27 March 2021: Clinical Research
Use of the Water-Soluble Contrast Medium Gastrografin in Treatment of Adhesive Small Bowel Obstruction in Patients with and Without Chronic Radiation Enteropathy: A Single-Center Retrospective Study
Lili Gu1BCEF, Feng Zhu1BDE, Tingbin Xie1BCD, Dengyu Feng1BEF, Jianfeng Gong1BDEG, Ning Li2ABEFG*DOI: 10.12659/MSM.930046
Med Sci Monit 2021; 27:e930046
Abstract
BACKGROUND: This retrospective cohort study from a single center aimed to compare patient outcomes following the use of the water-soluble contrast medium Gastrografin in the treatment of adhesive small bowel obstruction (ASBO) in patients with and without a history of chronic radiation enteropathy (CRE).
MATERIAL AND METHODS: Fifty-nine patients with CRE-induced small bowel obstruction (SBO) and 53 patients with ASBO at Jinling Hospital between April 2014 and February 2018 were enrolled. The patients were given 100 ml Gastrografin through a naso-jejunal tube, and erect abdominal X-rays were taken. Risk factors were found to be correlated with successful non-operative management (SNM) through statistical analyses.
RESULTS: The success rate of conservative treatment was higher in the Gastrografin group than in the control group (P<0.05). The Gastrografin challenge test is predictive of need for surgery in CRE-induced SBO and ASBO (AUC=0.860 and 0.749, respectively). The predictors associated with SNM in the CRE-induced SBO group were the total dose of radiotherapy, the Gastrografin challenge test, and previous operations for SBO. In the ASBO group, the predictors were the Gastrografin challenge test and previous operations for SBO. The operation rate of SBO patients with Gastrografin treatment was significantly lower than that in the control group (P<0.05).
CONCLUSIONS: The findings from this study showed that the use of Gastrografin effectively resolved ASBO in patients with and without a history of CRE, but a long-term requirement for surgery could not be avoided. The Gastrografin challenge may be a useful test to predict surgical outcomes.
Keywords: Diatrizoate Meglumine, Inflammatory Bowel Diseases, Radiation Effects, Cohort Studies, Contrast Media, Intestinal Obstruction, Intestine, Small, Radiation Injuries, Solubility, Tissue Adhesions, Water
Background
More than half of all patients with cancer, especially those with gastrointestinal (GI) cancers or urological and gynecological problems, receive radiotherapy (RT) either individually or along with chemotherapy or surgery [1]. However, ionizing radiation to the abdomen or pelvis is often accompanied by systemic GI damage [2]. The radiation-induced enteropathies can be divided into the acute (early) types, which occur within 3 months of RT, and the chronic (delayed) types, which occur >3 months after therapy. Chronic radiation enteropathy (CRE) may develop with various clinical manifestations such as abdominal pain, diarrhea, and intestinal obstruction. Depending on the type of tumor and RT, small bowel obstruction (SBO) due to radiation injury can occur in 8% to 13% of cases [3]. Around one-third of patients with CRE need operations, which are usually for the management of intestinal obstructions secondary to structures or adhesion [4,5].
Gastrografin, also known as diatrizoate, is a contrast agent for X-ray imaging, which is generally used to deal with adhesive SBO (ASBO) or prolonged postoperative ileus (PPOI) [6–9]. The therapeutic effect of Gastrografin is due to its hyper-osmolarity, which causes endosmosis from the intestinal wall and surrounding soft tissues into the lumen, thereby diminishing the edema-related inhibition of gastrointestinal contractility, as well as restoring intestinal motility [6,10,11]. There have been few investigations about the usage of oral water-soluble contrast media in CRE-induced SBO, and their clinical applications are promising despite bowel wall edema, which is thought to be a prominent feature of its pathogenesis [2,12–14].
We utilized Gastrografin to treat CRE-induced SBO and found that the rate of operative intervention and duration of hospital stay decreased. In terms of clinical outcomes, patients with CRE-induced SBO who received Gastrografin had a higher frequency of surgical intervention compared to patients without CRE-induced SBO. This retrospective study aimed to elucidate the clinical effects of Gastrografin in patients with CRE-induced SBO and ASBO, and determine the therapeutic and diagnostic utility of Gastrografin in CRE-induced SBO. We also assessed the clinical effects of Gastrografin in SBO patients by comparing the outcomes of SBO patients with and without Gastrografin treatments. This retrospective cohort study from a single center aimed to compare patient outcomes following the use of the water-soluble contrast medium, Gastrografin, in the treatment of adhesive small bowel obstruction in patients with and without a history of chronic radiation enteropathy.
Material and Methods
ETHICS STATEMENT AND PATIENTS:
The Ethics Committee in Jinling Hospital approved current study (Ref. No. JLH2014-018-EC). All patients who participated in the study provided written informed consent. Fifty-nine patients with CRE-induced SBO and 53 patients with ASBO who received Gastrografin at Jinling Hospital between April 2014 and February 2018 were enrolled. WE enrolled a control group of 30 patients, who did not undergo Gastrografin treatment but were treated conservatively, including placing a gastric tube for gastrointestinal decompression and use of somatostatin to inhibit digestive juice secretion.
Patients in the radiation SBO and ASBO groups had also undergone surgeries. All patients in our study underwent open surgery, and there was no minimally invasive surgery performed, which required surgical indications for patients with intestinal obstruction. Due to the sparse data, we randomly selected 30 patients with Gastrografin and 30 without Gastrografin treatments for comparison. All patients were admitted at least 6 months after completion of RT, and at the time of being diagnosed with CRE had associated SBO or ASBO as determined from clinical history, computed tomography (CT), and intraoperative and histological findings. SBO was diagnosed based on clinical symptoms (bilious vomiting, abdominal distension, and failure to pass gas or stool) and air-fluid levels on the abdominal radiograph, while the diagnostic criterion for ASBO was the presence of an obstruction secondary to adhesions. We excluded patients who: (a) underwent colostomy or ileostomy, had large bowel obstruction, metastatic disease or obstruction within 4 weeks after a recent operation or serious co-morbidity; or (b) had a known history of allergies or hypersensitivity to iodinated contrast agents; or (c) had signs of strangulation. Neoplasm recurrence was defined as any clinical, radiological, or histopathological evidence of cancer during the index admission. Clinical records of SBO patients containing detailed medical history, treatments, and concomitant pathologies were included in strict adherence to the STROCSS guidelines [15].
