03 July 2021: Clinical Research
Factors Associated with the Prognosis of Patients with Acute Myocardial Infarction and Cardiogenic Shock
Ke-Fu Feng1ABCDEF, Min Wu2BC, Li-Kun Ma1ADE*DOI: 10.12659/MSM.929996
Med Sci Monit 2021; 27:e929996
Abstract
BACKGROUND: Patients with acute myocardial infarction (AMI) complicated by cardiogenic shock (CS) usually have high mortality. This study aimed to identify factors related to the short-term survival of patients with AMI and CS treated by percutaneous coronary intervention (PCI) under intra-aortic balloon pump (IABP) support.
MATERIAL AND METHODS: This retrospective study included consecutive patients with AMI and CS treated with PCI under IABP support. Clinical characteristics, including the infarct-related artery, lesion number, aspiration catheter usage, conventional or delayed stenting, and thrombolysis in myocardial infarction (TIMI) flow grade before and after PCI, were collected. Patients were followed up postoperatively for 30 days. Multivariate logistic regression was used to identify factors associated with the 30-day mortality.
RESULTS: There were marked differences between the nonsurvival group (n=49) and the survival group (n=92) in the no-reflow after surgery (49.0% vs 14.1%, P<0.001), postoperative TIMI grade 3 flow (65.3% vs 91.3%, P<0.001), and delayed stent implantation (18.4% vs 37.0%, P=0.022). Factors associated with 30-day mortality were postoperative TIMI grade 3 flow (odds ratio [OR]: 0.227; 95% confidence interval [CI]: 0.076-0.678; P=0.008), delayed stent implantation (OR: 0.371; 95% CI: 0.139-0.988; P=0.047), and intraoperative no-reflow (OR: 2.737; 95% CI: 1.084-6.911; P=0.033).
CONCLUSIONS: For patients with AMI complicated by CS treated with emergent PCI under IABP support, prevention of no-reflow during surgery by delayed stent implantation can reduce postoperative 30-day mortality in selected cases.
Keywords: Intra-Aortic Balloon Pumping, percutaneous coronary intervention, Shock, Cardiogenic, ST elevation myocardial infarction
Background
Globally, ischemic heart disease is responsible for around 9 million deaths each year [1]. Acute myocardial infarction (AMI) is a major cause of mortality due to ischemic heart disease [2]. In the past decade, a 4-fold increase has occurred in hospital admissions for acute ST-segment elevation myocardial infarction (STEMI) in China, and the in-hospital mortality rate is around 10% [3]. Cardiogenic shock (CS) is a complication that occurs in 5–15% of AMI cases [4–6]. It manifests as a fall in systolic blood pressure (SBP), pulmonary congestion/elevated left-ventricular filling pressure, and impaired organ perfusion [7,8]. CS after AMI usually results from left ventricular dysfunction, although less common causes include acute mitral regurgitation, ventricular septal rupture, isolated right ventricular shock, tamponade, and cardiac rupture [7,8]. CS is a major cause of death after AMI, and it has been reported that the mortality rate of AMI patients with CS is around 50% [4–6].
Emergency percutaneous coronary intervention (PCI) is an effective treatment for restoring myocardial perfusion in AMI patients, and early PCI can reduce infarct size, mortality, and complications [9]. However, the postoperative 30-day mortality of AMI patients with CS remains at a high level even after reperfusion therapy [4,5], with reported in-hospital and 2-year mortality rates approaching 30% and 50%, respectively [10,11]. The early identification of high-risk AMI patients with CS may help clinicians select strategies to improve prognosis and reduce mortality.
Theoretically, the use of an intra-aortic balloon pump (IABP) can increase coronary perfusion and cardiac output, reduce afterload, decrease myocardial oxygen consumption, and improve the hemodynamics [12]. Although the IABP may be expected to reduce mortality and improve prognosis in AMI patients with CS, its clinical value in this patient population remains controversial. The SHOCK study indicated that IABP support reduced the 30-day mortality in AMI patients with CS, particularly when it was administered with thrombolytic therapy [13,14]. Although a meta-analysis by Romeo et al [15] also identified a beneficial effect of IABP support in combination with thrombolytic therapy (an 18% reduction in 30-day mortality rate), the short-term mortality was increased by 6% when IABP support was administered in patients treated with PCI. Similar findings have also been reported by Sjauw et al [16]. Romeo et al [15] also concluded that the efficacy of IABP-supported thrombolytic therapy was better than that of PCI. Two studies concluded that IABP support failed to reduce the 30-day mortality in patients for whom early revascularization was planned [17,18]; another 2 investigations indicated no effect of IABP on the 30-day mortality in AMI patients with CS who received PCI [19,20].
Despite the evidence that IABP may not reduce short-term mortality in AMI patients with CS, IABP support is still used to improve hemodynamics in many AMI patients with CS. However, data are limited regarding the factors related to the prognosis of AMI patients with CS treated with PCI and IABP support. Therefore, this retrospective study investigated the clinical factors affecting the prognosis of AMI patients with CS who were treated with PCI and IABP support. Our findings could help clinicians identify patients at high risk of poor prognosis and potentially implement strategies to reduce the risk of mortality. This article was created in accordance with the STROBE reporting checklist.
Material and Methods
STUDY DESIGN AND SUBJECTS:
This retrospective study included consecutive AMI patients with CS treated with PCI under IABP support at the Cardiovascular Department of the First Affiliated Hospital of the University of Science and Technology of China between January 2011 and June 2018. The inclusion criteria were as follows: (1) patients had a diagnosis of AMI and CS based on coronary angiography showing complete occlusion of the infarct-related artery (IRA) or severe residual stenosis (>70%) of major vessels; (2) patients received emergency PCI treatment under IABP support; and (3) only the IRA was treated. The exclusion criteria were as follows: (1) patients had other heart diseases, such as rheumatic heart disease, hyperthyroid heart disease, or dilated cardiomyopathy; (2) patients were diagnosed with AMI caused by aortic dissection; (3) patients had AMI in the prior 1 month; and (4) patients had comorbidities that could affect their prognosis, such as severe infection, malignant tumor, hematologic disease, or immunologic disorder. The AMI was diagnosed based on the Fourth Universal Definition of Myocardial Infarction [21]. The diagnostic criteria for CS were as follows: (1) patients had hypotension due to myocardial dysfunction (with hypovolemia excluded), defined as SBP <90 mmHg (1 mmHg=0.133 kPa) for ≥30 min or SBP decreased by >30% for ≥30 min in patients with hypertension; and (2) patients had clinical signs of hypoperfusion, such as cyanosis, cold limbs, sweating, mental state changes, persistent oliguria, and pulmonary congestion [7,8].
