28 February 2021: Clinical Research
Influence of Hostility on 24-Hour Diastolic Blood Pressure Load in Hypertension Patients with Depressive Disorders
Feihuan Cui1ABE, Na Zhang1D, Jin Yi1DF, Yulan Liang1CD, Qi Liu2AEF*DOI: 10.12659/MSM.929710
Med Sci Monit 2021; 27:e929710
Abstract
BACKGROUND: Hostility in hypertension patients combined with depressive disorders indicates a worse outcome for hypertension management. This study was designed to explore the influence of hostility on 24-h diastolic blood pressure in hypertension patients who also had depressive disorders.
MATERIAL AND METHODS: A total of 130 people with primary hypertension and depressive disorders were collected through unstructured psychiatric interview by a professional psychiatrist and ambulatory blood pressure monitor in this cross-sectional study. During the study, dynamic blood pressure was examined for 24 h by ambulatory blood pressure monitoring. Patients were divided into 3 groups according to the hostility level. Hostility was defined by hostile factors of the Symptom Checklist 90. The association between hostility and 24-h dynamic blood pressure was analyzed by multivariable logistic regression.
RESULTS: 30.8% (40 of 130) patients had a high level of 24-h dynamic blood pressure load (>30%), in which 14.6% was for male and 16.2% for female respectively. In male, the proportion of high 24 h DBP load (>30%) in highest hostility group was greater than that of low hostility group and median hostility group significantly (p=0.03). No significant differences were revealed among 3 groups in female. The age-adjusted odds-ratio (OR) 95% confidence interval of diastolic blood pressure across the categories of hostility were: in males, 1.44 (0.60, 3.47) (1 for reference), and in females, 5.86 (0.58, 59.06) (P for trend=0.04).
CONCLUSIONS: Our results showed that hostility may be a risk factor for increased 24-h diastolic blood pressure in hypertension patients who also have depressive disorders, especially in males. The clinical meaning of the study is that hypertension management should contain psychological interventions for better effects.
Keywords: Blood Pressure, Depression, Hostility, Hypertension, Blood Pressure Monitoring, Ambulatory, Cross-Sectional Studies, Depressive Disorder, Risk Factors
Background
Hypertension is a common chronic cardiovascular disease, with a prevalence of 30–45% in the general population [1,2]. The incidence of depression in hypertension patients is 27%, and is much higher than that in the general population [3–5]. Depression is a common combined disease in hypertension, causing exacerbation of hypertension complications [6]. The disturbance of serotonin (5-hydroxy tryptophan, 5-HT) in the brain is an important pathological pathway in progression of depression [7,8]. In peripheral vascular circulation, 5-HT is synthesized in intestinal cells and stored in granules, which are absorbed or stored in platelets, and can increase the reaction of platelets to stimulation. Thus, increased agglutination and vasoconstriction is caused [9,10], leading to elevated blood pressure. Elevated blood pressure is a risk factor for cardiovascular events [11,12], so depression in hypertension patients increases risks of higher blood pressure.
In a study, depressive symptoms were found to be most relevant as a patient-related predictor of the quality of the family physician-patient relationship [13]. Significant positive correlations were revealed between self-reported severity of depression and all subtypes of hostility in a medical center study [14]. Hostility is closely associated with depression. One of the important pathological mechanisms of hostility is the imbalance and low function of 5-HT in the central neurological system [15]. Previous studies have found that most hostile men have a range of risk factors for diabetes and cardiovascular diseases [16,17]. Thus, hostility is regarded as an additional risk factor for hypertension in hypertension patients who also have depression.
Blood pressure at 24 h is an indicator measured by ambulatory blood pressure monitoring (ABPM), and the prediction value is more significant than sporadic blood pressure. Both diastolic blood pressure (DBP) and systolic blood pressure (SBP) monitoring are useful in diagnosing onset cerebrovascular disease (CVD). When 24-h DBP exceeds 30%, the left ventricular diastolic function obviously declines [18–20]. The 22-year follow-up of the Multiple Risk Factor Intervention Trial population showed that cardiovascular mortality was associated with higher DBP, even in patients with systolic pressure below 120 mmHg [21]. Increased diastolic blood pressure is still meaningful for studies on hypertension management.
Totally, hostility may have more risks for hypertension patients who also have with depression, but the relationship between hostility and 24-h DBP has rarely been explored. The aim of our study was to explore the association between hostility severity and 24-h DBP in hypertension patients with depressive disorders. The study is presented in accordance with the STROBE reporting checklist as below.
