10 February 2021: Clinical Research
Comparison of Pregnancy Outcomes Between Single-Morula Embryo Transfer and Single-Blastocyst Transfer in Fresh IVF/ICSI Cycles
Hui-na Zhang1ABCDEFG, Ying-fen Ying1ABC, Hai-tao Xi1ABCD, Xiao-sheng Lu1ABCD, Jun-zhao Zhao1ACD*, Yi-lu Chen1ABCDEFGDOI: 10.12659/MSM.928737
Med Sci Monit 2021; 27:e928737
Abstract
BACKGROUND: This study investigated the effectiveness and feasibility of day 4 (D4) morula embryo transfer (ET) in comparison with day 5 (D5) blastocyst ET, with regards to their clinical data, laboratory test results, and pregnancy outcomes.
MATERIAL AND METHODS: This retrospective cohort study enrolled 1070 patients, including 178 cases in group D4 and 892 cases in group D5. The endpoint was live birth rate after fresh embryo transfer. Furthermore, the clinical outcomes of D4 embryos with different morphology were compared and assigned to 3 groups: in group 1 (n=66) the embryos were compacted but not expanded, in group 2 (n=102) the embryos were compacted and expanded (early blastocyst), and in group 3 (n=10) the embryos were not compacted.
RESULTS: Groups D4 and D5 had comparable clinical pregnancy rates (53.37% vs. 59.97%) and live birth rates (43.25% vs 50.89%), and there were no significant differences between the 2 groups. In group 3, there was only 1 clinical pregnancy and no live birth. In comparison between group 1 and group 2, the clinical pregnancy rate of group 2 showed an upward trend (48.48% vs 60.78%), but there was no significant difference. There was also no statistically significant difference in the live birth rate between the 2 groups (42.42% vs 49.01%).
CONCLUSIONS: Transferring of compacted embryos or early blastocysts can result in high clinical pregnancy rates and live birth rates. In addition to the cleavage and blastocyst ET, morula ET may serve as an alternative option for the clinician.
Keywords: Blastocyst, Live Birth, Morula, Embryo Transfer, Feasibility Studies, Infertility, Female, Pregnancy, Pregnancy Rate, Sperm Injections, Intracytoplasmic
Background
At present, cleavage-stage embryo transfer (ET) and blastocyst stage ET are commonly applied in many reproductive centers during fresh IVF/ICSI (in vitro fertilization/intracytoplasmic sperm injection) cycles. However, day 4 (D4) ET or single-morula embryo transfer (SMET) is often neglected. Previous studies have suggested that day 5 (D5) ET has a higher clinical pregnancy rate compared to day 3 (D3) ET. Elective single-blastocyst embryo transfer (SBET) can effectively lower the rate of multiple pregnancies, thereby reducing the risk of obstetric and neonatal complications [1,2]. However, contradictory findings have been reported. A recent study has demonstrated that fresh blastocysts offer no obvious advantage compared to cleavage-stage embryo transfer in women under 39 years old in terms of implantation and pregnancy rate [3], but the study involved transferring 2 cleavage embryos or blastocysts. According to both the National Institute for Health and Clinical Excellence (NICE) 2013 fertility guidelines and the Practice Committees of the American Society for Reproductive Medicine, the extended embryo culture into blastocyst stage during IVF/ICSI cycles can reduce the number of embryos that can be frozen, and there is a small increased the risk of adverse neonatal outcomes, but there is not enough evidence to prove a causal relationship [4,5].
Although the embryo culture system is constantly improving, it is different from the environment in the human body. There are potential increased risks of developmental arrest and reduced embryo quality after prolonged culture in vitro [6]. Hence, the balance between the risks and pregnancy rate remains a necessity. In addition, D5 ET is not always feasible for those clinics that are operate only on weekdays. Therefore, this study aimed to compare the clinical pregnancy and live birth rates between D4 and D5 ET, and the findings may provide evidence for the selection of D4 ET.
Material and Methods
STUDY OBJECTS:
This retrospective cohort study was conducted at the Reproductive Center of the Second Affiliated Hospital of Wenzhou Medical University. Female infertile patients who received single-morula embryo transfer (SMET) were selected, total of 178 cases from January 1, 2016 to August 31, 2019. There were a total of 892 cases of D5 transfer during January 1 2018 to December 31,2018.