GASTROGRAFIN ADMINISTRATION:
All patients were given a complete physical examination upon admission, with an emphasis on signs of bowel strangulation and peritonitis. They were prescribed a strict diet, intravenous fluid administration, somatostatin therapy, and nasogastric tube (NGT) placement. Abdominal X-rays were performed for all SBO patients in standing position, and abdominal CT with contrast agent was conducted to establish diagnosis effects. After 1-day aspiration through the NGT, a catheter was placed through the ligament of Treitz into the jejunum under fluoroscopy guidance, and 100 ml Gastrografin (Schering, Berlin, Germany) was injected through the naso-jejunal catheter (NJT) in an upright position and then clamped for 2 h. If the patient vomited, the NJT was reopened, but no additional Gastrografin or saline solution was administered. Erect abdominal X-rays were taken after 1 day, and based on the Ogaki system, the obstructions were classified as complete (type I/II) or incomplete (types IIIA/IIIB) [16]. The Gastrografin presence in colon or a bowel movement indicated a successful passage, and the non-operative therapy was continued. In case the Gastrografin therapy failed, surgical options were considered. The obstruction etiology was determined based on the operative report.
TREATMENT SLOTS:
The indications for surgical intervention were suspected ischemia of the gut (acute cramps, signs of peritonitis, fever and/or WBC counts >16 000/ml), absence of contrast in the cecum, and absence of flatus or stools 48 h after treatment [17]. In addition, patients who did not show any improvement after 5 days underwent surgery. In a previous study [18], similar surgery was introduced to treat ASBO. For both groups, we tracked the time to resolution of adhesive small intestine obstruction (ASIO) with restored flatus and bowel motion, which is the time elapsed between initiation of treatment and first bowel action, and length of hospital stay (in hours, calculated from the time of hospital admission to resolution of intestinal obstruction). Complete obstruction resolution was confirmed when its signs and symptoms subsided, which was followed by NGT removal and initiation of normal feeding. The criteria for discharge were absence of any obstructive symptoms and ability to tolerate a normal diet. The patients were followed up for 1 year after discharge.
STATISTICAL ANALYSIS:
Sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) were calculated for both CRE-induced SBO and ASBO groups. Sensitivity was defined as the percentage of patients who failed the Gastrografin challenge test among those who underwent surgical intervention. Specificity was the percentage of patients with successful Gastrografin challenge test among those who underwent non-surgical therapy [19,20]. Receiver operating characteristics (ROC) curves were drawn for the ASBO and CRE-induced SBO groups.
All statistical analyses were performed using IBM SPSS version 23.0 (IBM SPSS, Inc, Chicago, USA). For continuous variables, descriptive statistics are expressed as mean±SD. The patient groups were compared via chi-square test, Fisher exact test, 2-sample
Results
PATIENT IDENTIFICATIONS:
The mean age of the 112 (59 with CRE-SBO and 53 with ASBO) patients was 53.9±17.2 years, 31.2% (n=35) of whom were male. There was no significant difference (P value >0.05) between the 2 groups regarding age, laboratory test outcomes, abdominal CT-scan, and history of abdominal surgery (Table 1). The proportion of the patients with adhesiolysis was higher (P value=0.004) in the ASBO group (37.7%) compared to the CRE-induced SBO group (13.5%). The mortality rate in the entire cohort was 1.7%, and 1 patient in the CRE-induced SBO group died. We randomly selected 30 patients with Gastrografin treatments and compared their data with the control group. The proportion of patients with adhesiolysis was higher (P value=0.004) in the control group (33.3%) compared to the Gastrografin treatment group (20%) (Table 2). The rate of junction sign in controls (73.3%) was higher than that (46.6%) in the Gastrografin group (P value=0.03).
CLINICAL OUTCOMES:
The clinical outcomes of the patients are summarized in Table 3. The successful conservative treatment rate in the ASBO group was higher than that in the CRE-induced SBO group (58.4% vs 33.9%, P value=0.021). Consistently, the operative rate was lower in the ASBO group than in the CRE-induced SBO group (41.6% vs 66.1%, P value=0.031). However, the time to resolution, as reflected by the time to first feed after admission, was not significantly different between the 2 groups (P value=0.531). The proportion of strangulation and resection was much lower with the ASBO patients compared to the CRE-induced SBO group (5.6% vs 44.0%, P value <0.001). The ASBO group had a lower rate of readmission for SBO compared with that in CRE-induced SBO group (13.2% vs 28.8%, P value=0.038).
Table 4 shows the effects of Gastrografin on SBO and compares the clinical outcomes between patients with and without Gastrografin treatments. The rate of successful conservative treatment in the Gastrografin treatment group was higher than that in the control group (53.3% vs 20%, P value=0.002). Also, the operative rate was lower in the Gastrografin treatment group than that in the control group (46.6% vs 80%, P value=0.002). The proportion of strangulation and resection was lower in the patients with Gastrografin treatment compared to the control group (30% vs 43.3%, P value=0.007).
