30 May 2021: Clinical Research
Walking Training with a Weight Support Feedback Cane Improves Lower Limb Muscle Activity and Gait Ability in Patients with Chronic Stroke: A Randomized Controlled Trial
Young Sic Kang1BCE, Gku Bin Oh1BCF, Ki Hun Cho1AEG*DOI: 10.12659/MSM.931565
Med Sci Monit 2021; 27:e931565
Abstract
BACKGROUND: Induction of proper weight transfer to the affected lower limb should be considered the most essential factor for successful stroke cane gait training. This study aimed to investigate the effect of walking training with a weight support feedback cane on lower limb muscle activity and gait ability of chronic stroke patients.
MATERIAL AND METHODS: Thirty stroke patients were randomized into 2 groups: a weight support feedback cane gait training group (WSFC group, n=15) and a conventional cane gait training group (CC group, n=15). All subjects were enrolled in standard rehabilitation programs for 4 weeks. Additionally, the WSFC group participated in WSFC gait training and the CC group participated in conventional cane gait training for 4 weeks. During WSFC gait training, the weight support rate loaded on the cane was reduced by 10% every week from 60% to 30% based on the measured initial cane dependence, while the CC group participated in conventional cane gait training with verbal instruction to reduce cane dependence. Lower limb muscle activity and gait ability were measured using wireless surface electromyography and a 3-axis accelerometer during walking.
RESULTS: The WSFC group showed significantly greater improvement than the CC group in lower limb muscle activity and gait ability (P<0.05).
CONCLUSIONS: Cane gait training significantly improved lower limb muscle activity and gait ability in stroke regardless of the training method; however, the addition of real-time weight support feedback to cane gait training appears to provide further benefit compared with conventional cane gait training in chronic stroke patients.
Keywords: Body-Weight Trajectory, Gait, Stroke, Canes, Exercise Therapy, gait analysis, Gait Disorders, Neurologic, Lower Extremity, stroke rehabilitation, Walking, Walking Speed, Weight-Bearing
Background
Stroke is classified as ischemic, caused by blockage of blood vessels supplying blood to the brain, and hemorrhagic, caused by rupture of blood vessels in the brain [1]. Stroke is a leading cause of death and dysfunction worldwide [2] and in general, it is associated with muscle weakness, decreased sensation, decreased cognitive function, depression, and decreased quality of life [3–5]. In particular, muscle weakness in the affected side causes overuse and asymmetrical weight shift to the non-affected lower limb [6], leading to an increased risk of falls, decreased independence in daily life, decreased postural control, and asymmetrical walking pattern [7,8]. Therefore, rehabilitation for symmetrical weight transfer and gait enhancement is fundamental to improve the independence and quality of life of patients with stroke [9,10].
In clinical practice, various assistive devices, such as parallel bars, walker, and cane, are used for balance and gait training of stroke patients. Among them, a cane can help to increase the base of support for stroke patients to provide postural stability and improves weight transfer ability in the standing position and walking [11–13]. Using a cane during the single-limb stance phase helps to retrain weight transfer to the affected lower limb and provides tactile information about the ground [14,15]. In addition, using a cane can contribute to stable postural control by controlling the rapid movement of the center of gravity during the stance phase [16]. Park reported that the use of a cane is effective in improving the weight support rate of the affected lower limb in patients with stroke [17]. Moreover, Boonsinsukh et al reported that cane training with auditory feedback according to the weight support rate of the affected lower limb leads to improvement of muscle activity in the affected tensor fasciae latae and vastus medialis [18]. In contrast, several studies have shown that the use of a cane in the early rehabilitation period caused a decrease in muscle activity of the affected lower limb [12,19] and it interferes with symmetrical weight distribution, which ultimately interferes with acquisition of independent gait ability [20,21]. Although the main purpose of using a cane is to help weight distribution to the affected lower limb, improper use of a cane can contribute to an asymmetrical gait pattern by inducing excessive weight support to the non-affected lower limb [16].
Therefore, for successful cane gait training, induction of proper weight transfer to the affected lower limb should be considered the most essential factor [6,22]. However, in clinical practice, it is difficult to quantitatively monitor the weight carried on the cane during cane gait training due to technical problems. Additionally, it is difficult for patients to receive accurate feedback on weight support on the paretic lower limb during cane gait training [23]. Moreover, there is insufficient information on the effects of progressive weight support induction on the affected lower limb during cane gait training on muscle activity and gait in patients with stroke.
