10 March 2021: Clinical Research
High-Resolution Magnetic Resonance Imaging (HR-MRI) Imaging Characteristics of Vertebral Artery Dissection with Negative MR Routine Scan and Hypoperfusion in Arterial Spin Labeling
Yonggang Zhang1BCDEG, Chongchang Miao1CDEG, Yan Gu1ACDF*, Shunbin Jiang1BD, Jian Xu1ABCDOI: 10.12659/MSM.929445
Med Sci Monit 2021; 27:e929445
Abstract
BACKGROUND: Unruptured vertebral artery dissection (VAD) that causes ischemic infarction may require anticoagulant therapy or other treatments. However, anticoagulation therapy is not recommended for patients without ischemic infarction. To date, there has been no research on the imaging characteristics of patients with ischemic hypoperfusion that have a negative routine MRI scan.
MATERIAL AND METHODS: Patients with suspected VAD were recruited between June 2015 and June 2020 in order to perform high-resolution magnetic resonance imaging (HR-MRI). In total, 26 patients with negative MRI routine scans that underwent arterial spin labeling (ASL) examination were included in the study. The patients were divided into the hypoperfusion group and normal group based on whether hypoperfusion was found in ASL. The clinical features and HR-MRI features between these 2 groups were analyzed.
RESULTS: There were no statistical differences between the hypoperfusion group and normal group based on the patient’s clinical characteristics (P>0.05). According to imaging characteristics between the 2 groups, the effective lumen index and the vertebrobasilar artery minimum angle were statistically significant (P<0.001). Therefore, a vertebrobasilar artery minimum angle <90° was negatively correlated to the posterior circulation ischemia hypoperfusion, with a correlation coefficient of –0.686. The effective lumen index was also negatively correlated to the posterior circulation ischemia hypoperfusion, with a correlation coefficient of –0.671. However, the location of the dissection and other HR-MRI characteristics were not statistically significant between these 2 groups (P>0.05).
CONCLUSIONS: The hypoperfusion of posterior circulation ischemia caused by VAD is related to the effective lumen index, as well as the vertebrobasilar artery minimum angle.
Keywords: Ischemia, Magnetic Resonance Imaging, Vertebral Artery Dissection, Arteries, Radionuclide Imaging, Spin Labels, Vertebral Artery
Background
Arterial dissection refers to the intramural hematoma caused by a tear of the vascular intima or a rupture of the nourishing blood vessel, which is located either under the intima or adventitia. The former can lead to a secondary onset of vascular stenosis and occlusion, while the latter can easily cause lumen dilation [1]. Cervicocerebral artery dissection (CAD) is an important cause of ischemic stroke among young and middle-aged people in Asia [2]. Owing to a lack of specificity of clinical manifestations, a diagnosis of arterial dissection largely depends on imaging examination. Despite the fact that digital subtraction angiography (DSA) is regarded as the criterion standard for diagnosing intracranial vascular disease, the condition of the vessel wall itself cannot be observed. Hence, its diagnostic value for artery dissection with a normal lumen or non-specific stenosis or occlusion is limited [3]. Based on this, researchers recommend the application of arterial wall combined with luminal imaging technology to diagnose arterial dissection, and have pointed out that the diagnosis of dissection disease requires evidence of intramural hematoma or characteristics of dynamic imaging changes [4,5]. As a multi-parameter imaging sequence with ideal tissue contrast and spatial resolution, high-resolution magnetic resonance imaging (HR-MRI) is not only able to obtain luminal morphology information, but more importantly, the characteristic intramural hematoma, intimal flap, and double-lumen sign caused by arterial dissection can be directly visualized through wall imaging [6,7]. Therefore, HR-MRI is recommended as the first choice for diagnosing arterial dissection [4,8].
The specific etiology of CAD is currently unknown. The susceptibility factors based on epidemiology include hypertension, migraine, history of trauma, and recent infection [9]. In recent years, an increasing number of studies have concluded that most dissections tend to have a benign course. It has been recommended that patients with milder symptoms of unruptured dissection should be treated conservatively first and then followed up with imaging on a regular basis. Conservative treatment includes observation of mild symptoms or symptomatic treatment, treatment of acute stroke, and preventive treatment of recurrent ischemic stroke. According to the literature, for patients with ischemic symptoms without evidence of intracranial ischemia, the use of antiplatelet drugs or anticoagulants is controversial. Although these drugs can effectively prevent thrombotic occlusion or distal emboli, they can promote progression of dissection, which exacerbates ischemic symptoms and can cause rupture of aneurysm [10]. In some patients, despite the fact that MRI routine scans show normal manifestations, it does not necessarily mean that there is no intracranial ischemia focus in the brain. Arterial spin labeling (ASL) is a perfusion technique that does not require a contrast agent. It uses its own intravascular water molecules as an endogenous tracer, which can non-invasively and safely assess brain tissue blood perfusion, and can more objectively display intracranial ischemia than conventional MRI scans. At present, this technology has been widely used to assess blood perfusion in cerebrovascular and tumor diseases. Some patients have ischemia hypoperfusion but MRI plain scan can still be normal and there has not been a research report on how to treat these patients. Among CAD, vertebral artery dissection (VAD) is the most common. This study attempted to analyze the clinical and vascular wall morphological characteristics of patients with VAD who were negative on MRI routine scan but may show ischemic hypoperfusion in order to explore meaningful indicators that can guide the clinical treatments in a correct and individualized manner.
