17 March 2021: Clinical Research
Perineural Dexmedetomidine Reduces the Median Effective Concentration of Ropivacaine for Adductor Canal Block
Chunguang Wang1ABCDEF*, Zhiqiang Zhang2AEF, Wenhai Ma3BCE, Rui Liu1BC, Qinghui Li1BC, Yanjun Li3BDOI: 10.12659/MSM.929857
Med Sci Monit 2021; 27:e929857
Abstract
BACKGROUND: Multimodal analgesic regimens are well known as the best option for total knee arthroplasty. They include the adductor canal block, combined with local infiltration analgesia and a block of the interspace between the popliteal artery and the capsule of the posterior knee. However, these analgesic techniques all require a large amount of local anesthetics. In this study, we explored whether the quantity of local anesthetics could be decreased by using dexmedetomidine for the adductor canal block.
MATERIAL AND METHODS: Fifty-four patients scheduled for unilateral, primary total knee arthroplasty were allocated into 2 groups: the ropivacaine group (group R) and the dexmedetomidine group (group RD). Ropivacaine 0.5% was chosen as the initial concentration, and the concentration was decreased or increased according to the response of the previous participant. Based on Dixon’s up-and-down method, the median effective concentration was calculated.
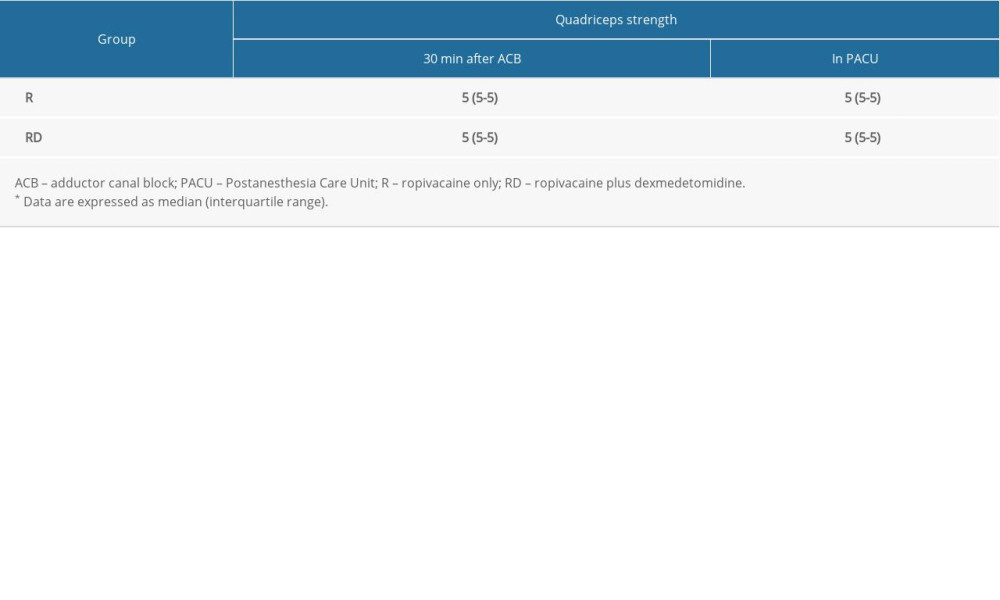
RESULTS: The quadriceps strength was similar between the 2 groups, both at 30 min after adductor canal block and during recovery from general anesthesia in the Postanesthesia Care Unit. None of the patients in this study exhibited bradycardia or hypotension. The median effective concentration of ropivacaine for adductor canal block was 0.29% (95% confidence interval [CI], 0.28–0.31%) in group RD, which was lower than that in group R (0.38% [95% CI, 0.36–0.41%]).
CONCLUSIONS: This study found perineural dexmedetomidine 1 μg/kg could reduce the median effective concentration of ropivacaine for the adductor canal block.