Thus, this study aimed to investigate the effect of weight support feedback cane gait training that provided real-time feedback of the user’s weight support loaded on a cane on the lower limb muscle activity and gait ability of patients with chronic stroke. We hypothesized that 4 weeks of weight support feedback cane gait training would show improvements in lower limb muscle activity and gait ability in chronic stroke patients.
Material and Methods
STUDY DESIGN:
This randomized controlled trial was conducted at a rehabilitation hospital (experimental period: June 2019 to December 2019). All subjects were randomized into 2 groups: a weight support feedback cane gait training group (WSFC group) and a conventional cane gait training group (CC group). Sealed envelopes were used to conduct randomization. The inside of each sealed envelope was marked with an O or X. Subjects who selected envelopes marked with O were assigned to the WSFC group, and those who selected envelopes marked with X were assigned to the CC group. Randomization was conducted before the pre-test by a physical therapist who did not participate in this study. In addition, until the post-test was performed, the randomization was concealed. The study was approved by the local ethics committee (KNUT IRB -2019-15) and conducted in accordance with the approved guidelines. Written informed consent was obtained from all subjects before inclusion.
SUBJECTS:
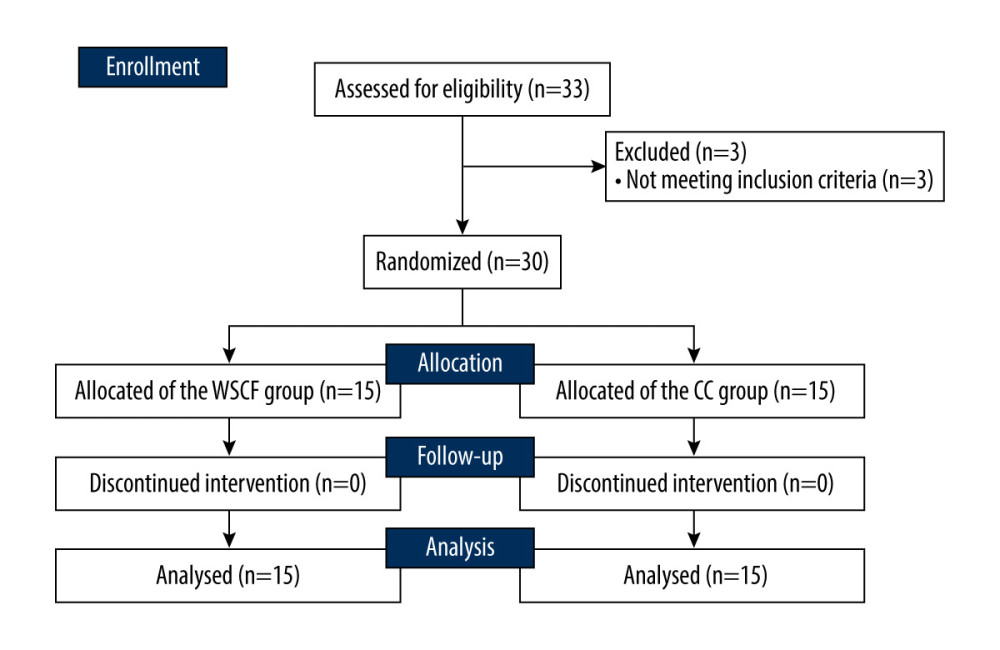
A minimum sample size of 15 participants per group was calculated using a power calculation tool (G*Power 3.1.9.3 software; Heinrich Heine University, Düsseldorf, Germany) with a power and alpha set at 0.80 and 0.05, respectively, and an effect size set at 0.87. Thirty-three stroke patients were recruited to perform this study. We included subjects with (1) residual hemiparesis at least 6 months after the onset of stroke, (2) those with adequate cognitive levels to perform this study (the score of the Korean version of the Mini-Mental State examination ≥24), (3) those who walked using a cane (functional ambulation category 2–3 levels), and (4) those who supported 7% or more of their body weight on a cane [24]. We excluded subjects with (1) a potential musculoskeletal condition that could interfere with safe walking, (2) hemispatial neglect, and (3) severe heart disease or uncontrolled hypertension. Three subjects were excluded because they did not meet the selection criteria (uncontrolled hypertension and MMSE 20 points). Finally, 30 subjects were included and randomly divided into 2 equal groups (Figure 1). The general characteristics of enrolled subjects are described in Table 1.