The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This study was approved by the Ethics Committee of the First Affiliated Hospital of USTC, Division of Life Sciences and Medicine, University of Science and Technology of China (No. 2019KY-61) and informed consent for this retrospective analysis was waived.
IMPLANTATION AND WITHDRAWAL OF IABP:
All patients underwent IABP before PCI. The intra-aortic balloon catheter (Linear 7.5 Fr; 34 or 40 cm3; Maquet, Rastatt, Germany) was implanted via the femoral approach with the modified Seldinger technique. The intra-aortic balloon was connected to a Datascope CS100 pump (Maquet). After the appropriate positioning of the catheter was confirmed, the IABP was triggered to operate in full assistance (1: 1) mode. The IABP was withdrawn when the hemodynamics were stable, based on the following criteria [22,23]: (1) cardiac index >2.5 L/min/m2; (2) urine volume > l mL/kg/h; (3) blood pressure remained stable after withdrawal of vasoactive drugs; (4) respiration was stable and results from arterial blood gas analysis were normal; and (5) the hemodynamic parameters remained stable for about 1 h when the IABP frequency was reduced to 1: 2. The average time of IABP in the delayed stenting group was 5.6 days in our study.
EMERGENCY CORONARY ANGIOGRAPHY:
All patients had indications for emergency interventional therapy and received antithrombotic therapy with aspirin (300 mg), clopidogrel (600 mg) [24], and low-molecular-weight heparin. Coronary angiography was performed through the radial or femoral artery approach. Left-side and right-side coronary angiographies with multiposition projection were performed using a multifunction or Judkins catheter to identify the IRAs and evaluate the coronary blood flow and the lesioned vessels with severe stenosis.
PERCUTANEOUS CORONARY INTERVENTION:
All PCI procedures were carried out by doctors of Associate Chief Physician grade or higher who had more than 5 years of experience in interventional therapy. Heparin (100 U/kg body weight) was administered via the sheath before surgery. PCI was performed using the radial or femoral artery approach. For a completely occluded IRA, a thrombus aspiration catheter was used to aspirate 3–5 times during the procedure. If the suction catheter could not pass the stenosed IRA, a 1.5/15 mm or 2.0/15 mm predilated balloon was used for dilation with 8–10 atm, and thrombus aspiration was then performed repeatedly. Following aspiration, a glycoprotein (GP)IIb/IIIa receptor antagonist (tirofiban, 10 μg/kg; Yuanda Pharmaceutical Co. Ltd., Wuhan, China) was selectively and slowly injected through the suction catheter into the site of IRA occlusion; the process was repeated if necessary. Delayed stenting was conducted after antithrombotic therapy for 2–7 days in patients with the following characteristics: (1) IRA antegrade blood flow was greater than or equal to thrombolysis in myocardial infarction (TIMI) grade 2 during angiography or returned to greater than or equal to TIMI grade 2 after low-pressure predilation with a small balloon and/or thrombus aspiration [25]; and (2) the hemodynamics were stable during IABP support with only low doses of vasoactive drugs required [25,26]. Otherwise, regular (immediate) stenting was conducted. If no-reflow occurred during surgery [27], a GPIIb/IIIa receptor antagonist was injected into the coronary artery after aspiration with the suction catheter to improve the coronary blood flow. After surgery, all patients received a GPIIb/IIIa receptor antagonist (0.1 μg/kg/min for 36 h) and dual antiplatelet therapy (aspirin [100 mg] plus clopidogrel [75 mg]).
GROUPING AND FOLLOW-UP:
Postoperatively, the patients were followed up once weekly for 30 days. Follow-up was conducted via hospital visit or telephone after discharge from the hospital. For the analysis, the patients were divided into a survival group and a nonsurvival group based on the clinical outcome during the postoperative 30-day follow-up.
COLLECTION OF CLINICAL DATA:
The following clinical data were extracted from the medical records: sex, age, and body mass index; history of smoking; hypertension, diabetes, or hyperlipidemia; serum creatinine; SBP; diastolic blood pressure (DBP); cardiac troponin I; blood glucose; glycated hemoglobin (HbA1c); high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C) on admission; prehospital thrombolysis history; onset to balloon time; locations of lesions identified during coronary angiography; TIMI flow grade before PCI (grade 0, no perfusion; grade 1, penetration without perfusion; grade 2, partial perfusion; grade 3, complete perfusion) [28]; use of aspiration catheter; conventional or delayed stenting; coronary blood flow after coronary stenting; no-reflow after coronary stenting [29]; and survival outcome. Any adverse events or complications were also recorded.
STATISTICAL ANALYSIS:
SPSS version 20.0 statistical software was used for data analysis (IBM Corp., Armonk, NY, USA). Normally distributed continuous data are expressed as mean±standard deviation and were compared between groups with
Results
BASELINE CLINICAL CHARACTERISTICS OF PATIENTS:
Patient disposition is shown in Figure 1. Among 148 patients, 5 were excluded due to failure of IABP implantation (n=3), concomitant lung cancer (n=1), and death before interventional therapy (n=1). Another 2 patients were excluded due to the use of extracorporeal membrane oxygenation and IABP support after surgery (n=1) and being lost to follow-up (n=1). Therefore, 141 patients were included in the final analysis. The postoperative 30-day mortality rate was 34.8% (49/141). The causes of death were severe heart failure or blood pressure fluctuation (n=44), malignant ventricular arrhythmia (n=2), moderate-to-severe bleeding (n=2), and stent thrombosis (n=1). The baseline clinical characteristics of 92 patients in the survival group and 49 patients in the nonsurvival group are shown in Table 1. There were no significant differences between groups in the smoking status; prevalence of hypertension, diabetes, or hyperlipidemia; history of thrombolysis; onset to balloon time [30]; prevalence of abnormal creatine level (≥133 μmol/L); body mass index; history of myocardial infarction; history of PCI; history of stroke; SBP; DBP; cardiac troponin I; blood glucose; HbA1c; HDL-C; or LDL-C (Table 1). However, the patients in the nonsurvival group were significantly older (71.1±11.2 years vs 67.0±12.2 years, P=0.016) and the proportion of men in the nonsurvival group was significantly lower than in the survival group (67.3% vs 82.6%, P=0.039).