Keywords: Anesthesia, Local, Anesthetics, Local, Dexmedetomidine, Analgesia, Analgesics, Opioid, Arthroplasty, Replacement, Knee, Femoral Nerve, Knee Joint, Nerve Block, pain management, Pain Measurement, Quadriceps Muscle, ropivacaine, Thigh
Background
With the rapid increase in the aging population, surgical treatment is becoming more common among elderly people, especially those with degenerative knee disease. Total knee arthroplasty is the most effective treatment for restoring the function of the knee joint for patients with end-stage knee osteoarthritis. Unfortunately, the management of moderate to severe pain among these patients during the postoperative period remains a considerable challenge for the anesthesiologist [1]. Multimodal analgesic regimens are well known to be the best option for total knee arthroplasty. Such regimens can include adductor canal block, combined with local infiltration analgesia and a block of the interspace between the popliteal artery and the capsule of the posterior knee [2–6]. However, these analgesic techniques require a large amount of local anesthetics. Furthermore, most of the patients undergoing total knee arthroplasty are elderly. Compared with younger patients, the elderly are more sensitive to local anesthetics and metabolize them more slowly, which may lead to accumulation of these agents and even toxicity. To achieve effective analgesia, it is essential to reduce the consumption of local anesthetics during the perioperative period. Perineural adjuvant of local anesthetics is a useful technique to address this problem [7]. Previous studies found that dexmedetomidine can improve the potency of local anesthetics, while sparing nerve injury [8–10]. However, whether the quantity of local anesthetic for adductor canal block can be reduced by dexmedetomidine has not been reported. We speculated that the quantity of local anesthetics could be decreased by perineural administration of dexmedetomidine. Hence, we investigated the effect of perineural dexmedetomidine on the median effective concentration (EC50) of ropivacaine for adductor canal block.
Material and Methods
SUBJECT SELECTION:
The study complied with the Declaration of Helsinki. After approval by the Ethics Committee of our institution (no. [2018] 038) and obtaining written informed consent, we enrolled patients undergoing selective, unilateral primary total knee arthroplasty in our study. Patients with a contraindication for nerve block administration, diabetes, allergy to local anesthetics or dexmedetomidine, bradycardia, long-term administration of analgesics, renal or hepatic dysfunction, or an inability to complete assessments were excluded. According to a computer-generated randomization sequence, stored in sealed opaque envelopes, all subjects were randomly assigned to an experimental group: the ropivacaine group (group R) or the dexmedetomidine group (group RD). In group R, only ropivacaine was used for adductor canal block. In group RD, a mixture of dexmedetomidine 1 μg/kg and ropivacaine was used for adductor canal block. The computer-generated randomization sequence and study medication were prepared by 2 of us (ZZ, RL). A senior anesthesiologist implemented adductor canal block, and another anesthesiologist performed the assessment on nerve block. Both anesthesiologists were blinded to the randomization of group allocation, type of medicine, and the concentration of ropivacaine. A nurse who did not participate in assessment was in charge of preparing the medication based on the assessment result.
PROTOCOL:
Participants received oxygen by nasal cannula and were placed in a supine position with the lower extremity externally rotated. Standard monitors were utilized and no premedication was used in the operation room. With a short-axis view, an ultrasound probe (liner transducer, 6–13 MHz, M-Turbo, Sonosite, USA) was placed on the anteromedial part of the thigh at the level of the midpoint, between the greater trochanter of the femur and the proximal edge of patella. The structure of the adductor canal, surrounded by the sartorius muscle, the vastus medialis muscle, and the adductor longus muscle, was identified clearly. After aseptic precaution, lidocaine 1% was injected into skin and subcutaneously. Then, an 80-mm short-beveled needle (PAJUNK®, PAJUNK GmbH Medizintechnologie, Germany), guided by ultrasound, was inserted through the sartorius muscle into the region between femoral artery and saphenous nerve. Local anesthetics were subsequently injected for adductor canal block.
Cutaneous sensation innervated by the saphenous nerve (the anteromedial aspect of the knee, shin area) was assessed 30 min after injection. The absence of acupuncture sensation in the area innervated by the saphenous nerve was defined as a complete sensory block. The scoring for sensory evaluation was as follows: 0 (totally absence of sensation), 1 (loss of acupuncture sensation but not touch sensation), and 2 (no loss of sensation, similar to contralateral side) [11]. The muscle strength was evaluated immediately after sensory assessment and recovery from general anesthesia in the Postanesthesia Care Unit. The scoring for the evaluation of muscle strength was as follows: 0 (no contraction), 1 (contraction, but patient cannot move joint), 2 (patient can move joint, but cannot resist gravity), 3 (patient can resist gravity), 4 (patient can counter resistance), and 5 (patient can counter full resistance) [12]. Adverse effects, such as bradycardia (heart rate <50 beats/min) and hypotension (the decrease of mean arterial pressure >20% baseline value), were recorded from the time of injection of local anesthetics to the induction of general anesthesia.