PROCEDURE:
All subjects participated in standard rehabilitation programs composed of physical and occupational therapy conducted for 4 weeks (5 times per week). Neurodevelopmental treatment was provided in physical therapy, and upper limb functional training for improving daily living performance was performed in occupational therapy. In addition, the subjects from the WSFC group participated in weight support feedback cane gait training conducted for 30 min per day, 3 times per week, for 4 weeks, while the subjects from the CC group participated in conventional cane gait training conducted for 30 min per day, 3 times per week, for 4 weeks. Pre- and post-tests for lower limb muscle activity and gait ability were conducted 1 week before the intervention period and 1 day after the intervention period. Pre- and post-tests were conducted by 3 physical therapists blinded to treatment allocations. In addition, before starting the intervention, cane dependence (average weight support loaded on a cane while walking) was assessed in all subjects during a 20-m walk through a smartphone application connected to the weight support feedback cane via Bluetooth. Average weight support was calculated by dividing the sum of the degree of weight support at each step by the number of steps.
WEIGHT SUPPORT FEEDBACK CANE (WSFC) GAIT TRAINING: WSFC gait training was performed with a WSFC and a smartphone application capable of quantitative measurement of cane dependence during walking (Figure 2). WSFC measured the cane dependence by a load cell located at the bottom of the WSFC handle, and the measured cane dependence was displayed on the WSFC handle and the smartphone application in real time. Based on cane dependence, the subject set a different weight support rate (60% to 30% of cane dependence) for each week. Setting the weight support rate was performed using the smartphone application. If a weight above the preset weight support rate was loaded on the WSFC during gait training, a beeping sound was generated until the weight support loaded on the WSFC was below the preset weight support rate. According to the pilot study on 3 stroke patients and recommendations from clinical experts, the weight support rate loaded on the WSFC was reduced by 10% every week, from 60% (weight support rate in the first week of training) to 30% (weight support rate in the fourth week of training), based on the initial measured cane dependence. During every training session, the gait success rate (the proportion of the number of steps that showed cane dependence below the preset weight bearing rate of the total number of steps in WSFC gait training) was recorded by the smart phone application. When the gait success rate for a week was more than 80%, the weight support rate of the next step (from 60% to 30%) was applied. WSFC gait training was performed at a comfortable speed and the subjects were asked to walk without generating an auditory feedback (beeping sound) as much as possible during WSFC gait training.
CONVENTIONAL CANE (CC) GAIT TRAINING:
The subjects in the CC gait training group participated in gait training using a conventional standard mono cane without auditory feedback (beeping sound) for the same amount of time as those in the WSFC group. The subjects were verbally asked to reduce the weight support loaded on the cane during CC gait training for each week instead of providing auditory feedback according to the set weight support rate. In the first week of CC gait training, subjects were asked to walk at a comfortable speed and 60% of their usual cane dependence; in the following weeks of training, they were asked to walk at their comfortable speed with a reduction in cane dependence to 10% in the last week.
MEASUREMENT:
The affected lower limb muscle activity during the stance phase of the gait cycle was measured using wireless surface electromyography (sEMG). Wireless sEMG electrode attachment was conducted at the 4 major muscles of the affected lower limb (rectus femoris, biceps femoris, medial gastrocnemius, and gluteus medius). Before the start of measurement, the skin hair at the attachment site was removed to avoid skin resistance, and the attachment site was cleaned using an alcohol. Finally, the wireless sEMG electrode was attached in accordance with the direction of muscle fibers. The EMG Analyzer v. 2.9.37.0 (BTS Bioengineering, Milano, Italy) was used to obtain lower limb muscle activity during the stance phase of the gait cycle. To eliminate high-frequency noise, sEMG raw data were filtered at 20–500 Hz. The root mean square values were calculated over a time constant of 50 ms and all values were expressed as% reference voluntary contraction to normalize the sEMG signal. The affected lower limb muscle activity during the stance phase of the gait cycle was measured 3 times, and the average value was used.
