19 May 2021: Clinical Research
Bone Allograft and Locking Plate for Severe Proximal Humeral Fractures: Early and Late Outcomes
Elias Polykandriotis12CEF*, Annelie Zschiegner3BD, Raymund E. Horch2E, Matthias Schürmann4ACDGDOI: 10.12659/MSM.928982
Med Sci Monit 2021; 27:e928982
Abstract
BACKGROUND: Early failure of osteosyntheses is common even with use of locking plates. In patients with comminuted fractures and epiphyseal osseous defects, we performed a series of osteosyntheses by locking plate in combination with an allograft bone augmentation. Because of encouraging short-term results in the literature, we assumed that the method could be a potential alternative to a reverse shoulder prosthesis.
MATERIAL AND METHODS: Twenty-six patients with a dislocated proximal humeral fracture (Neer IV/V/VI) were studied. A lyophilized allogeneic bone graft was used to reinforce the humeral head fragments before locking plate osteosynthesis. The outcomes of fractures were assessed with Disabilities of the Arm, Shoulder and Hand (DASH) and Constant-Murley (Constant) scores, range of motion, a visual analog scale, and with radiological testing. The Constant-Murley scores were the endpoint of our study.
RESULTS: The Neer classification of the fractures was type IV in 4 patients, type V in 20 patients, and type VI in 2 patients. The mean DASH score was 52.85 (range, 4.17-79.3) and the mean Constant score was 39.26 (range, 17-88). We observed late necrosis of the humeral head in 15 of 24 patients (62.5%), although early radiological follow-up showed that the humeral head had been anatomically reconstructed.
CONCLUSIONS: Long-term follow-up demonstrated inferior functional results, as displayed by poor Constant scores. There was a high incidence of necrosis, in spite of initial anatomical reconstruction. Biointegration of the allogeneic bone graft and revascularization of the humeral head fragments could be impaired in geriatric patients who have gross dislocation. Therefore, augmentation of the humeral head with allogeneic bone grafts cannot be recommended in these patients.
Keywords: Allografts, Femur Head Necrosis, humeral head, Shoulder Fractures, Aged, 80 and over, Bone Plates, Bone Transplantation, Fracture Fixation, Internal, Fracture Healing, Radiography, Range of Motion, Articular
Background
Up to 86% of patients who experience a proximal humeral fracture (PHF) are older than age 60 years [1]. Eighty-seven percent of PHFs are low-energy injuries that occur as a result of a fall from standing height [1] and the proximal humerus is the third most common site of fracture after the proximal femur and distal radius [2]. The level of dislocation and rate of occurrence rise exponentially with age and concomitant osteoporosis [1,2]. Furthermore, because additional comorbidities are common in older patients, the ultimate goals for them are early mobilization and fast rehabilitation back into home care [3].
In geriatric patients, osteosynthesis also is linked with a high complication rate [4], whereas nailing is not always an option [5]. Furthermore, internal fixation with a locking plate is associated with a complication rate of 30% and a 20% risk of revision [6]. One should always bear in mind that, for PHFs, conservative treatment has been proven to provide equivalent results, especially in elderly patients [7–11]. In addition to age, factors such as fracture type (4-part fractures), diabetes mellitus, smoking, female sex, and osteoporosis have been found, in other studies, to predict humeral head necrosis and malunion/non-union [12].
The current recommendations for severe dislocated PHF with 3 to 4 fragments are treatment primarily with implantation of an endoprosthesis or a reverse prosthesis, particularly in elderly patients [6]. In those cases, both anatomical prostheses and complete reverse prostheses can be utilized [13]. Guery et al [14] postulated a 10-year survival rate of 91% for total reverse shoulder prostheses. Early loosening of the prostheses tended to happen approximately 3 years postoperatively, whereas late-onset functional deterioration started approximately 3 years later. Guery recommended reverse prostheses for elderly patients. Favard et al [10] described a 10-year revision-free period in 89% of patients after a reverse prosthesis. Of his patients, 72% had a Constant-Murley (Constant) score >30% after 10 years. Radiographic changes and scapular notching were observed after 5 years, on average. Favard also concluded that reverse prostheses are best suited for geriatric patients.
Erdel et al [15] recently presented a broad review of the literature as well as his own patients, with a comparison of open reduction and plate fixation (ORPF), anatomic arthroplasty (AA), and reverse total arthroplasty (RTA). He included a surgical algorithm with which the decision among ORPF, AA, and RTA would be made according to age, severity of injury to the tubercula, and perspective regarding whether the head itself could be salvaged. Patient age, fracture complexity, and bone quality all play a role in the choice of surgery. Since 2014, guidelines from the German Society for Trauma and Orthopedic Surgery have recommended a primary endoprosthesis as the treatment of choice for complex fractures in patients with osteoporosis [16].
In the past years 2, reports have been published about a novel joint-preserving method [17,18]. This technique involves a locking plate fixation in combination with a lyophilized femoral head allograft for further stabilization. The favorable short-term results with this approach may encourage other orthopedic surgeons to use this technique for comminuted PHF. The goal of the present study is to inform the scientific community about the long-term outcome with it.
Material and Methods
STUDY DESIGN:
The present study was an observational report on a series of consecutive patients. Our assessments of outcomes after the novel procedure were retrospective and made without a control group.
PATIENT RECRUITMENT:
The patients in the present study had undergone surgery in our department for treatment of a comminuted proximal femoral fracture with the aforementioned technique between 2010 and 2016. We stopped performing the procedure after 2016 for 2 reasons. First, new guidelines issued in 2014 highly recommended a shoulder prosthesis in such cases. Second, long-term results with the previous surgeries needed to be evaluated. Therefore, use of the technique was reserved for comminuted fractures with a Neer classification of IV or higher, for which a substantial osseous defect was to be expected.
All of the surgeries represented in the present study were performed during the acute period, with a mean interval between trauma and the procedure of 5.2 days (range, 0–21). Patients who had experienced a minor trauma with a 2-part fracture or who had minimal dislocation were offered other surgical or conservative treatment. Likewise, children, young adults with healthy skeletons, and patients in whom surgery was contraindicated were not considered for the procedure. In 3 cases, a previous procedure had failed; in 2 of those cases, an intramedullary nail was initially placed. On postoperative days (PODs) 8 and 18, respectively, the nail broke. In both cases, there was late femoral head necrosis. In the third case, a plate fixation initially was performed but failed on POD 12. That patient had good bone healing. Gross preexisting arthritis also was an exclusion criterion.
All patients were operated on by the senior author. Data acquisition was performed by reviewing patient records, assessing previous X-rays, and performing interviews with standardized questionnaires and physical examinations. The present study was approved by the Institutional Review Board of the University of Erlangen, Germany. (Nr. 460_20 B).