MEASUREMENTS:
Based on previous research, 0.5% ropivacaine 15 mL was chosen as the initial concentration [13,14]. The interval of concentration was set at a ratio of 1: 1.2. According to the response of the previous subject (complete block or incomplete block), the concentration was decreased or increased. The 2 groups were run in parallel. According to Dixon’s up-and-down method, the ending rule requires 6 consecutive up-and-down sequences [15]. In the current study, the primary outcome was the EC50 of ropivacaine for adductor canal block, and the value of EC50 was determined by the Dixon and Massey method. Eight consecutive up-and-down sequences, considered sufficient to study the EC50 of ropivacaine, were achieved with 24 patients in group R and 30 patients in group RD.
STATISTICAL ANALYSIS:
Statistical analysis was conducted using SPSS 17.0 (SPSS Inc., Chicago, IL, USA). Data are shown as mean±standard deviation, median (interquartile range), or number. Data were tested for normal distribution using the Kolmogorov-Smirnov test. Normally distributed continuous variables were tested using
Results
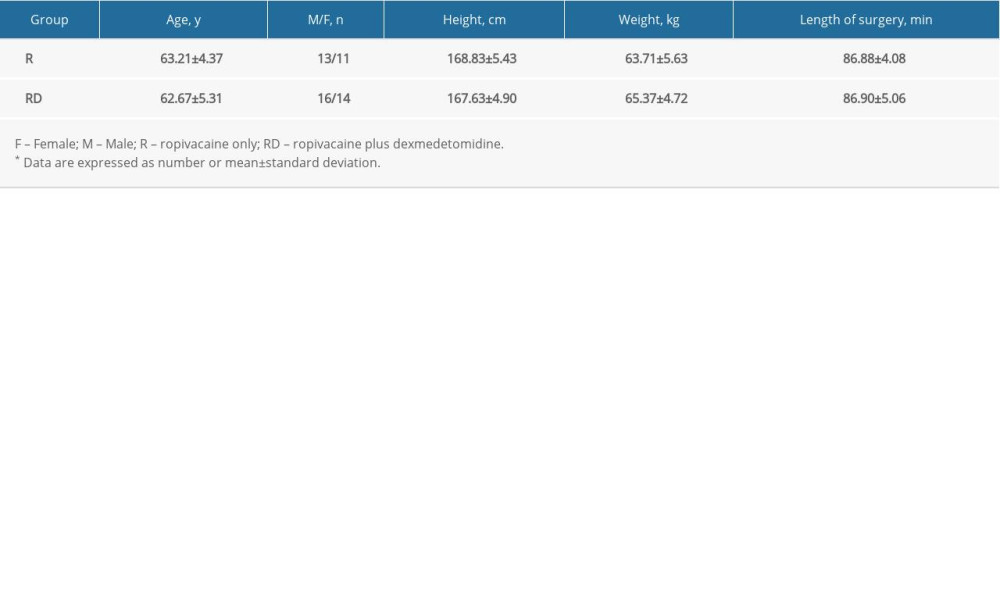
Fifty-nine subjects were recruited for this study. Five declined to participate, and 54 participants completed the study (Figure 1). The 2 experimental groups were similar in terms of age, sex, height, weight, and the length of surgery (Table 1;
Discussion
Multimodal analgesic regimens with nerve block as the core have become the best option for total knee arthroplasty. These local anesthesia techniques allow reducing the use of opioids. However, for patients undergoing simultaneous bilateral total knee arthroplasty, the use of high-dose local anesthetics may increase the risk of toxicity. Adjunct medications, such as dexmedetomidine, clonidine, and dexamethasone, can enhance the analgesic effect of local anesthetics [7–11,16–18].