CORONARY ANGIOGRAPHY AND PCI DATA:
There were no significant differences between the survival group and the nonsurvival group in the IRA, use of aspiration, number of lesions, and preoperative blood flow (Table 2). However, in comparison with the survival group, the patients in the nonsurvival group had a significantly higher rate of no-reflow after surgery (49.0% vs 14.1%, P<0.001) and a markedly lower rate of postoperative TIMI grade 3 blood flow after stent implantation (65.3% vs 91.3%, P<0.001). In addition, the proportion of patients undergoing delayed stent implantation in the nonsurvival group was significantly smaller than in the survival group (18.4% vs 37.0%, P=0.022).
SURVIVAL ANALYSIS:
Among the 141 patients in the present study, 98 patients were treated with conventional stenting and 43 patients with delayed stenting. During the 30-day follow-up, death was noted in 40 patients (40/98; 40.8%) who had received conventional stenting and 9 patients (9/43; 20.9%) who had undergone delayed stenting. Kaplan-Meier analysis (Figure 2) revealed significantly poorer survival in the patients treated with conventional stenting than in those treated with delayed stenting (P=0.030, log-rank test).
FACTORS ASSOCIATED WITH 30-DAY MORTALITY:
The following independent variables were included in the univariate logistic regression analysis: age, sex, postoperative TIMI grade 3 blood flow, no-reflow during surgery, and delayed stent implantation. Based on the results of univariate analysis (Table 3), sex was excluded from the multivariate regression model. The multivariate analysis showed postoperative TIMI grade 3 blood flow (OR: 0.227; 95% CI: 0.076–0.678; P=0.008) and delayed stent implantation (OR: 0.371; 95% CI: 0.139–0.988; P=0.047) were associated with lower odds ratio of death during the 30-day follow-up, whereas intraoperative no-reflow (OR: 2.737; 95% CI: 1.084–6.911; P=0.033) was associated with higher odds ratio of death (Table 3).
ADVERSE EVENTS:
The most common adverse event was no-reflow during surgery, which was noted in 13 of 92 patients (14.1%) in the survival group and 24 of 49 patients (49.0%) in the nonsurvival group (P<0.01). Less common adverse events included malignant arrhythmia, stent thrombosis, stroke, and bleeding, and there were no significant differences in these less common adverse events between the 2 groups (Table 4).
Discussion
Our study showed marked differences in the age, sex, postoperative no-reflow, postoperative TIMI grade 3 blood flow, and delayed stenting between the nonsurvival group and the survival group, whereas no differences were observed in other baseline characteristics, IRA, use of aspiration, number of lesions, and preoperative blood flow. Importantly, factors associated with 30-day mortality included postoperative TIMI grade 3 flow (protective), delayed stent implantation (protective), and intraoperative no-reflow (risk factor). These findings indicate that achieving grade 3 blood flow after surgery, preventing intraoperative no-reflow, and delayed stenting in selected cases can reduce the postoperative 30-day mortality of AMI patients with CS treated with emergency PCI under IABP support.
The incidence of CS in AMI patients is around 10% [4–6]. The prognosis of AMI patients with CS is poor, and CS has been a major cause of death after AMI. In the present study, the 30-day mortality rate was 34.8%, which was consistent with previously reported rates. Seyfarth et al [31] reported the 30-day mortality rate was 46% despite PCI under IABP support. In the IABP-SHOCKII study, the 30-day mortality rate in AMI patients with CS after emergency reperfusion therapy was about 40%, regardless of use of IABP support [18]. A “real-life” experience reported by de la Espriella-Juan et al [19] also revealed no difference in the 30-day mortality between patients with and without IABP support (29.5% vs 27.6%) among AMI patients with CS treated with PCI. A meta-analysis also concluded that IABP support may not contribute to improved short-term survival in AMI patients with CS after PCI [20]. Thus, IABP support may not improve the short-term survival of patients treated with PCI, despite its theoretical advantages [12] and efficacy in the setting of thrombolytic therapy [13–15]. In the present study, all patients were treated with IABP before surgery due to hemodynamic disorders. Although current guidelines do not recommend routine prophylactic IABP in AMI patients with CS, it has been shown that IABP may improve myocardial perfusion and disruption of the shock spiral [32]. Furthermore, IABP support after PCI has been shown to increase the mortality rate [32,33], suggesting that IABP should be used before PCI.