SURGICAL TECHNIQUE:
The procedure was performed in the “beach chair” position with free access to the shoulder [19]. The C-arm fluoroscope was positioned after the patient had been draped. Access was gained through a deltopectoral approach in a plane between the 2 muscles, with care taken to spare the cephalic vein and the axillary and musculocutaneous nerves. The subacromial bursa was excised and the humeral head was exposed with a Langenbeck retractor. The major tubercle was sutured in the area of the insertion of the infraspinatus and supraspinatus muscles. The fragments of the humeral head were set in the former anatomic position. The central bone defect was estimated and the surgeon then chose an allograft (frozen lyophilized femoral head, German Institute for Cellular and Tissue Replacement, DIZG gGmbH, Berlin, Germany). Using an oscillating saw or Luer pliers, the allograft was shaped to fit in the bony defect. The shaft of the allograft was used to mortise into the femoral shaft and the convex (mushroom-like) component was used to fill the defect in the humeral head. The major and minor tubercle were closed over the graft and a proximal humerus interlocking plate (PHILOS plate, DePuy Synthes, Raynham, United States) was used for osteosynthesis. The position of the graft and the plate fixation were maintained under fluoroscopic guidance. Physical therapy was initiated on POD 2. Weight bearing began 6 weeks postoperatively.
RADIOGRAPHICAL EVALUATION:
X-rays and computed tomography (CT) scans were evaluated by a radiologist and the orthopedic surgeon who performed the surgery. The initial preoperative radiographic images were assessed according to the Neer classification [20]. Early postoperative radiographic images (1–6 m) were evaluated for reduction, implant position, and implant loosening as well as allograft position. A head-shaft angle <120 degrees was defined as “varus malreduction” [21]. The relationship between the varus malreduction and the Disabilities of the Arm, Shoulder and Hand (DASH) or Constant scores was evaluated and statistically assessed. Late radiographic follow-up images (6.5–81 m) were evaluated for complications including bone healing, secondary implant dislocation or loosening arthritis of the humeral head, necrosis of the humeral head, and integrity and position of the hardware. In addition, a possible relationship between Neer classification and humeral head necrosis was statistically evaluated. No additional radiographs or CT scans had to be performed for the present study.
PATIENT INTERVIEW AND PHYSICAL EXAMINATION:
All patients were contacted via mail or by telephone. Those who agreed to participate in the present study were sent a standardized form that included the quick DASH (qDASH) questionnaire and questions about average daily pain level, presented in terms of a visual analog scale (VAS) score. The questionnaires and evaluation scores were in German and have been validated for use with German patients. During the interviews, the questionnaire was reviewed and additional information was obtained about patient postoperative history, possible revision surgery, and adherence to physical therapy. The patients also underwent a physical examination to complete the criteria for the Constant score [22]. The above-mentioned interviews and physical examination were performed only once.
STATISTICAL ANALYSIS:
Descriptive statistical analysis was performed with Prism 8 statistical software (GraphPad, San Diego, California, United States). The results are presented as means with ranges and standard deviations (±). Linear regression was calculated by means of a Spearman non-parametric correlation because the sample was small; no normal distribution of score values was possible. Otherwise, a chi-square test was used, as described in the results section.
Correlation analysis was performed between the malreduction angle and the DASH and Constant scores. Further correlation analysis was performed between the Constant scores and the Neer classifications. A chi-square analysis was performed to evaluate the significance of the Neer classification for humeral head necrosis; however, because of the small sample, the statistical power of this analysis was limited.
Results
STUDY POPULATION AND INJURY CHARACTERISTICS:
Twenty-six patients were identified who had undergone the aforementioned procedure. Their average age was 69.8 years (range, 46–92±12.38). Ten patients (38%) were younger than age 65 years and 16 (62%) were older than age 65 years. We were able to interview 19 of the 26 patients (73%). No contact could be established with 2 of the patients and 3 had already died, 1 of whom had experienced cardiopulmonary failure 7 days after surgery. Two other patients declined to be interviewed because of very bad general health. In 66% of patients, their dominant side was affected. Two of 20 patients with Neer V fractures and 1 of 2 with Neer VI fractures had a head-split injury. The study population and injury characteristics are summarized in Table 1.
PERIOPERATIVE CONSIDERATIONS:
In 23 of the patients, surgery was performed as a primary procedure. In 3 cases, it was a revision after failure of a previous procedure. In 2 cases, intramedullary nailing initially was performed; the nail broke on PODs 8 and 18, respectively. In both cases, there was late femoral head necrosis. In the third case, a plate fixation initially was performed but failed on POD 12. That patient had good bone healing.
The mean time between injury and surgery was 5.42 days (range, 0–21±5.03). There were no intraoperative injuries to the axillary nerve nor any major blood loss requiring transfusion. Following surgery, 1 patient had a slight motoric deficit of the deltoid muscle with no loss of sensitivity. In 2 cases, because of an early plate cut, the plate fixation had to be performed anew and reinforced with cerclages. The allograft was left in situ. The results are summarized in Table 2.
FOLLOW-UP:
All patients underwent surgery between 2010 and 2016. The mean interval between surgery and late follow-up was 27.95 months (range, 6.5–81±19.11). A correlation between follow-up time and Constant score was excluded by means of simple linear regression (R2=0.037, F=0.6546,
PATIENT SATISFACTION AND VAS:
Asked whether they considered their surgery “very satisfactory,” “moderately satisfactory,” or “unsatisfactory,” 10 patients (52.6%) chose “very satisfactory,” 4 (21.1%) chose “moderately satisfactory,” and 5 patients (26.3%) chose “unsatisfactory” because of limitations in range of motion (ROM) and loading pain. In terms of VAS score for everyday activities, the mean score provided by patients was 2.73 (range, 0–6±2.02). Need for analgesics was indicated as “regularly” by 4 patients, “as required” by 4 patients, and “none required” by 11 patients.
DASH SCORE, CONSTANT SCORE, AND RANGE OF MOTION:
The mean DASH score was 52.85±21.4. The mean Constant score was 39.26±17.99. ROM for flexion was 68.50 degrees ±30 and abduction was 67.50 degrees ±26.73. A summary of the above results is shown in Table 3 and Figure 1. The population was divided into younger and older age groups (<65 years vs >65 years). There was no significant difference between the groups in terms of DASH (unpaired t test, P=0.450) or Constant scores (unpaired t test, P=0.916). The results are summarized in Table 3.
PERIOPERATIVE RADIOLOGIC EVALUATION:
All fractures were categorized according to their Neer classification by means of an X-ray and a CT scan. The latter was available for 23 of 26 patients but X-ray follow-up could only be performed in 25 patients because of 1 early postoperative death. A combination of early and late postoperative radiologic follow-up was obtained from 21 patients. There were 22 patients with early and 24 with late follow-up X-rays. All of the postoperative X-rays displayed anatomic reduction. In 1 patient, a glenoid screw had to be inserted, and in another, a coracoid screw fixation had to be performed. Three patients had previous underlying shoulder disease; in 2 cases, it was arthritis of the shoulder and in the third case, it was arthritis of the acromion surface. The defined varus malreduction angle was 132.1 degrees (range, 113–145±8.38). Only 1 patient was found with an angle <120 degrees and in another 2 X-rays, the angle was exactly 120 degrees. There was no significant correlation between varus malreduction angle and Constant score (Spearman correlation, r=−0.286, P=0.23) or between the varus malreduction angle and the DASH score (Spearman correlation, r=0.251, P=0.29). The results are summarized in Table 3 and Figure 2.