GASTROGRAFIN CHALLENGE TEST PREDICTS NEED FOR SURGERY:
To determine the diagnostic utility of Gastrografin challenge, we performed ROC curve analysis of the operative rate against Gastrografin challenge test results. In the CRE-induced SBO group, the sensitivity and specificity of the test were 90.0% and 83.7%, respectively, with area under curve (AUC) of 0.860 (
FACTORS ASSOCIATED WITH SUCCESSFUL NON-OPERATIVE MANAGEMENT (SNM):
The significant predictors associated with SNM in the CRE-induced SBO group were the total dose of radiotherapy (OR=0.911, 95% CI 0.678–1.144, P value <0.041), successful Gastrografin administration (OR=4.812, 95% CI 3.343–6.281, P value <0.001), and the previous operation for SBO (OR=0.364, 95% CI 0.262–0.466, P value < 0.007). In ASBO group, successful Gastrografin administration (OR=3.191, 95% CI 1.447–4.935, P value <0.001) and the previous operation for SBO (OR=0.601, 95% CI 0.136–1.066, P value <0.023) were associated with successful non-operative treatment (Table 5).
To compare the SNM between the Gastrografin group and non-Gastrografin group, we provided Table 3. The significant predictors associated with SNM in the Gastrografin group were the successful Gastrografin administration (OR=3.58, 95% CI 2.83–5.54, p value <0.001), and the previous operation for SBO (OR=0.27, 95% CI 0.14–0.34, P value <0.007). In non-Gastrografin group, no factors were associated with successful non-operative treatment (Table 6).
LONG-TERM OUTCOMES OF SUCCESSFUL CONSERVATIVE TREATMENT:
Thirty-one ASBO patients and 20 CRE-induced SBO patients had successful conservative treatment (Table 7) and were discharged without surgery. During 1-year follow-up, 17 out of 20 (85%) CRE-induced SBO patients had a relapse and 13 out of 31 (41.9%) ASBO patients had a relapse. Strikingly, CRE-induced SBO patients had significantly higher reoperation rates than ASBO patients upon readmission (70.0% vs 11.2%) (Table 7). We assessed the long-term efficacy of Gastrografin by comparing patients with and without Gastrografin in Table 8, from which we know that the Gastrografin group has lower reoperation rates than the non-Gastrografin group regarding the readmission (20.0% vs 23.3%).
Discussion
We discovered that the effects of Gastrografin through the naso-intestinal tube on CRE-induced SBO and ASBO are disparate. Studies showed that Gastrografin is the first-line conservative treatment for ASBO [21]. The effective rate of conservative treatment can be as high as 76.8%, which is close to our results. A recent study demonstrated that even patients who were not cured by conservative treatment with Gastrografin within 48 h can still avoid surgery via conservative treatments [22]. Our data indicated that the pathogenesis and mechanism of CRE-induced SBO differ from those of ASBO. The intestinal fibrosis of CRE is a gradual process. Even if conservative treatment with Gastrografin is employed to restore intestinal patency, it is ultimately necessary to undergo surgical treatment, but it bought time for the clinicians to avoid emergency surgery and increased the chance of ileostomy during the operations.
Both overall and non-operative stay length of the 2 groups were similar (5.3±1.9 days vs 5.0±2.1 days and 2.1±1.3 days vs 2.5±1.9 d) in terms of hospitalization, suggesting that comorbidities of CRE-induced obstruction and ASBO were not significantly different. However, the non-operative group had a significantly shorter stay length comparing with the overall population (CRE-induced group,
Radiation enteritis refers to any injury to the small intestine resulting from radiotherapy (RT) [23]. However, little is known regarding the pathophysiological basis of radiation-induced bowel injury (RBI). RT induces long-term changes in bowel function as a result of progressive endothelial damage, which induces ischemia and subsequent fibrosis. These pathological changes manifest clinically as partial or complete bowel obstruction due to strictures, impaired motility, fistulae, GI bleeding, impaired nutrition absorption, and perforation with sepsis in some cases. Intestinal obstruction is the most common manifestation, which is a difficult surgical challenge [24]. More than two-thirds of all small bowel obstructions are due to peritoneal adhesions. Adhesive obstruction may occur at any time after surgery, and almost 20% of the obstructions appear more than 10 years after the initial abdominal operation [25].
The Gastrografin challenge test has been shown to guide management and predict need for exploration in SBO patients [26]. Our data agreed with previous studies and investigated the predictive value of the Gastrografin challenge test in CRE-induced and adhesive SBO. We found that Gastrografin challenge test failure was highly predictive of need for surgery, especially in CRE-induced SBO. However, the specificity of this test in the ASBO group was relatively low (68.7%). One explanation might be that some patients with ASBO failed the Gastrografin challenge test, but the administration of Gastrografin resolved the acute symptoms, thus avoiding the need for surgery.
The osmolarity of Gastrografin in the intestinal cavity is around 1900 mM, which is 6 times that of extracellular fluid. Its water solubility makes it difficult to absorb in the gastrointestinal tract. Even if intestinal perforation occurs, it can be easily absorbed by peritoneal membranes after it enters the abdominal cavity, with little irritation. Due to its ability to cause endosmosis from the edematous bowel wall into the lumen, Gastrografin is also used as a laxative. Its therapeutic effect in adhesive SBO relies on its ability to improve myocyte activity, to induce peristalsis, and to create a longitudinal pressure difference across the site of obstruction [6,13]. The barium contrast material, on the other hand, can lead to complete obstruction by decreasing the viscosity of bowel contents. Furthermore, leakage of barium into the abdominal cavity in case of perforation is potentially lethal [27,28]. Several studies showed that Gastrografin reduces the surgical rate of adhesive intestinal obstruction and shortened the hospitalization time of patients [24]. We found that while Gastrografin accelerated time to flatus or stool, resolution of distension, and tolerance of enteral nutrition in patients with CRE-induced SBO, it did not have any effects on the operation rate and the hospital stay length. These findings may be related to the progressive nature of CRE.
