18 June 2021: Clinical Research
Relationship of Bone Status with Serum Uric Acid and Bilirubin in Men with Type 2 Diabetes: A Cross-Sectional Study
Yang Wu1ABCDEF, Shoukui Xiang1BCDE, Xiaohong Jiang1B, Long Wang1BF, Kun Wang2AG, Fei Hua1AG*DOI: 10.12659/MSM.930410
Med Sci Monit 2021; 27:e930410
Abstract
BACKGROUND: Accumulating evidence has shown that serum uric acid and bilirubin are associated with some chronic diseases, owing to their antioxidant capacity, but the previous research produced discrepant results regarding the relation between uric acid, as well as bilirubin, and bone health. This study was designed to assess the relationship of serum uric acid and total bilirubin with bone mineral density and bone turnover markers in men with type 2 diabetes.
MATERIAL AND METHODS: In total, 631 male patients with type 2 diabetes were included. Data of patients’ medical history, biochemical index, bone mineral density of the lumbar vertebra, femoral neck, and total hip, and bone turnover markers including osteocalcin (OC), amino-terminal propeptide of type I procollagen (PINP), type I collagen carboxy-terminal peptide (CTX), and parathyroid hormone were collected and retrospectively analyzed.
RESULTS: Both serum uric acid and total bilirubin were positively related to bone mineral density of the lumbar vertebra (b=0.179, p<0.001; β=0.095, p=0.030), femoral neck (β=0.133, p=0.002; β=0.089, p=0.029), and total hip (β=0.142, p=0.001; β=0.087, p=0.032), respectively. Serum uric acid concentration was negatively related to bone turnover markers (OC: r=-0.148, p=0.037; PINP: r=-0.139, p=0005; CTX: r=-0.200, p=0.005). Each unit increase of serum uric acid and total bilirubin was associated with a 0.4% and 5.6% lower risk of osteoporosis or osteopenia (OR=0.996, 95% CI=0.994-0.998; OR=0.944, 95% CI=0.899-0.992), respectively. The risk of osteoporosis and osteopenia in patients with low-tertile concentrations of serum uric acid and total bilirubin was increased (OR=3.486, 95% CI=1.535-7.913).
CONCLUSIONS: In men with type 2 diabetes, serum uric acid level and total bilirubin were significantly associated with bone mineral density and were protective factors against osteoporosis and osteopenia.
Keywords: bilirubin, Bone Density, Diabetes Mellitus, Type 2, Uric Acid
Background
Osteoporosis is a common bone disease characterized by impaired bone mass, compromised bone strength, and increased risk of fracture. Because of atypical symptoms in the early stages, people are often unaware about the occurrence of osteoporosis until severe problems arise, such as pain or fracture.
The pathogenesis of osteoporosis is complex. Accumulating studies have shown that oxidative stress has detrimental effects that are involved in the development of osteoporosis, such as inhibiting the differentiation of osteoblasts and stimulation of osteoclastogenesis [1]. In recent years, the antioxidant capacity of several metabolites, such as uric acid (UA) and bilirubin, has been demonstrated [2,3]. UA is the end-product of purine catabolism. Although elevated serum UA level has been suggested to be strongly associated with atherosclerotic diseases [4], a potential protective role of UA was reported against neurologic diseases owing to its antioxidant ability [5–7]. With regard to the association between UA and bone health, clinical research has produced discrepant results. Some researchers have found UA is associated with higher bone mineral density (BMD) [8–10], while others have not found any correlation between UA and BMD or bone turnover markers (BTMs) [11]. Bilirubin, the end-product of heme catabolism, was generally known as a neurotoxin until 1987, when Ames et al revealed its beneficial role as a physiological antioxidant at low concentrations in vitro [3]. Past research had controversial results regarding the relationship between bilirubin and bone status. Some studies have shown that bilirubin is a risk factor for osteoporosis in patients with liver disease [12,13], some studies found bilirubin inversely associated with the prevalence of osteoporosis in patients without liver disease [14,15], and other studies have not found any correlation between bilirubin and bone metabolism [16]. Whether UA or bilirubin, most previous research has been based on data analysis of postmenopausal women, with few studies conducted among men.
The increasing prevalence of type 2 diabetes mellitus (T2DM) has become a worldwide health problem. Although BMD of patients with T2DM is similar to or even higher than that of patients without T2DM, the risk of fragility fracture is increased owing to impaired bone quality and strength [17,18]. It has been reported that the concentration of endogenous antioxidants is changed in patients with T2DM. However, few studies have evaluated the relationship of bone status with UA and bilirubin in men with T2DM. Recent epidemiological data show that in older Chinese men, the prevalence of osteoporosis and osteopenia is 6.46% and 55%, respectively [19]. Therefore, further study is needed to identify the influence of UA and bilirubin on the bone health of men with T2DM.