Dexmedetomidine, a selective alpha-2 adrenergic receptor agonist, was demonstrated to strengthen the quality of peripheral nerve block both in experimental and clinical research [7–11]. Brummett et al [8] showed that dexmedetomidine could increase the action time and improve the potency of ropivacaine in rats. Andersen et al [10] found that dexmedetomidine could increase the action time of ulnar nerve block. Andersen et al [14] also reported that dexmedetomidine could extend the duration of nerve block. In our study, we found that the EC50 of ropivacaine for adductor canal block was 0.29% (95% CI, 0.28–0.31%), which could be reduced to 0.38% (95% CI, 0.36–0.41%) when combined with 1 μg/kg dexmedetomidine. Our results indicated that the quantity of local anesthetics could be decreased by about 24% through perineural administration of dexmedetomidine. Ye et al [19] found that retrobulbar dexmedetomidine enhanced the effect of retrobulbar block and decreased the minimum local anesthetic concentration of ropivacaine by about 22%, without any neurotoxic effects. Zhang and Li [20] reported that epidural dexmedetomidine for labor analgesia reduced the EC50 of ropivacaine by about 25%. These results were consistent with our results showing a decrease of 24% of EC50. Raof et al [21] found that the minimum local anesthetic concentration decreased by about 35% with dexmedetomidine for ultrasound-guided transversus abdominis plane block. The differences in the types of local anesthetics and the dose of dexmedetomidine may explain the variation in results. Lu et al [9] reported that EC50 of ropivacaine was decreased by about 49% with dexmedetomidine for obturator nerve block. Those results exceeded our results, which showed a 24% decrease in EC50. The differences may be related to variations in the assistance modes of the nerve block (ultrasound vs nerve stimulator) and assessment methods (motor block vs sensory block).
The mechanism of dexmedetomidine in analgesia is still unclear. Previous studies suggested that a selective alpha-2 adrenergic receptor agonist could inhibit the release of substance P from the spinal dorsal horn neurons and activate the alpha-2 adrenergic receptors in locus ceruleus [22]. However, more research attention has been paid to the peripheral mechanism of dexmedetomidine rather than the central mechanism. Alpha-2 adrenergic receptor agonists could produce an effect similar to local anesthetics by inhibiting the release of norepinephrine and production of non-receptor-dependent action potentials in alpha and C fibers [23,24]. Brummett et al [8] found that hyperpolarization-activated cation currents could be blocked by peripheral dexmedetomidine, which extended the hyperpolarization of unmyelinated C fibers. Moreover, there are some mechanisms independent of alpha-2 adrenergic receptors by which the K+ current and Na+ current could be blocked by dexmedetomidine, leading to inhibition of neuronal activity [25].
Prior to perineural administration of dexmedetomidine, it is important to understand its adverse effects, including neurotoxicity, bradycardia, and hypotension. Most previous studies have not found evidence of neurological toxicity of dexmedetomidine when it is used as an adjuvant to local anesthetics. Brummett et al [26] found that dexmedetomidine did not cause injury of axons or myelin sheaths, but it could improve bupivacaine-induced perineural inflammation. Kim et al [27] found that dexmedetomidine could reduce inflammation and nerve injury induced by ropivacaine after intraneural injection. Keplinger et al [28] found that perineural dexmedetomidine used at a clinical concentration did not cause long-term postblock paresthesia. Lu et al [9] reported that no painful paresthesia or nerve injury occurred after obturator nerve block with dexmedetomidine added to lidocaine. Bradycardia and hypotension can be caused by dexmedetomidine in a dose-dependent manner. Esmaoglu et al [29] reported that dexmedetomidine caused a high incidence of bradycardia and hypotension from 5 to 90 min after injection. However, we did not observe bradycardia or hypotension in the current study. The differences may be explained by different experimental protocols and doses of dexmedetomidine.
There are some limitations to this research. First, the dose of dexmedetomidine was chosen empirically based on previous research [30]. The optimal dose should be explored in future research. In addition, the neurotoxicity of dexmedetomidine was not investigated in this study. Dexmedetomidine has not been associated with neurotoxicity when used as an adjuvant to local anesthetics in most previous studies, but Yu et al [31] found that dexmedetomidine aggravated nerve injury induced by local anesthetics in diabetic rats. Therefore, it is important to be mindful of the potential risk of neurotoxicity for patients with diabetes.
