25 May 2021: Clinical Research
Outcomes from Osteochondral Autograft Transplant or Mosaicplasty in 26 Patients with Type V Osteochondral Lesions of the Talus
Lei Zhang1234ABCDEFG, Yuxi Luo5ABCDEF, Xin Zhou123ABD, Shijie Fu123ABF, Guoyou Wang123ABF*DOI: 10.12659/MSM.930527
Med Sci Monit 2021; 27:e930527
Abstract
BACKGROUND: Mosaicplasty osteochondral transplantation (MOT) has been proved a feasible choice for the treatment of talus osteochondral injury. It can reduce ankle pain and allow performance of daily living activities and elementary sports. However, there are very little data on the restoration of normal life with large lesions. Our investigation focused on assessing outcomes in patients with large lesions.
MATERIAL AND METHODS: The MOT operation was used, and the donor site was located at the lateral condyle of the femur. Clinical evaluation included the Berndt and Harty outcome question, Visual Analog Scale (VAS) pain score (during rest, walking and running), American Orthopedic Foot and ankle Association (AOFAS) score, International Knee Documentation Committee (IKDC) subjective knee evaluation form, and the Short Form 36 (SF-36). Twenty-four months after surgery, the graft binding was assessed by MRI using the magnetic resonance observation of cartilage repair tissue (MOCART) score.
RESULTS: We assessed 26 patients, including 14 males and 12 females. The average follow-up time was 33.9±5.2 months. The average lesion size was 173.1±23.5 mm². The average VAS score during rest improved from 4.62±0.85 preoperatively to 1.08±0.27 postoperatively (P<0.05), the score during walking improved from 5.19±0.63 preoperatively to 1.15±0.37 postoperatively (P<0.05), and the score during running improved from 6.08±0.74 preoperatively to 1.39±0.57 postoperatively (P<0.05). The average postoperative AOFAS ankle score improved to 91.5±2.6 (range, 88 to 96), compared with preoperative 75.0±2.8 (range, 70 to 79) (P<0.05). Two patients developed pain in the donor site of the knee joint, and both of them had 2 or more osteochondral plugs harvested. The postoperative SF-36 score increased to 92.2±2.4 (P<0.05). In the last follow-up, 18 patients answered the Berndt and Harty outcome question, all with “good” as the result.
CONCLUSIONS: MOT is a feasible choice for patients with larger lesions. It can improve the VAS/AOFAS/IKDC/SF-36 scores, and has high patient satisfaction. Graft incorporation helps improve patient quality of life. Our results indicate that a larger osteochondral plug area increases the risk of developing knee donor site pain.
Keywords: Cartilage Diseases, Talus, Transplantation, Autologous, Bone Transplantation, Quality of Life
Background
Ankle injuries often lead to osteochondral lesion of the talus (OLT), and 50% of OLTs occur from ankle sprains and fractures [1]. OLTs may occur when an ankle sprain or fracture causes the talar dome to hit the distal tibia plafond [2]. Although the incidence rate is relatively low, in most cases, it is necessary to heal the cartilage and osteochondral talus injury because it has a great influence on daily life, particularly in young people and those who wish to actively participate in sports [3]. Indeed, nondisplaced cartilage lesions were often treated with a nonoperative approach, and symptomatic injuries were surgically treated [4–6]. The success rate of surgical treatment is higher after a period of non-surgical treatment [7]. In 1959, Berndt and Harty defined in detail osteochondritis dissecans of the talus and considered osteochondral fracture was caused by trauma [8]. Previous studies include post-traumatic defects, osteochondritis, vascular necrosis, and osteoarthritis [7].
There are various clinical techniques to choose from in treating OLT. One of the options is a traditional conservative nonoperative treatment [9]. Patients who were symptomatic, failing nonoperative treatment, or with acute avulsion debris should receive operative treatment, including bone marrow stimulation, internal fixation, autologous bone or osteochondral grafting, and biological adjuncts to cartilage repair [4,10]. However, some osteotomy and orthopedic treatments have the risk of fracture nonunion, allogeneic cartilage transplantation has the risk of rejection and infection, and the efficacy of biological adjuncts for bone cysts is not yet clear, so MOT can be a relatively good choice.
Mosaicplasty osteochondral grafting is commonly used in patients with OLT of the ankle joint with a large lesion area (>150 mm2). However, some studies have reported poor results when the lesion area is larger than 150 mm2 [11]. Several cylindrical osteochondral grafts are taken from the non-weight-bearing region of the autogenous joint, and then are pressed into the repaired cartilage defects. In 2009, Raikin [12] reported successful results of fresh allogeneic osteochondral transplantation in treatment of large talus cystic lesions. Scranton, McDermott [11], and Hangody et al [14] used autologous osteochondral transplantation to treat talus cartilage injuries and achieved very good clinical results. The success rate of the former reached 90%, and the success rate of the latter reached 94%. During the follow-up of 62.8 months, 87.4% of the patients had good or excellent outcomes in a new meta-analysis of autogenous osteochondral transplantation (AOT) procedures, which showed clear improvement in AOFAS score [15].
The shortcoming of non-osteochondral grafting is that it achieves poorer biomechanical results and takes a long time to repair [16–18]. However, mosaicplasty osteochondral grafts can be performed under arthroscopy without a secondary operation, and the repaired tissue is more similar to normal hyaline cartilage. At present, the limitations mainly include donor site injury, a limited area, the number of grafts, and differences in orientation, thickness, and biomechanical characteristics between donor and recipient cartilage. In previous studies, a potential confounding factor was the significant change of lesion size treated by AOT, and the analysis usually includes injury area less than 150 mm2 [11,15].