Material and Methods
STUDY POPULATION:
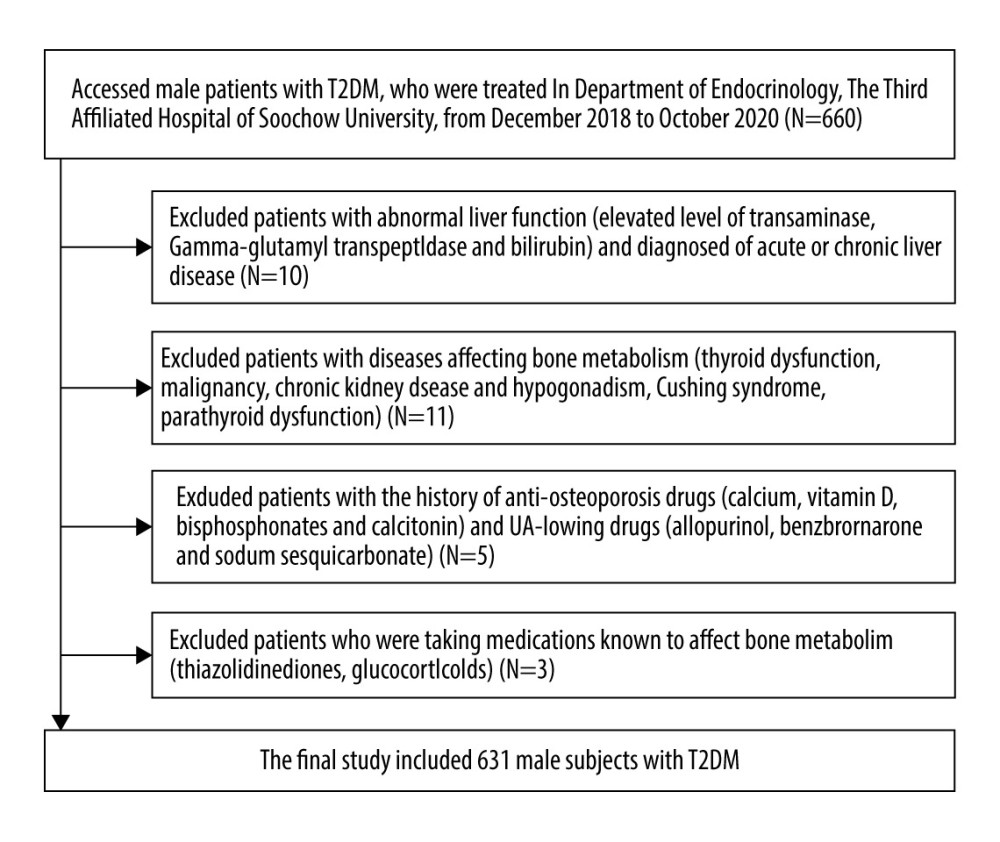
We retrospectively reviewed the data of 631 men with T2DM hospitalized in the Department of Endocrinology of the Third Affiliated Hospital of Soochow University from December 2018 to October 2020. All patients were diagnosed with T2DM and were admitted to the hospital for adjustment of their hypoglycemic treatment and comprehensive assessment of chronic diabetic complications. Figure 1 shows the screening process of participants. This study was approved by the Ethics Committee of the Third Affiliated Hospital of Soochow University.
BIOCHEMICAL MEASUREMENTS:
Blood samples were taken the morning after participants had fasted overnight for at least 10 hours. The concentrations of serum total bilirubin (TBIL), gamma-glutamyl transpeptidase, albumin, UA, creatinine (Cr), urea nitrogen, total cholesterol (TC), triglyceride (TG), high-density lipoprotein (HDL), low-density lipoprotein (LDL), calcium, and phosphorus were measured using an automated AU-5800 analyzer (Beckman Coulter, Brea, CA, USA). Fasting levels of BTMs (osteocalcin [OC], amino-terminal propeptide of type I procollagen [PINP], type I collagen carboxy-terminal peptide [CTX], parathyroid hormone [PTH]) and 25-hydroxy vitamin D (25(OH)D3) were analyzed on Cobas E601 (Roche Diagnostics, Mannheim, Germany). Glycated hemoglobin (HbA1c) was tested using an automated glycosylated hemoglobin analyzer (Bio-Rad, Hercules, CA, USA).
BMD MEASUREMENT:
BMD was assessed at the lumbar vertebra (LV), femoral neck (FN), and total hip (TH) using dual-energy X-ray absorptiometry (DEXA; Hologic Discovery Wi, Ontario, Canada). The T-score is the difference in standard deviation between the BMD value of each individual and that of healthy reference adults. As defined by the World Health Organization, osteoporosis is diagnosed with T-score -2.5 or below; osteopenia is diagnosed with T-score −1.0 to −2.5. In this study, osteoporosis/osteopenia was defined as a T-score below −1.