FOLLOW-UP RADIOLOGIC EVALUATION:
Radiologic results were satisfactory in 16 of 22 patients (73%) on early follow-up (0–6 m). In 5 patients (23%), there was evidence of perforation of screws into the joint. In 2 cases (9%), revision surgery was necessary due to secondary dislocation of the plate. In 3 patients (14%), the onset of humeral head necrosis was already evident. Finally, 1 patient had juxta-articular heterotopic calcifications.
On late follow-up (6.5–81 months), 15 of 24 patients (62.5%) had humeral head necrosis. Of them, 14 (93%) had experienced a Neer V or VI fracture. The risk for head necrosis was not age-related (comparison of patients aged <65 vs >65 years) (chi-square, P=0.231) but there was a significant tendency toward humeral head necrosis with increasing Neer classification (chi-square for trend 5.241, P=0.021). This effect is shown in Figure 3. Marked arthritis of the glenohumeral joint was evident in 14 of 24 patients (58%). In 5 patients, there was screw penetration into the shoulder joint, whereas 10 patients already had the hardware removed. Heterotopic calcification was evident in 1 patient.
Average Constant scores were 49 in the Neer IV group, 38 in the Neer V group, and 32 in the Neer VI group. Because the sample was small, there was no significant correlation between Neer classification and Constant score (Spearman r=−0.1113, P=0.65). The effect is demonstrated in Figure 4.
Discussion
CASE PRESENTATION:
A 56-year-old man (Patient 21) suffered an occupational accident when he fell from a height of approximately 2 meters. He landed on his right shoulder and sustained multiple injuries, including a head-split fracture of the proximal humerus classified as a Neer V fracture of 4 fragments as well as an avulsion of the coracoid process (Figures 5, 6). Underlying diseases included obesity and arterial hypertension.
The patient underwent surgery 4 days later with the aforementioned technique using a femur allograft and locking plate (Figure 7). The initial reduction was satisfactory, with a varus malreduction angle of 130 degrees (Figure 8). The surgery took 142 min.
The allograft was sculpted into a mushroom form by means of a bone rongeur and a saw blade. The “stalk” of the form was intended to be a perfect match to the shaft hollow, whereas the transition point to the cap “sat” on the fragment of the humeral shaft. Care was taken not to tailor too big of a cap so that the tuberculae could be reduced anatomically and sufficiently adapted with the PHILOS plate. After the allograft was inserted, an elevator instrument was used to cover the allograft with the humeral head dome. The end of the plate was congruent with the cranial end of the major tubercule.
The patient was discharged 2 days after surgery. He was allowed to engage in passive motion after week 4 and active motion after week 5. He returned 10 months after surgery with a complaint of persistent shoulder pain. Secondary perforation of the screws and the beginning of a humeral head necrosis could be seen (Figure 9).
After hardware removal, the patient continued to have pain due to humeral head necrosis. At 18 months’ follow-up, he had a DASH score of 56.7 and a Constant score of 45. At 18 months after the initial surgery, conversion to a hemiprosthesis was performed (Figure 10).
Conclusions
Recent guidelines for surgical treatment of PHF in the elderly recommend use of a reverse prosthesis as a primary technique for severe comminuted and/or head-split fractures. In the present study, an alternative joint-conserving operation that includes anatomical open reduction and reinforcement of the locking plate fixation with a bone allograft was retrospectively assessed. Despite encouraging short-term results with the technique, in the long run, the concept fell short of our expectations for a better outcome than conservative therapy. The decisive point was the development of humeral head necrosis in most of our patients.
With this insight, we recommend the use of a reverse prosthesis in the setting of comminuted fractures in the elderly.
Figures
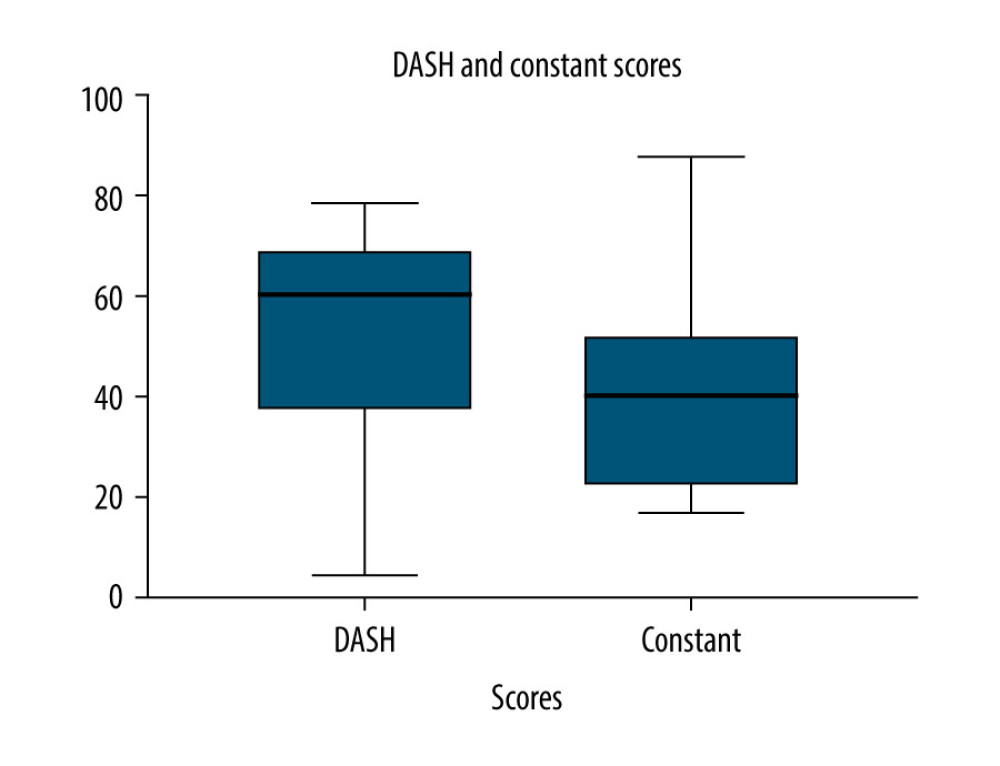 Figure 1. Distribution of Disabilities of the Arm, Shoulder and Hand and Constant-Murley scores displayed as a whisker plot.
Figure 1. Distribution of Disabilities of the Arm, Shoulder and Hand and Constant-Murley scores displayed as a whisker plot. 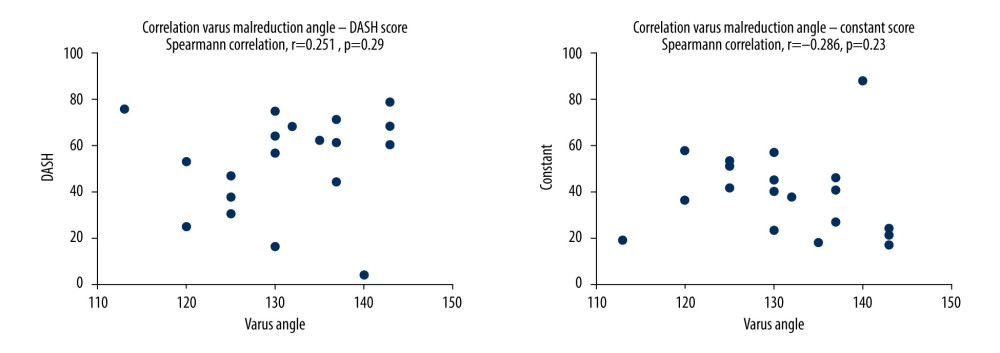 Figure 2. No statistically significant correlation was found between the angle of varus malreduction and the Constant or Distribution of Disabilities of the Arm, Shoulder and Hand scores.