Many factors potentially affect the prognosis of AMI patients with CS. In the present study, multivariate logistic regression analysis revealed that postoperative TIMI grade 3 blood flow and delayed stenting were associated with reduced odds of death in the 30 days after PCI. It has been well established that TIMI grade 3 blood flow after PCI in AMI patients is a predictor of survival [34], and this has also been observed in AMI patients with CS [35]. In our study, delayed stenting appeared to be associated with a lower incidence of no-reflow after stenting. Theoretically, AMI patients with CS have a hemodynamic disorder, and no-reflow due to the obstruction of a small thrombus would likely have a substantial impact on the therapeutic effects of emergency PCI. Currently, the value of delayed stenting is still controversial in AMI patients. The DEFER-STEMI study indicated that delayed stenting in patients with STEMI could reduce the incidence of postoperative no-reflow, increase the occurrence of TIMI grade 3 blood flow, suppress the incidence of coronary microvascular embolization, reduce infarct size, and increase the viable myocardium after stenting [36]. However, the above results were not confirmed by the DANAMI 3-DEFER study, which revealed that, although left ventricular ejection fraction was superior in the delayed stenting group to that in the conventional stenting group at 18 months after surgery, there were no significant differences between groups in the primary endpoints (postoperative 2-year all-cause mortality, hospital admission due to heart failure, recurrent myocardial infarction, and unplanned target vessel reconstruction) [37]. The investigators speculated that the delayed stenting did not improve the prognosis of these patients. However, further analysis indicated that most of the patients enrolled in the study had relatively good cardiac function, and only 7% of patients had the cardiac function of Killip class II–V. Therefore, the effects on the hemodynamics of AMI patients who have relatively good cardiac function and small infarct size would likely be limited unless there is severe no-reflow. This might explain the similar incidence of major adverse cardiovascular events despite a superior LVEF at 18 months [37]. As the effect of delayed stenting on the prognosis is still unclear, Pascal et al [25] and Belle et al [26] further assessed the value of modified delayed stenting (MIMI technique). However, the results were still inconsistent. Pascal et al [25] found that delayed stenting could reduce postoperative no-reflow and improve TIMI blood flow after coronary stenting. Furthermore, postoperative follow-up for 1 year showed the incidence of major adverse cardiovascular events was significantly lower in patients receiving delayed stenting than in those receiving conventional stenting. However, Belle et al [26] found that delayed stenting did not reduce the area of infarcted myocardium 5 days after operation and the incidence of major adverse cardiovascular events at 6 months. Further analysis showed that the patients included in the study of Belle et al [26] had certain characteristics (grade I–II cardiac function in all patients, right coronary lesions in most patients [50.7% vs 47.8%], and a relatively short time to delayed stenting [36 h]). In addition, the most important disadvantage of delayed stenting was the re-occlusion of the revascularized IRA. Theoretically, IABP support can increase the coronary blood supply in the diastolic phase and reduce the risk of IRA re-occlusion [12]. In the present study, the modified delayed stenting (MIMI technique) was used under IABP support. In the delayed stenting group, the stent was implanted at 2–7 days after antithrombotic therapy, which minimized the risk of IRA re-occlusion, improved the coronary blood supply, and decreased the incidence of no-reflow during surgery. Furthermore, in this study, we found that age was a risk factor in univariate analysis, but it was eliminated in multivariate analysis. This finding might be related to selection bias and the small sample size in the study, the results of which need to be confirmed by randomized controlled trial or more studies with a large sample size.
In this study, 6 patients with thrombolysis and recanalization received delayed stenting after intensive antithrombotic therapy, no-reflow was not found during surgery, and the prognosis was relatively good. In our patients, the incidence of no-reflow (including transient slow blood flow) was 32.6% (32/98) in those receiving conventional stenting and only 11.6% (5/43) in those undergoing delayed stenting. It is also worth noting that 49.0% of patients in the nonsurvival group had no-reflow during surgery, compared with 14.1% in the survival group. Thirteen patients with no-reflow developed ventricular tachycardia, ventricular fibrillation, or decreased blood pressure that eventually resulting in death. Thus, the mortality after PCI may be related to the no-reflow during conventional stenting due to the distal microembolization of the coronary artery or other factors [38]. Notably, the multivariate analysis in the present study identified no-reflow during surgery as an independent risk factor for postoperative death.
There were several limitations in the present study. This was a retrospective study, and there may have been selection bias or information bias. Since this study involved only a single center, the generalizability of the results is unknown. The sample size was relatively small, and thus the study may have been underpowered to detect some real differences between groups. The follow-up was limited to 30 days, and longer-term outcomes were unclear in these patients. In addition, there were several limitations when the coronary angiography was used in the diagnosis of postoperative no-reflow. Further, the optimal timing of delayed stenting was not examined.
Conclusions
For patients with AMI complicated by CS treated with emergent PCI under IABP support, prevention of no-reflow during surgery by delayed stent implantation can reduce postoperative 30-day mortality in selected cases. More clinical studies with a large sample size are needed to confirm our findings.
Figures
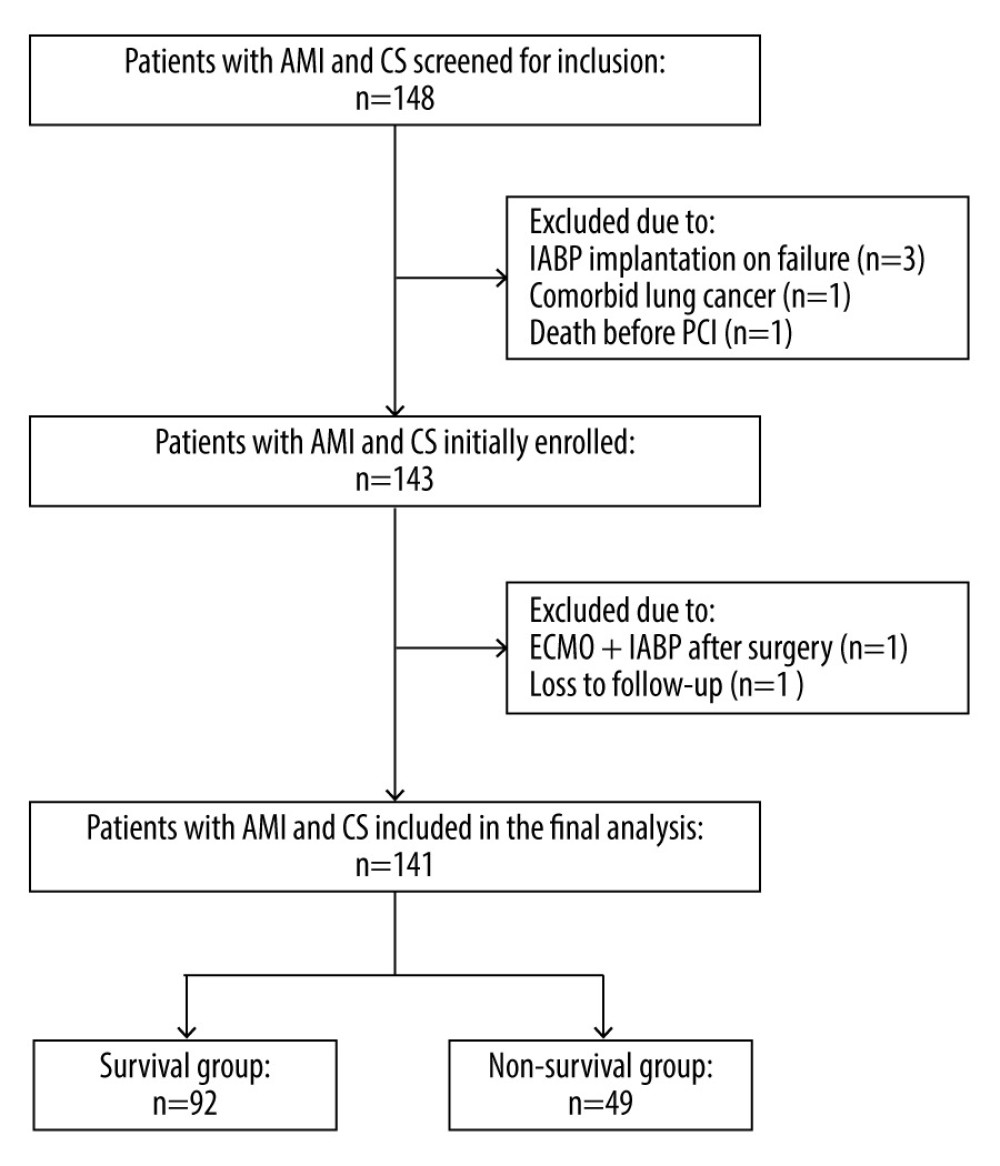 Figure 1. Patient disposition. AMI – acute myocardial infarction; CS – cardiogenic shock; ECMO – extracorporeal membrane oxygenation; IABP – intra-aortic balloon pump; PCI – percutaneous coronary intervention.