At present, there is little information on results of MOT in treatment of large OLTs. The purpose of the present study was to ascertain whether a MOT is a better way to restore activities of daily living in patients with lesions greater than 150 mm2, including short-term and long-term effects.
Material and Methods
MATERIALS:
This study was approved by the Ethics Committee of the Affiliated Traditional Chinese Medicine Hospital of Southwest Medical University (No. KY2019043). We reviewed 26 cases who had received treatment by mosaicplasty osteochondral grafting for OLT between 2016 and 2018, and in whom the lesion size was at least 150 mm2. Exclusion criteria included history of joint infection, degenerative joint disease, and inflammatory joint disease. The lesion size was gauged by magnetic resonance imaging (MRI) or previous arthroscopy. There were 14 males and 12 females, and the average age was 45.9±9.7 years. There were 12 left ankle injuries and 14 right ankle injuries. The mean duration of symptoms before operation was 13.8±4.8 years (range, 7 months to 2 years). Details of the 26 patients with osteochondral defects of the talus are provided in Table 1. Preoperative assessment of cartilage lesions was performed with X-ray and MRI. With the numbers available, no significant differences could be detected.
We used the anatomic talus „9-zone” grid scheme to categorize lesion location [19]. This is classified according to the direct visual examination during the operation. Multiple zones were recorded when lesions were large enough. The great majority of lesions in our patients were situated in “Zone 4” (medial and middle), which was most often affected.
OPERATIVE TECHNIQUE:
Under neuronal block anesthesia, the patient was placed supine, and an upper thigh gas capsule hemostatic band was installed on the affected limb with 40 kPa pressure. The medial arc incision extended from the middle of the medial malleolus to the proximal end of the medial malleolus and extended for 4–5 cm, and the joint capsule incision was cut from the anterior edge of the medial malleolus layer by layer. Medial malleolar osteotomy was used to flip the medial malleolus bone mass and expose the medial lesion area of the talus (Figure 1) to identify the cartilage lesion area. We used a micro bone knife and curette to clean the cavity. Additional drilling was performed on the subchondral bone layer for cyst debridement, and we measured and recorded the length, width, and depth of the cyst. The special instrument was placed in the upper edge of the lateral patellar joint of the femoral condyle, then entered into the condyle of the femur, and the graft was removed. The depth and method of the material collection were consistent with those of the recipient area, and grafts were 2 mm larger than the surrounding cartilage. We aimed to put the graft beneath the cartilage layer. The defect was filled by implantation of the recipient’s talus. After insertion of plugs, the ankle joint range of motion was examined to ensure good and stable graft implantation. Then, we reduced the internal ankle joint and 2 hollow screws were used to fix it. After washing, the incision was sutured layer by layer, and the aseptic excipients were bandaged under pressure.
POSTOPERATIVE REHABILITATION:
Postoperative rehabilitation included precautions against infection and possible inflammation, restoring the normal ankle range of motion, increasing muscle power, improving nerve control of muscle activity, and passive ankle flexion and extension exercise. The ultimate purpose was to achieve proprioceptive recovery and allow the patient to resume normal activities of daily living. The ankle was not loaded for 3 weeks. Simple passive ankle movement and physical therapy were performed between the third and sixth weeks. Six weeks after surgery, partial weightbearing exercises of the ankle joint were started, and complete loading was permitted after 8 weeks. Clinical examination and continuous X-ray examination were performed 5 and 10 weeks after the operation. We also used radiography to review graft placement and the malleolar osteotomy.
CLINICAL OUTCOME MEASURES:
We used the Berndt and Harty outcome questions to pre-evaluate the subjective patient outcomes at a primary stage [8]. The clinical outcome measures were the VAS pain score (during rest, walking and running) and the AOFAS score. The functional outcome was obtained for the knee using the IKDC subjective knee evaluation form and the IKDC objective knee examination form [20]. The Short Form 36 (SF-36) [10] was used to assess quality of life. We recorded information on all complications and other surgical processes, including infection, the second surgery, and the development of knee pain at the donor site.
The answer to Berndt and Harty’s outcome question was combined with 3 conditions; the patient classified the ankle as good, fair, or poor [8]. VAS pain score is a scale of 0–10 points, one end of the horizontal line is 0, indicating no pain; the other end is 10, indicating severe pain. The AOFAS score is a combination of objective and subjective clinical scoring systems that ranges from 1 to 100 and it was subdivided into 3 categories: pain (40 scores), function (50 scores), and alignment (10 scores). It is the most commonly used evaluation in foot and ankle treatment. The SF-36 is a well-known and widely recognized result index for evaluating quality of life [19]. It consists of 2 parts; one is a physical component scale and the other is the mental component scale. When the following conditions occur, it indicates the failure of the operation: the pain did not gradually relieve or became more serious during the follow-up after the operation, the AOFAS score did not increase significantly or decreased during the follow-up, imaging observation of long-term poor fusion of the transplantation site and severe local edema, postoperative infection, or free graft, causing secondary damage.
RADIOGRAPHIC EVALUATION:
X-ray and MRI were used to assess defect size and to evaluate the healing and consistency of osteotomy reduction and internal fixation after the operation (Figures 2, 3). MRI was used when the CT scans were unable to show the defect. Both X-ray and MRI showed good results (Figure 3).