Material and Methods
RESEARCH SUBJECTS:
This study protocol was approved by the Ethics Committee of our hospital (201506002). All patients included in the study signed informed consent prior to undergoing HR-MRI examination. From June 2015 to June 2020, patients ages 18–50 years old with suspected CAD were consecutively recruited from the Department of Neurosurgery at our hospital. The baseline clinical data of patients, including sex, age, hypertension, smoking history, clinical manifestations, and time of onset, were recorded. After diagnosis, all patients underwent anticoagulation therapy or symptomatic conservative treatment based on imaging manifestations and clinical symptoms. The follow-up visit for recovery was carried out 1 month after treatment.
Specific inclusion criteria included:
Exclusion criteria included:
IMAGE INSPECTION:
The all-digital magnetic resonance scanner (Philips Ingenia 3.0T) was used for scanning. Patients were required to keep their head still during the scan. All patients underwent head MRI plain scan and three-dimensional time-of-flight (3D-TOF) MRA first. Patients who were negative on the MRI plain scan underwent 3D-ASL. Two phases (PLD 1.5s and PLD 2.5s) of 3D-ASL were acquired. According to the original axial image of 3D-TOF-MRA, the location was conducted along the long axis of the blood vessel, and the coronal scan of HR-MRI was carried out at a thickness of 1 mm. The scanning sequence and parameters of HR-MRI included: (1) T1WI VISTA, TR/TE 800 ms/70 ms, FOV l60 mm×160 mm, thickness 1 mm, matrix 272×271; (2) T2WI VISTA, TR/TE 1800 ms/236 ms, FOV l60 mm×160mm, thickness 1 mm, matrix 276×271. T1WI VISTA coronal scanning was adopted for enhanced sequences, with an intravenous injection of 10% Gd.DTPA. A dose of 0.2 ml/kg body weight was used, and the flow rate of manual injection into the median cubital vein was approximately 1.5–3 ml/s. At 5 min after injection, the enhanced scanning was carried out and the catheter was flushed using 50 ml of normal saline.
DIAGNOSTIC CRITERIA FOR VAD:
HR-MRI showed indications of intra-vertebral artery hematoma (high signal of the crescent around the artery on T1WI), intimal flap, or double-lumen signs, all of which suggest VAD [11–13].
HR-MRI images of each patient were analyzed and diagnosed by 2 independent neuroradiologists with substantial experience in analysis. Both neuroradiologists were blinded to patient clinical information. When encountering divergent diagnoses for the same patient, the final decision was made after consultation with the entire imaging department.
The Likert scale [14] was used to classify image quality, and the image was scored from 1 to 5 points. Images with a score ≤3 points were discarded. The scoring standards included:
RELEVANT CLINICAL RISK FACTORS AND RESEARCH INDEX DEFINITIONS:
The demographic characteristics, vascular-related risk factors, and clinical manifestations of enrolled patients were collected. The risk factors include:
STATISTICAL ANALYSIS:
Data analysis was performed using the SPSS16.0 software. Depending on whether hypoperfusion occurred in ASL, VAD was divided into either the ASL hypoperfusion or the normal group. Measurement data presented normal distribution, which was expressed as mean±SD. The independent-samples
Results
BASELINE DATA ANALYSIS OF PATIENTS WITH DISSECTION:
In total, 97 patients with suspected head and neck dissection due to clinical symptoms underwent HR-MRI imaging. Among them, 68 patients were diagnosed as VAD by HR-MRI, while 58 confirmed patients were unilateral VAD. Additionally, 31 patients were examined within 7 days of onset, among which 27 were negative on MRI routine scan. One patient had poor coordination during examination, and showed movement artifacts. Since their Likert scale score was 3, they did not meet the diagnostic requirements. Therefore, a total of 26 patients were included in the study.
Among these 26 patients (14 females, 12 males), 17 patients had normal ASL (Figure 2), while 9 patients had hypoperfusion with ASL (Figure 3). The baseline data of 26 patients with VAD are shown in Table 1. There was no statistically significant difference between the hypoperfusion and normal group with regards to sex, age, BMI, hypertension, and drinking history.