Accidental aspiration of the contrast medium is the major complication of Gastrografin therapy. Therefore, to avoid any aspiration, we administrated Gastrografin through a naso-jejunal feeding tube. This was effective in preventing aspiration as well as shortening the examination time. Some studies show that compared to the traditional gastric tube, the trans-anal intestinal obstruction catheter has a stronger effect in reducing the intestinal lesions and improving the general condition of patients [29,30]. No adverse events were seen following Gastrografin administration in our cohort. However, any imbalances in electrolytes should be corrected in patients with intestinal obstruction prior to the Gastrografin treatment to prevent further deterioration. In addition, Gastrografin therapy is not recommended for people with iodine allergies, liver and kidney dysfunction, active tuberculosis, multiple myeloma, or hyperthyroidism.
Certain limitations need to be considered when interpreting our results. Our investigation was a retrospective, single-center study with a relatively small cohort size, which could not adjust for potential confounders using methods like propensity score matching. Furthermore, the inclusion criteria in our study had no age limitation, which might have introduced a bias since age >65 years has been shown to be a risk factor for the failure of Gastrografin therapy [31,32]. In addition, the cost of hospitalization can also be analyzed, but we only used the length of stay to reflect morbidity. Certainly, there are limitations of the study, which are the small sample size, the use of a single center, and the bias that may be introduced.
Conclusions
The findings from this study showed that the use of Gastrografin effectively resolved ASBO in patients with and without a history of CRE, but a long-term requirement for surgery could not be avoided. The use of Gastrografin challenge may be a possible test to predict surgical outcomes. Following Gastrografin administration, the rate of successful conservative treatment and the operative rate were higher and lower, respectively, in the ASBO compared to the CRE-induced SBO group, which is consistent with our initial hypothesis that CRE-induced SBO requires more frequent surgical intervention. The Gastrografin protocol and previous surgery for SBO were the 2 important factors that influenced the efficacy of non-operative management in both patient groups.
Tables
Table 1. Patient characteristics of CRE-induced SBO and ASBO.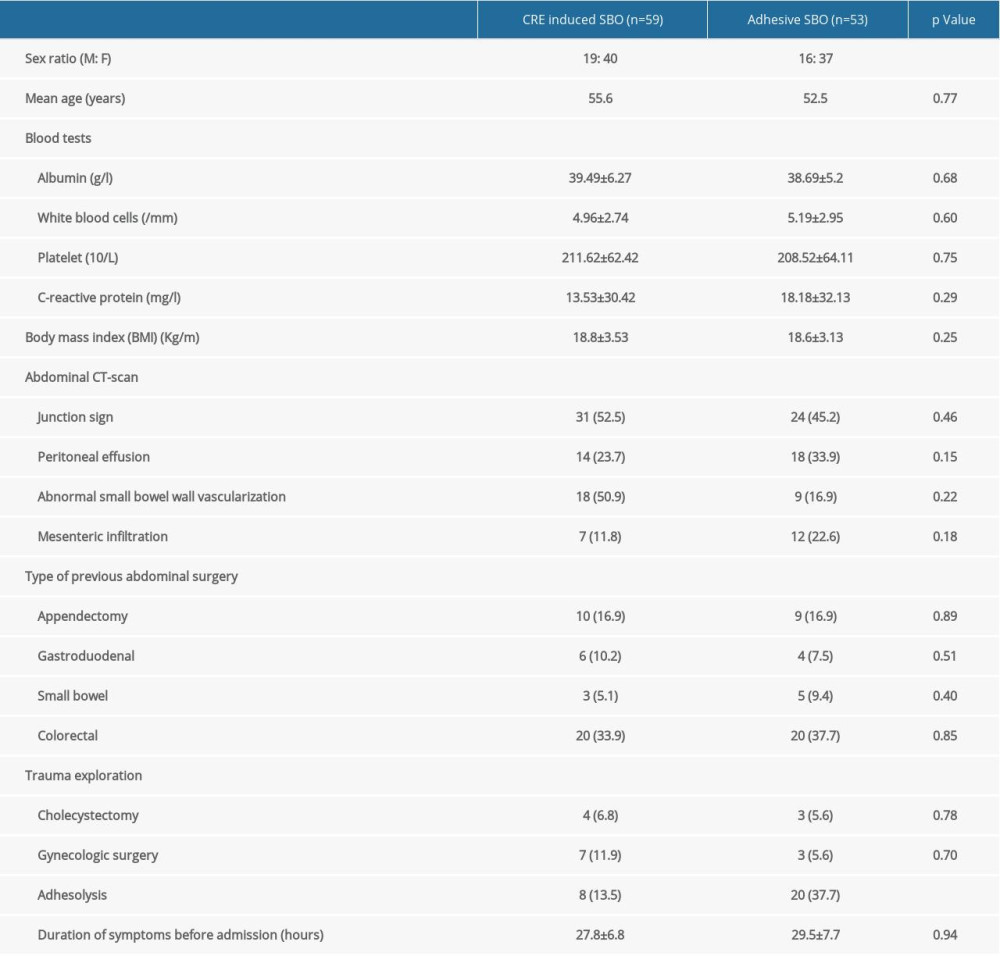 Table 2. Patient characteristics regarding Gastrografin challenge test.