STATISTICAL ANALYSIS:
Results are expressed as the mean±standard deviation (SD). Statistical analysis was performed using SPSS. The paired samples
Results
Within the timeline of this study, 26 people underwent MOT for their OLTs. The subjects consisted of 14 males (53.8%) and 12 females (46.2%). The left talus was involved in 12 patients (46.2%) and the right talus in 14 patients (53.8%). Average follow-up time was 33.9±5.2 months (range, 28 to 48 months). The mean duration of symptoms to surgery was 13.8±4.8 months. The Berndt and Harty clinical outcome after AOT was good in 18 cases (69.2%) and fair in 8 cases (30.8%) (Table 2). The mean lesion size was 173.1±23.5 mm2 (range, 150–230 mm2). Before MOT, 22 (84.6%) patients had previously undergone surgery, including conservative treatment, microfracture, and ligament reconstruction. A mean of 1 plug was used at surgery. In most patients, 1 osteochondral plug was implanted (23 cases; 88.5%), with 3 patients having 2 or more osteochondral plugs harvested. No patients underwent additional operations.
Table 3 shows the AOFAS score, VAS score, IDKC score, and SF-36 score. The average postoperative AOFAS ankle score improved to 91.5±2.6 (range, 88 to 96), compared with preoperative score 75.0±2.8 (range, 70 to 79). The ankle score of patients with large transplanted cartilage area was poor. The VAS scores during rest improved from 4.62±0.85 preoperatively to 1.08±0.27 postoperatively (P<0.05), during walking they improved from 5.19±0.63 preoperatively to 1.15±0.37 postoperatively (P<0.05), and during running they improved from 6.08±0.74 preoperatively to 1.39±0.57 postoperatively. Last follow-up IDKC score was 97±0.98 (range, 96 to 98).
In this study of patients, the average SF-36 physical and mental composition scale was within the normal range of the Dutch population [21]. During an average of 24 months of follow-up, 4 (15.3%) of the 26 patients had radiographs showing elevated plugs in the ankle joint plane. Postoperative radiographs were available for the other 22 (84.7%) patients and demonstrated that all grafts and osteotomies healed. In addition, there is no evidence of grafts sinking. Of 26 patients, 18 patients (69.2%) reported postoperative imaging results. However, only 5 patients (19.2%) underwent follow-up assessment using MRI (Figure 3). Two patients reporting MRI results were systematically assessed using MOCART score, and the weighted mean score of MOCART was 75±5.5 (range, 73.1–86.7).
No infection or wound healing problems required additional operations. Two patients (7%) required ankle arthroscopy at the subsequent stage. Two patients (7%) had donor site morbidity of the knee. The increase of patients’ age is related to the poor knee joint score after the operation. The knee score of patients over 40 years old was 96, and that of patients under 30 years old was 98 (
Discussion
The notable result of the current research was that the MOT surgery has been proven to have good results in those who had large osteochondral lesions and wanted to get back to a normal activity. Our rate was similar to a study by Al-Shaikh RA et al [22] evaluating AOT in 2002. The study reviewed 19 patients, including 6 males and 13 females, with follow-up of 16 months. The authors recorded a meaningful improvement in AOFAS scores. In that study, 73.7% of the donor sites were fully functional, and 36.8% had postoperative morbidity. It is worth noting that the talus injury size in this research was smaller than in our study, with an average size 120 mm2 of the lesion, compared with our mean lesion size of 173.1 mm2. However, short-term follow-up outcomes were reported in the majority of studies. In 2018, Shimozono et al [23] reported that autologous osteochondral transplantation surgery gave exceptional results and significantly increased the score of clinical results, with a mean follow-up time of 62.8 months. Excellent and good clinical outcomes were reported in 87.4% of those patients.
There are many clinical methods used to treat talus cartilage injury. The choice of method depends on many factors, including the talus lesion size and stability of the injury, the continuity of the cartilage surface, and the condition of the damaged surrounding talus [24], and different lesion sizes need different treatment methods. In 2016, Guney et al [25] found that the mosaicplasty technique is a little better than the microfracture technique. Hangody et al [26] suggested mosaicplasty was better than drilling, microfracture surgery, or abrased arthroplasty, and this treatment has been widely used. Hangody et al developed the mosaicplasty method, using a cylindrical osteochondral graft removed from the lateral condyle of the femur, then implanting the bone plug in the focus area, thus implanting the spongy bone and the hyaline cartilage at the same time to repair the subchondral depression. This ensures that it has the function of hyaline cartilage. In this research, 2 patients experienced persistent donor site pain after surgery, although these patients did not have lateral femoral condylar arthritis. In our patients, malleolar osteotomy provided good operative exposure and improved operative manipulation, which helps the recovery of ankle biomechanics.
Our study documented donor site morbidity in 2 of 26 patients (7.7%), which is similar to the rates of 5.2% to 8.8% reported in the literature [15]. The patients who had 2 or more plug grafts experienced higher donor site morbidity. We treated 3 patients with 2 or more plug grafts; 1 patient had postoperative knee pain and 1 patient only had pain during running. That was consistent with a report that 2 or more plugs results in higher donor site morbidity [9]. Another study, by Kolker et al, reported significant outcomes [27]. The average lesion size in this group was smaller (170×10 millimeter) than in our research. In general, the knees obtained excellent results using the Cincinnati and HSS Knee Scale.
Although, some reports suggested that mosaicplasty was applicable for the transplantation of smaller surface areas and, it might be related to higher scores in knees and ankles. Also, large talus defects (greater than 150 mm2) tended to do poorly in natural. We did find excellent outcomes in MOCART scores and AOFAS scores. It was noticed that graft incorporation played an important part in higher ankle scores. In the present study, we use concentrated bone marrow aspirate to improve local biology, which has been proved to improve the integration of magnetic resonance images of MOT [28]. In our study, we believe this technique would help those patients to obtain higher functional outcomes and to speed to back to their normal life.