ANALYSIS OF HR-MRI IMAGING INDEXES OF PATIENTS WITH DISSECTION:
The differences in HR-MRI imaging characteristics of 26 patients with VAD between the 2 groups are shown in Table 2. We found that the vertebrobasilar artery minimum angle was significantly smaller in the hypoperfusion group compared to the normal group (P<0.001). The differences between the 2 groups were statistically significant, which indicated a negative correlation and a correlation coefficient r=−0.686. The vertebrobasilar artery minimum angle less than 90o was more likely to cause posterior circulation hypoperfusion. The effective lumen index in the hypoperfusion group was lower compared to the normal group, and differences between the 2 groups were statistically significant (P<0.001), but with a negative correlation. The correlation coefficient was r=−0671. However, there were no significant differences with regards to location of dissection, basilar artery curvature, hematoma distribution, enhancement, and other characteristics among the 2 groups.
TREATMENT AND FOLLOW-UP OF PATIENTS WITH DISSECTION:
Overall, there were 9 cases of hypoperfusion in 26 patients with ASL. Additionally, 2 patients progressed to cerebral infarction due to a worsening of symptoms within 3 days after the examination, and were treated using antiplatelet and statins therapy. The other 7 cases were treated with antiplatelet therapy alone. Finally, 17 patients who showed negative signs of perfusion were treated conservatively and symptomatically, and their symptoms were significantly relieved at 1 month of follow-up.
Discussion
In this study, we discuss the characteristics of young and middle-aged patients with VAD who only show low perfusion but have negative MRI routine scan. We found no differences in clinical baseline data of patients in the hypoperfusion group and the normal group. In addition, with regards to the imaging characteristics of the lesion, we found that the bending angle of the basilar artery between the 2 groups was not significantly different. However, the vertebrobasilar artery minimum angle was statistically different among the 2 groups. Furthermore, when the bending angle was less than 90°, it was negatively correlated with the hypoperfusion group, with a correlation coefficient of −0.686. The smaller the angle, the greater the chance of ischemia.
There are few studies on the bending angle of the vertebrobasilar artery in VAD patients. Previous researchers [15–18] have found that vertebrobasilar dysplasia was related to VAD and posterior circulation ischemia according to research on vertebrobasilar dysplasia. The reason included that the bending of blood vessels can easily cause blood retention, slow flow rate, and cause insufficient blood supply to the distal end, and the curved blood vessels can also cause high blood flow resistance, which easily results in hypoperfusion infarction when the blood pressure fluctuates or blood volume is insufficient. Under physiological state, due to the existence of the compensatory mechanism of human blood supply, the changes can cause occurrence of non-obvious subjective symptoms. Nonetheless, with increasing age, the occurrence of vascular diseases and degenerative diseases, and coupled with a decline of the body’s compensatory ability, different degrees of cerebral ischemia symptoms can occur [19]. Kim et al [20] studied the influence of the morphological characteristics of the vertebrobasilar artery on the prognosis of VAD and concluded that patients with unruptured VADs who possess less BA (basilar artery) bending, a smaller VUBA (vertebral-union-basilar angle) and VUVA (vertebral-union-vertebral angle) could have a better prognosis compared with those without such features. They speculate that enlargement of the VUBA, VUVA, proximity of the dissection to the BA, and BA bending could cause changes in blood inflow and VA shear stress. These changes could heighten the vulnerability of the VA, thus affecting vascular healing. Although the definitions of the specific vertebrobasilar artery bending angles they studied are different and the purpose of the research is also different, their research principles are similar to this research. However, these studies include elderly patients over the age of 50 years. The selected population in this study included young and middle-aged people between 18 and 50 years old. Compared to the patients in the other studies, the relative vascular condition in this study is better, with a lower incidence of vascular disease and degeneration. In this study, the average bending angle of the basilar artery is 133°, with the conclusion that the curvature of VAD is related to the basilar artery, which is consistent with results of many researchers. However, no statistically significant difference was found between the 2 groups. The primary reason may be that the basilar artery curvature is a predisposing factor of dissection, and is not necessarily a cause for ischemia, although ischemia is also correlated to the angle of basilar artery curvatures. Among the 26 cases analyzed in this study, the basilar artery curvature grade was small, with a few cases showing a basilar artery curvature angle of less than 90°. However, in this study, the vertebrobasilar artery minimum angle was related to hypoperfusion ischemia. Our analysis indicates 2 reasons for this. First, if the dissection is located in the proximal segment of V1–3 or V4, the vertebrobasilar artery minimum angle is selected according to the minimum angle of the bending angle between basilar artery and the V4 segment of the vertebral artery. Therefore, the angle is more likely to be lower than 90°. Second, in this ischemic hypoperfusion group, the proportion of vertebrobasilar artery minimum angle less than 90° was 8/9. Obviously, the proportion of bending angles lower than 90° was greater. The greater the bending angle, the easier the change of blood flow form, which can eventually form a vortex and cause a decrease in blood flow speed. Since the curved inner wall has low wall shear stress and high blood flow resistance, when blood pressure fluctuates or blood volume is insufficient, the blood supply disorder occurred in the posterior circulatory system to form hypoperfusion or even infarction [21].