Figure 1. Patient disposition. AMI – acute myocardial infarction; CS – cardiogenic shock; ECMO – extracorporeal membrane oxygenation; IABP – intra-aortic balloon pump; PCI – percutaneous coronary intervention. 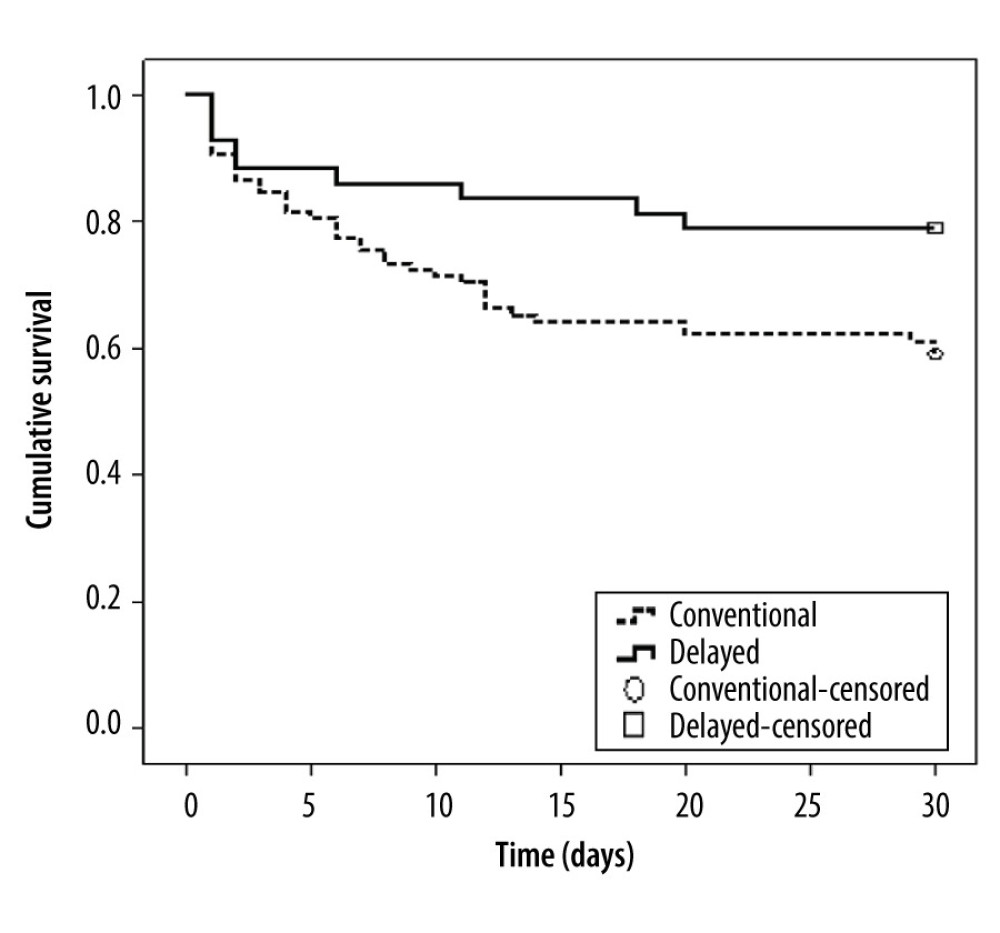 Figure 2. Kaplan-Meier analysis of survival in patients receiving conventional stenting and those receiving delayed stenting. Log-rank test: P=0.03.