Conclusions
This study found that perineural dexmedetomidine 1 μg/kg could reduce the EC50 of ropivacaine for adductor canal block.
Figures
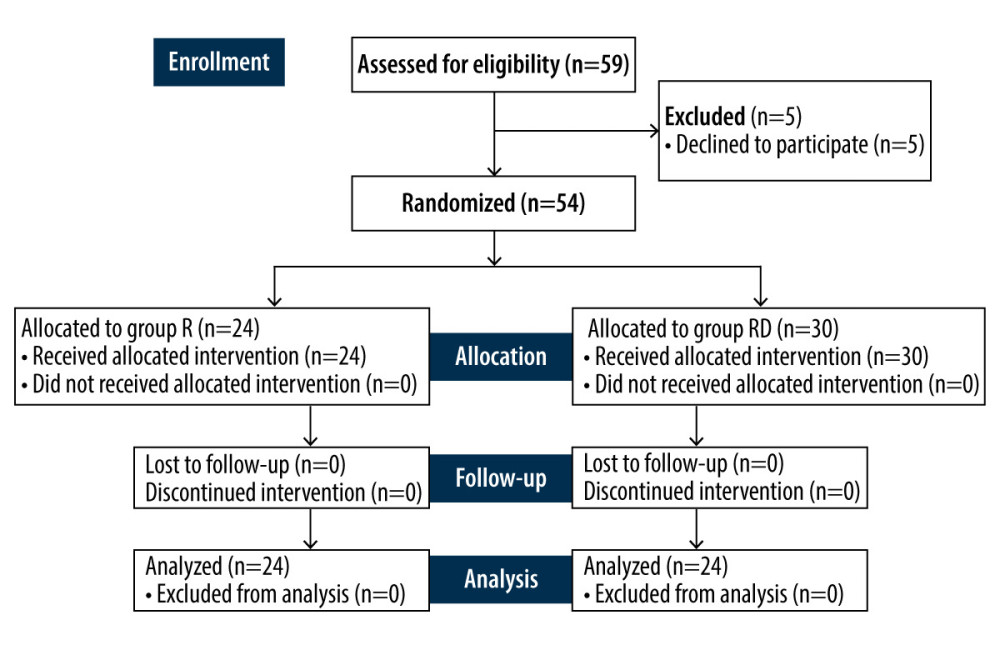 Figure 1. Study flow diagram. R – ropivacaine only; RD – ropivacaine mixed with dexmedetomidine.
Figure 1. Study flow diagram. R – ropivacaine only; RD – ropivacaine mixed with dexmedetomidine. 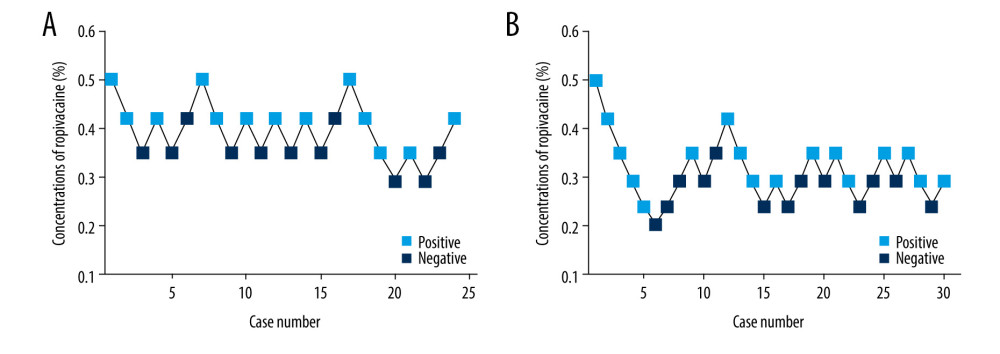 Figure 2. Sequential responses to up-and-down concentrations of ropivacaine for adductor canal block. (A) The sequential responses to up-and-down concentrations of ropivacaine in Group R. (B) The sequential responses to up-and-down concentrations of ropivacaine in Group RD. Empty squares indicate a positive response (ie, complete sensory block), and black squares indicate a negative response (ie, incomplete sensory block).