Table 2. Patient characteristics regarding Gastrografin challenge test.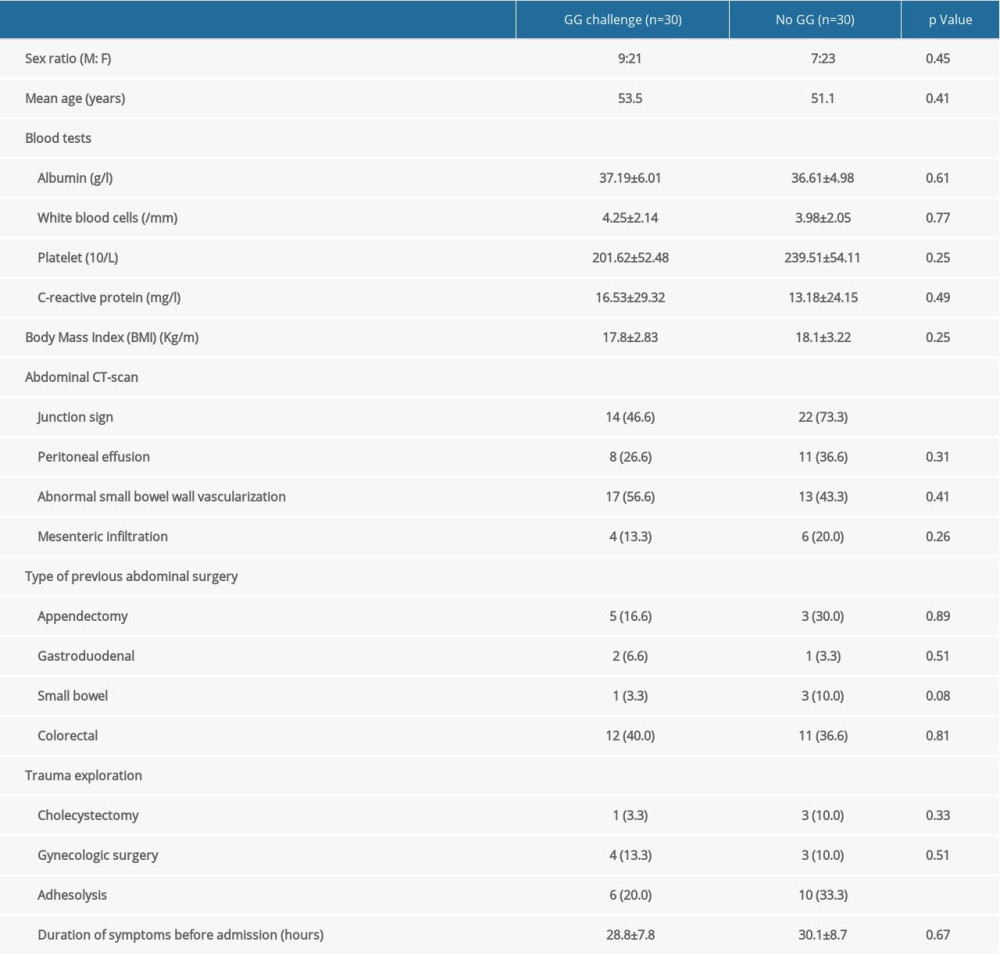 Table 3. Outcomes of RCE-induced SBO and adhesive SBO.
Table 3. Outcomes of RCE-induced SBO and adhesive SBO.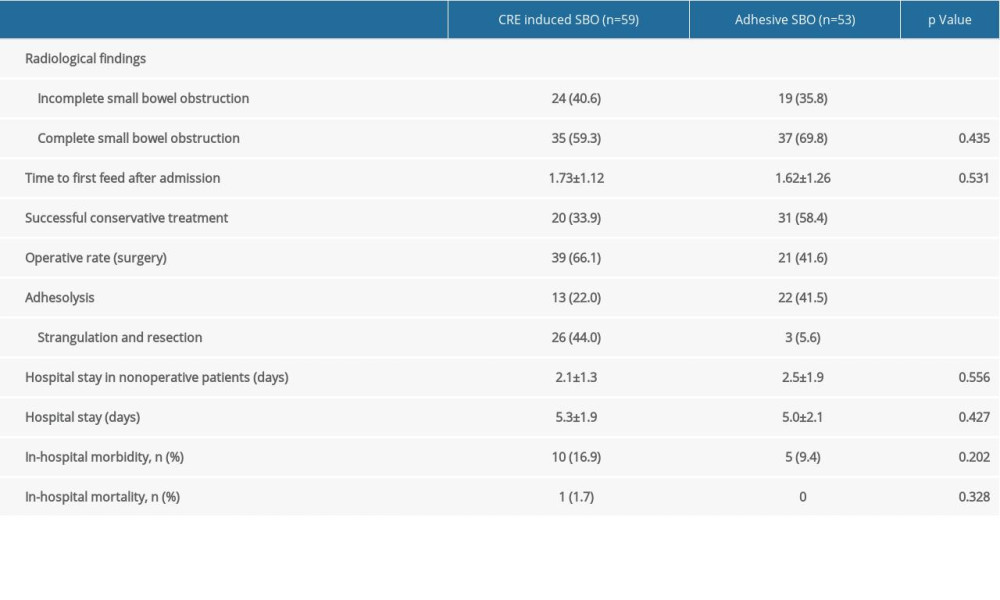 Table 4. Outcomes of patients with and without Gastrografin challenge.