Studies have indicated that the blood flow velocity is proportional to the 4th power of the vessel radius [22], indicating that blood flow velocity is slow when the vessel lumen is narrow. As the dissection mostly occurs in the endothelium, blood enters between the intima and the medium, and then coagulates rapidly [23], leading to different degrees of stenosis of the lumen. In this study, we found that the difference in effective lumen index was statistically significant between the hypoperfusion and the normal group. The effective lumen index was smaller in the ischemia hypoperfusion group, which was negatively correlated. We found that because the effective inner diameter of the lumen was smaller, the blood flow of the affected vertebral artery was lower, and the lower blood flow into the posterior circulation tissue was dominated by the patient’s vertebral artery per unit time, leading to hypoperfusion in ASL. Even in extreme cases, when the effective lumen index of the blood vessel was as small as almost 0, it causes the vertebral artery on the affected side to collapse, leading to obstruction of the ipsilateral blood vessel, and ultimately leading to appearance of large-scale infarction on the same side of the dissection.
In addition, we found in this study that the occurrence of ischemia caused by dissection was not related to location or morphology. Furthermore, among the 26 patients that underwent enhanced vascular wall imaging, 25 had vascular wall enhancement. Studies have shown that enhancement of the vascular wall may be related to inflammation or repair response after occurrence of arterial dissection [24,25]. Finally, studies have suggested that enhancement of the dissected vascular wall may originate from slow blood flow of the false lumen or arterial nourishment blood vessels [26]. We did not do a final pathological study, and so we also agree with their speculation. However, between the 2 groups, punctate enhancement and diffuse enhancement were not significantly different between the 2 groups, which indicates that enhancement and the enhancement type of the dissection wall were not practically significant in distinguishing whether dissection had ischemic changes.
This study had some limitations. First, data from this study are based on a single research center, which cannot represent all ischemic manifestations of VAD, leading to bias. Secondly, few cases were included in the study, and risk factor prediction studies could not be conducted; only simple correlation analysis could be conducted. Hence, future multi-center and large-sample studies are needed. Third, as DSA is an invasive examination, none of the patients underwent the criterion standard DSA examination.
Although this study has certain limitations, it still imparts important information. In patients with VAD, we need to pay particular attention to those patients with infarcts on MRI routine scans, as they might actually have ischemia. Therefore, we believe that for those dissection patients with negative MRI routine scans, ASL should be carried out to determine whether it is an actual ischemic disease. This is particularly true for patients with dissection lesions where the vertebrobasilar artery minimum angle is less than 90° and the effective lumen index is small. Thus, it should be highly suspected that there is ischemic lesion in the cranium, which needs to be taken seriously in order to optimize stroke prevention and perform treatment through early management.
Conclusions
Posterior circulation ischemia in patients with VAD is related to the vertebrobasilar artery minimum angle and effective lumen index. For patients with a vertebrobasilar artery minimum angle less than 90° and a small effective lumen index, the incidence of ischemia is higher. It has been recommended that antiplatelet therapy should be actively performed for strict control of risk factors, and patients with worsening symptoms need further antiplatelet and statins therapy or endovascular therapy. However, patients without these manifestations and a negative ASL should be treated conservatively and symptomatically.
Figures
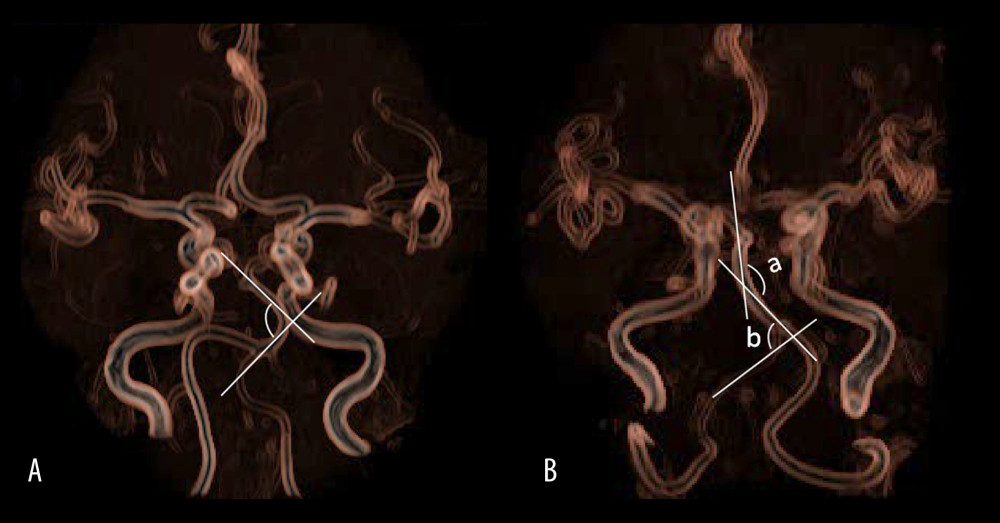 Figure 1. (A) is a schematic diagram to measure the bending angle of the basilar artery. The arrow indicates the angle formed by 2 sides of the basilar artery curvature toward the midline. (B) is a schematic diagram to measure the vertebrobasilar artery minimum angle. Take the smallest angle of the distal base artery or the V4 segment of the vertebral artery in the dissection lesion. The vertebral-basal artery at the distal end of the dissection lesion formed 2 angles, which were the basilar artery bending angle and the vertebral artery bending angle. The vertebral artery angle was 85°, while the basilar artery bending angle was 135°. Therefore, the vertebrobasilar artery minimum angle was 85°.