Figure 2. Sequential responses to up-and-down concentrations of ropivacaine for adductor canal block. (A) The sequential responses to up-and-down concentrations of ropivacaine in Group R. (B) The sequential responses to up-and-down concentrations of ropivacaine in Group RD. Empty squares indicate a positive response (ie, complete sensory block), and black squares indicate a negative response (ie, incomplete sensory block). References
1. Hebl JR, Dilger JA, Byer DE, A pre-emptive multimodal pathway featuring peripheral nerve block improves perioperative outcomes after major orthopedic surgery: Reg Anesth Pain Med, 2008; 33; 510-17
2. Henshaw DS, Jaffe JD, Reynolds JW, An evaluation ultrasound-guided adductor canal blockade for postoperative analgesia after medial unicondylar knee arthroplasty: Anesth Analg, 2016; 122; 1192-201
3. Kampitak W, Tanavalee A, Ngarmukos S, Amarase C, Opioid-sparing analgesia and enhanced recovery after total knee arthroplasty using combined triple nerve blocks with local infiltration analgesia: J Arthroplasty, 2019; 34; 295-302
4. Grosso MJ, Murtaugh T, Lakra A, Adductor canal block compared with periarticular bupivacaine injection for total knee arthroplasty: A prospective randomized trial: J Bone Joint Surg Am, 2018; 100(13); 1141-46
5. Sankineani SR, Reddy ARC, Eachempati KK, Comparison of adductor canal block and IPACK block (interspace between the popliteal artery and the capsule of the posterior knee) with adductor canal block alone after total knee arthroplasty: A prospective control trial on pain and knee function in immediate postoperative period: Eur J Orthop Surg Traumatol, 2018; 28(7); 1391-95
6. Runge C, Bjorn S, Jensen JM, The analgesic effect of a popliteal plexus blockade after total knee arthroplasty: A feasibility study: Acta Anaesthesiol Scand, 2018; 62; 1127-32
7. Vorobeichik L, Brull R, Abdallah FW, Evidence basis for using perineural dexmedetomidine to enhance the quality of brachial plexus nerve blocks: A systematic review and meta-analysis of randomized controlled trials: Br J Anaesth, 2017; 118(2); 167-81
8. Brummett CM, Hong EK, Janda AM, Perineural dexmedetomidine added to ropivacaine for sciatic nerve block in rats prolongs the duration of analgesia by blocking the hyperpolarization-activated cation current: Anesthesiology, 2011; 115(4); 836-43
9. Lu Y, Sun J, Zhuang X, Perineural dexmedetomidine as an adjuvant reduces the median effective concentration of lidocaine for obturator nerve blocking: A double-blinded randomized controlled trial: PLoS One, 2016; 11(6); e0158226
10. Andersen JH, Jaeger P, Grevstad U, Systemic dexmedetomidine is not as efficient as perineural dexmedetomidine in prolonging an ulnar nerve block: Reg Anesth Pain Med, 2019; 44; 333-40
11. Wang CG, Yang JP, Hu CQ, Ding YL, The effect of adding dexmedetomidine to ropivacaine for lumbar plexus and sciatic nerve block: Int J Clin Exp Med, 2016; 9; 14198-204
12. Wintz MM, Variations in current manual muscle testing: Phys Ther Rev, 1959; 39; 466-75
13. Andersen HL, Andersen SL, Tranum-Jensen J, The spread of injectate during saphenous nerve block at the adductor canal: A cadaver study: Acta Anaesthesiol Scand, 2015; 59(2); 238-45
14. Andersen JH, Grevstad U, Siegel H, Does dexmedetomidine have a perineural mechanism of action when used as an adjuvant to ropivacaine? A paired, blinded, randomized trial in healthy volunteers: Anesthesiology, 2017; 126(1); 66-73
15. Dixon WJ, Massey FJ: Introduction to statistical analysis, 1983; 428-39, New York, McGraw-Hill
16. Hutschala D, Mascher H, Schmetterer L, Clonidine added tobupivacaine enhances and prolongs analgesia after brachial plexus block via a local mechanism in healthy volunteers: Eur J Anaesthesiol, 2004; 21; 198-204