STATISTICAL ANALYSIS:
We used SPSS version 19.0 software for the statistical analysis (IBM Corp., Armonk, NY, USA). Continuous variables with a normal distribution and categorical variables are reported as mean±standard deviation (SD) and percentage using the
Results
PARTICIPANT CHARACTERISTICS:
The baseline characteristics of participants in this study are presented in Table 1. We divided the 631 male participants with T2DM into 2 groups, according to BMD T-scores: the normal BMD group (T-score ≥-1) and osteoporosis/osteopenia group (T-score <-1). The average age of all participants was 57.3±12.0 years. The mean duration of T2DM was 8.4±7.8 years and participants’ mean level of HbA1c was 9.7±2.4%. The average BMD of the LV, FN, and TH was −0.8±1.3, −1.1±0.9, −0.5±0.8 g/cm2, respectively. Participants with T-scores <-1 had significantly lower serum concentrations of UA, Cr, and BMI than those with T-scores ≥-1. The 2 groups showed no significant differences in the duration of T2DM; level of HbA1c; fasting blood glucose, TC, TG, HDL, LDL, and 25(OH)D3; history of hypertension; smoking; alcohol intake; and use of insulin/analogs.
ASSOCIATIONS AMONG UA, TBIL, BMD, AND BTMS:
We calculated the associations of UA and TBIL with BMD and BTMs using Spearman correlation analysis. Serum UA level was positively correlated with BMD of the LV, FN, and TH and inversely correlated with BTMs (OC, PINP, CTX). The level of serum TBIL was also positively related to BMD of the LV, FN, and TH (Table 2).
To determine the relationship of serum UA and TBIL with BMD and BTMs in male patients with T2DM, we used multiple linear regression analysis. Variables including BMI and Cr were adjusted in Model I. In Model II, we adjusted variables including age, BMI, duration of T2DM, history of hypertension, and insulin/analog use, smoking, drinking, and levels of HbA1c, FBG, Cr, albumin, TC, TG, HDL, LDL, and 25(OH)D3. The results suggested that UA was associated with BMD of the LV, FN, and TH (β=0.179, p<0.001; β=0.133, p=0.002; β=0.142, p=0.001, respectively) and was also associated with BTMs including OC, PINP, and CTX (β=−0.193, p=<0.001; β=−0.185, p<0.001; β=−0.233, p<0.001, respectively). UA was not associated with PTH. TBIL was associated with BMD of the LV, FN, and TH (β=0.095, p=0.030; β=0.089, p=0.029; β=0.087, p=0.032, respectively). TBIL and BTMs presented no significant association (Table 3).
INFLUENCING FACTORS ASSOCIATED WITH THE PREVALENCE OF OSTEOPOROSIS AND OSTEOPENIA:
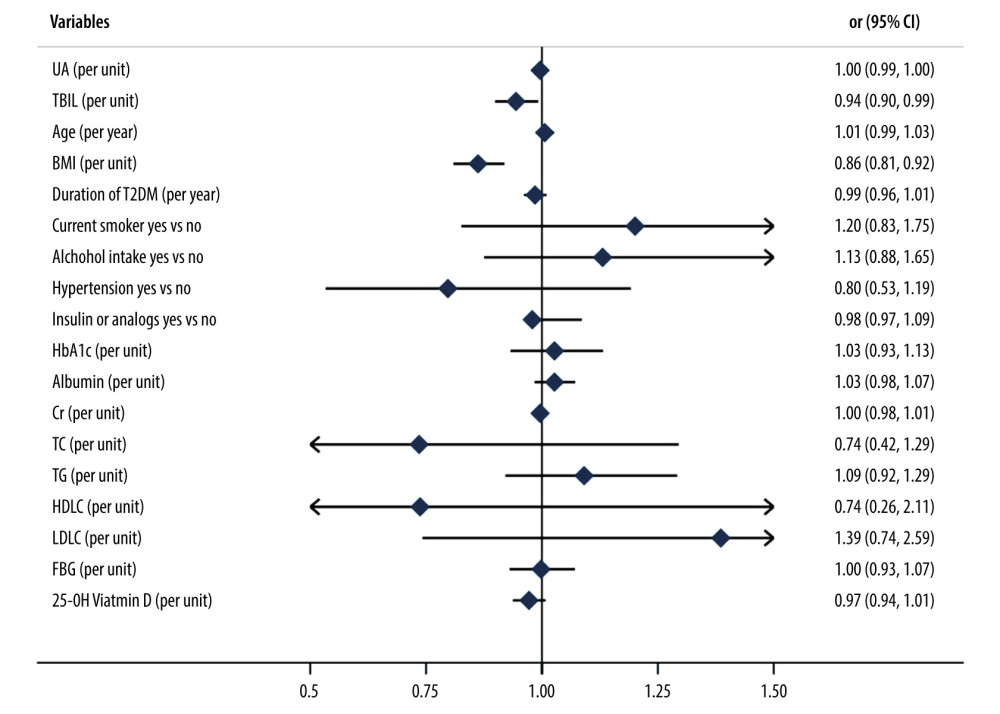
To clarify the contributions made by serum UA and TBIL in the prevalence of osteoporosis and osteopenia, we performed binary logistic regression analysis. The OR (95% CI) of osteoporosis and osteopenia was 0.996 (0.994, 0.998), 0.944 (0.899, 0.992), and 0.862 (0.808, 0.919) for UA, TBIL, and BMI, respectively, in the multivariable-adjusted model, indicating that each unit increase of UA, TBIL, and BMI was associated with a 0.4%, 5.6%, and 13.8% lower risk of osteoporosis and osteopenia, respectively (Table 4). A forest plot showed that UA, TBIL, and BMI were protective factors against osteoporosis and osteopenia (Figure 2).