Figure 1. (A) is a schematic diagram to measure the bending angle of the basilar artery. The arrow indicates the angle formed by 2 sides of the basilar artery curvature toward the midline. (B) is a schematic diagram to measure the vertebrobasilar artery minimum angle. Take the smallest angle of the distal base artery or the V4 segment of the vertebral artery in the dissection lesion. The vertebral-basal artery at the distal end of the dissection lesion formed 2 angles, which were the basilar artery bending angle and the vertebral artery bending angle. The vertebral artery angle was 85°, while the basilar artery bending angle was 135°. Therefore, the vertebrobasilar artery minimum angle was 85°. 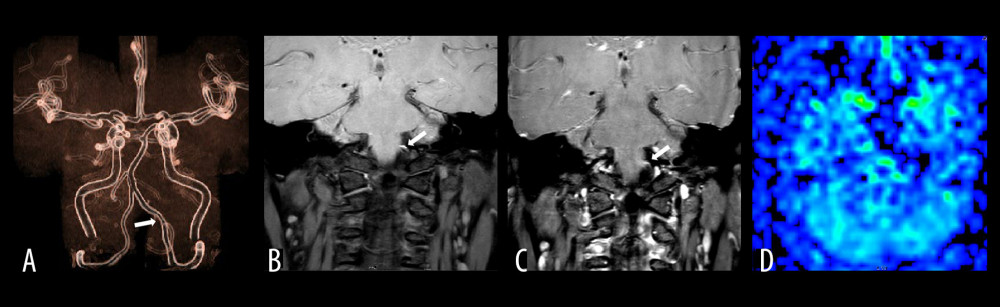 Figure 2. The left vertebral artery V4 proximal dissection images of a 45-year-old male patient with dizziness for 3 days. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which was measured to be approximately 135°. (B) Is a T1 VISTA scan image, which shows an eccentric crescent-shaped high signal at the proximal end of the left vertebral artery. (C) Is a punctate enhancement of the vessel wall after T1VSTA-enhancement. (D) Is an ASL image, and the manifestation of hypoperfusion in posterior circulation area on both sides is invisible.
Figure 2. The left vertebral artery V4 proximal dissection images of a 45-year-old male patient with dizziness for 3 days. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which was measured to be approximately 135°. (B) Is a T1 VISTA scan image, which shows an eccentric crescent-shaped high signal at the proximal end of the left vertebral artery. (C) Is a punctate enhancement of the vessel wall after T1VSTA-enhancement. (D) Is an ASL image, and the manifestation of hypoperfusion in posterior circulation area on both sides is invisible. 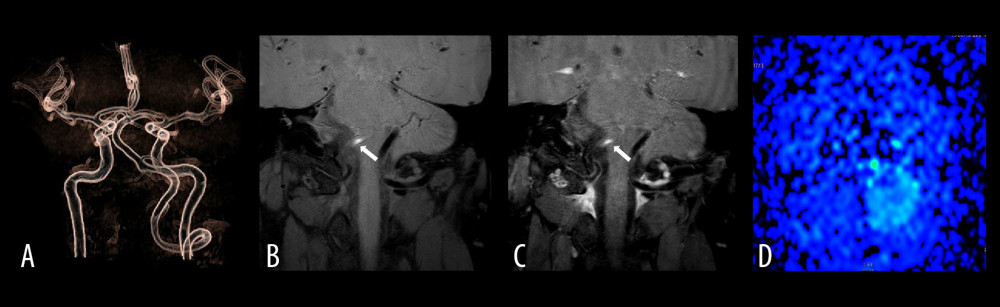 Figure 3. The right vertebral artery V4 proximal dissection images of a 40-year-old female patient with dizziness and instable walking for 6 hours. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which is measured to be approximately 75°. (B) Is a T1 VISTA scan image, showing eccentric crescent-shaped high signal at the proximal end of the right vertebral artery. (C) Shows no enhancement of vessel wall after T1 VISTA-enhancement. (D) Is an ASL image, and the right cerebellar hemisphere shows hypoperfusion.