Material and Methods
PARTICIPANTS:
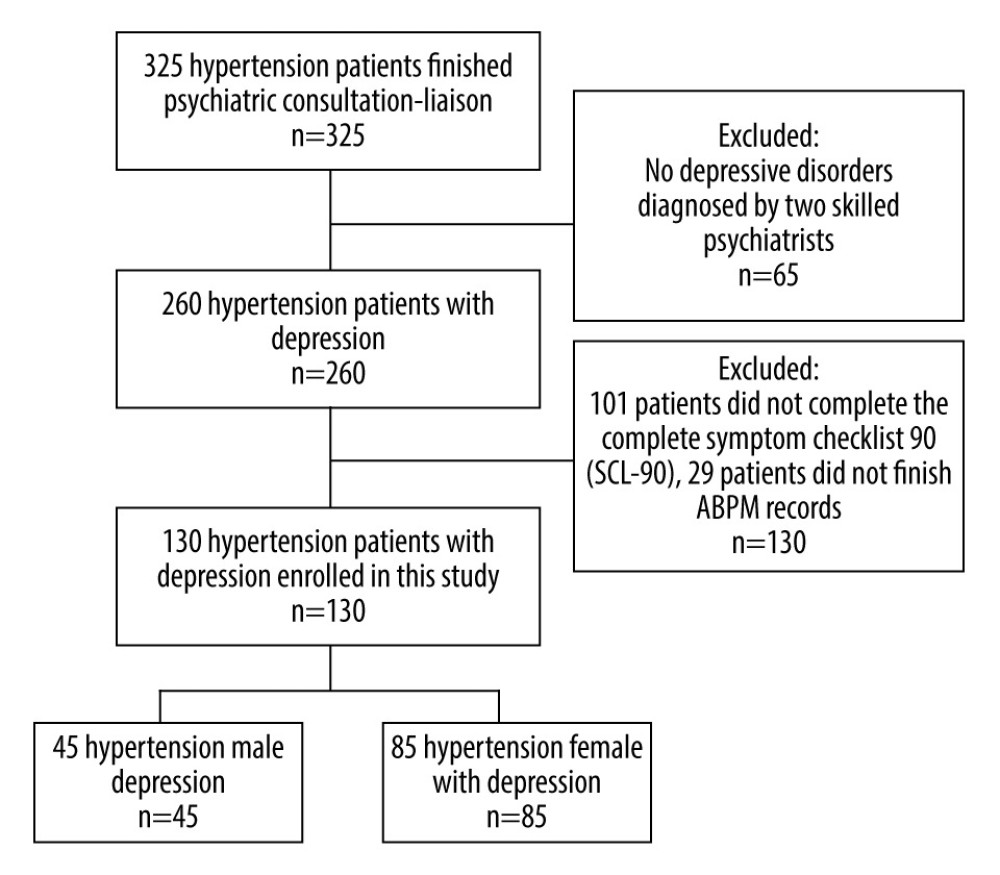
This study was conducted according to the Declaration of Helsinki and was approved by the Institutional Research Ethics Committee of our hospital, and written informed consent was obtained from all participants. This cross-sectional study enrolled 130 hypertension patients who finished ABPM measurements and were diagnosed with depression. A total of 325 hypertension patients finished psychiatric consultation-liaison in the hypertension unit of our hospital between January 2014 and December 2018. Medical staff recorded the patients’ medical history, including use of hypertensive drugs, other chronic diseases, and lifestyle factors such as smoking and drinking, and introduced the psychiatric consultation-liaison service to them. Two skilled psychiatrists performed unstructured psychiatric interview with each patient in a private location. Depressive disorders were defined and diagnosed by the psychiatrists according to 10th revision Diagnostic Criteria for Mental Behavior Disorders of International Statistical Classification of Diseases and Related Health Problems (ICD-10). The diagnoses of the 2 psychiatrists were similar and the kappa score was 0.99. If the 2 psychiatrists had different diagnoses, a more senior psychiatrist was introduced for another interview to make the final result. After the diagnosis, 260 of the patients were in compliance with the diagnosis of depression disorders, while 65 of them were excluded (17 with no mental disorders, 21 with anxiety disorders, 12 with sleep-related disorders, 3 with organic mental disorders, 2 with bipolar disorders, 2 with harmful use of substances, 5 with somatoform disorders, 1 with obsessive-compulsive disorder, and 2 with stress-related disorders). Of the 260 patients, 101 patients did not complete the complete Symptom Checklist 90 (SCL-90) and 29 patients did not finish ambulatory blood pressure monitoring (ABPM). We finally included and followed up 130 patients in this study (Figure 1).
In the study, 34.6% (45 of 130) of participants were males, with mean age±SD (45.2±12.1 years) and 65.4% (85 of 130) of participants were females, with mean age±SD (56.3±10.8 years). The status of hostility in the 3 categories (≤60; >60, ≤90; >90) was 27.8%, 33.3%, 80.0% in males and 72.2%, 66.7%, 20.0% in females, respectively. Males and females were analyzed differently in this study because hostility is significantly different in males vs females [15,16].
INCLUSION AND EXCLUSION CRITERIA:
ASSESSMENT OF HYPERTENSION AND 24-H DIASTOLIC BLOOD PRESSURE:
Hypertension was defined as SBP ≥140 mmHg or/and DBP ≥90 mmHg, and the mean values were based on 2 or more measurements on different days without anti-hypertension drugs used. ABPM was finished on each enrolled patient and was recorded using Spacelabs 90217 equipment (Spacelabs, Redmond, Washington, USA). Blood pressure for 24 h is the percentage of DBP or SBP measurements in 24 h (daily mean >140/90 mmHg and night mean >120/80mmHg). The patients stopped using antihypertensive drugs for 1 week before the test. Blood pressure was monitored by professionally trained staff. The cuff was fixed on the left upper arm of the patient, and the air bag in the cuff wrapped at on least 80% of the upper arm. The recorder was placed on the waist, and removed after 24 h. The interval of daytime measurement was 20 min, and the interval of night measurement was 30 min. It was stipulated that 6: 00-22: 00 was daytime, and 22: 00-6: 00 was nighttime. During the test, the patients could not unfasten the cuff. When sleeping, the monitor was placed on one side of the body to avoid bending the pressure tube.