Figure 2. No statistically significant correlation was found between the angle of varus malreduction and the Constant or Distribution of Disabilities of the Arm, Shoulder and Hand scores. 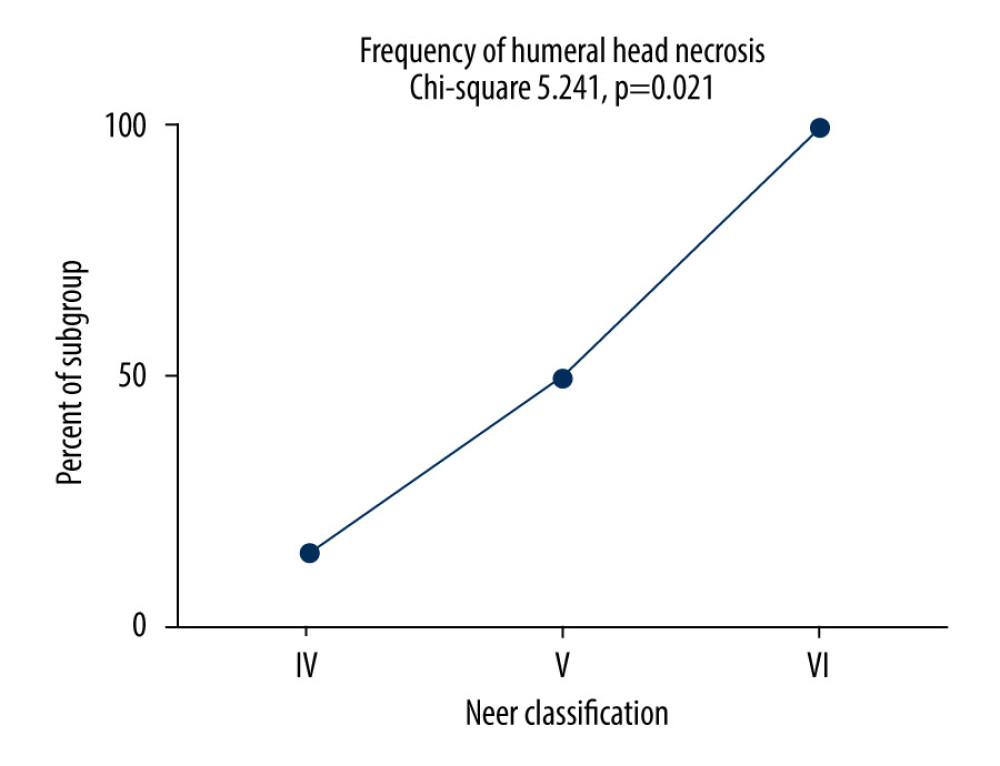 Figure 3. As the Neer classification increased, there was a significant increase in the risk of humeral head necrosis.
Figure 3. As the Neer classification increased, there was a significant increase in the risk of humeral head necrosis. 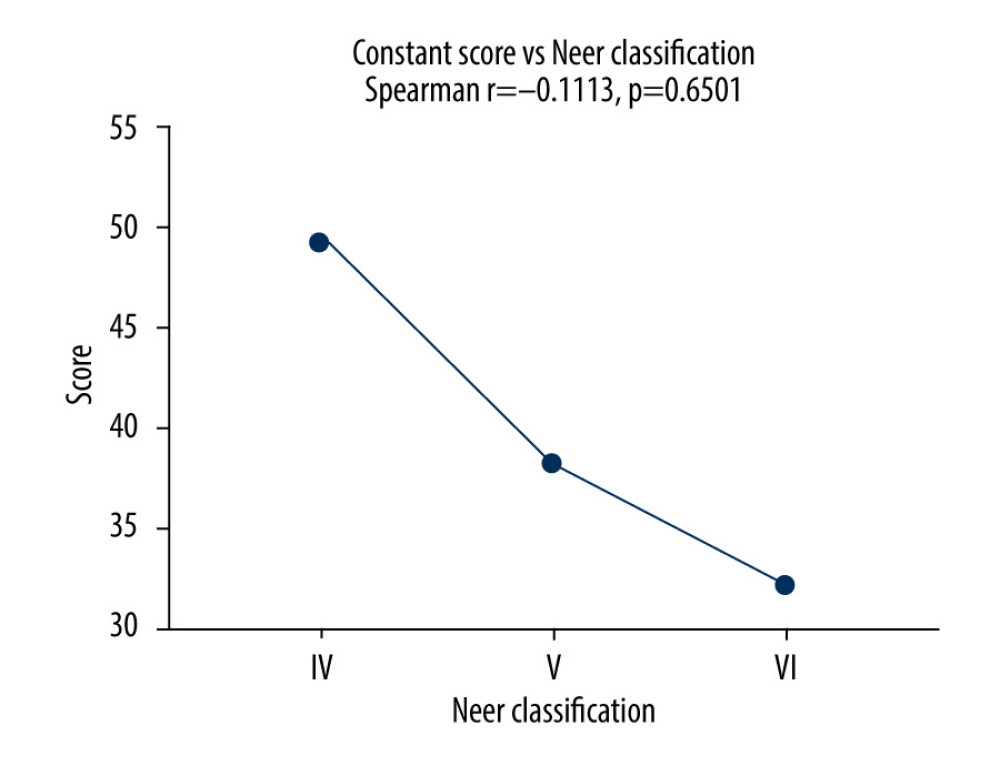 Figure 4. As the Neer classification increased, the Constant-Murley score decreased, but the effect did not reach statistical significance.
Figure 4. As the Neer classification increased, the Constant-Murley score decreased, but the effect did not reach statistical significance. 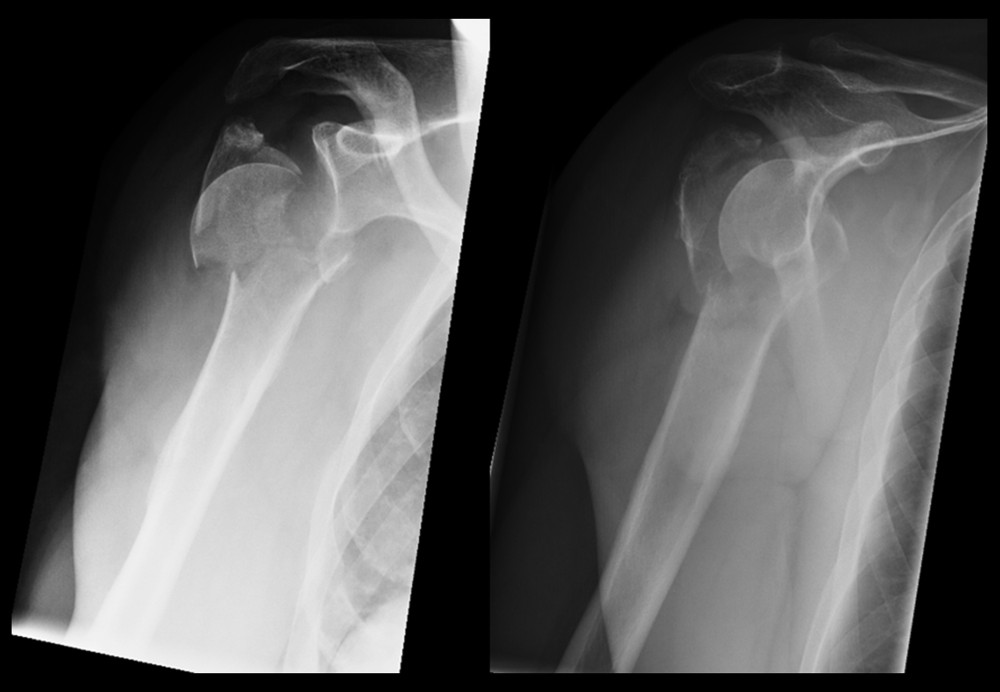 Figure 5. A 56-year-old patient with an avulsion of the coracoid process and a comminuted proximal humeral fracture (Neer V).