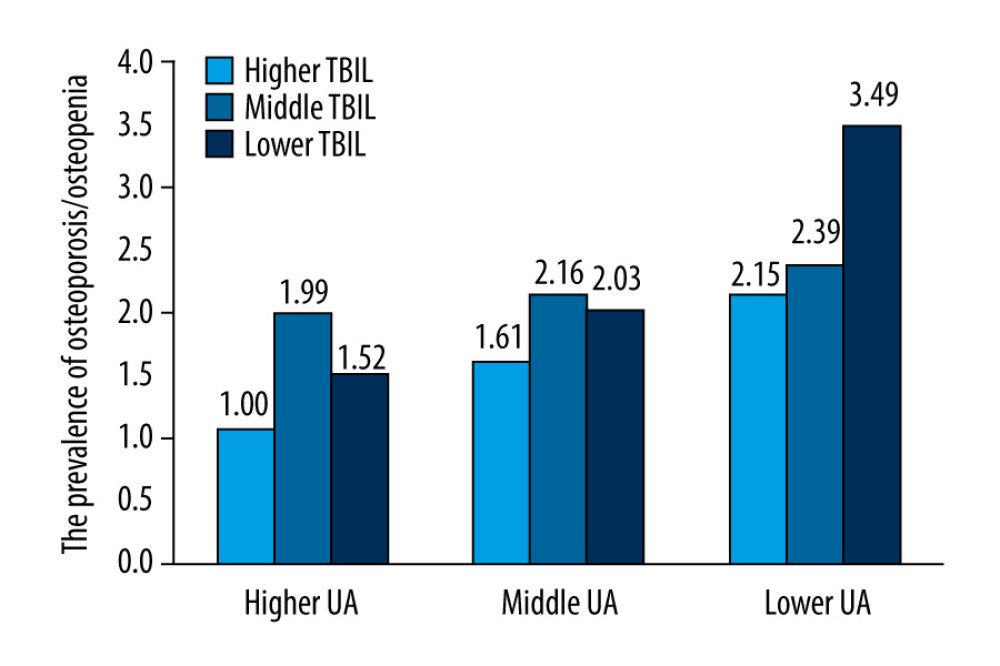
To identify the influence of serum UA and TBIL at different concentrations on the prevalence of osteoporosis and osteopenia, these were divided into 3 groups according to tertiles. The prevalence of osteoporosis and osteopenia in each combination was compared. Table 5 and Figure 3 show that individuals with lower serum UA combined with lower serum TBIL had 3.49 times the prevalence of osteoporosis and osteopenia as compared with individuals who had higher serum UA combined with higher serum TBIL, after multivariable adjustment.
Discussion
The present study focused on male patients with T2DM who were at risk of osteoporosis and osteopenia. It has been reported that mortality after osteoporotic fractures is significantly higher in men than in women [20]. However, less attention has always been paid to the bone health of men. We investigated the association between endogenous antioxidants and bone status in male patients with T2DM to provide additional evidence in this area. The current study suggested a positive relationship among the levels of UA, TBIL, and BMD of the LV, FN, and TH. The level of UA was negatively associated with BTMs including OC, PINP, and CTX. Each unit increase in the concentration of serum UA and TBIL was related to a 0.4% and 5.6% lower risk of osteoporosis/osteopenia. The prevalence of osteoporosis and osteopenia in individuals with low tertiles of UA and TBIL was 3.49 times that of individuals with high tertiles of UA and TBIL.
Concerning the relationship between UA concentration and BMD, our findings were consistent with those of several existing studies showing that serum UA was positively related to BMD of the LV, FN, and TH [8–10]. These past studies were mostly based on data analysis of individuals without diabetes, especially postmenopausal women. Studies on male patients with T2DM are limited. A recent study performed among Chinese men with T2DM had results similar to ours, but the researchers had not explored the relationship between serum UA and BTMs [10]. BTMs are sensitive indicators of the bone turnover process. OC and PINP are bone formation markers, reflecting the activity of osteoblasts. CTX is a marker of bone resorption, reflecting the activity of osteoclasts. The dynamic balance between bone formation and resorption plays an important role in the maintenance of bone mass. In this study, we found that serum UA was negatively associated with OC, PINP, and CTX, indicating the inhibitory effect of serum UA on the bone turnover process of men with T2DM. It has been reported that reactive oxygen species could activate the differentiation of pre-osteoclasts into osteoclasts. Bone formation is tightly coupled with bone resorption. In this study, the positive influence of serum UA on BMD was probably associated with the inhibitory effect of serum UA on the bone turnover process owing to its antioxidant ability. In vitro studies have provided evidence that the genesis of osteoclasts is inhibited by UA in a dose-dependent manner and the formation of reactive oxygen species is also reduced in osteoclast precursors, providing laboratory support for clinical findings [21]. However, some recent studies have suggested that serum UA is not associated with BMD and BTMs in men, including a study conducted in men with T2DM by Tanaka et al [11]. Participants in that study were elderly men with a relatively long duration of diabetes. The difference in the basic characteristics of study participants could be the reason for the discrepant results.