ASSESSMENT OF HOSTILITY AND GROUPING:
Symptom Checklist 90 (SCL-90) in Chinese version [22] was applied to assess the psychological distress of patients diagnosed with depressive disorder. This version of SCL-90 was translated from the Hopkin’s Symptom Checklist (HSCL1973) made by Derogatis [23]. The validity of the Chinese version was assessed in previously published studies, like Dr. Liu’s study published in the Community Mental Health Journal [24]. The scale contained 9 factors: somatization, compulsion, interpersonal disorder, depression, anxiety, hostility, fear, paranoia, and psychosis. Factor scores reflected the severity of symptoms in this dimension. Factors were transferred into standard scores according to age and sex. Hostility was ranked into 3 degrees according to the T-value of the hostility subscale in SCL-90. Categorical variables are presented as equal intervals of T-score for 3 hostility levels (hostility ≤60 was defined as low hostility; 60–90 was defined as median hostility; >90 was defined as high hostility). In our study, according to SCL-90, Item 11 is “easily becomes annoyed and excited”, Item 24 is “loses temper uncontrollably”, Item 63 is “the urge to hit or hurt others”, Item 67 is “wants to break or destroy things”, Item 74 is “argues with people”, and Item 81 is “yells or throws things”, and these items were used to evaluate the hostility factor. Each item is scored on a scale of 1 (none) to 5 (severe), and the rough score of the scale is converted into a standard score (30–120) according to the formula. The above process is completed through the Heisman psychological CT network system (Heisman Psychological Computerized Tomoscan Machine, which is has been used for more than 15 years).
ASSESSMENT OF OTHER VARIABLES:
Previous disease history was collected by internal physicians, including hyperlipidemia, diabetes, coronary heart disease and stroke. Information on antihypertensive medications was obtained from patients’ electronic medical records database after patients provided consent. The variables were evaluated in the week before and the week after the interview. Diabetes was defined as a fasting blood glucose (FBG) level ≥126 mg/dl (7.0 mmol/L), or oral glucose tolerance test ≥200 mg/dl (11.1mmol/L), or HbA1c ≥48 mmol/mol (6.5%) or a history of T2DM (type 2 diabetes mellitus). Hyperlipidemia was defined as total cholesterol (TC) ≥5.17 mmol/L or triglyceride (TG) ≥1.7 mmol/L or low-density lipoprotein (LDL) cholesterol ≥3.37 mmol/L. Coronary heart disease was defined as a degree of coronary artery stenosis greater than 50% revealed through coronary angiography or a history of coronary heart disease (CHD). Stroke was defined as a history of ischemic stroke, hemorrhage stroke, or transient ischemic attack. Sociodemographic variables were also assessed using comprehensive questionnaires which included age, sex, marital status, occupation, drinking status, and smoking status. Body mass index (BMI) was calculated as weight in kilograms divided by squared height in meters (kg/m2).
STATISTICAL ANALYSIS:
Statistical analysis was carried out with SPSS version 25.0 (IBM Corp, Armonk, NY, USA). The bivariate analysis was performed using the Mann-Whitney U test or Fisher’s exact test. For further analysis, the presence of high 24-h DBP was used as a dependent variable and the categories of hostility were used as independent variables. Logistic regression analysis was used to examine the association between the degree of hostility and high level of 24-h DBP after adjustment for potential confounding factors. Interactions between the degree of hostility and potential confounders were tested by the addition of the cross-product terms in the regression model. To avoid multicollinearity, single components of blood pressure were entered separately into the models. Odds ratios (ORs) and 95% confidence interval (CI) of age and hostility were calculated. Nominal, 2-tailed
Results
CHARACTERISTICS OF PARTICIPANTS:
Characteristics of participants according to hostility are shown in Table 1. Patients with higher hostility were more likely to be male (P=0.00) and younger than in the other 2 groups (P=0.00). Patients with a low degree of hostility were not significantly different from the other 2 groups in marital status, occupation, body mass index (BMI), diabetes, coronary heart disease (CHD), stroke, hyperlipidemia, smoking, or drinking. The 3 groups did not significantly differ in use of calcium channel blocker (CCB), diuretics, angiotensin-converting enzyme inhibitors (ACEI), angiotensin receptor blocker (ARB), α-blocker, or β-blocker.
ASSOCIATION BETWEEN SCL-90 AND 24-H DBP LOAD:
The distributions of different degrees of hostility in higher 24-h DBP load (>30%) were different in males and females (Table 2). The proportion of patients with a high level of 24-h DBP load (>30%) was 30.8% (40 of 130) (14.6% and 16.2% for males and females, respectively). In males, the proportion of high 24-h DBP load (>30%) in the highest hostility group was significantly greater than in the low- and median-hostility groups (P=0.03). There were no significant differences among the 3 groups in females.
The SCL-90 subscale analysis (Table 3) showed that there were significant differences in ANX (anxiety) and HOST (hostility) between patients with high DBP load >30% and those with <30%. In Table 4, DBP load >30% was defined as a positive outcome. OR and 95% CI were calculated with logistic regression modeling. The crude model only included hostility. The age-adjusted model was additionally adjusted with age. In Table 5, sensitivity analysis was calculated in male patients. A model was built with only hostility and age-adjustment. Due to the small sample, there were not more factors in the equation. The multivariable adjusted odds ratios (OR, 95% confidence interval) of DBP load across the categories of hostility were: in males, 1.00 was for reference, the data were 1.86 (0.50, 6.94) and 8.50 (1.01, 88.56) (P for trend=0.03); in general, 1.00 was for reference, the data were 1.72 (0.75, 3.92) and 11.65 (1.24, 109.66) (P for trend=0.04). The age was adjusted in models; in general, the adjusted odds ratios (OR, 95% confidence interval) were 1 (ref), 1.97 (0.52, 7.49), and 7.27 (0.68, 78.72) (P for trend=0.10), and 1 (ref), 1.44 (0.60, 3.47), 5.86 (0.58, 59.06) (P for trend=0.04) in males (Tables 4, 5). Logistic regression analysis of subscales between patients with high DBP load >30% and <30% (Table 6) showed that subscale HOST (OR 3.61, 95% CI 1.45, 8.98) was a risk factor affecting DBP load.