Figure 5. A 56-year-old patient with an avulsion of the coracoid process and a comminuted proximal humeral fracture (Neer V). 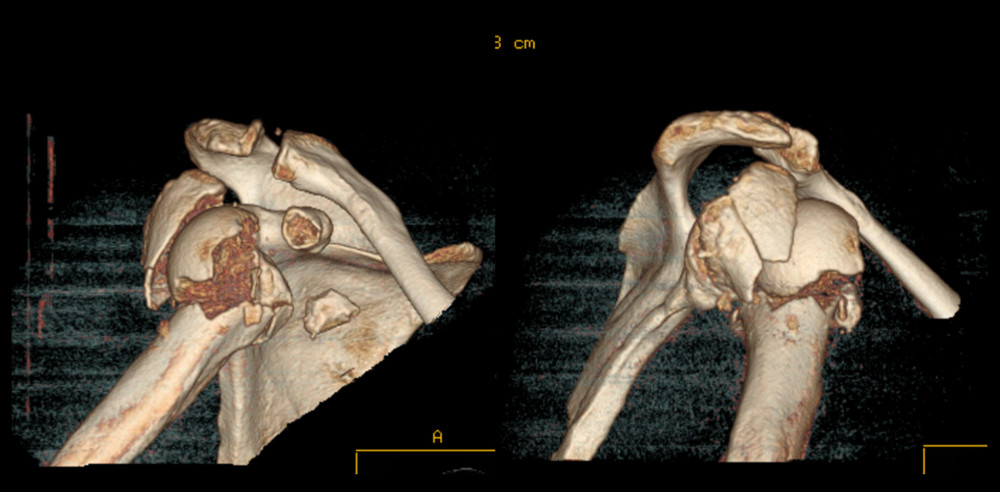 Figure 6. A 3-dimensional preoperative reconstruction in the same patient.
Figure 6. A 3-dimensional preoperative reconstruction in the same patient. 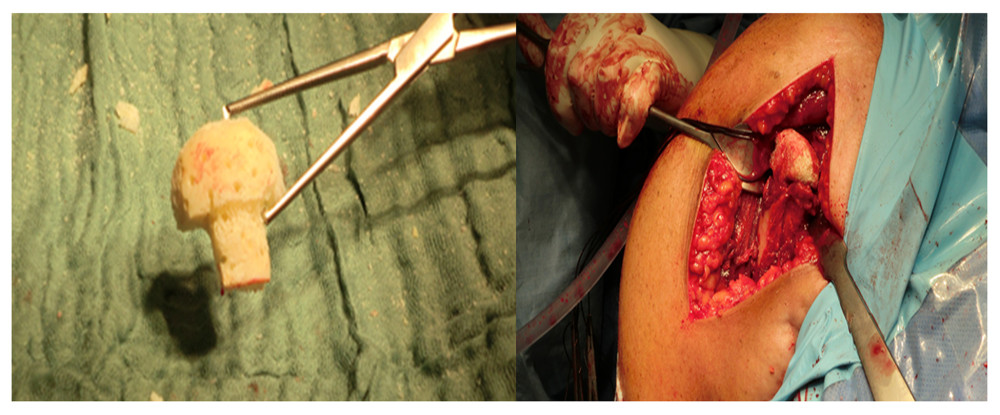 Figure 7. Trimming and inset of the lyophilized femoral bone allograft.
Figure 7. Trimming and inset of the lyophilized femoral bone allograft. 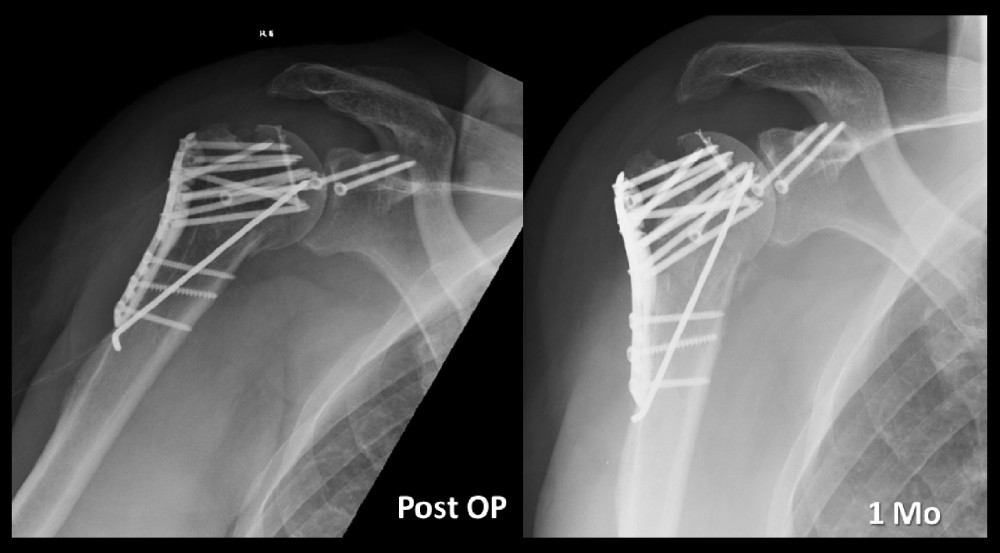 Figure 8. Early postoperative X-rays demonstrating a satisfactory reduction.