Clinical studies have yielded controversial results regarding the association between serum TBIL levels and bone metabolism; most of these studies were conducted among participants without diabetes [12–16]. Recently, Yan et al found that higher TBIL levels are linked to a higher BMD and lower risk of developing osteoporosis in Chinese patients with T2DM; however, those authors did not evaluate the relationship of serum TBIL with BTMs [22]. In the present study, we found that increased levels of serum TBIL contributed to the reduced prevalence of osteoporosis and osteopenia, which is in accordance with several previous studies. However, the concentration of TBIL was not found to be associated with BTMs. Similar to the present study, a case-control study showed that patients with Gilbert syndrome characterized by hyperbilirubinemia in the absence of hepatocellular disease or hemolysis showed no difference in PTH, CTX, or OC levels compared with controls [16]. Another study among patients with chronic liver disease suggested that the change in OC was not connected with serum bilirubin levels [23]. However, only limited laboratory data concerning the influence of physiological concentrations of bilirubin on bone metabolism are available. Considering the complex regulation factors involved in the process of bone turnover, we cannot rule out the possibility that there are confounding factors that were not taken into account and that affected the association between serum TBIL and BTMs in the present study.
Although both UA and TBIL are endogenous antioxidants, whether their protective effect on BMD is decreased with lower levels of UA combined with lower TBIL levels remains unclear. In the present study, we found a significantly higher prevalence of osteoporosis/osteopenia among men with T2DM who had low tertiles of UA and TBIL, compared with other combinations, which perhaps indicates that physicians should pay greater attention to the bone health of these patients, for early detection of osteoporosis and osteopenia in clinical practice.
Our study had several limitations. First, as a cross-sectional study, the change in BMD and BTMs and the occurrence of osteoporotic fractures over time could not be evaluated without long-term follow-up. Therefore, we could not explore the exact mechanism and infer a causal relationship. Second, although we attempted to consider as many confounding factors as possible, the existence of additional potential confounders cannot be completely ruled out. Third, the sample size was not sufficiently large to conduct subgroup analysis for more detailed results. Finally, we reviewed the data from hospitalized patients, who might not represent all patients with T2DM owing to a possibly more severe state of disease compared with the general population who have T2DM.
Conclusions
Both serum UA and TBIL were found to be related to BMD in men with T2DM. Longitudinal clinical studies are needed to clarify whether higher levels of serum UA and TBIL could be protective factors against fracture in patients with T2DM.
Tables
Table 1. Characteristics of the participants.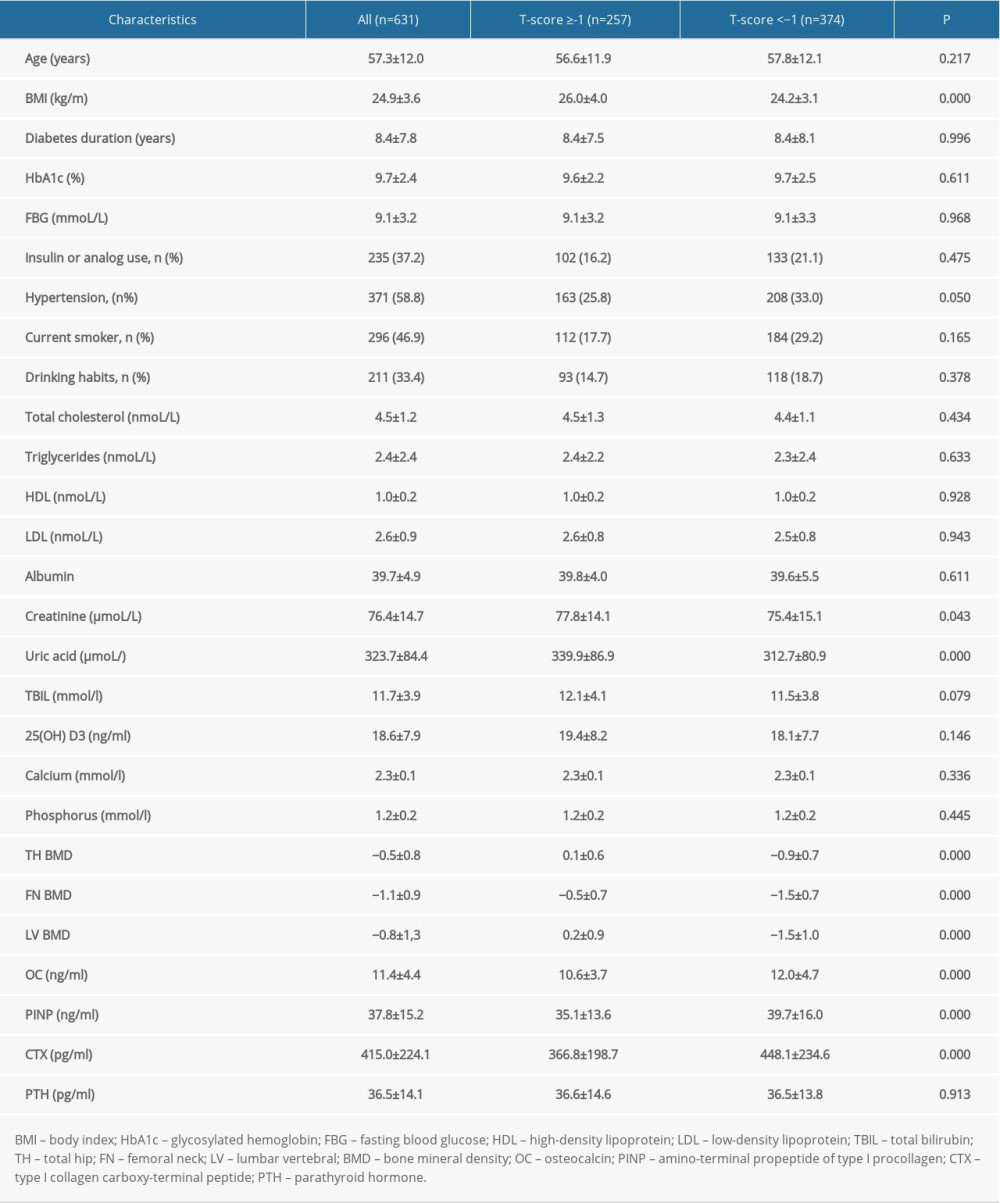 Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs.
Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs.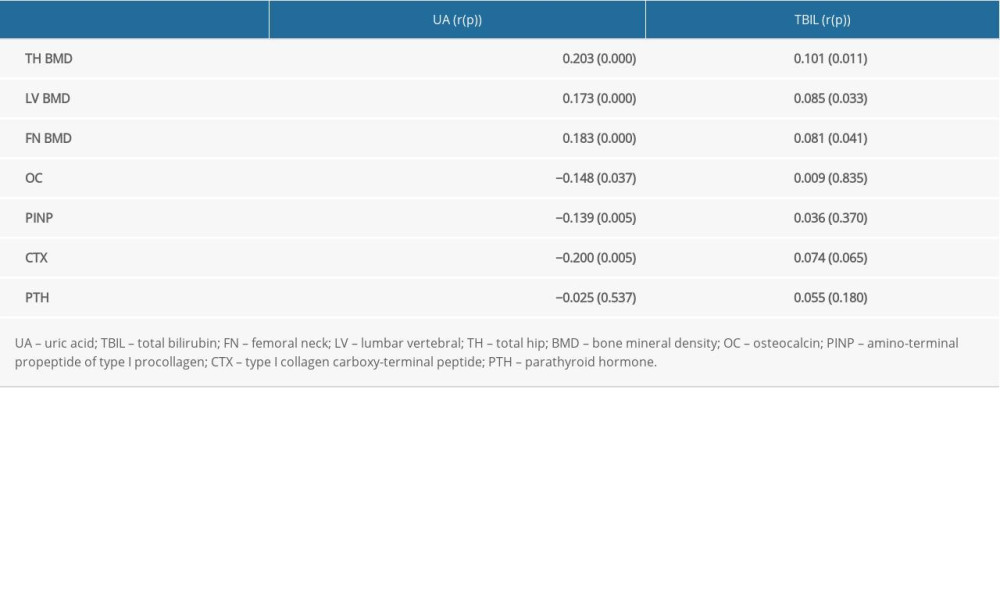 Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs.
Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs.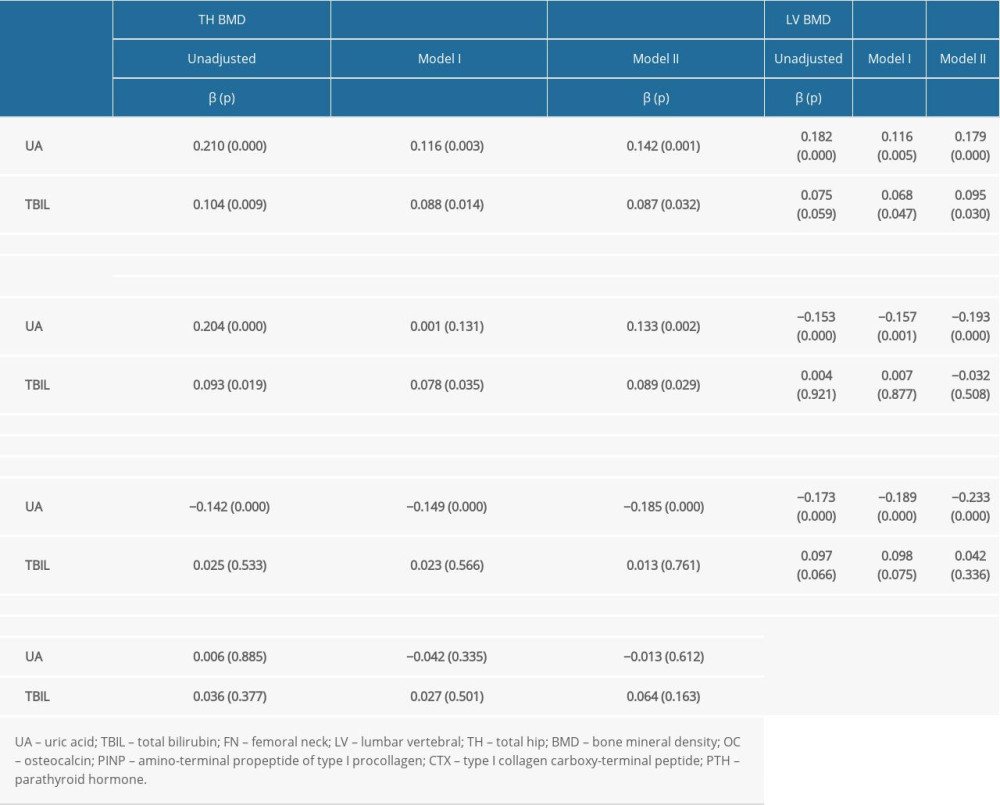 Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM.
Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM.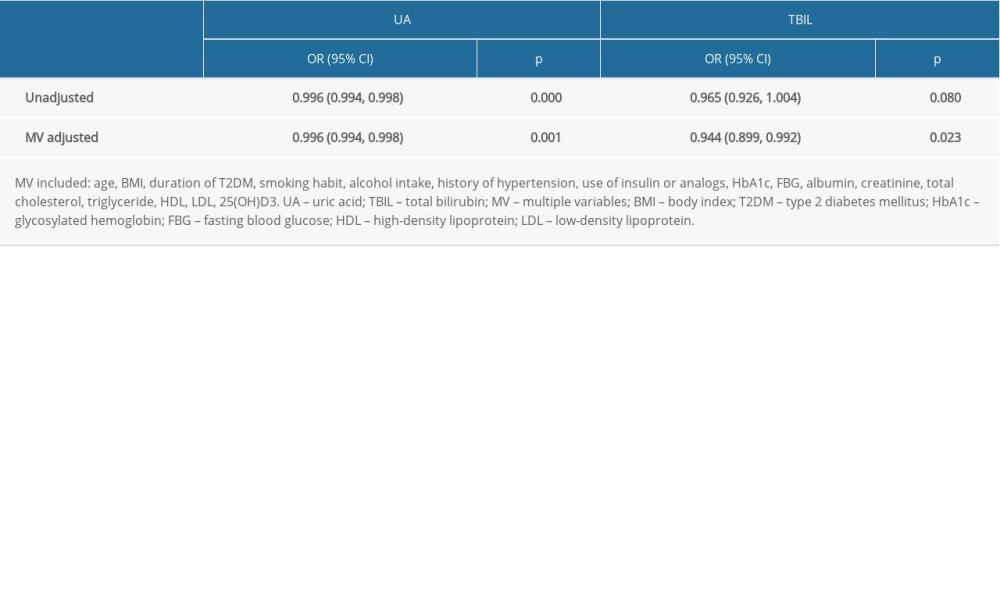 Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM.
Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM.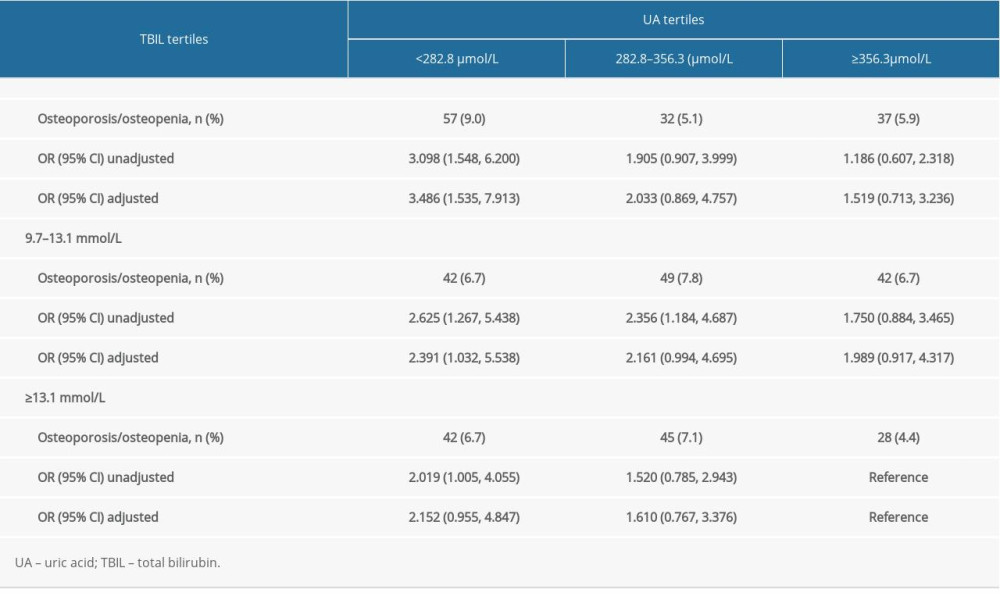
References
1. Corrado A, Cici D, Rotondo C, Molecular basis of bone aging: Int J Mol Sci, 2020; 21(10); 3679
2. Glantzounis GK, Tsimoyiannis EC, Kappas AM, Uric acid and oxidative stress: Curr Pharm Des, 2005; 11(32); 4145-51
3. Stocker R, Yamamoto Y, McDonagh AF, Bilirubin is an antioxidant of possible physiological importance: Science, 1987; 235(4792); 1043-46
4. Ndrepepa G, Uric acid and cardiovascular disease: Clin Chim Acta, 2018; 484; 150-63
5. Tana C, Ticinesi A, Prati B, Uric acid and cognitive function in older individuals: Nutrients, 2018; 10(8); 975
6. Yang D, Weng Y, Lin H, Serum uric acid levels in patients with myasthenia gravis are inversely correlated with disability: Neuroreport, 2016; 27(5); 301-5
7. Çelık RGG, Köksal A, Şahın B, The relationship between serum uric acid levels and clinical features in essential tremor: Noro Psikiyatr Ars, 2020; 57(1); 33-36
8. Dong X, Tian H, He J, Elevated serum uric acid is associated with greater bone mineral density and skeletal muscle mass in middle-aged and older adults: PLoS One, 2016; 11(5); e0154692
9. Yan D, Wang J, Hou X, Association of serum uric acid levels with osteoporosis and bone turnover markers in a Chinese population: Acta Pharmacol Sin, 2018; 39(4); 626-32
10. Zhao DD, Jiao PL, Yu JJ, Higher serum uric acid is associated with higher bone mineral density in Chinese men with type 2 diabetes mellitus: Int J Endocrinol, 2016; 2016 2528956
11. Tanaka KI, Kanazawa I, Notsu M, Higher serum uric acid is a risk factor of vertebral fractures in postmenopausal women with type 2 diabetes mellitus: Exp Clin Endocrinol Diabetes, 2020; 128(1); 66-71
12. Menon KV, Angulo P, Weston S, Bone disease in primary biliary cirrhosis: Independent indicators and rate of progression: J Hepatol, 2001; 35(3); 316-23
13. Kramer RA, Zemel BS, Arvay-Nezu JL, Bone health in nonjaundiced population of children with biliary atresia: Gastroenterol Res Pract, 2009; 2009 387029
14. Bian LQ, Li RZ, Zhang ZY, Effects of total bilirubin on the prevalence of osteoporosis in postmenopausal women without potential liver disease: J Bone Miner Metab, 2013; 31(6); 637-43
15. Kim BJ, Koh JM, Ahn SH, High serum total bilirubin as a protective factor against hip bone loss in healthy middle-aged men: Calcif Tissue Int, 2013; 92(6); 501-8
16. Minuk GY, Greenberg R, Uhanova J, Bone mineral densities in individuals with Gilbert’s syndrome: A cross-sectional, case-control pilot study: Can J Gastroenterol, 2009; 23(6); 431-36
