024 : Clinical Research
Effects of Thermal Insulation on Recovery and Comfort of Patients Undergoing Holmium Laser LithotripsyMed Sci Monit In Press; DOI: 10.12659/MSM.942836
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952