Figure 8. Early postoperative X-rays demonstrating a satisfactory reduction. 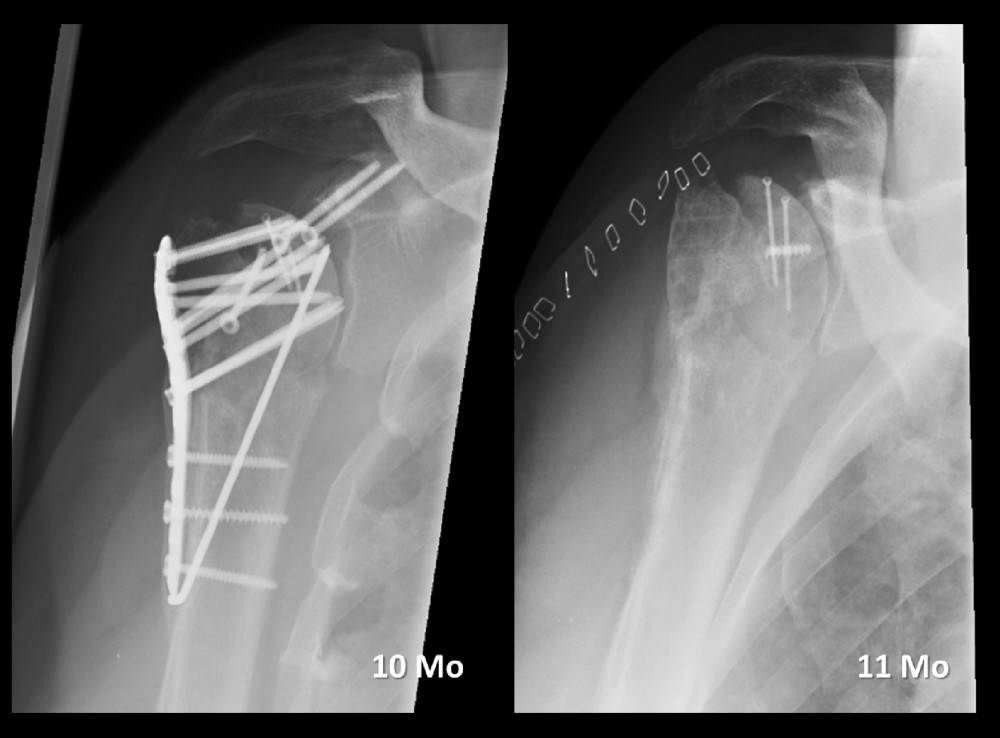 Figure 9. Because of screw perforation, the hardware had to be removed at 11 months.
Figure 9. Because of screw perforation, the hardware had to be removed at 11 months. 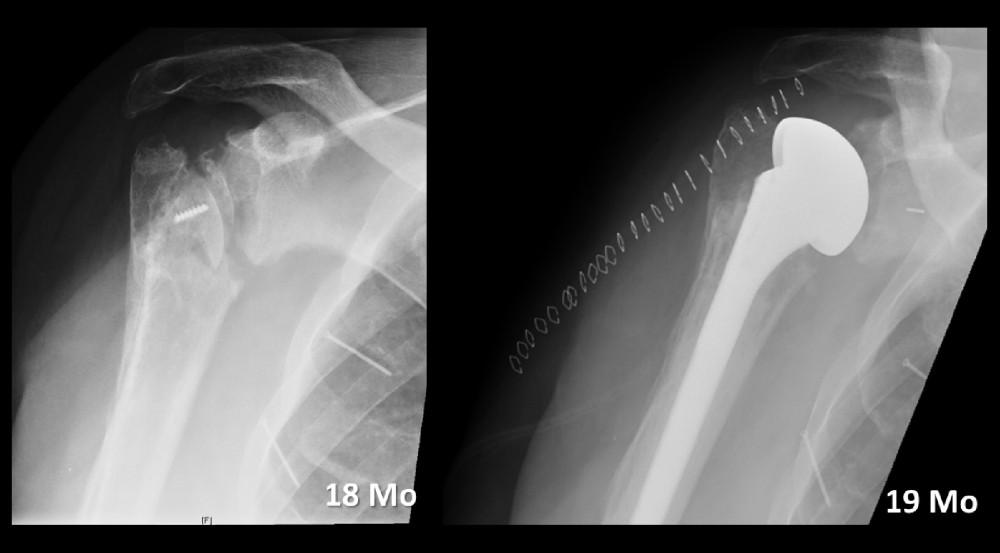 Figure 10. Necrosis of the humeral head necrosis was found at the 18-month follow-up. The patient underwent hemiprosthesis surgery.
Figure 10. Necrosis of the humeral head necrosis was found at the 18-month follow-up. The patient underwent hemiprosthesis surgery. References
1. Court-Brown CM, Garg A, McQueen MM, The epidemiology of proximal humeral fractures: Acta Orthop Scand, 2001; 72(4); 365-71
2. Hirzinger C, Tauber M, Resch HProximal humerus fracture: New aspects in epidemiology, fracture morphology, and diagnostics: Unfallchirurg, 2011; 114(12); 1051-58 [in German]
3. Kutscha-Lissberg F, Kollig E, Keller MFracture management in the aged: Orthopade, 2000; 29(4); 274-80 [in German]
4. Vester H, Huber-Lang MS, Kida Q, The immune response after fracture trauma is different in old compared to young patients: Immun Ageing, 2014; 11(1); 20
5. Laux CJ, Grubhofer F, Werner CML, Current concepts in locking plate fixation of proximal humerus fractures: J Orthop Surg Res, 2017; 12(1); 137
6. Schnetzke M, Bockmeyer J, Porschke F, Quality of reduction influences outcome after locked-plate fixation of proximal humeral type-C fractures: J Bone Joint Surg Am, 2016; 98(21); 1777-85
7. Krettek C, Wiebking UProximal humerus fracture: Is fixed-angle plate osteosynthesis superior to conservative treatment?: Unfallchirurg, 2011; 114(12); 1059-67 [in German]
8. Fjalestad T, Stromsoe K, Blucher J, Fractures in the proximal humerus: Functional outcome and evaluation of 70 patients treated in hospital: Arch Orthop Trauma Surg, 2005; 125(5); 310-16
9. Ek ET, Neukom L, Catanzaro S, Gerber C, Reverse total shoulder arthroplasty for massive irreparable rotator cuff tears in patients younger than 65 years old: Results after five to fifteen years: J Shoulder Elbow Surg, 2013; 22(9); 1199-208
10. Favard L, Levigne C, Nerot C, Reverse prostheses in arthropathies with cuff tear: are survivorship and function maintained over time?: Clin Orthop Relat Res, 2011; 469(9); 2469-75
11. Spross C, Meester J, Mazzucchelli RA, Evidence-based algorithm to treat patients with proximal humerus fractures – a prospective study with early clinical and overall performance results: J Shoulder Elbow Surg, 2019; 28(6); 1022-32
12. Boesmueller S, Wech M, Gregori M, Risk factors for humeral head necrosis and non-union after plating in proximal humeral fractures: Injury, 2016; 47(2); 350-55
13. Ockert B, Biermann N, Haasters FReverse shoulder arthroplasty for primary fracture treatment Displaced three and four part fractures of the proximal humerus in the elderly patient: Unfallchirurg, 2013; 116(8); 684-90 [in German]
14. Guery J, Favard L, Sirveaux F, Reverse total shoulder arthroplasty. Survivorship analysis of eighty replacements followed for five to ten years: J Bone Joint Surg Am, 2006; 88(8); 1742-47
15. Erdle B, Izadpanah K, Eberbach HPrimary fracture protheses and reverse shoulder arthroplasty in complex humeral head fractures: An alternative to joint-preserving osteosynthesis?: Orthopade, 2018; 47(5); 410-19 [in German]
16. Frosch KH, Kammerlander C, Helfen T, S1 Guidelines: Humeral head fractures [Oberarmkopffraktur]: AWMF, 2017 10/20172017
17. Euler SA, Hengg C, Wambacher M, Allogenic bone grafting for augmentation in two-part proximal humeral fracture fixation in a high-risk patient population: Arch Orthop Trauma Surg, 2015; 135(1); 79-87
18. López CRE, Krappinger D, Riedl M, Femoral head augmentation in 3–4 part proximal humerus fractures plating in elderly population and it’s failure predictors: Ortho-tips, 2019; 15(2); 121-29
19. Skyhar MJ, Altchek DW, Warren RF, Shoulder arthroscopy with the patient in the beach-chair position: Arthroscopy, 1988; 4(4); 256-59
20. Neer CS, Displaced proximal humeral fractures. I. Classification and evaluation: J Bone Joint Surg Am, 1970; 52(6); 1077-89
21. Agudelo J, Schurmann M, Stahel P, Analysis of efficacy and failure in proximal humerus fractures treated with locking plates: J Orthop Trauma, 2007; 21(10); 676-81
22. Constant CR, Murley AH, A clinical method of functional assessment of the shoulder: Clin Orthop Relat Res, 1987(214); 160-64
23. Katthagen JC, Huber M, Grabowski S, Failure and revision rates of proximal humeral fracture treatment with the use of a standardized treatment algorithm at a level-1 trauma center: J Orthop Traumatol, 2017; 18(3); 265-74
24. Maier D, Jaeger M, Izadpanah K, Proximal humeral fracture treatment in adults: J Bone Joint Surg Am, 2014; 96(3); 251-61