17. Compston J, Type 2 diabetes mellitus and bone: J Intern Med, 2018; 283(2); 140-53
18. Qei L, Zillikens MC, Dehghan A, High bone mineral density and fracture risk in type 2 diabetes as skeletal complications of inadequate glucose control: The Rotterdam Study: Diabetes Care, 2013; 36(6); 1619-28
19. Zeng Q, Li N, Wang Q, The prevalence of osteoporosis in China, a nationwide, multicenter DXA Survey: J Bone Miner Res, 2019; 34(10); 1789-97
20. Kim BJ, Baek S, Ahn SH, Higher serum uric acid as a protective factor against incident osteoporotic fractures in Korean men: A longitudinal study using the National Claim Registry: Osteoporosis Int, 2014; 25(7); 1837-44
21. Ahn SH, Lee SH, Kim BJ, Higher serum uric acid is associated with higher bone mass, lower bone turnover, and lower prevalence of vertebral fracture in healthy postmenopausal women: Osteoporos Int, 2013; 24(12); 2961-70
22. Yan PJ, Zhang ZH, Feng J, Association between serum total bilirubin levels, bone mineral density and prevalence of osteoporosis in Chinese patients with type 2 diabetes: Int J Clin Exp Pathol, 2017; 10(5); 5784-98
23. Szalay F, Lakatos P, Németh J, Decreased serum osteocalcin level in non-alcoholic and alcoholic chronic liver disease: Orv Hetil, 1991; 132(24); 1301-5
Figures
Tables
 Table 1. Characteristics of the participants.
Table 1. Characteristics of the participants. Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs.
Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs. Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs.
Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs. Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM.
Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM. Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM.
Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM. Table 1. Characteristics of the participants.
Table 1. Characteristics of the participants. Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs.
Table 2. Spearman correlations of serum UA and TBIL with BMD and BTMs. Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs.
Table 3. Multiple linear regression analysis showing the association of serum UA and TBIL with BMD and BTMs. Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM.
Table 4. The influence of the change in serum UA and TBIL on the prevalence of osteoporosis and osteopenia in male patients with T2DM. Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM.
Table 5. ORs (95% CI) for the prevalence of osteoporosis and osteopenia in different combinations of serum UA and TBIL level in male patients with T2DM. In Press
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952