Figure 3. The right vertebral artery V4 proximal dissection images of a 40-year-old female patient with dizziness and instable walking for 6 hours. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which is measured to be approximately 75°. (B) Is a T1 VISTA scan image, showing eccentric crescent-shaped high signal at the proximal end of the right vertebral artery. (C) Shows no enhancement of vessel wall after T1 VISTA-enhancement. (D) Is an ASL image, and the right cerebellar hemisphere shows hypoperfusion. References
1. Schievink WI, Spontaneous dissection of the carotid and vertebral arteries: N Engl J Med, 2001; 344; 898-906
2. Debette S, Compter A, Labeyrie MA, Epidemiology, pathophysiology, diagnosis, and management of intracranial artery dissection: Lancet Neurol, 2015; 14; 640-54
3. Lee SH, Jung JM, Kim KY, Intramural hematoma shape and acute cerebral infarction in intracranial artery dissection: A high-resolution magnetic resonance imaging study: Cerebrovasc Dis, 2020; 49; 269-76
4. Debette S, Compter A, Labeyrie MA, Epidemiology, pathophysiology, diagnosis, and management of intracranial artery dissection: Lancet Neurol, 2015; 14; 640-54
5. Mandell DM, Mossa-Basha M, Qiao Y, Intracranial vessel wall MRI: principles and expert consensus recommendations of the American society of neuroradiology: Am J Neuroradiol, 2017; 38; 218-29
6. Choi JW, Han M, Hong JM, Feasibility of improved motion-sensitized driven-equilibrium (iMSDE) prepared 3D T1-weighted imaging in the diagnosis of vertebrobasilar artery dissection: J Neuroradiol, 2018; 45; 186-91
7. Yun SY, Heo YJ, Jeong HW, Spontaneous intracranial vertebral artery dissection with acute ischemic stroke: High-resolution magnetic resonance imaging findings: Neuroradiol J, 2018; 1; 262-69
8. Yuan X, Cui X, Gu H, Evaluating cervical artery dissections in young adults: A comparison study between high-resolution MRI and CT angiography: Int J Cardiovasc Imaging, 2020; 36; 1113-19
9. Ro A, Kageyama N, Pathomorphological differentiation between traumatic rupture and nontraumatic arterial dissection of the intracranial vertebral artery: Leg Med (Tokyo), 2014; 16; 121-27
10. Vineetha VS, Sreedharan SE, Sarma PS, Antiplatelets versus anticoagulants in the treatment of extracranial carotid and vertebral artery dissection: Neurol India, 2019; 67; 1056-59
11. Park KJ, Jung SC, Kim HS, Multi-contrast high-resolution magnetic resonance findings of spontaneous and unruptured intracranial vertebral artery dissection: Qualitative and quantitative analysis according to stages: Cerebrovasc Dis, 2016; 42; 23-31
12. Zhang FL, Liu Y, Xing YQ, Diagnosis of cervical artery dissection using 3-T magnetic resonance imaging: JAMA Neurol, 2015; 72; 600-1
13. Atsina KB, Rothstein A, Messé SR, Intracranial vessel wall MR imaging of an intradural vertebral artery dissection: Clin Imaging, 2020; 68; 108-10
14. Woo S, Kim SY, Cho JY, Apparent diffusion coefficient for prediction of parametrial invasion in cervical cancer: A critical evaluation based on stratification to a Likert scale using T2-weighted imaging: Radiol Med, 2018; 123; 209-16
15. Zhou M, Zheng H, Gong S, Vertebral artery hypoplasia and vertebral artery dissection. A hospital-based cohort study: Neurology, 2015; 84; 818-24
16. Hori S, Hori E, Umemura K, Anatomical variations of vertebrobasilar artery are closely related to the occurrence of vertebral artery dissection – an MR angiography study: J Stroke Cerebrovasc Dis, 2020; 29; 104636
17. Park M, Shin NY, Yoo J, Association between morphologic subtypes of vertebral artery dissection and vertebral artery hypoplastic appearance: Eur J Radiol, 2019; 116; 84-89
18. Hwang J, Chung JW, Cha J, Selective application of high-resolution 3 T MRI in the evaluation of intracranial vertebral artery dissection: J Neuroimaging, 2017; 27; 71-77
19. Cosar M, Yaman M, Eser O, Basilar artery angulation and vertigo due to the hemodynamic effect of dominant vertebral artery: Med Hypotheses, 2008; 70; 941-43
20. Kim MK, Lim YC, Conservative management of unruptured spontaneous intracranial vertebral artery dissection: World Neurosurg, 2019; 126; e402-9
21. Lee SH, Hur N, Jeong SK, Geometric analysis and blood flow simulation of basilar artery: J Atherosler Thromb, 2012; 19; 397-405
22. Nakamura Y, Hirayama T, Ikeda K, Clinicoradiologic features of vertebrobasilar dolichoectasia in stroke patients: J Stroke Cerebrovasc Dis, 2012; 21; 5-10
23. Tiu C, Terecoasa E, Grecu N, Vertebral artery dissection: A contemporary perspective: Maedica (Buchar), 2016; 11; 144-49
24. Saito A, Fujimura M, Endo H, Diagnostic value of contrast-enhanced magnetic resonance vessel wall imaging on the onset type of vertebral artery dissection: Cerebrovasc Dis, 2019; 48; 124-31
25. Arai D, Satow T, Komuro T, Evaluation of the arterial wall in vertebrobasilar artery dissection using high-resolution magnetic resonance vessel wall imaging: J Stroke Cerebrovasc Dis, 2016; 25; 1444-50
26. Sakurai K, Miura T, Sagisaka T, Evaluation of luminal and vessel wall abnormalities in subacute and other stages of intracranial vertebrobasilar artery dissections using the volume isotropic turbo-spin-echo acquisition (VISTA) sequence: A preliminary study: J Neuroradiol, 2013; 40; 19-28
Figures
 Figure 1. (A) is a schematic diagram to measure the bending angle of the basilar artery. The arrow indicates the angle formed by 2 sides of the basilar artery curvature toward the midline. (B) is a schematic diagram to measure the vertebrobasilar artery minimum angle. Take the smallest angle of the distal base artery or the V4 segment of the vertebral artery in the dissection lesion. The vertebral-basal artery at the distal end of the dissection lesion formed 2 angles, which were the basilar artery bending angle and the vertebral artery bending angle. The vertebral artery angle was 85°, while the basilar artery bending angle was 135°. Therefore, the vertebrobasilar artery minimum angle was 85°.