To measure gait ability, a 3-axis accelerometer (G-Walk, BTS Bioengineering, Milano, Italy) was used. The 3-axis accelerometer is a portable and wireless system with wearable sensors. The wearable sensor was attached at the first sacrum level of the subjects using a semi-elastic belt. All acceleration data (velocity, cadence, single-limb support phase of the affected side, and symmetry index) were transmitted via Bluetooth to the special software program G-Studio (BTS Bioengineering, Milano, Italy).
STATISTICAL ANALYSIS:
SPSS (version 21.0; IBM Corp., Armonk, NY) was used to conduct statistical analyses. To confirm the normal distribution of all variables, the Shapiro-Wilk test was used. The independent
Results
The general characteristics and baseline clinical assessment of the subjects are summarized in Table 1. No significant differences were observed between the WSFC and CC groups.
Changes in lower limb muscle activity and gait ability after intervention are shown in Table 2. In lower limb muscle activity, both groups showed significant improvements in the rectus femoris (WSFC group: 274.1 to 311.0%RVC, CC group: 247.6 to 273.8%RVC), biceps femoris (WSFC group: 201.3 to 237.8%RVC, CC group: 222.0 to 235.2%RVC), medial gastrocnemius (WSFC group: 224.9 to 279.4%RVC, CC group: 181.4 to 204.8%RVC), and gluteus medius (WSFC group: 204.7 to 261. 7%RVC, CC group: 195.5 to 206.7%RVC, the CC group showed no statistical significance) (
In gait ability, both groups showed significant improvements in velocity (WSFC group: 6.0 to 6.7 m/sec, CC group: 6.7 to 7.1 m/sec), cadence (WSFC group: 65.8 to 71.2 steps/min, CC group: 69.2 to 74.1 steps/min), affected single-limb support phase (WSFC group: 29.0 to 35.4%, CC group: 28.9 to 30.5%) and symmetry index (WSFC group: 75.0 to 84.5, CC group: 77.3 to 82.3) (
Discussion
This study investigated the effect of WSFC gait training, which provides real-time feedback of the user’s weight support loaded on a cane, on lower limb muscle activity and gait ability of stroke patients. As a result, lower limb muscle activity and gait ability were significantly improved in both the WSFC and CC groups who underwent 4 weeks of weight support feedback cane gait training and conventional cane gait training (
Improvement of gait function is an important measure of motor function recovery in stroke [25], and independent gait is an essential factor in increasing the quality of life [7]. Patients with stroke experience reduced muscle activity and gait function due to decreased weight support to the affected lower limb, and a cane is used to improve gait ability or to compensate for decreased gait function in patients with stroke [26]. Several previous studies have reported that proper use of a cane during gait training can induce an increase in weight support to the affected lower limb, thereby improving gait symmetry and stability [11,18,19]. Beauchamp et al reported that cane gait training was effective in improving gait symmetry, velocity, and distance in patients with stroke [27]. In addition, another study reported that the use of a cane was effective in improving the maximum walking distance in patients with stroke [11]. The training protocols used on this study (both WSFC and CC groups) were designed to ensure a gradual decrease in the weight loaded on the cane as cane gait training progressed every week. Such training protocols might have induced functional improvement and weight support to the affected lower limb, as observed in previous studies.
An interesting finding of this study was that the WSFC group showed higher improvement in lower limb muscle activity (rectus femoris and medial gastrocnemius) and gait ability (affected single-limb support phase and symmetry index) compared to the CC group (all
Although this study was a randomized controlled trial sufficiently powered to determine the effect of WSFC gait training on lower limb muscle activity and gait in patients with chronic stroke, it has some limitations. First, the sample size was relatively small and the follow-up period was short; a large randomized controlled trial with a long follow-up period should be conducted for a more accurate analysis of the effects of weight support feedback cane gait training. Second, this study did not consider factors (eg, the extent of the lesion and dominant side) that may have affected functional recovery of stroke. Therefore, the possibility of these factors influencing the study cannot be excluded.