17. Vieira PA, Pulai I, Tsao GC, Dexamethasone with bupivacaine increases duration of analgesia in ultrasound-guided interscalene brachial plexus blockade: Eur J Anaesthesiol, 2010; 27; 285-88
18. Choi S, Rodseth R, McCartney CJ, Effects of dexamethasone as a local anaesthetic adjuvant for brachial plexus block: A systematic review and meta-analysis of randomized trials: Br J Anaesth, 2014; 112; 427-39
19. Ye W, Hu Z, Jin X, Retrobulbar dexmedetomidine decreases the MLAC of ropivacaine in vitreoretinal surgery in children: Eur J Ophthalmol, 2015; 25(4); 352-56
20. Zhang W, Li C, EC50 of epidural ropivacaine combined with dexmedetomidine for labor analgesia: Clin J Pain, 2018; 34(10); 950-53
21. Raof RA, El Metainy SA, Alia DA, Wahab MA, Dexmedetomidine decreases the required amount of bupivacaine for ultrasound-guided transversus abdominis plane block in pediatric patients: A randomized study: J Clin Anesth, 2017; 37; 55-60
22. Guo TZ, Jiang JY, Buttermann AE, Dexmedetomidine injection into the locus ceruleus produces antinociception: Anesthesiology, 1996; 84(4); 873-81
23. Butterworth JF, Strichartz GR, The alpha2 adrenergic agonists clonidine and guanfacine produce tonic and phasic block of conduction in rat sciatic nerve fibres: Anaesth Analg, 1993; 76(4); 295-301
24. Nakamura M, Ferreira SH, Peripheral analgesic action of clonidine: Mediation by release of endogenous enkephalin like substances: Eur J Pharmacol, 1988; 146(6); 223-28
25. Chen BS, Peng H, Wu SN, Dexmedetomidine, an α2-adrenergic agonist, inhibits neuronal delayed rectifier potassium current and sodium current: Br J Anaesth, 2009; 103; 382-94
26. Brummett CM, Norat MA, Palmisano JM, Lydic R, Perineural administration of dexmedetomidine in combination with bupivacaine enhances sensory and motor blockade in sciatic nerve block without inducing neurotoxicity in rats: Anesthesiology, 2008; 109; 502-11
27. Kim BS, Choi JH, Baek SH, Lee DH, Effects of intraneural injection of dexmedetomidine in combination with ropivacaine in rat sciatic nerve block: Reg Anesth Pain Med, 2018; 43(4); 378-84
28. Keplinger M, Marhofer P, Kettner SC, A pharmacodynamic evaluation of dexmedetomidine as an additive drug to ropivacaine for peripheral nerve blockade: A randomised, triple-blind, controlled study in volunteers: Eur J Anaesthesiol, 2015; 32(11); 790-96
29. Esmaoglu A, Yegenoglu F, Akin A, Yildirim C, Dexmedetomidine added to levobupivacaine prolongs axillary brachial plexus block: Anesth Analg, 2010; 111; 1548-51
30. Rancourt MP, Albert NT, Cote M, Posterior tibial nerve sensory blockade duration prolonged by adding dexmedetomidine to ropivacaine: Anesth Analg, 2012; 115; 958-62
31. Yu ZY, Geng J, Li ZQ, Dexmedetomidine enhances ropivacaine-induced sciatic nerve injury in diabetic rats: Br J Anaesth, 2019; 122(1); 141-49
Figures
 Figure 1. Study flow diagram. R – ropivacaine only; RD – ropivacaine mixed with dexmedetomidine.
Figure 1. Study flow diagram. R – ropivacaine only; RD – ropivacaine mixed with dexmedetomidine. Figure 2. Sequential responses to up-and-down concentrations of ropivacaine for adductor canal block. (A) The sequential responses to up-and-down concentrations of ropivacaine in Group R. (B) The sequential responses to up-and-down concentrations of ropivacaine in Group RD. Empty squares indicate a positive response (ie, complete sensory block), and black squares indicate a negative response (ie, incomplete sensory block).
Figure 2. Sequential responses to up-and-down concentrations of ropivacaine for adductor canal block. (A) The sequential responses to up-and-down concentrations of ropivacaine in Group R. (B) The sequential responses to up-and-down concentrations of ropivacaine in Group RD. Empty squares indicate a positive response (ie, complete sensory block), and black squares indicate a negative response (ie, incomplete sensory block). In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952