Discussion
Many psychological risk factors, including depression, anger, anxiety, hostility, and certain personality traits, can negatively influence the prognosis of CHD. In the Coronary Artery Risk Development in Young Adults (CARDIA) study, hostility was found to be related with long-term risks of hypertension in a general population [25]. One cross-sectional study suggested that the specific feature of hostility affected the circadian variation of hypertension [26]. A Dutch cohort study found that symptoms of depression and anxiety were associated with the incidence of hypertension 5 years later, and patients who met the criterion for possible clinical depression and anxiety were also more likely to be hypertensive [27]. Another study found that high-hostility individuals reported more negative emotions and higher blood pressure, and had higher rates of cardiovascular morbidity and mortality [28].
In a small-sample study of 25 depression patients, long-term emotional disturbance was linked to irreversible increased blood pressure, and their blood pressure could recover after treatment of depression [29]. Furthermore, hostility and depression were considered as risk factors of elevated blood pressure, a lack of circadian variation in blood pressure, diabetes, and myocardial infarction in epidemiological studies. All of these diseases share risk factors with high-load blood pressure [30,31]. Alteration of the hypothalamic-pituitary adrenal axis and autonomic dysfunction were found in depression patients with hostility, causing endothelial dysfunction, inflammation, and a prothrombotic state. Furthermore, the vascular smooth muscle constricted and caused an elevation of blood pressure. The personality trait of hostility was associated with high levels of pro-inflammatory and inflammatory factors [32]. A weak positive relationship between hostility and systolic blood pressure and a strong positive relationship between hostility and diastolic blood pressure were revealed by a study [33]. The results of the present study show that 24-h DBP and hostility may be meaningful variables for hypertension management.
The damage caused by hostility was greater in men than women [34,35]. Additionally, the behavioral mechanism of depression with high hostility can partly explain the relationship with hypertension. Hostility can be viewed as an attitude of cynical and suspicious thinking about others [36]. The hostile behavior or emotional expression causes more interpersonal conflict and a feeling of social isolation. A feeling of having less support can be related to less perceived resources to cope with the disease, causing difficulty and helplessness in management of hypertension [37]. Also, lack of social support can cause higher rates of alcohol or tobacco consumption, especially in males, deteriorating the process of hypertension. Our results suggest that after adjustment for age, the proportion of high 24-h DBP load was 4.857 times higher in males with high hostility (hostility >90) than in those with low hostility. In contrast, no significant association was observed between high 24-h DBP load and hostility in females. In male depression patients, the higher degree of hostility may influence the 24-h DBP load and can increase the risk of left ventricular diastolic dysfunction, which thus adversely affects the prognosis of hypertension. Our study confirmed that there were differences between men and women in hypertension control.
This investigation observed that in the SC90-subscale, HOST is a risk factor affecting DBP load, but the pseudo R2 (McFadden’s Rho-Squared=0.08.) was too low and had no predictive value. There are many factors that can affect DBP, including genetic factors and environmental influences. Genetic factors explained 39% of the DBP variation in the Muzabinho population [38]. Blood pressure is inversely proportional to the level of physical activity. DBP in adulthood is significantly related to physical exercise (genetic, rg=−0.27 and environment, re=−0.18) [39]. However, there are still some limitations for this study. Firstly, because of the small sample, the association between hostility and hypertension patients with depressive disorders still needs to be validated in a larger population. Secondly, the study still needs a longitudinal follow-up to explore the long-term impact of hostility on hypertension patients with depression. Thirdly, the subjects of this study were mainly from north China, which only represents a part of Asia. The applicability of our results for European and American countries are unclear due to different racial characteristics, geographical environment, and living habits. Further studies are required to confirm our conclusions. Finally, the absence of structured psychiatry interviews and the use of the specific Chinese version depression scale did not have overall control on the patients’ information, which may have led to some bias in scale results.
Conclusions
In summary, the present study demonstrated that higher hostility was associated with higher burden of blood pressure, especially in males. This provides a new perspective on how hostility can worsen the outcome of patients combined who have both hypertension and depression, which suggests clinical psychological interventions. Moreover, simple, inexpensive, non-invasive methods like ABPM, unstructured interview, and electronic medical records database were used in the process of data collection. These kinds of methods could be applied in developing countries for clinical diagnosis. The most important implication of the study is that timely identification of hostile emotions in patients during diagnosis and treatment can help physicians promptly conduct psychological interventions combined with routine hypertension management, which is very helpful in treating hypertension patients who also have depression and hostility.