25. Hsiao CK, Tsai YJ, Yen CY, Intramedullary cortical bone strut improves the cyclic stability of osteoporotic proximal humeral fractures: BMC Musculoskelet Disord, 2017; 18(1); 64
26. Gardner MJ, Boraiah S, Helfet DL, Indirect medial reduction and strut support of proximal humerus fractures using an endosteal implant: J Orthop Trauma, 2008; 22(3); 195-200
27. Saltzman BM, Erickson BJ, Harris JD, Fibular strut graft augmentation for open reduction and internal fixation of proximal humerus fractures: A systematic review and the authors’ preferred surgical technique: Orthop J Sports Med, 2016; 4(7) 2325967116656829
28. Kruithof RN, Formijne Jonkers HA, van der Ven DJC, Functional and quality of life outcome after non-operatively managed proximal humeral fractures: J Orthop Traumatol, 2017; 18(4); 423-30
29. Chen L, Xing F, Xiang Z, Effectiveness and safety of interventions for treating adults with displaced proximal humeral fracture: A network meta-analysis and systematic review: PLoS One, 2016; 11(11); e0166801
30. Bois AJ, Knight P, Alhojailan K, Clinical outcomes and complications of reverse shoulder arthroplasty used for failed prior shoulder surgery: A systematic review and meta-analysis: JSES Int, 2020; 4(1); 156-68
31. Chelli M, Lo Cunsolo L, Gauci MO, Reverse shoulder arthroplasty in patients aged 65 years or younger: A systematic review of the literature: JSES Open Access, 2019; 3(3); 162-67
32. Tauber M, Resch H, Frakturbiologie und -morphologie: Die proximale Humerusfraktur, 2014, Berlin, Heidelberg, Springer \in German]
33. Thua T, Pham D, Lê K, Tissue engineering using mesenchymal stem cell with periosteal wrap for bone defect repair in rabbits: Plast Aesthet Res, 2015; 2; 340-45
34. Kneser U, Schaefer DJ, Polykandriotis E, Tissue engineering of bone: The reconstructive surgeon’s point of view: J Cell Mol Med, 2006; 10(1); 7-19
35. Hettrich CM, Boraiah S, Dyke JP, Quantitative assessment of the vascularity of the proximal part of the humerus: J Bone Joint Surg Am, 2010; 92(4); 943-48
36. Gerber C, Schneeberger AG, Vinh TS, The arterial vascularization of the humeral head. An anatomical study: J Bone Joint Surg Am, 1990; 72(10); 1486-94
37. Brooks CH, Revell WJ, Heatley FW, Vascularity of the humeral head after proximal humeral fractures. An anatomical cadaver study: J Bone Joint Surg Br, 1993; 75(1); 132-36
38. Claes L, Eckert-Hubner K, Augat P, The fracture gap size influences the local vascularization and tissue differentiation in callus healing: Langenbecks Arch Surg, 2003; 388(5); 316-22
Figures
 Figure 1. Distribution of Disabilities of the Arm, Shoulder and Hand and Constant-Murley scores displayed as a whisker plot.
Figure 1. Distribution of Disabilities of the Arm, Shoulder and Hand and Constant-Murley scores displayed as a whisker plot. Figure 2. No statistically significant correlation was found between the angle of varus malreduction and the Constant or Distribution of Disabilities of the Arm, Shoulder and Hand scores.
Figure 2. No statistically significant correlation was found between the angle of varus malreduction and the Constant or Distribution of Disabilities of the Arm, Shoulder and Hand scores. Figure 3. As the Neer classification increased, there was a significant increase in the risk of humeral head necrosis.
Figure 3. As the Neer classification increased, there was a significant increase in the risk of humeral head necrosis. Figure 4. As the Neer classification increased, the Constant-Murley score decreased, but the effect did not reach statistical significance.
Figure 4. As the Neer classification increased, the Constant-Murley score decreased, but the effect did not reach statistical significance. Figure 5. A 56-year-old patient with an avulsion of the coracoid process and a comminuted proximal humeral fracture (Neer V).
Figure 5. A 56-year-old patient with an avulsion of the coracoid process and a comminuted proximal humeral fracture (Neer V). Figure 6. A 3-dimensional preoperative reconstruction in the same patient.
Figure 6. A 3-dimensional preoperative reconstruction in the same patient. Figure 7. Trimming and inset of the lyophilized femoral bone allograft.
Figure 7. Trimming and inset of the lyophilized femoral bone allograft. Figure 8. Early postoperative X-rays demonstrating a satisfactory reduction.
Figure 8. Early postoperative X-rays demonstrating a satisfactory reduction. Figure 9. Because of screw perforation, the hardware had to be removed at 11 months.
Figure 9. Because of screw perforation, the hardware had to be removed at 11 months. Figure 10. Necrosis of the humeral head necrosis was found at the 18-month follow-up. The patient underwent hemiprosthesis surgery.