Furthermore, our study had a long period of symptoms before recopied AOT surgery (average 13.8 months). So many patients failed in no surgery treatment that led to a sclerotic talus bone surrounding the lesion which might show in the MRI. Therefore, these patients might have extensive blood vessels in the area, and simply drilling might not create enough blood flow. However, removing the hardened bone bolt of subchondral bone hemorrhage may establish the necessary blood vessels [26]. Our rate was the equivalent to that of previous reports. This might explain why large OLTs can have high ankle scores. With aging, knee results become worse and donor sites have more morbidity.
This study has certain limitations. The sample size was small, there were some measurement errors, the follow-up period was short, we used an unanchored pain scale, and the study design was retrospective. Further comparative studies would help to define the benefits of this procedure.
Conclusions
In conclusion, our study found that MOT was a valid procedure of treating large OLTs. It demonstrated good clinical and functional outcomes, including short-term and long-term effects, and, most importantly, helped patients resume normal activities.
Figures
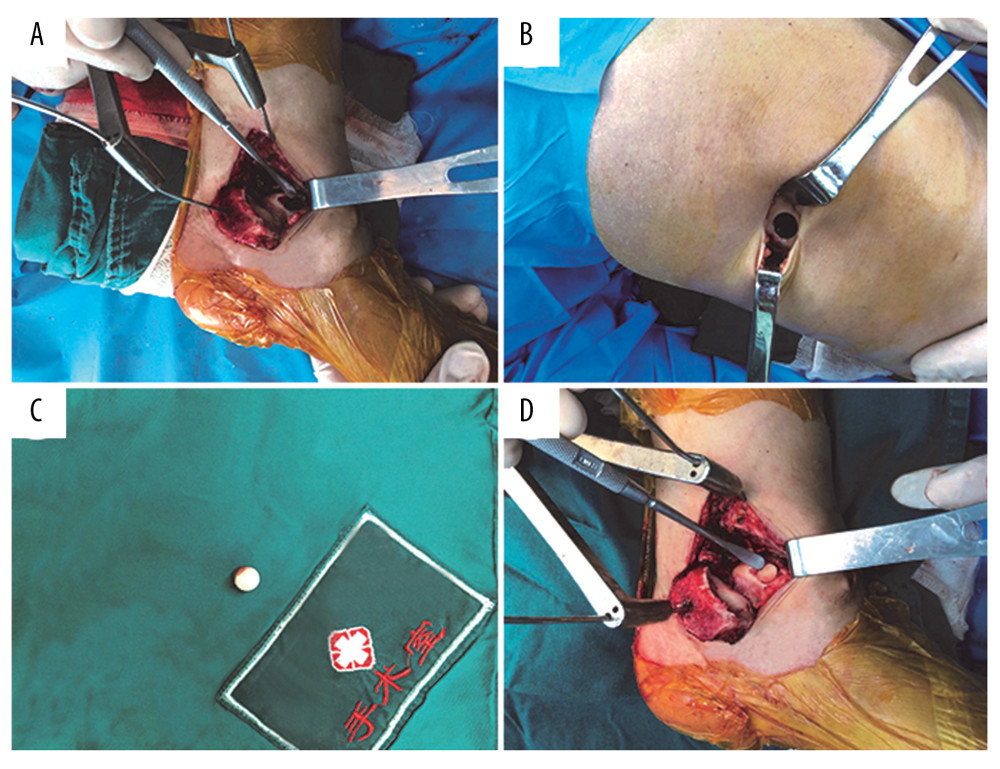 Figure 1. Surgical process. Medial malleolar osteotomy for exposure of posteromedial OCD talar lesion, cleanup subchondral cysts (A), the lesion size was 160 mm2. Lateral knee arthrotomy exposing the trochlear border of the lateral femoral condyle after removal of the osteochondral plug (B). Removal of the osteochondral plug (C). The plug size was 155 mm2. We implanted the osteochondral plug into the talar lesion, and osteochondral plug surface is flush with the talar articular cartilage (D).