Figure 1. (A) is a schematic diagram to measure the bending angle of the basilar artery. The arrow indicates the angle formed by 2 sides of the basilar artery curvature toward the midline. (B) is a schematic diagram to measure the vertebrobasilar artery minimum angle. Take the smallest angle of the distal base artery or the V4 segment of the vertebral artery in the dissection lesion. The vertebral-basal artery at the distal end of the dissection lesion formed 2 angles, which were the basilar artery bending angle and the vertebral artery bending angle. The vertebral artery angle was 85°, while the basilar artery bending angle was 135°. Therefore, the vertebrobasilar artery minimum angle was 85°. Figure 2. The left vertebral artery V4 proximal dissection images of a 45-year-old male patient with dizziness for 3 days. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which was measured to be approximately 135°. (B) Is a T1 VISTA scan image, which shows an eccentric crescent-shaped high signal at the proximal end of the left vertebral artery. (C) Is a punctate enhancement of the vessel wall after T1VSTA-enhancement. (D) Is an ASL image, and the manifestation of hypoperfusion in posterior circulation area on both sides is invisible.
Figure 2. The left vertebral artery V4 proximal dissection images of a 45-year-old male patient with dizziness for 3 days. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which was measured to be approximately 135°. (B) Is a T1 VISTA scan image, which shows an eccentric crescent-shaped high signal at the proximal end of the left vertebral artery. (C) Is a punctate enhancement of the vessel wall after T1VSTA-enhancement. (D) Is an ASL image, and the manifestation of hypoperfusion in posterior circulation area on both sides is invisible. Figure 3. The right vertebral artery V4 proximal dissection images of a 40-year-old female patient with dizziness and instable walking for 6 hours. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which is measured to be approximately 75°. (B) Is a T1 VISTA scan image, showing eccentric crescent-shaped high signal at the proximal end of the right vertebral artery. (C) Shows no enhancement of vessel wall after T1 VISTA-enhancement. (D) Is an ASL image, and the right cerebellar hemisphere shows hypoperfusion.
Figure 3. The right vertebral artery V4 proximal dissection images of a 40-year-old female patient with dizziness and instable walking for 6 hours. (A) Is an MRA image. It can be seen that the vertebrobasilar artery minimum angle in this case is the basilar artery bending angle, which is measured to be approximately 75°. (B) Is a T1 VISTA scan image, showing eccentric crescent-shaped high signal at the proximal end of the right vertebral artery. (C) Shows no enhancement of vessel wall after T1 VISTA-enhancement. (D) Is an ASL image, and the right cerebellar hemisphere shows hypoperfusion. Tables
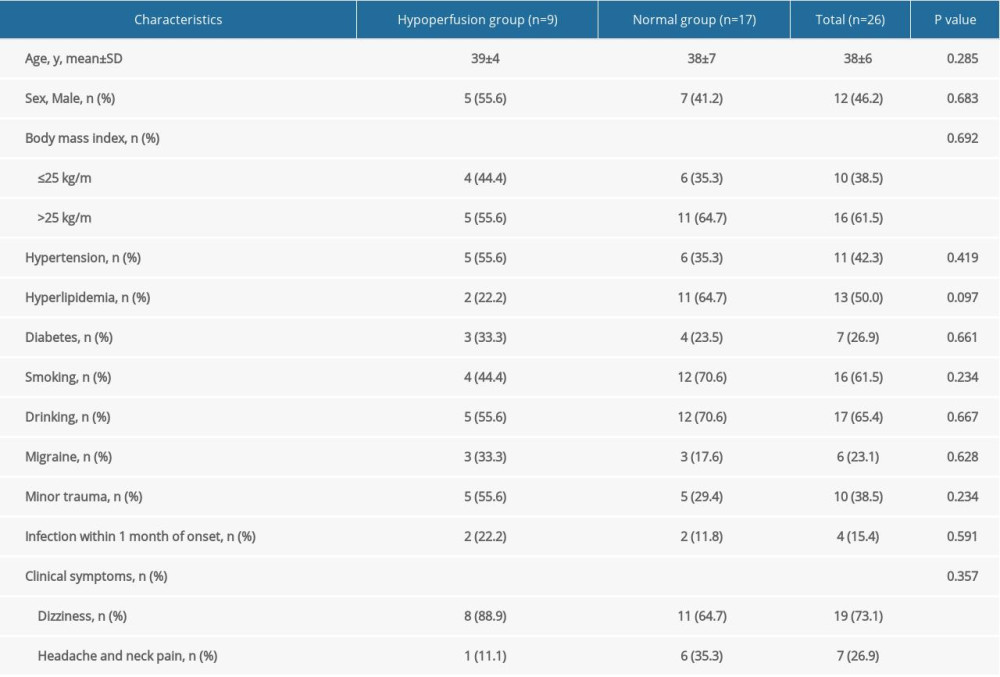 Table 1. Clinical characteristics of VAD with negative MRI routine scan categorized into 2 groups.