Table 4. Outcomes of patients with and without Gastrografin challenge.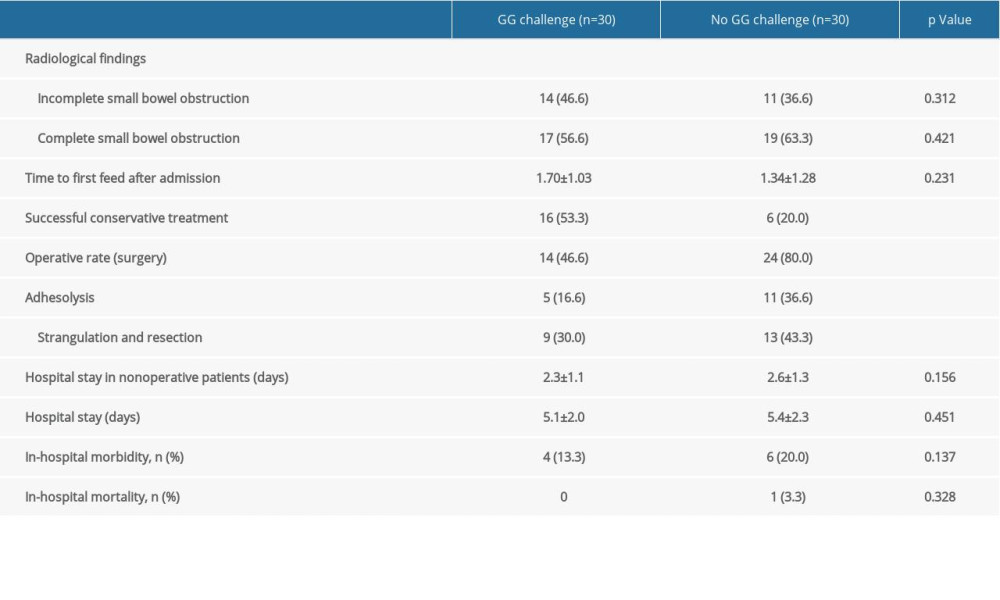 Table 5. Multivariable model for features associated with successful non-operative management in CRE-induced SBO and adhesive SBO.
Table 5. Multivariable model for features associated with successful non-operative management in CRE-induced SBO and adhesive SBO.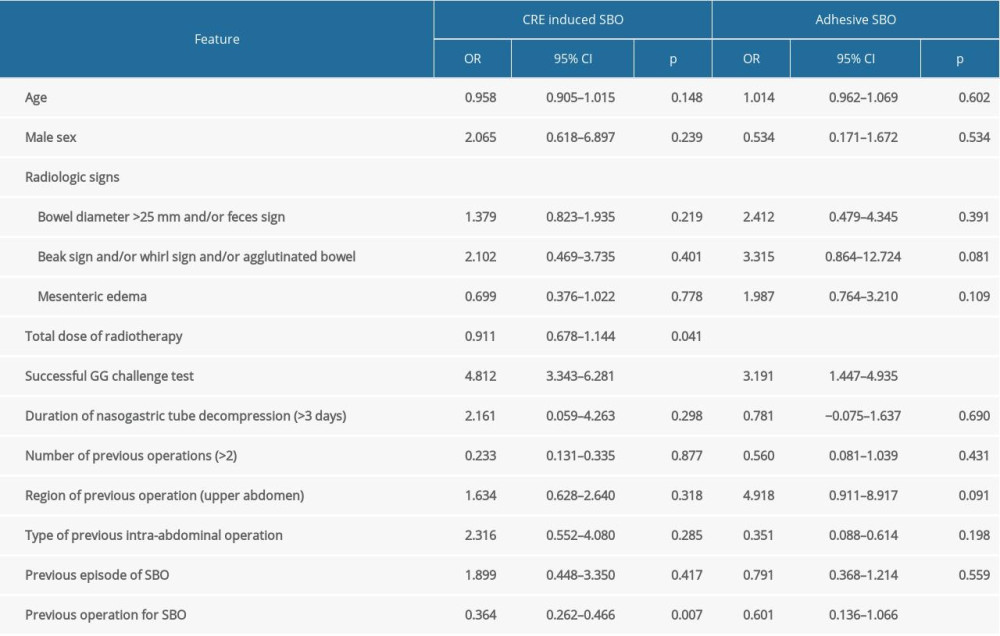 Table 6. Multivariable model for features associated with successful non-operative management in patients with and without Gastrografin challenge.
Table 6. Multivariable model for features associated with successful non-operative management in patients with and without Gastrografin challenge.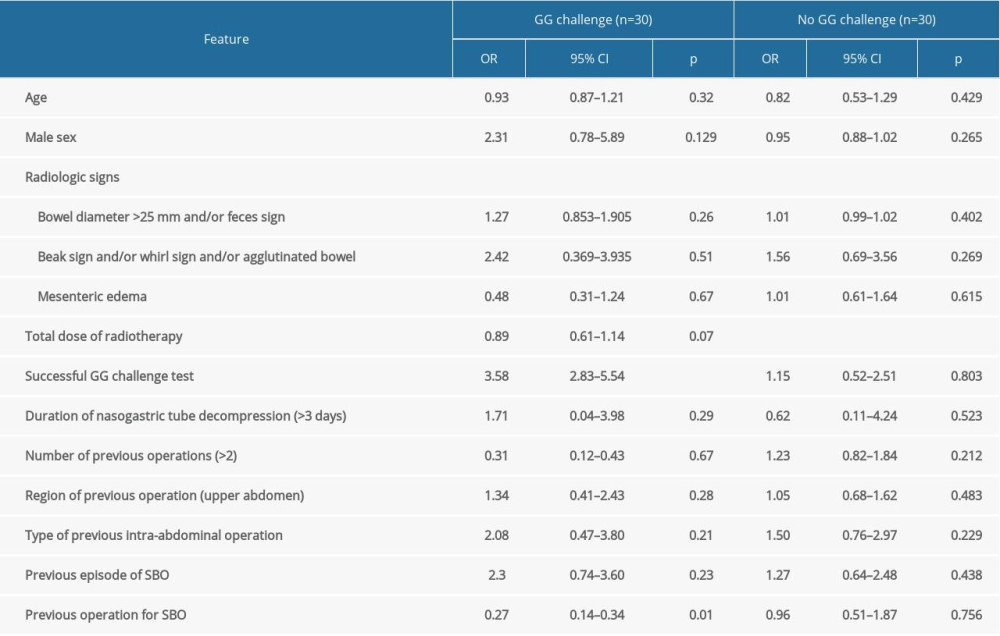 Table 7. Long-term outcomes for patients underwent conservative treatment.