Tables
Table 1. Characteristics of participants.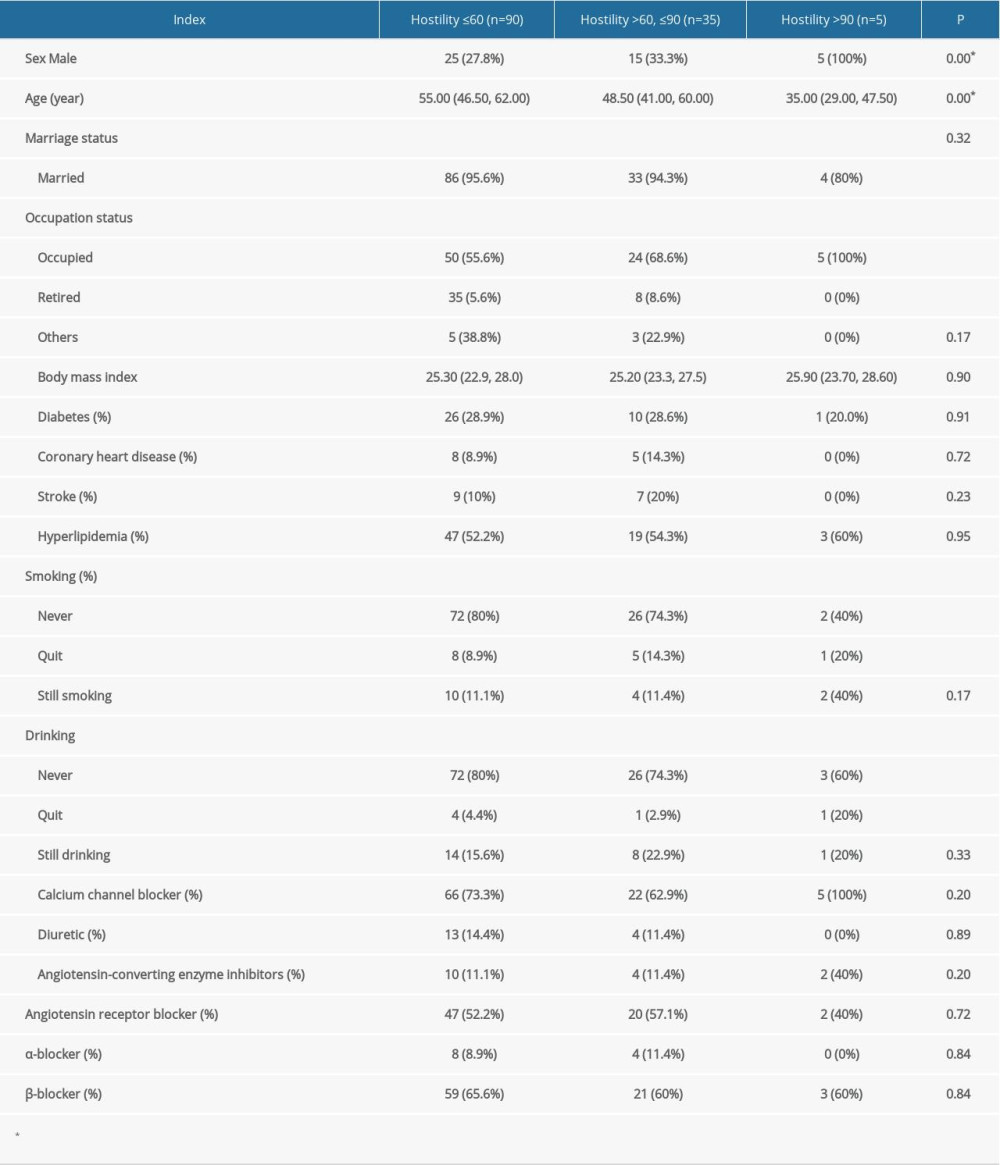 Table 2. Distribution of hostility and diastolic blood pressure load in males and females.
Table 2. Distribution of hostility and diastolic blood pressure load in males and females.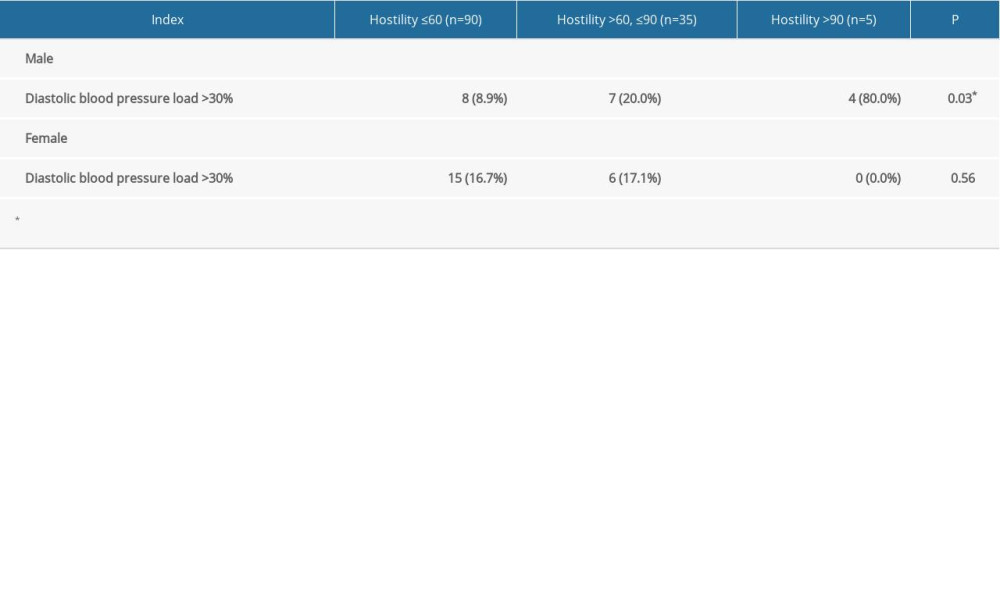 Table 3. Mean and SD of subscales of Symptom Checklist 90.