Third, the subjects in the WSFC gait training group participated in WSFC gait training with different weight support rate settings via the load cell located at the bottom of the WSFC handle. However, the CC group subjects were verbally asked to walk at 60%, 50%, 40%, and 30% of their usual cane dependence during CC gait training. The possibility that these differences in accuracy regarding cane dependence could have affected the study findings cannot be excluded. Finally, because the placebo effect was not considered in the CC group, it was difficult to clearly explain the effects of real-time weight support feedback. Thus, further studies considering the placebo effect should be conducted.
Conclusions
This study investigated the effect of weight support feedback cane gait training that provided real-time feedback of the user’s weight support loaded on a cane on lower limb muscle activity and gait ability of patients with stroke. We found that cane gait training could significantly improve lower limb muscle activity and gait ability in patients with stroke by inducing weight support to the affected side regardless of the training method; however, the addition of real-time weight support feedback to cane gait training provided additional benefits compared to conventional cane gait training in stroke patients.
References
1. Members WG, Lloyd-Jones D, Adams RJ, Executive summary: Heart disease and stroke statistics – 2010 update: A report from the American Heart Association: Circulation, 2010; 121; 948-54
2. GBD 2017 Causes of Death Collaborators, Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: A systematic analysis for the Global Burden of Disease Study 2017: Lancet, 2018; 392(10159); 1736-88 [Erratum in: Lancet. 2019;393(10190): e44, Erratum in: Lancet. 2018;392(10160): 2170]
3. Ikai T, Kamikubo T, Takehara I, Dynamic postural control in patients with hemiparesis: Am J Phys Med Rehabil, 2003; 82; 463-69
4. Michael KM, Allen JK, Macko RF, Reduced ambulatory activity after stroke: The role of balance, gait, and cardiovascular fitness: Arch Phys Med Rehabil, 2005; 86; 1552-56
5. Shumway-Cook A, Woollacott MH: Motor control: translating research into clinical practice, 2007, Lippincott Williams & Wilkins
6. Choi EP, Yang SJ, Jung AH, Na HS, Changes in lower limb muscle activation and degree of weight support according to types of cane-supported gait in hemiparetic stroke patients: Biomed Res Int, 2020; 2020 9127610