Table 7. Long-term outcomes for patients underwent conservative treatment.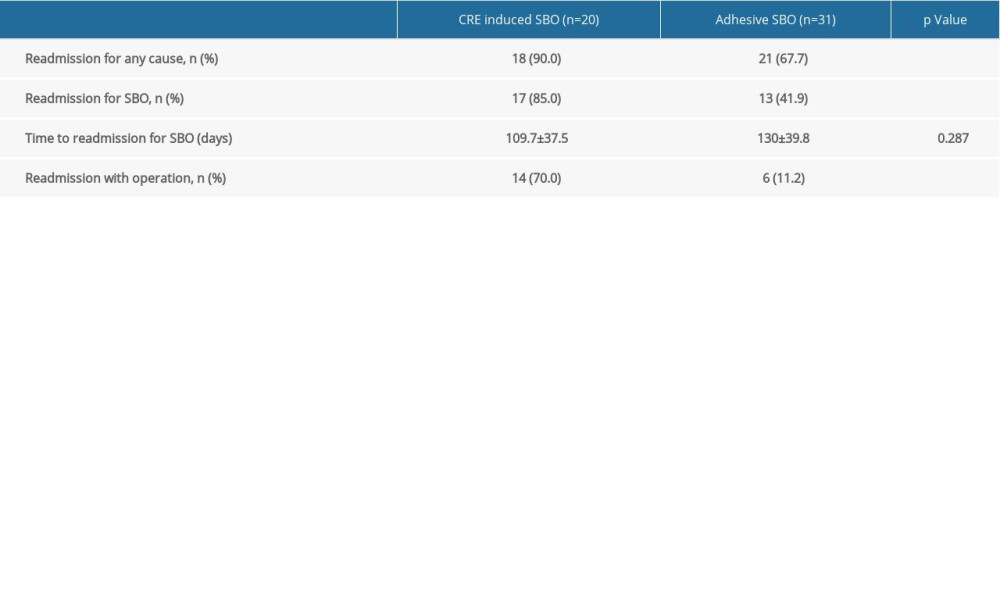 Table 8. Long-term outcomes for patients with and without Gastrografin challenge.
Table 8. Long-term outcomes for patients with and without Gastrografin challenge.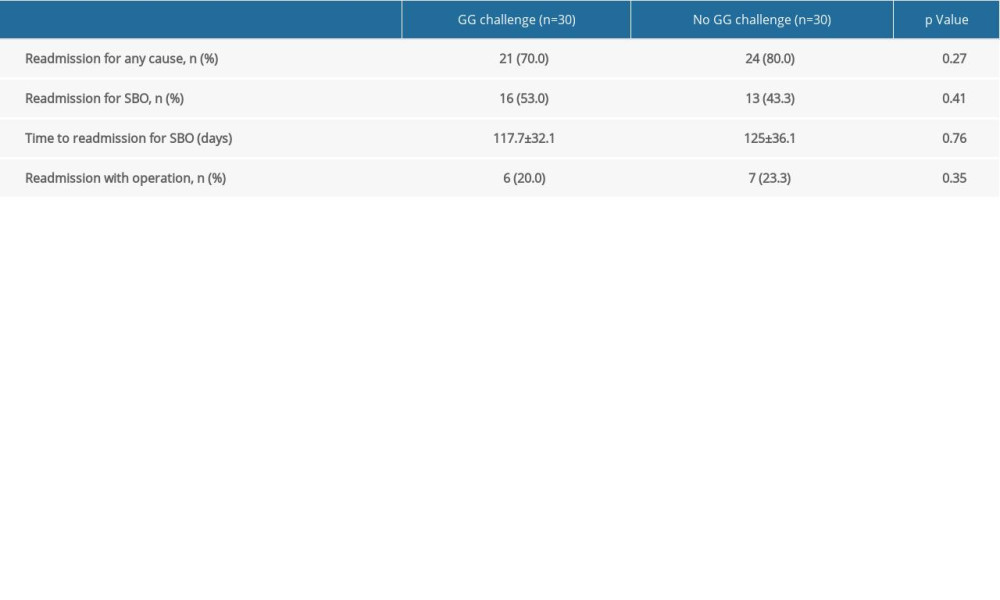
References
1. Ashburn JH, Kalady MF, Radiation-induced problems in colorectal surgery: Clin Colon Rectal Surg, 2016; 29; 85-91
2. Hauer-Jensen M, Denham JW, Andreyev HJ, Radiation enteropathy – pathogenesis, treatment and prevention: Nat Rev Gastroenterol Hepatol, 2014; 11; 470-79
3. Li N, Zhu W, Gong J, Ileal or ileocecal resection for chronic radiation enteritis with small bowel obstruction: Outcome and risk factors: Am J Surg, 2013; 206; 739-47
4. Wang J, Yao D, Zhang S, Laparoscopic surgery for radiation enteritis: J Surg Res, 2015; 194; 415-19
5. Theis VS, Sripadam R, Ramani V, Lal S, Chronic radiation enteritis: Clin Oncol (R Coll Radiol), 2010; 22; 70-83
6. Vather R, Josephson R, Jaung R, Gastrografin in prolonged postoperative ileus: A double-blinded randomized controlled trial: Ann Surg, 2015; 262; 23-30
7. Abbas SM, Bissett IP, Parry BR, Meta-analysis of oral water-soluble contrast agent in the management of adhesive small bowel obstruction: Br J Surg, 2007; 94; 404-11
8. Catena F, Di Saverio S, Kelly MD, Bologna guidelines for diagnosis and management of adhesive small bowel obstruction (ASBO): 2010 Evidence-Based Guidelines of the World Society of Emergency Surgery: World J Emerg Surg, 2011; 6; 5
9. Diaz JJ, Bokhari F, Mowery NT, Guidelines for management of small bowel obstruction: J Trauma, 2008; 64; 1651
10. Di Saverio S, Coccolini F, Galati M, Bologna guidelines for diagnosis and management of adhesive small bowel obstruction (ASBO): 2013 update of the evidence-based guidelines from the World Society Of Emergency Surgery ASBO Working Group: World J Emerg Surg, 2013; 8; 42.9
11. Di Saverio S, Catena F, Ansaloni L, Water-soluble contrast medium (gastrografin) value in adhesive small intestine obstruction (ASIO): A prospective, randomized, controlled, clinical trial: World J Surg, 2008; 32; 2293
12. Abbas SM, Bissett IP, Parry BR, Meta-analysis of oral water-soluble contrast agent in the management of adhesive small bowel obstruction: Br J Surg, 2007; 94; 404
13. Abbas S, Bissett IP, Parry BR, Oral water soluble contrast for the management of adhesive small bowel obstruction: Cochrane Database Syst Rev, 2007; 2007; CD004651
14. Ceresoli M, Coccolini F, Catena F, Water-soluble contrast agent in adhesive small bowel obstruction: A systematic review and meta-analysis of diagnostic and therapeutic value: Am J Surg, 2016; 211; 1114
15. Agha RA, Borrelli MR, Vella-Baldacchino Mfor the STROCSS Group, The STROCSS statement: Strengthening the reporting of cohort studies in surgery: Int J Surg, 2017; 46; 198-202
16. Mori H, Kaneoka Y, Maeda A, Determination of therapeutic strategy for adhesive small bowel obstruction using water-soluble contrast agents: An audit of 776 cases in a single center: Surgery, 2017; 162; 139-46
17. Khasawneh MA, Eiken PW, Srvantstyan B, Use of the gastrografin challenge in patients with a history of abdominal or pelvic malignancy: Surgery, 2013; 154; 769-75
18. Haule C, Ongom PA, Kimuli T, Efficacy of gastrografin compared with standard conservative treatment in management of adhesive small bowel obstruction at Mulago National Referral Hospital: J Clin Trials, 2013; 3; 1000144
19. Farid M, Fikry A, El Nakeeb A, Clinical impacts of oral gastrografin follow-through in adhesive small bowel obstruction (SBO): J Surg Res, 2010; 162; 170-76