Figure 1. Surgical process. Medial malleolar osteotomy for exposure of posteromedial OCD talar lesion, cleanup subchondral cysts (A), the lesion size was 160 mm2. Lateral knee arthrotomy exposing the trochlear border of the lateral femoral condyle after removal of the osteochondral plug (B). Removal of the osteochondral plug (C). The plug size was 155 mm2. We implanted the osteochondral plug into the talar lesion, and osteochondral plug surface is flush with the talar articular cartilage (D). 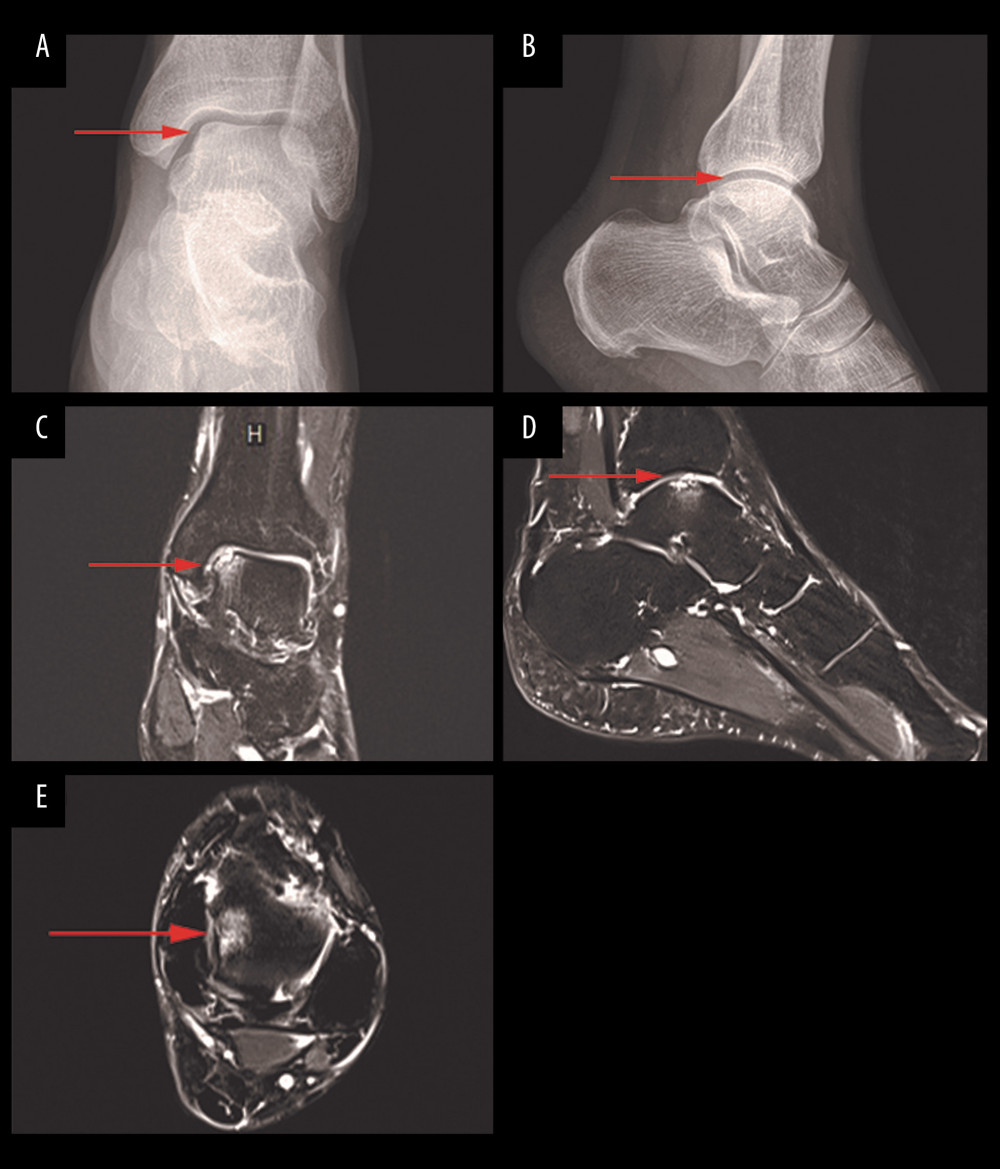 Figure 2. Preoperative X-ray and MRI showing talar cartilage damage. Anteroposterior (A) and lateral (B) ankle radiograph of the ankle. The radiograph demonstrated an incomplete articular surface (arrow). Coronal position (C), sagittal position (D), and transection (E) ankle MRI of the ankle demonstrated osteochondral lesion on the medial talar dome (arrow).
Figure 2. Preoperative X-ray and MRI showing talar cartilage damage. Anteroposterior (A) and lateral (B) ankle radiograph of the ankle. The radiograph demonstrated an incomplete articular surface (arrow). Coronal position (C), sagittal position (D), and transection (E) ankle MRI of the ankle demonstrated osteochondral lesion on the medial talar dome (arrow). 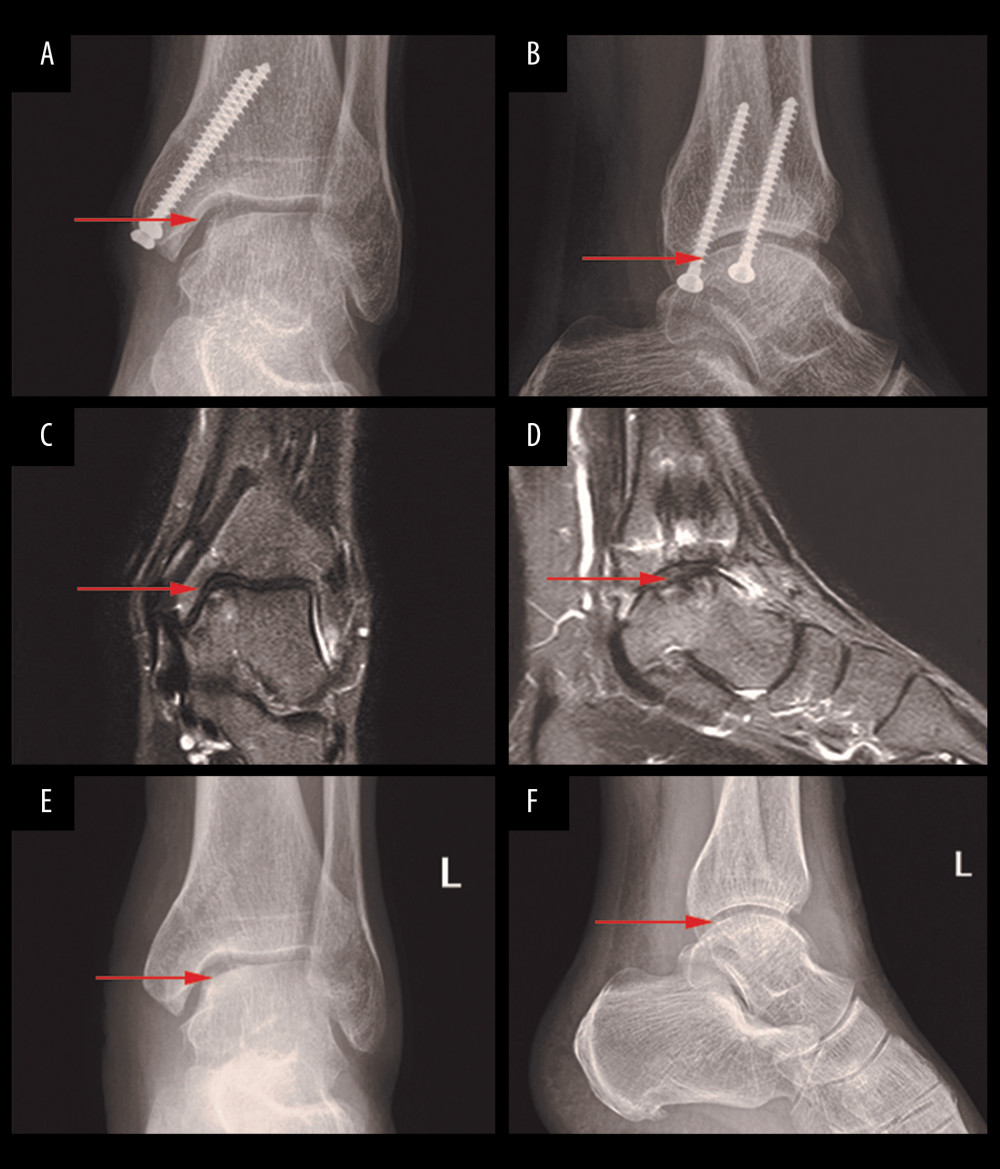 Figure 3. Postoperative X-ray and 24-month follow-up MRI and X-ray. Anteroposterior (A) and lateral (B) ankle radiographs of the ankle 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow). The radiographs demonstrated an almost healed osteotomy and intact graft. At the same time, MRI of the ankle Coronal position (C), sagittal position (D) 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow), and the edema had almost disappeared. The anteroposterior (E) and lateral (F) X-ray images of ankle joint after internal fixation was taken out.