Figure 10. Necrosis of the humeral head necrosis was found at the 18-month follow-up. The patient underwent hemiprosthesis surgery. Tables
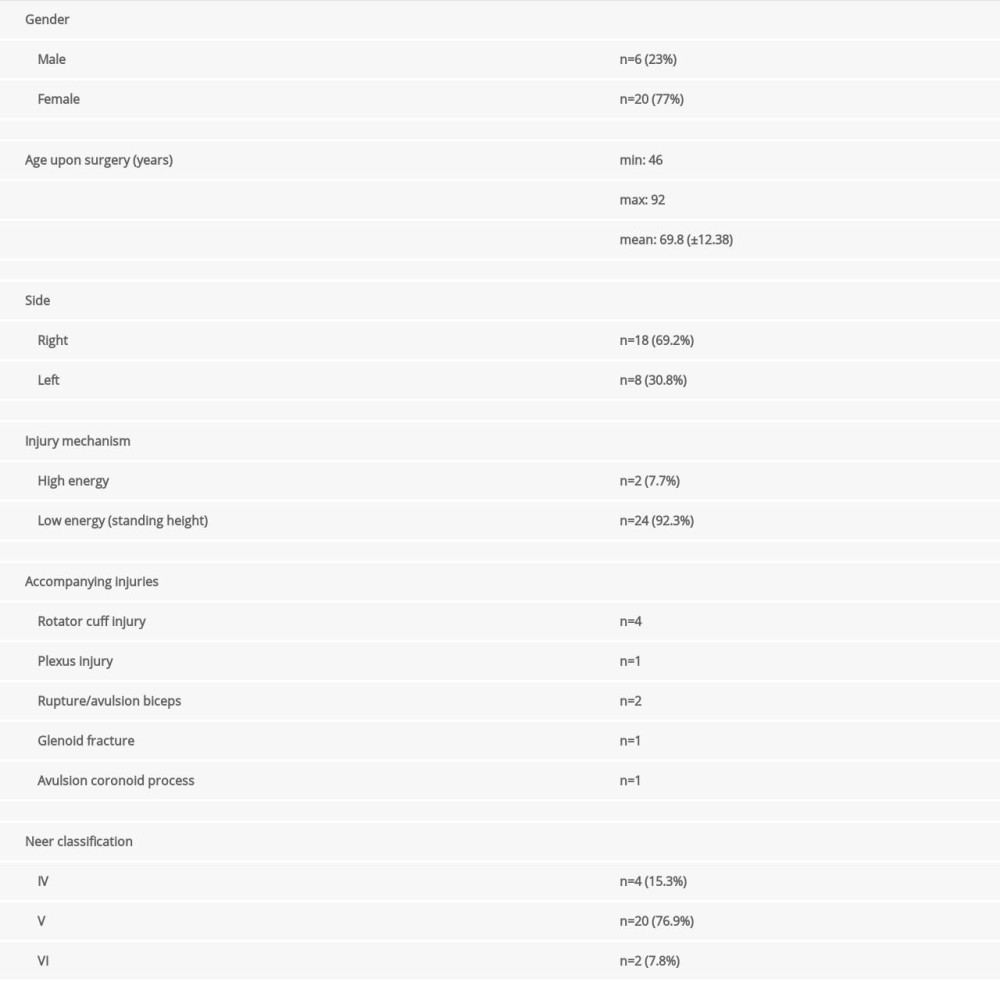 Table 1. Characteristics of the study population and their injuries.
Table 1. Characteristics of the study population and their injuries.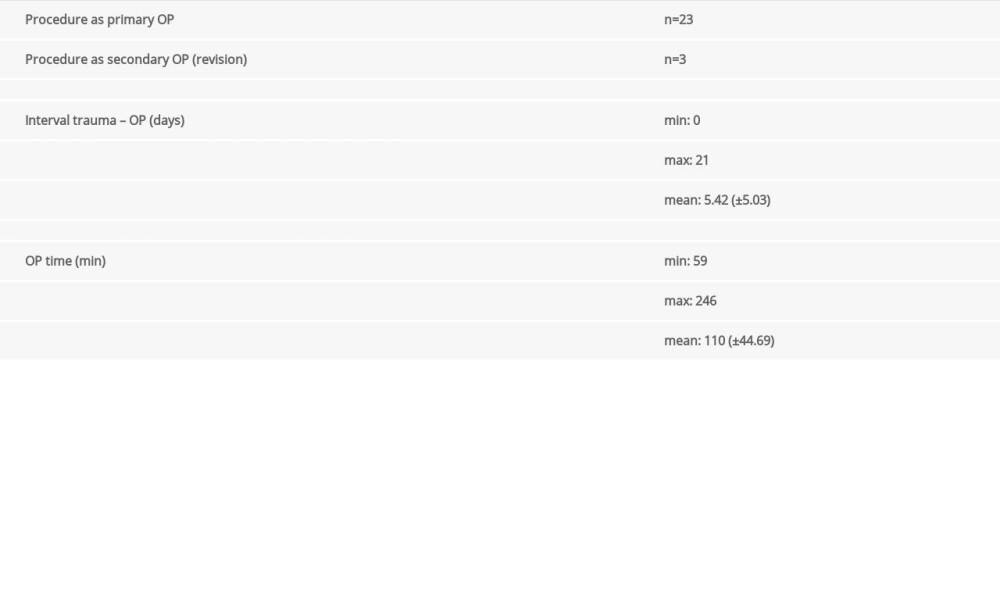 Table 2. Summary of perioperative considerations.
Table 2. Summary of perioperative considerations.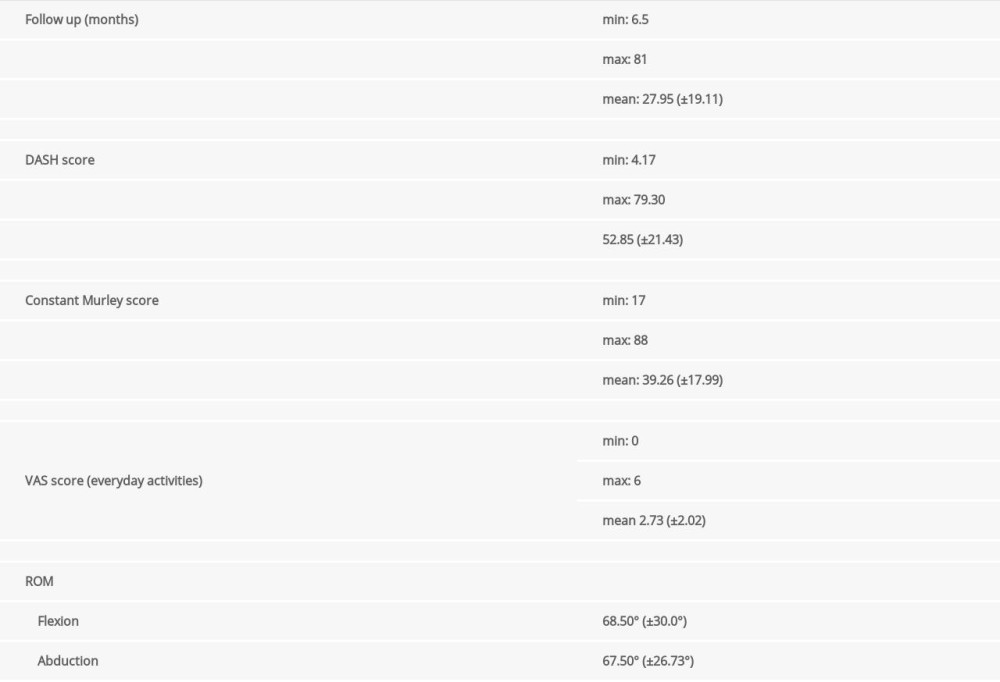 Table 3. Summary data from patient physical examinations.
Table 3. Summary data from patient physical examinations. Table 1. Characteristics of the study population and their injuries.
Table 1. Characteristics of the study population and their injuries. Table 2. Summary of perioperative considerations.
Table 2. Summary of perioperative considerations. Table 3. Summary data from patient physical examinations.
Table 3. Summary data from patient physical examinations. In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