Table 3. Mean and SD of subscales of Symptom Checklist 90.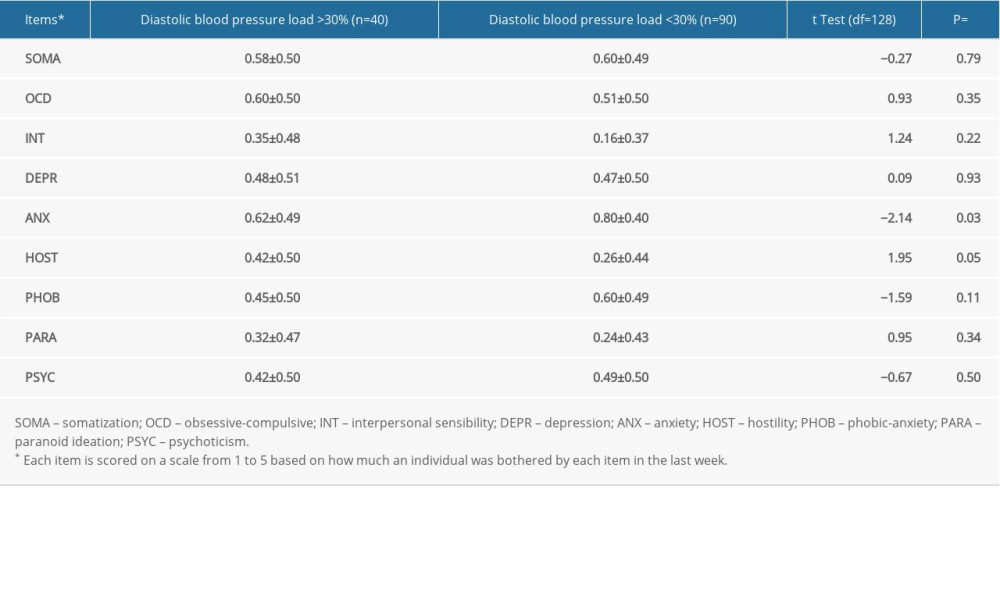 Table 4. Logistic regression of hostility and diastolic blood pressure load.
Table 4. Logistic regression of hostility and diastolic blood pressure load.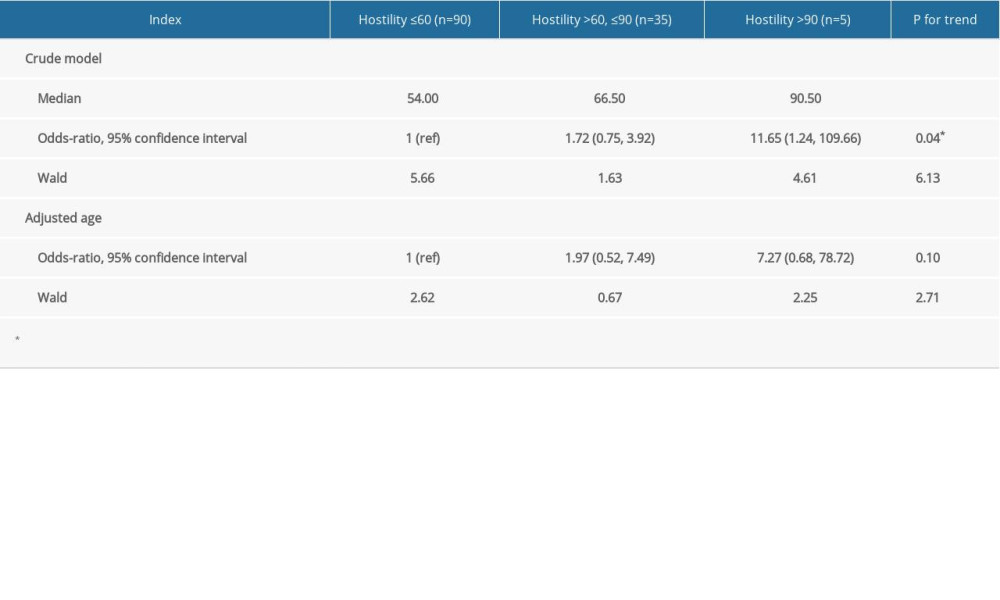 Table 5. Logistic regression of hostility and diastolic blood pressure load in males.
Table 5. Logistic regression of hostility and diastolic blood pressure load in males.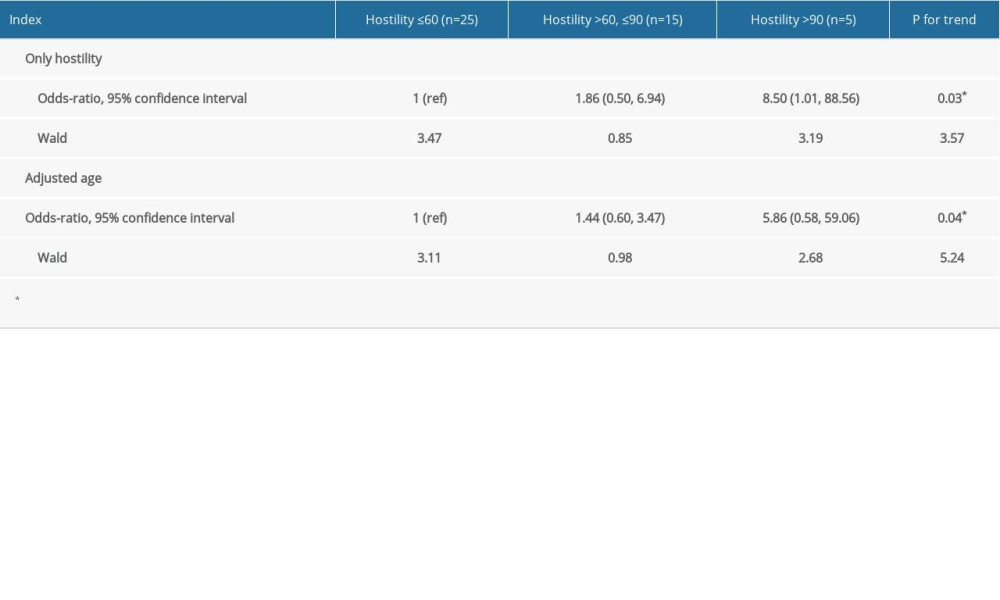 Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%.
Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%.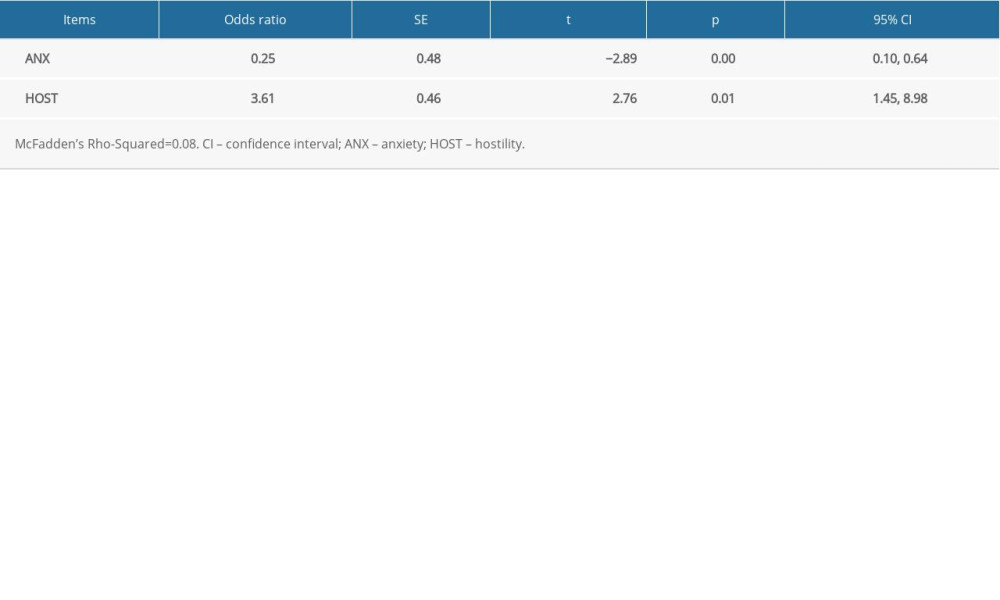
References
1. Chow CK, Teo KK, Rangarajan S, Prevalence, awareness, treatment, and control of hypertension in rural and urban communities in high-, middle-, and low-income countries: JAMA, 2013; 310(9); 959-68
2. Lang IM, Palazzini M, The burden of comorbidities in pulmonary arterial hypertension: Eur Heart J Suppl, 2019; 21(Suppl K); K21-28
3. Li Z, Li Y, Chen L, Prevalence of depression in patients with hypertension: A systematic review and meta-analysis: Medicine (Baltimore), 2015; 94(31); e1317
4. Li Z, Li Y, Chen L, Prevalence of depression in patients with hypertension. A systematic review and meta-analysis: Erratum: Medicine (Baltimore), 2018; 97(22); e11059
5. Agustini B, Mohebbi M, Woods RLASPREE Investigator Group, The association of antihypertensive use and depressive symptoms in a large older population with hypertension living in Australia and the United States: A cross-sectional study: J Hum Hypertens, 2020; 34(11); 787-94
6. Doubova SV, Martinez-Vega IP, Aguirre-Hernandez R, Association of hypertension-related distress with lack of self-care among hypertensive patients: Psychol Health Med, 2017; 22(1); 51-64
7. Dell’Osso L, Carmassi C, Mucci F, Depression, serotonin and tryptophan: Curr Pharm Des, 2016; 22(8); 949-54
8. Kraus C, Castrén E, Kasper S, Serotonin and neuroplasticity – Links between molecular, functional and structural pathophysiology in depression: Neurosci Biobehav Rev, 2017; 77; 317-26
9. Williams MS, Ziegelstein RC, McCann UD, Platelet serotonin signaling in patients with cardiovascular disease and comorbid depression: Psychosom Med, 2019; 81(4); 352-62
10. Zhang Y, Chen Y, Ma L, Depression and cardiovascular disease in elderly: Current understanding: J Clin Neurosci, 2018; 47; 1-5
11. Yano Y, Reis JP, Tedla YG, Racial differences in associations of blood pressure components in young adulthood with incident cardiovascular disease by middle age: Coronary Artery Risk Development in Young Adults (CARDIA) study: JAMA Cardiol, 2017; 2(4); 381-89
12. Franklin SS, Lopez VA, Wong ND, Single versus combined blood pressure components and risk for cardiovascular disease: The Framingham Heart Study: Circulation, 2009; 119(2); 243-50
13. Dinkel A, Schneider A, Schmutzer GThe quality of the family physician-patient relationship. Patient-related predictors in a sample representative for the german population: Psychother Psychosom Med Psychol, 2016; 66(3–4); 120-27 [in German]
14. Moreno JK, Selby MJ, Fuhriman A, Laver GD, Hostility in depression: Psychol Rep, 1994; 75(3 Pt 1); 1391-401
15. Hibbeln JR, Umhau JC, Linnoila M, A replication study of violent and nonviolent subjects: Cerebrospinal fluid metabolites of serotonin and dopamine are predicted by plasma essential fatty acids: Biol Psychiatry, 1998; 44(4); 243-49
16. Steel JL, Cheng H, Pathak R, Psychosocial and behavioral pathways of metabolic syndrome in cancer caregivers: Psychooncology, 2019; 28(8); 1735-42
17. Newman JD, Davidson KW, Shaffer JA, Observed hostility and the risk of incident ischemic heart disease: A prospective population study from the 1995 Canadian Nova Scotia Health Survey: J Am Coll Cardiol, 2011; 58(12); 1222-28
18. Gaborieau V, Delarche N, Gosse P, Ambulatory blood pressure monitoring versus self-measurement of blood pressure at home: Correlation with target organ damage: J Hypertens, 2008; 26(10); 1919-27
19. Ringrose JS, Bapuji R, Coutinho W, Patient perceptions of ambulatory blood pressure monitoring testing, tolerability, accessibility, and expense: J Clin Hypertens (Greenwich), 2020; 22(1); 16-20
20. Zachariah PK, Sumner WR, The clinical utility of blood pressure load in hypertension: Am J Hypertens, 1993; 6(6 Pt 2); 194S-97S
21. Strandberg TE, Pitkala K, What is the most important component of blood pressure: Systolic, diastolic or pulse pressure?: Curr Opin Nephrol Hypertens, 2003; 12(3); 293-97
22. Wang ZYSymptom Checklist 90 (SCL-90): Shanghai Psychiatry, 1984(2); 68-70 [in Chinese]
23. Derogatis LR, Lipman RS, Rickels K, The Hopkins Symptom Checklist (HSCL):A self-report symptom inventory: Behav Sci, 1974; 19(1); 1-15
24. Liu X, Effect of a mindfulness-based intervention program on comprehensive mental health problems of Chinese undergraduates: Community Ment Health J, 2019; 55(7); 1179-85