20. Maglinte DDT, Klevin FM, Sandrasegaran K, Radiology of small bowel obstruction: Contemporary approach and controversies: Abdom Imaging, 2005; 30; 160-78
21. Katano T, Shimura T, Nishie H, The first management using intubation of a nasogastric tube with Gastrografin enterography or long tube for non-strangulated acute small bowel obstruction: A multicenter, randomized controlled trial: J Gastroenterol, 2020; 55(9); 858-67
22. Mulder MB, Hernandez M, Ray-Zack MD, A significant proportion of small bowel obstructions require >48 hours to resolve after gastrografin: J Surg Res, 2019; 233; 408-12
23. Stacey R, Green JT, Radiation-induced small bowel disease: Latest developments and clinical guidance: Ther Adv Chronic Dis, 2014; 5; 15-29
24. Tsai MS, Liang JT, Surgery is justified in patients with bowel obstruction due to radiation therapy: J Gastrointest Surg, 2006; 10; 575-82
25. Rahmani N, Mohammadpour RA, Khoshnood P, Prospective evaluation of oral gastrografin(R) in the management of postoperative adhesive small bowel obstruction: Indian J Surg, 2013; 75; 195-99
26. Goussous N, Eiken PW, Bannon MP: J Gastrointest Surg, 2013; 17(1); 110-16 discussion 116–17
27. Choi HK, Chu KW, Law WL, Therapeutic value of gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective randomized trial: Ann Surg, 2002; 236; 1-6
28. Stallmann HP, Borstlap J, Bollen TL, Water-soluble contrast agents in small bowel obstruction: A useful discriminator: Am J Roentgenol, 2012; 199; W783
29. Ishizuka M, Nagata H, Takagi K, Transnasal fine gastrointestinal fiberscope – guided long tube insertion for patients with small bowel obstruction: Gastrointest Surg, 2009; 13(3); 550-54
30. Schwenter F, Poletti PA, Platon A, Clinico radiological score for predicting the risk of strangulated small bowel obstruction: Br J Surg, 2010; 97(7); 1119-25
31. Bueno-Lledo J, Barber S, Vaque J, Adhesive small bowel obstruction: Predictive factors of lack of response in conservative management with gastrografin: Dig Surg, 2016; 33(1); 26-32
32. Miquel J, Biondo S, Kreisler E: Int J Colorectal Dis, 2017; 32(7); 1051-55
Tables
 Table 1. Patient characteristics of CRE-induced SBO and ASBO.
Table 1. Patient characteristics of CRE-induced SBO and ASBO. Table 2. Patient characteristics regarding Gastrografin challenge test.
Table 2. Patient characteristics regarding Gastrografin challenge test. Table 3. Outcomes of RCE-induced SBO and adhesive SBO.
Table 3. Outcomes of RCE-induced SBO and adhesive SBO. Table 4. Outcomes of patients with and without Gastrografin challenge.
Table 4. Outcomes of patients with and without Gastrografin challenge. Table 5. Multivariable model for features associated with successful non-operative management in CRE-induced SBO and adhesive SBO.
Table 5. Multivariable model for features associated with successful non-operative management in CRE-induced SBO and adhesive SBO. Table 6. Multivariable model for features associated with successful non-operative management in patients with and without Gastrografin challenge.
Table 6. Multivariable model for features associated with successful non-operative management in patients with and without Gastrografin challenge. Table 7. Long-term outcomes for patients underwent conservative treatment.
Table 7. Long-term outcomes for patients underwent conservative treatment. Table 8. Long-term outcomes for patients with and without Gastrografin challenge.
Table 8. Long-term outcomes for patients with and without Gastrografin challenge. In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