7. Schmid A, Duncan PW, Studenski S, Improvements in speed-based gait classifications are meaningful: Stroke, 2007; 38; 2096-100
8. Sung Y-H, Kim C-J, Yu B-K, A hippotherapy simulator is effective to shift weight bearing toward the affected side during gait in patients with stroke: NeuroRehabilitation, 2013; 33; 407-12
9. Chen C-L, Chen H-C, Tang SF-T, Gait performance with compensatory adaptations in stroke patients with different degrees of motor recovery: Am J Phys Med Rehabil, 2003; 82; 925-35
10. Martins CP, Rodrigues EdC, Pedron CA, Feasibility of a task-oriented training and muscle-strengthening programme to weight-bearing symmetry after stroke: Eur J Physiother, 2017; 19; 160-66
11. Allet L, Leemann B, Guyen E, Effect of different walking aids on walking capacity of patients with poststroke hemiparesis: Arch Phys Med Rehabil, 2009; 90; 1408-13
12. Buurke J, Hermens HJ, Erren-Wolters C, The effect of walking aids on muscle activation patterns during walking in stroke patients: Gait Posture, 2005; 22; 164-70
13. Laufer Y, The effect of walking aids on balance and weight-bearing patterns of patients with hemiparesis in various stance positions: Phys Ther, 2003; 83; 112-22
14. Kaye HS, Kang T, LaPlante MP, Mobility device use in the United States: Disability Statistics Report 14, 2000
15. Polese JC, Nascimento LR, Faria CDCdMPerception of patients with chronic hemiplegia regarding the use of assistive walking devices: Rev Panam Salud Publica, 2011; 30; 204-8 [in Portuguese]
16. Guillebastre B, Rougier PR, Sibille B, When might a cane be necessary for walking following a stroke?: Neurorehabil Neural Repair, 2012; 26; 173-77
17. Park K: The effects of methods of using assist devices on weight bearing, balance, ambulation in hemiplegic patients [dissertation], 2013, Seoul, Korea University
18. Boonsinsukh R, Panichareon L, Phansuwan-Pujito P, Light touch cue through a cane improves pelvic stability during walking in stroke: Arch Phys Med Rehabil, 2009; 90; 919-26
19. Polese JC, Teixeira-Salmela LF, Nascimento LR, The effects of walking sticks on gait kinematics and kinetics with chronic stroke survivors: Clin Biomech, 2012; 27; 131-37
20. Bateni H, Maki BE, Assistive devices for balance and mobility: Benefits, demands, and adverse consequences: Arch Phys Med Rehabil, 2005; 86; 134-45
21. Son S-M, Choi Y-W, Kim C-S, Effect of motor functions of ipsilateral upper limb induced by long-term cane usage in chronic stroke patients: J Kor Phys Ther, 2012; 24; 151-56