Figure 3. Postoperative X-ray and 24-month follow-up MRI and X-ray. Anteroposterior (A) and lateral (B) ankle radiographs of the ankle 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow). The radiographs demonstrated an almost healed osteotomy and intact graft. At the same time, MRI of the ankle Coronal position (C), sagittal position (D) 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow), and the edema had almost disappeared. The anteroposterior (E) and lateral (F) X-ray images of ankle joint after internal fixation was taken out. References
1. Hintermann B, Regazzoni P, Lampert C, Arthroscopic findings in acute fractures of the ankle: J Bone Joint Surg Br, 2000; 82(3); 345-51
2. Kerkhoffs GMMJ, Karlsson J, Osteochondral lesions of the talus: Knee Surg Sports Traumatol Arthrosc, 2019; 27(9); 2719-20
3. López-Alcorocho JM, Guillén-Vicente I, Rodríguez-Iñigo E, High-density autologous chondrocyte implantation as treatment for ankle osteochondral defects: Cartilage, 2019 [Online ahead of print]
4. Looze CA, Capo J, Ryan MK, Evaluation and management of osteochondral lesions of the talus: Cartilage, 2017; 8(1); 19-30
5. Akpancar S, Gül D, Comparison of platelet rich plasma and prolotherapy in the management of osteochondral lesions of the talus: A retrospective cohort study: Med Sci Monit, 2019; 25; 5640-47
6. Beck S, Claßen T, Haversath M, Operative technique and clinical outcome in endoscopic core decompression of osteochondral lesions of the talus: A pilot study: Med Sci Monit, 2016; 22; 2278-83
7. Reilingh ML, Kerkhoffs GM, Telkamp CJ, Treatment of osteochondral defects of the talus in children: Knee Surg Sports Traumatol Arthrosc, 2014; 22(9); 2243-49
8. Berndt AL, Harty M, Transchondral fractures (osteochondritis dissecans) of the talus: J Bone Joint Surg Am, 1959; 41-A; 988-1020
9. Badekas T, Takvorian M, Souras N, Treatment principles for osteochondral lesions in foot and ankle: Int Orthop, 2013; 37(9); 1697-706
10. Ware JE, Gandek B, Overview of the SF-36 Health Survey and the International Quality of Life Assessment (IQOLA) Project: J Clin Epidemiol, 1998; 51(11); 903-12
11. Kennedy JG, Murawski CD, The treatment of osteochondral lesions of the talus with autologous osteochondral transplantation and bone marrow aspirate concentrate: Surgical technique: Cartilage, 2011; 2(4); 327-36
12. Raikin SM, Fresh osteochondral allografts for large-volume cystic osteochondral defects of the talus: J Bone Joint Surg Am, 2009; 91(12); 2818-26
13. Scranton PE, McDermott JE, Treatment of type V osteochondral lesions of the talus with ipsilateral knee osteochondral autografts: Foot Ankle Int, 2001; 22(5); 380-84
14. Hangody L, Kish G, Módis L, Mosaicplasty for the treatment of osteochondritis dissecans of the talus: Two to seven year results in 36 patients: Foot Ankle Int, 2001; 22(7); 552-58
15. Hurley ET, Murawski CD, Paul J, Osteochondral autograft: Proceedings of the International Consensus Meeting on Cartilage Repair of the Ankle: Foot Ankle Int, 2018; 39(1 Suppl); 28S-34S
16. Komárek J, Vališ P, Repko MTreatment of deep cartilage defects of the knee with autologous chondrocyte transplantation: Long-term results: Acta Chir Orthop Traumatol Cech, 2010; 77(4); 291-95 [in Czech]
17. Solheim E, Hegna J, Strand T, Randomized study of long-term (15–17 years) outcome after microfracture versus mosaicplasty in knee articular cartilage defects: Am J Sports Med, 2018; 46(4); 826-31
18. Wang D, Chang B, Coxe FR, Clinically meaningful improvement after treatment of cartilage defects of the knee with osteochondral grafts: Am J Sports Med, 2019; 47(1); 71-81
19. Elias I, Zoga AC, Morrison WB, Osteochondral lesions of the talus: Localization and morphologic data from 424 patients using a novel anatomical grid scheme: Foot Ankle Int, 2007; 28(2); 154-61
20. Hefti F, Müller W, Jakob RP, Stäubli HU, Evaluation of knee ligament injuries with the IKDC form: Knee Surg Sports Traumatol Arthrosc, 1993; 1(3–4); 226-34
21. Aaronson NK, Muller M, Cohen PD, Translation, validation, and norming of the Dutch language version of the SF-36 Health Survey in community and chronic disease populations: J Clin Epidemiol, 1998; 51(11); 1055-68