OVARIAN STIMULATION PROTOCOL:
All patients received a long-term protocol of pituitary down-regulation with gonadotrophin-releasing hormone (GnRH) agonist for controlled ovarian hyper-stimulation (COH). Firstly, the patients were treated with 3.75 mg of GnRH agonist on the 2nd to 4th day of menstruation, and luteal-phase ovarian stimulation was initiated 30 to 40 days later. The stimulation was adjusted according to the size of antral follicles and the serum levels of follicle stimulating hormone (FSH), luteinizing hormone (LH), estradiol (E2), and progesterone (P). In addition, gonadotropins (Gn), such as recombinant FSH and human menopausal gonadotropins (hMG), were used for COH. The starting dose of Gn ranged from 75 to 300 IU, depending on patient age and ovarian function, as well as their responses to previous ovarian stimulation. Gn doses were based on the growth of ovarian follicles. When at least 2 follicles had a mean diameter of 18 mm, the final oocyte maturation was triggered by 4000 to 10 000 IU of human chorionic gonadotropin (hCG). Lastly, transvaginal ovum retrieval was carried out 34 to 36 hours after hCG administration. Fertilization was observed 20 hours after insemination based on the appearance of 2PN. The embryos were cultured in G-1 and G-2 medium (Vitrolife Co., Ltd., Australia) at 37°C, under 6% CO2, 5% O2, and 89% N2.
EMBRYO GRADING:
Grading of D4 embryos was conducted according to the 2011 ESHRE Istanbul Consensus and Ryh-sheng Li’s system for day 4 embryos [7,8]. On day 5, blastocyst stage embryo grading was conducted according to Gardner’s embryo grading system [9], by taking into account of the degree of expansion and the development of inner cell mass and trophectoderm. Based on this grading system, the ideal embryos were categorized into 3AA, 4AA, 5AA, 3AB/BA, 4AB/BA, and 5AB/BA. Meanwhile, cleavage-stage embryo grading was carried out by referring to the 2011 ESHRE Istanbul Consensus for D3 embryo [7], which involved the amount of cell fragmentation (%), cell multi-nucleation, cell symmetry, vacuoles, and zona pellucida. Based on this grading system, the optimal embryos were categorized into 7A, 8A, 9A, 7B, 8B, and 9B.
EMBRYO TRANSFER AND LUTEAL PHASE SUPPORT:
Embryo transfer (ET) was performed under the guidance of transabdominal ultrasound. The starting time of luteal phase support depended on serum P level on the day of hCG trigger. When P<1.2 ng/ml, luteal support was initiated 1 day after oocyte retrieval. When Pg≥1.2 ng/ml, luteal support was initiated 2 days after ovulation. If Pg≥1.5 ng/ml, ET was canceled. Crinone gel and dydrogesterone tablets were used for luteal phase support until day 13–14 after ET. Luteal support was continued until week 10–12 of pregnancy.
OUTCOME MEASUREMENT:
The primary endpoint of this study was the live birth rate, while the secondary endpoints were clinical pregnancy rate, early spontaneous abortion rate, ectopic pregnancy rate, multiplets pregnancy rate, preterm delivery rate, and neonate weight.
We defined the pregnancy outcomes in this study according to “CSRM consensus on key indicators for quality control in ART clinical operation” [10].
STATISTICAL ANALYSIS:
Statistical analysis was performed using SPSS software version 23.0 (IBM Corp, Armonk, NY, USA). The
Results
PREGNANCY OUTCOMES BETWEEN D4 AND D5 GROUPS:
As shown in Table 3, the D4 group and D5 group had similar clinical pregnancy rates (53.37% vs 59.97%, P>0.05), early spontaneous abortion rate (16.84% vs 10.6%), live birth rate (43.25% vs 50.89%), ectopic pregnancy rate (2.10% vs 0.74%), monozygotic twins rate (2.1% vs 0.74%), preterm delivery rate (5.19% vs 7.26%), and neonate weight (3258.68±577.23 vs 3207.27±470.95). There was no statistically significant difference between the 2 groups (P>0.05).
Among the 178 patients in the D4 group, there were 10 cases without compaction, including 1 case of clinical pregnancy but early abortion. There were 66 patients with compaction but without expanding (group 1), and 102 cycles with early blastocyst formation (group 2). The clinical data and pregnancy outcomes of the 2 groups were compared. Patient characteristics and laboratory data between group 1 and group 2 are summarized in Tables 4 and 5. There were no statistically significant differences in age, infertility duration, basic FSH, AFC, days of Gn, doses of Gn, E2 on trigger day, number of retrieved oocytes, number of MII oocytes, number of fertilized oocytes, number of D3, or number of D3 optimal embryos, between the 2 groups (P>0.05). However, there were significantly fewer frozen high-quality blastocysts and total frozen blastocysts in group 1 than in group 2.
PREGNANCY OUTCOMES IN GROUP 1 AND GROUP 2:
The clinical pregnancy rate of group 2 was higher than in group 1 (48.48% vs 60.78%, P>0 0.05), but the difference was not statistically significant, nor was there any statistically significant difference in the live birth rate (42.42% vs 49.01%, P>0.05), as shown in Table 6.