22. Kang YS, Cho KH, Changes in lower limb muscle activation and gait function according to cane dependence in chronic stroke patients: Technol Health Care, 2021; 29; 133-41
23. Arefin P, Habib MS, Arefin A, A review on current mechanical and electronic design aspects and future prospects of smart canes for individuals with lower limb difficulties: Mat Sci Res India, 2020; 17; 25-33
24. Chen C-L, Chen H-C, Wong M-K, Temporal stride and force analysis of cane-assisted gait in people with hemiplegic stroke: Arch Phys Med Rehabil, 2001; 82; 43-48
25. Patterson KK, Gage WH, Brooks D, Evaluation of gait symmetry after stroke: A comparison of current methods and recommendations for standardization: Gait Posture, 2010; 31; 241-46
26. Den Otter A, Geurts A, Mulder T, Gait recovery is not associated with changes in the temporal patterning of muscle activity during treadmill walking in patients with post-stroke hemiparesis: Neurophysiol Clin, 2006; 117; 4-15
27. Beauchamp MK, Skrela M, Southmayd D, Immediate effects of cane use on gait symmetry in individuals with subacute stroke: Physiother Can, 2009; 61; 154-60
28. Jung K, Kim Y, Cha Y, Effects of gait training with a cane and an augmented pressure sensor for enhancement of weight bearing over the affected lower limb in patients with stroke: A randomized controlled pilot study: Clin Rehabil, 2015; 29; 135-42
29. Sungkarat S, Fisher BE, Kovindha A, Efficacy of an insole shoe wedge and augmented pressure sensor for gait training in individuals with stroke: A randomized controlled trial: Clin Rehabil, 2011; 25; 360-69
30. Batavia M, Gianutsos JG, Kambouris M, An augmented auditory feedback device: Arch Phys Med Rehabil, 1997; 78; 1389-92
Figures
Tables
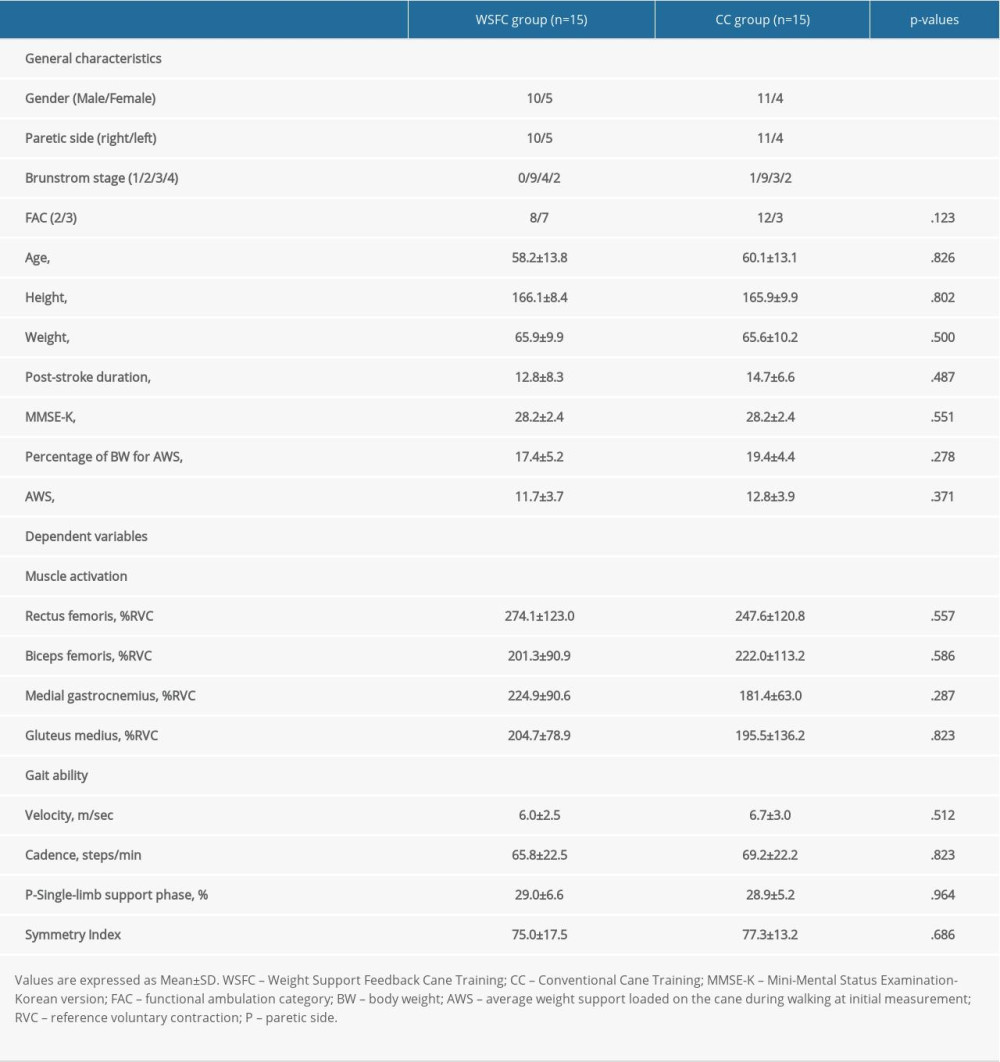 Table 1. Homogeneity test for general characteristics and dependent variables of the subjects (N=30).
Table 1. Homogeneity test for general characteristics and dependent variables of the subjects (N=30).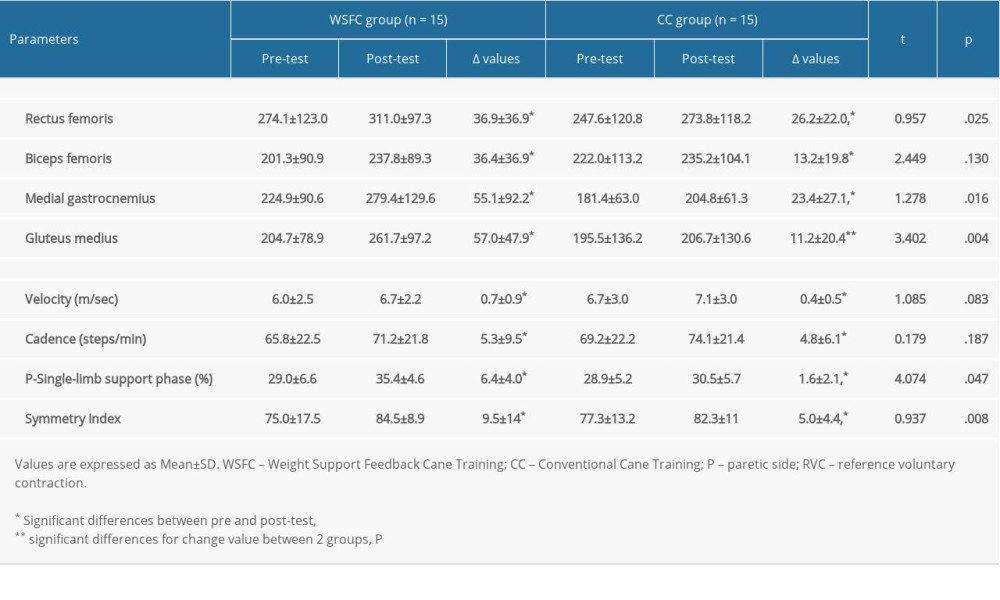 Table 2. Changes of lower limb muscle activity and gait ability (N=30).
Table 2. Changes of lower limb muscle activity and gait ability (N=30). Table 1. Homogeneity test for general characteristics and dependent variables of the subjects (N=30).
Table 1. Homogeneity test for general characteristics and dependent variables of the subjects (N=30). Table 2. Changes of lower limb muscle activity and gait ability (N=30).
Table 2. Changes of lower limb muscle activity and gait ability (N=30). In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952