22. Al-Shaikh RA, Chou LB, Mann JA, Autologous osteochondral grafting for talar cartilage defects: Foot Ankle Int, 2002; 23(5); 381-89
23. Shimozono Y, Hurley ET, Myerson CL, Kennedy JG, Good clinical and functional outcomes at mid-term following autologous osteochondral transplantation for osteochondral lesions of the talus: Knee Surg Sports Traumatol Arthrosc, 2018; 26(10); 3055-62
24. Browne JE, Branch TP, Surgical alternatives for treatment of articular cartilage lesions: J Am Acad Orthop Surg, 2000; 8(3); 180-89
25. Guney A, Yurdakul E, Karaman I, Medium-term outcomes of mosaicplasty versus arthroscopic microfracture with or without platelet-rich plasma in the treatment of osteochondral lesions of the talus: Knee Surg Sports Traumatol Arthrosc, 2016; 24(4); 1293-98
26. Hangody L, Ráthonyi GK, Duska Z, Autologous osteochondral mosaicplasty. Surgical technique: J Bone Joint Surg Am, 2004; 86-A(Suppl 1); 65-72
27. Gautier E, Kolker D, Jakob RP, Treatment of cartilage defects of the talus by autologous osteochondral grafts: J Bone Joint Surg Br, 2002; 84(2); 237-44
28. Kumai T, Takakura Y, Higashiyama I, Tamai S, Arthroscopic drilling for the treatment of osteochondral lesions of the talus: J Bone Joint Surg Am, 1999; 81(9); 1229-35
Figures
 Figure 1. Surgical process. Medial malleolar osteotomy for exposure of posteromedial OCD talar lesion, cleanup subchondral cysts (A), the lesion size was 160 mm2. Lateral knee arthrotomy exposing the trochlear border of the lateral femoral condyle after removal of the osteochondral plug (B). Removal of the osteochondral plug (C). The plug size was 155 mm2. We implanted the osteochondral plug into the talar lesion, and osteochondral plug surface is flush with the talar articular cartilage (D).
Figure 1. Surgical process. Medial malleolar osteotomy for exposure of posteromedial OCD talar lesion, cleanup subchondral cysts (A), the lesion size was 160 mm2. Lateral knee arthrotomy exposing the trochlear border of the lateral femoral condyle after removal of the osteochondral plug (B). Removal of the osteochondral plug (C). The plug size was 155 mm2. We implanted the osteochondral plug into the talar lesion, and osteochondral plug surface is flush with the talar articular cartilage (D). Figure 2. Preoperative X-ray and MRI showing talar cartilage damage. Anteroposterior (A) and lateral (B) ankle radiograph of the ankle. The radiograph demonstrated an incomplete articular surface (arrow). Coronal position (C), sagittal position (D), and transection (E) ankle MRI of the ankle demonstrated osteochondral lesion on the medial talar dome (arrow).
Figure 2. Preoperative X-ray and MRI showing talar cartilage damage. Anteroposterior (A) and lateral (B) ankle radiograph of the ankle. The radiograph demonstrated an incomplete articular surface (arrow). Coronal position (C), sagittal position (D), and transection (E) ankle MRI of the ankle demonstrated osteochondral lesion on the medial talar dome (arrow). Figure 3. Postoperative X-ray and 24-month follow-up MRI and X-ray. Anteroposterior (A) and lateral (B) ankle radiographs of the ankle 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow). The radiographs demonstrated an almost healed osteotomy and intact graft. At the same time, MRI of the ankle Coronal position (C), sagittal position (D) 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow), and the edema had almost disappeared. The anteroposterior (E) and lateral (F) X-ray images of ankle joint after internal fixation was taken out.
Figure 3. Postoperative X-ray and 24-month follow-up MRI and X-ray. Anteroposterior (A) and lateral (B) ankle radiographs of the ankle 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow). The radiographs demonstrated an almost healed osteotomy and intact graft. At the same time, MRI of the ankle Coronal position (C), sagittal position (D) 24 months after OATS procedure for an osteochondral lesion of the medial talus (arrow), and the edema had almost disappeared. The anteroposterior (E) and lateral (F) X-ray images of ankle joint after internal fixation was taken out. Tables
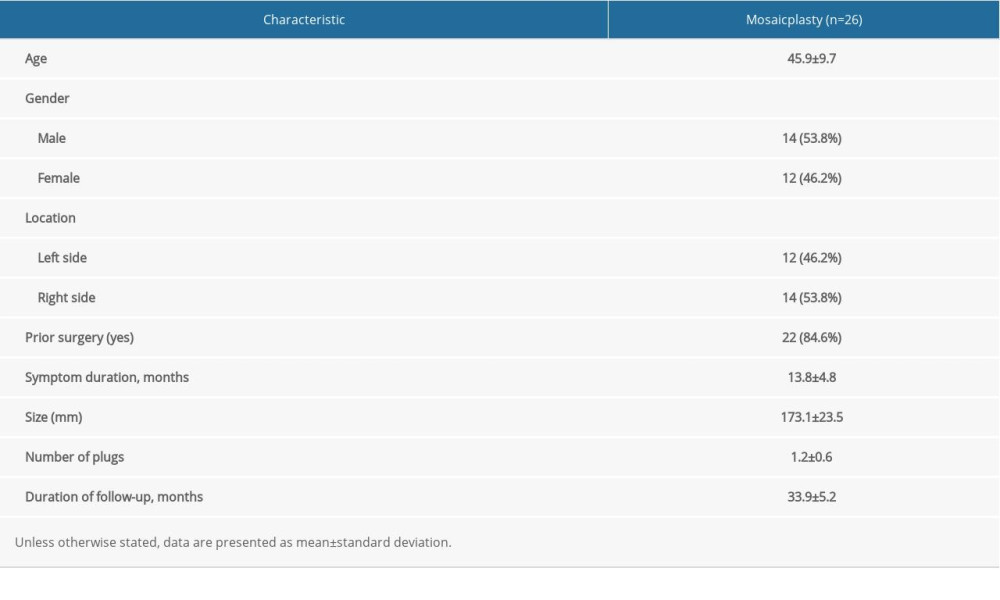 Table 1. Characteristics of the patients.