Table 1. Clinical characteristics of VAD with negative MRI routine scan categorized into 2 groups.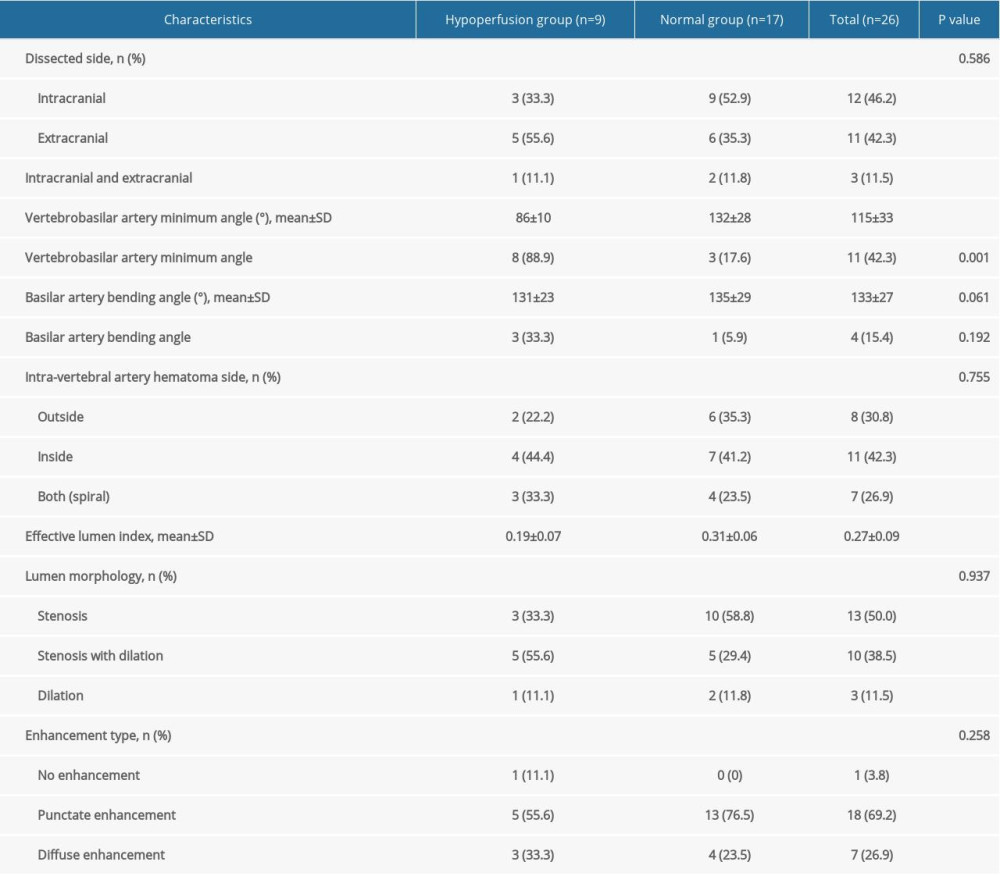 Table 2. Comparison of HR-MR characteristics of the 2 groups with VAD.
Table 2. Comparison of HR-MR characteristics of the 2 groups with VAD. Table 1. Clinical characteristics of VAD with negative MRI routine scan categorized into 2 groups.
Table 1. Clinical characteristics of VAD with negative MRI routine scan categorized into 2 groups. Table 2. Comparison of HR-MR characteristics of the 2 groups with VAD.
Table 2. Comparison of HR-MR characteristics of the 2 groups with VAD. In Press
05 Mar 2024 : Clinical Research
Muscular Function Recovery from General Anesthesia in 132 Patients Undergoing Surgery with Acceleromyograph...Med Sci Monit In Press; DOI: 10.12659/MSM.942780
05 Mar 2024 : Clinical Research
Effects of Thermal Insulation on Recovery and Comfort of Patients Undergoing Holmium Laser LithotripsyMed Sci Monit In Press; DOI: 10.12659/MSM.942836
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