Figure 2. Kaplan-Meier analysis of survival in patients receiving conventional stenting and those receiving delayed stenting. Log-rank test: P=0.03. References
1. GBD 2015 Mortality and Causes of Death Collaborators, Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: A systematic analysis for the Global Burden of Disease Study 2015: Lancet, 2016; 388(10053); 1459-544
2. Reed GW, Rossi JE, Cannon CP, Acute myocardial infarction: Lancet, 2017; 389; 197-210
3. Li J, Li X, Wang Q, ST-segment elevation myocardial infarction in China from 2001 to 2011 (the China PEACE-Retrospective Acute Myocardial Infarction Study): A retrospective analysis of hospital data: Lancet, 2015; 385; 441-51
4. Aissaoui N, Puymirat E, Tabone X, Improved outcome of cardiogenic shock at the acute stage of myocardial infarction: A report from the USIK 1995, USIC 2000, and FAST-MI French nationwide registries: Eur Heart J, 2012; 33; 2535-43
5. Goldberg RJ, Spencer FA, Gore JM, Thirty-year trends (1975 to 2005) in the magnitude of, management of, and hospital death rates associated with cardiogenic shock in patients with acute myocardial infarction: A population-based perspective: Circulation, 2009; 119; 1211-19
6. Jeger RV, Radovanovic D, Hunziker PR, Ten-year trends in the incidence and treatment of cardiogenic shock: Ann Intern Med, 2008; 149; 618-26
7. Thiele H, Ohman EM, Desch S, Management of cardiogenic shock: Eur Heart J, 2015; 36; 1223-30
8. Khalid L, Dhakam SH, A review of cardiogenic shock in acute myocardial infarction: Curr Cardiol Rev, 2008; 4; 34-40
9. Gaffar R, Habib B, Filion KB, Optimal timing of complete revascularization in acute coronary syndrome: A systematic review and meta-analysis: J Am Heart Assoc, 2017; 6(4); e005381
10. Krishnan U, Brejt JA, Schulman-Marcus J, Characteristics of hospitalizations for cardiogenic shock after acute myocardial infarction in the United States: Int J Cardiol, 2017; 244; 213-19
11. Vergara R, Valenti R, Migliorini A, A new risk score to predict long-term cardiac mortality in patients with acute myocardial infarction complicated by cardiogenic shock and treated with primary percutaneous intervention: Am J Cardiol, 2017; 119; 351-54
12. de Waha S, Desch S, Eitel I, Intra-aortic balloon counterpulsation – basic principles and clinical evidence: Vascul Pharmacol, 2014; 60; 52-56
13. Sanborn TA, Sleeper LA, Bates ER, Impact of thrombolysis, intra-aortic balloon pump counterpulsation, and their combination in cardiogenic shock complicating acute myocardial infarction: A report from the SHOCK Trial Registry. SHould we emergently revascularize Occluded Coronaries for cardiogenic shocK?: J Am Coll Cardiol, 2000; 36; 1123-29
14. Hochman JS, Buller CE, Sleeper LA, Cardiogenic shock complicating acute myocardial infarction – etiologies, management and outcome: A report from the SHOCK Trial Registry. SHould we emergently revascularize Occluded Coronaries for cardiogenic shocK?: J Am Coll Cardiol, 2000; 36; 1063-70
15. Romeo F, Acconcia MC, Sergi D, The outcome of intra-aortic balloon pump support in acute myocardial infarction complicated by cardiogenic shock according to the type of revascularization: A comprehensive meta-analysis: Am Heart J, 2013; 165; 679-92
16. Sjauw KD, Engstrom AE, Vis MM, A systematic review and meta-analysis of intra-aortic balloon pump therapy in ST-elevation myocardial infarction: Should we change the guidelines?: Eur Heart J, 2009; 30; 459-68
17. Khashan MY, Pinsky MR, Does intra-aortic balloon support for myocardial infarction with cardiogenic shock improve outcome?: Crit Care, 2013; 17; 307
18. Thiele H, Zeymer U, Neumann FJ, Intraaortic balloon support for myocardial infarction with cardiogenic shock: N Engl J Med, 2012; 367; 1287-96
19. de la Espriella-Juan R, Valls-Serral A, Trejo-Velasco B, Impact of intra-aortic balloon pump on short-term clinical outcomes in ST-elevation myocardial infarction complicated by cardiogenic shock: A “real life” single center experience: Med Intensiva, 2017; 41; 86-93
20. Zheng XY, Wang Y, Chen Y, The effectiveness of intra-aortic balloon pump for myocardial infarction in patients with or without cardiogenic shock: A meta-analysis and systematic review: BMC Cardiovasc Disord, 2016; 16; 148
21. Thygesen K, Alpert JS, Jaffe AS, Fourth universal definition of myocardial infarction (2018): Glob Heart, 2018; 13; 305-38
22. Lewis PA, Mullany DV, Courtney M, Coyer F, Australasian trends in intra-aortic balloon counterpulsation weaning: Results of a postal survey: Crit Care Resusc, 2006; 8; 361-67
23. Onorati F, Santini F, Amoncelli E, How should I wean my next intra-aortic balloon pump? Differences between progressive volume weaning and rate weaning: J Thorac Cardiovasc Surg, 2013; 145; 1214-21
24. Neumann FJ, Sousa-Uva M, Ahlsson A, 2018 ESC/EACTS Guidelines on myocardial revascularization: Eur Heart J, 2019; 40; 87-165
25. Pascal J, Veugeois A, Slama M, Delayed stenting for ST-elevation acute myocardial infarction in daily practice: A single-centre experience: Can J Cardiol, 2016; 32; 988-95
26. Belle L, Motreff P, Mangin L, Comparison of immediate with delayed stenting using the Minimalist Immediate Mechanical Intervention approach in acute ST-segment-elevation myocardial infarction: The MIMI study: Circ Cardiovasc Interv, 2016; 9; e003388
27. Rezkalla SH, Kloner RA, Coronary no-reflow phenomenon: From the experimental laboratory to the cardiac catheterization laboratory: Catheter Cardiovasc Interv, 2008; 72; 950-57
28. TIMI Study Group, The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings: N Engl J Med, 1985; 312; 932-36
29. Rezkalla SH, Stankowski RV, Hanna J, Management of no-reflow phenomenon in the catheterization laboratory: JACC Cardiovasc Interv, 2017; 10; 215-23
30. van Diepen S, Katz JN, Albert NM, Contemporary management of cardiogenic shock: A scientific statement from the American Heart Association: Circulation, 2017; 136; e232-68
31. Seyfarth M, Sibbing D, Bauer I, A randomized clinical trial to evaluate the safety and efficacy of a percutaneous left ventricular assist device versus intra-aortic balloon pumping for treatment of cardiogenic shock caused by myocardial infarction: J Am Coll Cardiol, 2008; 52; 1584-88
32. Yuan L, Nie SP, Efficacy of intra-aortic balloon pump before versus after primary percutaneous coronary intervention in patients with cardiogenic shock from ST-elevation myocardial infarction: Chin Med J (Engl), 2016; 129; 1400-5
33. Schwarz B, Abdel-Wahab M, Robinson DR, Predictors of mortality in patients with cardiogenic shock treated with primary percutaneous coronary intervention and intra-aortic balloon counterpulsation: Med Klin Intensivmed Notfmed, 2016; 111; 715-22
34. Halkin A, Singh M, Nikolsky E, Prediction of mortality after primary percutaneous coronary intervention for acute myocardial infarction: The CADILLAC risk score: J Am Coll Cardiol, 2005; 45; 1397-405
35. Poss J, Koster J, Fuernau G, Risk stratification for patients in cardiogenic shock after acute myocardial infarction: J Am Coll Cardiol, 2017; 69; 1913-20
36. Carrick D, Oldroyd KG, McEntegart M, A randomized trial of deferred stenting versus immediate stenting to prevent no- or slow-reflow in acute ST-segment elevation myocardial infarction (DEFER-STEMI): J Am Coll Cardiol, 2014; 63; 2088-98
37. Kelbaek H, Hofsten DE, Kober L, Deferred versus conventional stent implantation in patients with ST-segment elevation myocardial infarction (DANAMI 3-DEFER): An open-label, randomised controlled trial: Lancet, 2016; 387; 2199-206
38. Gupta S, Gupta MM, No reflow phenomenon in percutaneous coronary interventions in ST-segment elevation myocardial infarction: Indian Heart J, 2016; 68; 539-51
Figures
 Figure 1. Patient disposition. AMI – acute myocardial infarction; CS – cardiogenic shock; ECMO – extracorporeal membrane oxygenation; IABP – intra-aortic balloon pump; PCI – percutaneous coronary intervention.