25. Yan LL, Liu K, Matthews KA, Psychosocial factors and risk of hypertension. The Coronary Artery Risk Development in Young Adults (CARDIA) study: JAMA, 2003; 290(16); 2138-48
26. Eleni K, Charalabos P, Efstathios M, Dipping status and hostility in newly diagnosed essential hypertension: Int J Psychiatry Med, 2011; 42(2); 181-94
27. Ginty AT, Carroll D, Roseboom TJ, Depression and anxiety are associated with a diagnosis of hypertension 5 years later in a cohort of late middle-aged men and women: J Hum Hypertens, 2013; 27(3); 187-90
28. Räikkönen K, Matthews KA, Flory JD, Effects of hostility on ambulatory blood pressure and mood during daily living in healthy adults: Health Psychol, 1999; 18(1); 44-53
29. Heine BE, Sainsbury P, Chynoweth RC, Hypertension and emotional disturbance: J Psychiatr Res, 1969; 7(2); 119-30
30. Spruill TM, Shallcross AJ, Ogedegbe G, Psychosocial correlates of nocturnal blood pressure dipping in African Americans: The Jackson Heart Study: Am J Hypertens, 2016; 29(8); 904-12
31. Tilov B, Semerdzhieva M, Bakova D, Study of the relationship between aggression and chronic diseases (diabetes and hypertension): J Eval Clin Pract, 2016; 22(3); 421-24
32. Girard D, Tardif JC, Boisclair Demarble J, Trait hostility and acute inflammatory responses to stress in the laboratory: PLoS One, 2016; 11(6); e0156329
33. Daniels IN, Harrell JP, Floyd LJ, Hostility, cultural orientation, and casual blood pressure readings in African Americans: Ethn Dis, 2001; 11(4); 779-87
34. Linden W, Chambers L, Maurice J, Sex differences in social support, self-deception, hostility, and ambulatory cardiovascular activity: Health Psychol, 1993; 12(5); 376-80
35. Chida Y, Steptoe A, The association of anger and hostility with future coronary heart disease: A meta-analytic review of prospective evidence: J Am Coll Cardiol, 2009; 53(11); 936-46
36. Tellawi G, Williams MT, Chasson GS, Interpersonal hostility and suspicious thinking in obsessive-compulsive disorder: Psychiatry Res, 2016; 243; 295-302
37. Osamor PE, Social support and management of hypertension in South-West Nigeria: Cardiovasc J Afr, 2015; 26(1); 29-33
38. Hernelahti M, Levalahti E, Simonen RL, Relative roles of heredity and physical activity in adolescence and adulthood on blood pressure: J Appl Physiol, 2004; 97; 1046-52
39. Krieger H, Morton NE, Rao DC, Azevedo E, Familial determinants of blood pressure in northeastern Brazil: Hum Genet, 1980; 53; 415-18
Tables
 Table 1. Characteristics of participants.
Table 1. Characteristics of participants. Table 2. Distribution of hostility and diastolic blood pressure load in males and females.
Table 2. Distribution of hostility and diastolic blood pressure load in males and females. Table 3. Mean and SD of subscales of Symptom Checklist 90.
Table 3. Mean and SD of subscales of Symptom Checklist 90. Table 4. Logistic regression of hostility and diastolic blood pressure load.
Table 4. Logistic regression of hostility and diastolic blood pressure load. Table 5. Logistic regression of hostility and diastolic blood pressure load in males.
Table 5. Logistic regression of hostility and diastolic blood pressure load in males. Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%.
Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%. Table 1. Characteristics of participants.
Table 1. Characteristics of participants. Table 2. Distribution of hostility and diastolic blood pressure load in males and females.
Table 2. Distribution of hostility and diastolic blood pressure load in males and females. Table 3. Mean and SD of subscales of Symptom Checklist 90.
Table 3. Mean and SD of subscales of Symptom Checklist 90. Table 4. Logistic regression of hostility and diastolic blood pressure load.
Table 4. Logistic regression of hostility and diastolic blood pressure load. Table 5. Logistic regression of hostility and diastolic blood pressure load in males.
Table 5. Logistic regression of hostility and diastolic blood pressure load in males. Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%.
Table 6. Logistic regression analysis of subscales between patients with high DBP load >30% and <30%. In Press
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952