Table 1. Characteristics of the patients.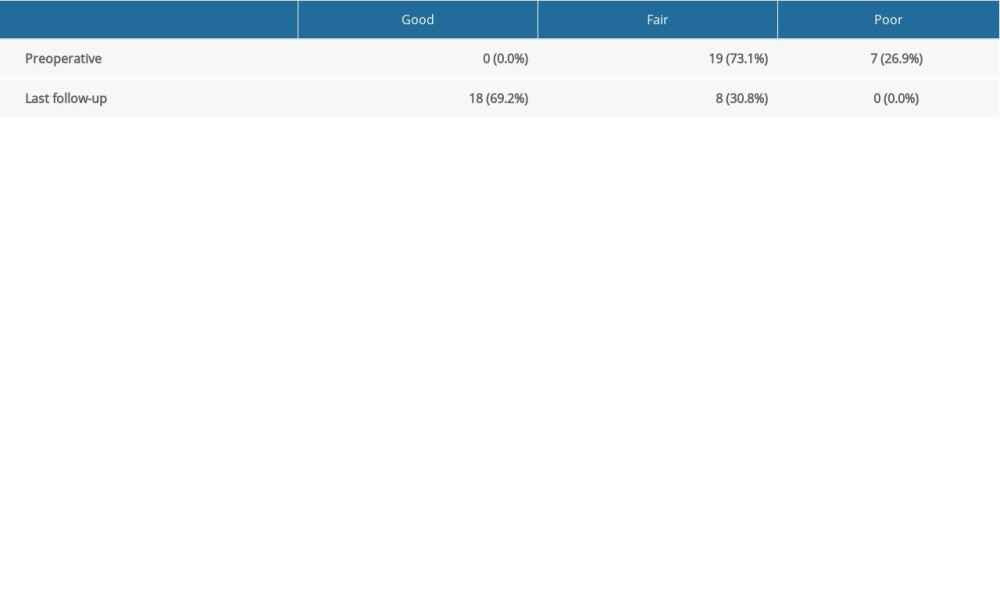 Table 2. Preoperative and last follow-up Berndt and Harty outcome question.
Table 2. Preoperative and last follow-up Berndt and Harty outcome question.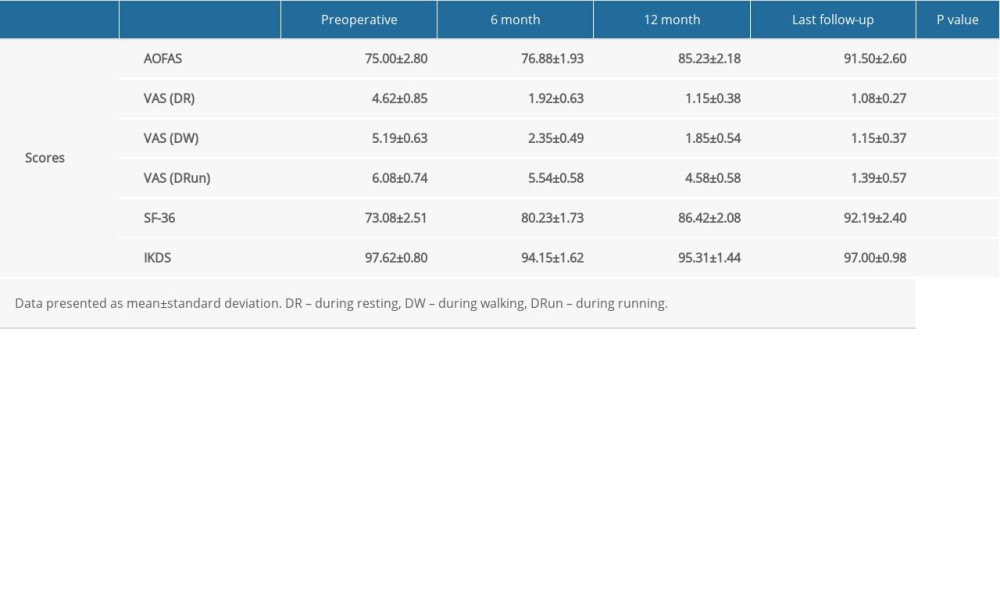 Table 3. Comparison of pain and functional assessment scores at various stages.
Table 3. Comparison of pain and functional assessment scores at various stages. Table 1. Characteristics of the patients.
Table 1. Characteristics of the patients. Table 2. Preoperative and last follow-up Berndt and Harty outcome question.
Table 2. Preoperative and last follow-up Berndt and Harty outcome question. Table 3. Comparison of pain and functional assessment scores at various stages.
Table 3. Comparison of pain and functional assessment scores at various stages. In Press
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