Figure 1. Patient disposition. AMI – acute myocardial infarction; CS – cardiogenic shock; ECMO – extracorporeal membrane oxygenation; IABP – intra-aortic balloon pump; PCI – percutaneous coronary intervention. Figure 2. Kaplan-Meier analysis of survival in patients receiving conventional stenting and those receiving delayed stenting. Log-rank test: P=0.03.
Figure 2. Kaplan-Meier analysis of survival in patients receiving conventional stenting and those receiving delayed stenting. Log-rank test: P=0.03. Tables
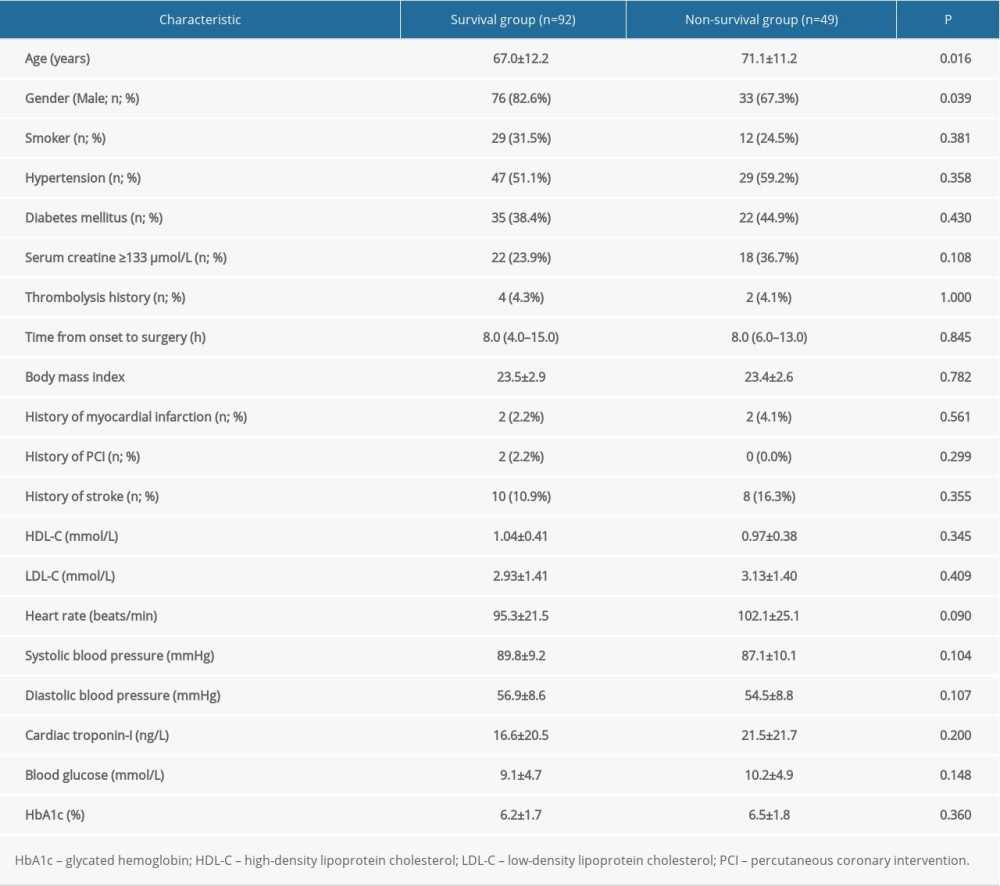 Table 1. Baseline clinical characteristics of patients in the 2 groups.
Table 1. Baseline clinical characteristics of patients in the 2 groups.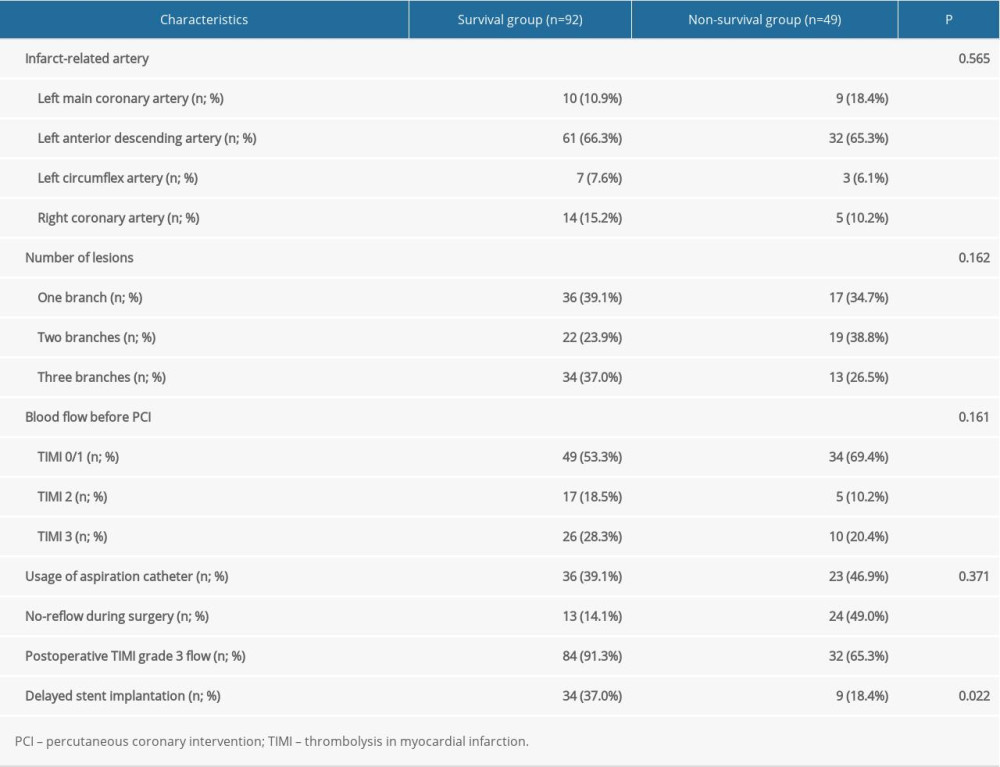 Table 2. Surgery related characteristics of patients in the 2 groups.
Table 2. Surgery related characteristics of patients in the 2 groups.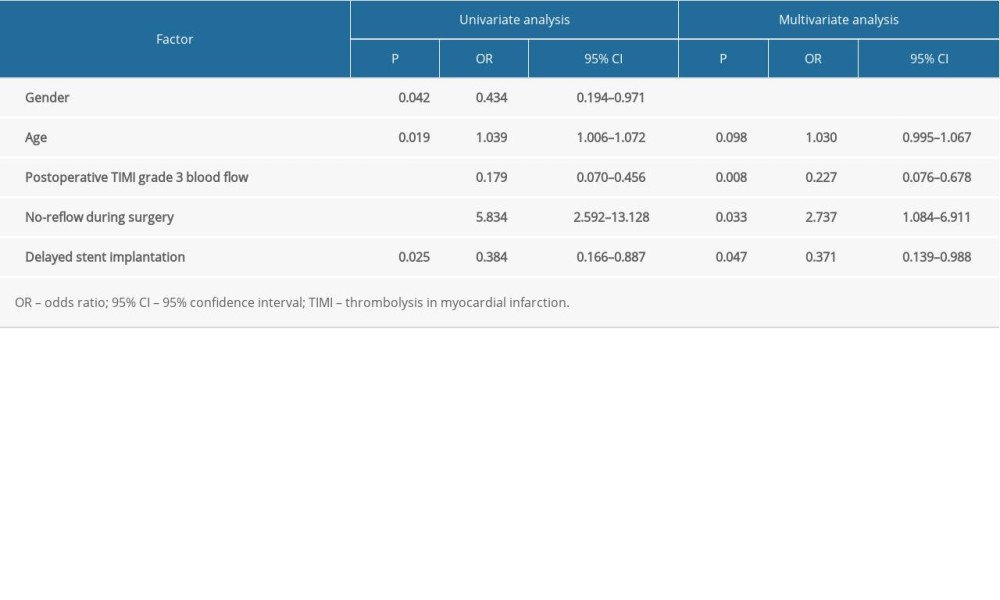 Table 3. Logistic regression analysis of factors associated with death during the 30-day follow-up.
Table 3. Logistic regression analysis of factors associated with death during the 30-day follow-up.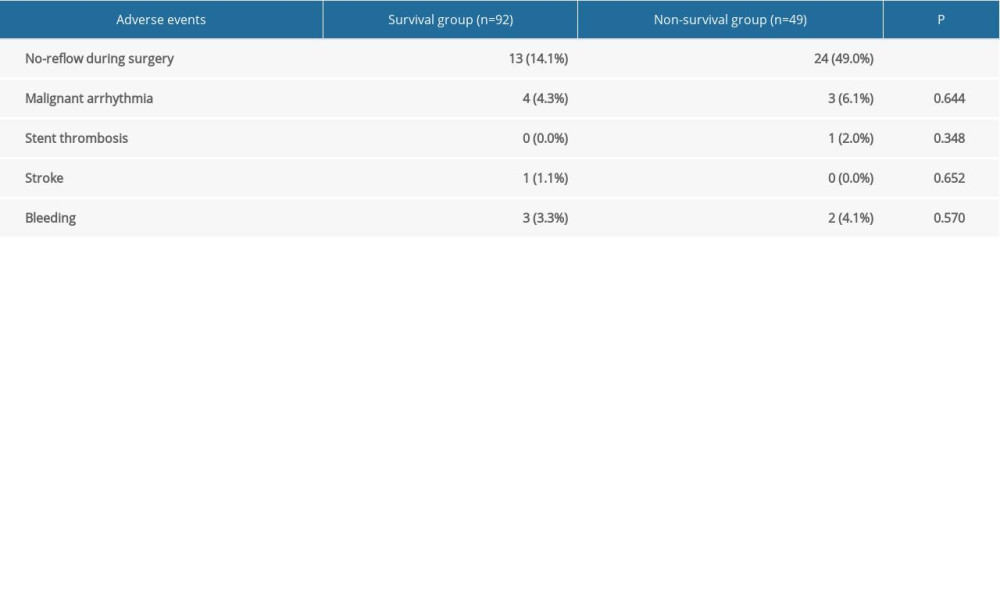 Table 4. Adverse events in the 2 groups.
Table 4. Adverse events in the 2 groups. Table 1. Baseline clinical characteristics of patients in the 2 groups.
Table 1. Baseline clinical characteristics of patients in the 2 groups. Table 2. Surgery related characteristics of patients in the 2 groups.
Table 2. Surgery related characteristics of patients in the 2 groups. Table 3. Logistic regression analysis of factors associated with death during the 30-day follow-up.
Table 3. Logistic regression analysis of factors associated with death during the 30-day follow-up. Table 4. Adverse events in the 2 groups.
Table 4. Adverse events in the 2 groups. In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