Discussion
The findings of many studies indicated that blastocyst ET had a higher clinical pregnancy rate compared to cleavage ET [11,12]. This is probably because the blastocyst transfer can improve synchronization between the endometrium and embryo, and due to the reduced proportion of chromosomal abnormalities in blastocysts, which increased the selection of suitable embryos for transfer [13,14]. However, several studies have shown that the cumulative pregnancy rate of blastocyst transplantation is not significantly different from or is even lower than that of cleavage embryos [15,16]. A recent meta-analysis also concluded that D5 transfer is not superior to D3 transfer, although the current evidence is low-quality or moderate-quality [17]. In addition, it has been reported that the blastocyst formation rate of D3 optimal embryos is approximately 30% to 50% [18,19]. Although this proportion is increasing with the development of embryo culture technology, the blastocyst formation rate of D3 optimal embryos in our study was more than 50%. If all patients receive blastocyst culture, the total number of transplantable embryos will inevitably decrease, and there may even be no embryos for transfer. In this study, 44 cases in the D4 group had no blastocysts frozen (including D5 and D6) after D4 transfer; 11 of them had no high-quality D3 embryos. Of the 11 cases, 4 had clinical pregnancy, and 3 had live births. Therefore, compared with D5 transfer, D4 transfer appears to have higher embryo utilization but similar clinical pregnancy rate and live birth rate. However, this study did not compare the embryo transfer cycle cancelation rate between the 2 groups because it was only a retrospective study. Because the patients who cancel the transfer due to embryo problems on D4 may have to cancel the transfer again on D5 because no cultured embryos are available then, we need to design a stricter RCT to compare the embryo transfer cycle cancelation rate between the 2 groups. Meanwhile, we would study more about the blastocyst formation rates of different grades of embryos in D4. In this study, it was also found that the basic conditions of the D4 and D5 groups were different, whether from age or number of retrieved oocytes, D3 number of embryos, D3 number of total embryos, D3 number of high-quality blastocysts, and total blastocysts. The D5 group was superior to the D4 group. It may be related to our transfer strategy. If there are few retrieved oocytes, or if the embryo compaction was not good on D4, we ask the patient’s opinion about whether to transfer. The other cycles of day 4 transfer were mainly because of organizational reasons; for example, when day 5 was a Sunday or public holiday.
Clinical pregnancy rates and live birth rates were similar to those in the D5 group, even though the age and embryo conditions of patients in the D4 group were not as good as in the D5 group. This is consistent with previous studies [20–22]. Therefore, it is suggested that blastocyst transfer can increase the pregnancy rate in each ET cycle, but limit the number of viable embryos transferred. D4 has a higher transfer rate than D5, and has a comparable clinical pregnancy rate and live birth rate. Additionally, prolonged culture in vitro may be detrimental to embryos. Research has shown that the risk of preterm birth and congenital anomalies may be higher in blastocyst transfer than in cleavage transfer [23]. In this study, the D4 prematurity rate was 5.19% and the D5 rate was 7.26%, and there was no significant difference between the 2 groups. Other potential risks of D5 ET have been reported previously, such as the higher risk of monozygous twins, large for gestational age babies, altered sex ratio, and higher birthweight [24–27], but the mechanism needs to be further studied. There are only animal experiments that shows differences in the expression of several genes, particularly of imprinted genes involved in apoptosis, oxidative stress, and gap junction formation in prolonged cultured embryos [28]. In our study there was no significant difference in the rate of monozygotic twins or birth weight between the 2 groups, but our sample size was small.
Compared to cleavage-stage ET, morula-stage ET had the same or higher implantation and pregnancy rates, but with fewer embryos transferred [29]. There are 2 possible reasons underlying the increased pregnancy rate among patients treated with D4 ET compared to D3 ET. Firstly, the expression of embryonic genes is initiated on D4, and thus the embryos with higher developmental potential can be selected after D4. As a consequence, D4 morula-stage embryos confer a greater selection value than cleavage-stage embryos [29,30]. Secondly, the uterine contractility is reduced at D4, and the embryos demonstrate improved synchronicity with the receptive endometrium [31].
To assess which D4 embryo is more conducive to good clinical outcomes, we further divided the D4 group into 3 groups: in group 1 the embryo was compacted but not expanded, in group 2 the embryo was compacted and expanded, and in group 3 the embryo was not compacted. We found that there were no live births in group 3. The clinical pregnancy rate of group 2 showed an upward trend compared with group 1 (48.48% vs 60.78%,
Conclusions
Our results suggest that D4 ET can allow a more flexible ET scheduling between clinicians and patients and avoid ET during weekends and holidays, without affecting IVF success rates. It offers an easier, flexible, and valuable method for routine ET. D4 transfer could be complementary to our current transfer strategy. In this way, patients, clinicians, and laboratorians would have more choices on the transfer day.
Due to the relatively small sample size in this study, further investigations with larger sample sizes are warranted.
Tables
Table 1. Comparison of demographic and clinical data between D4 and D5 group.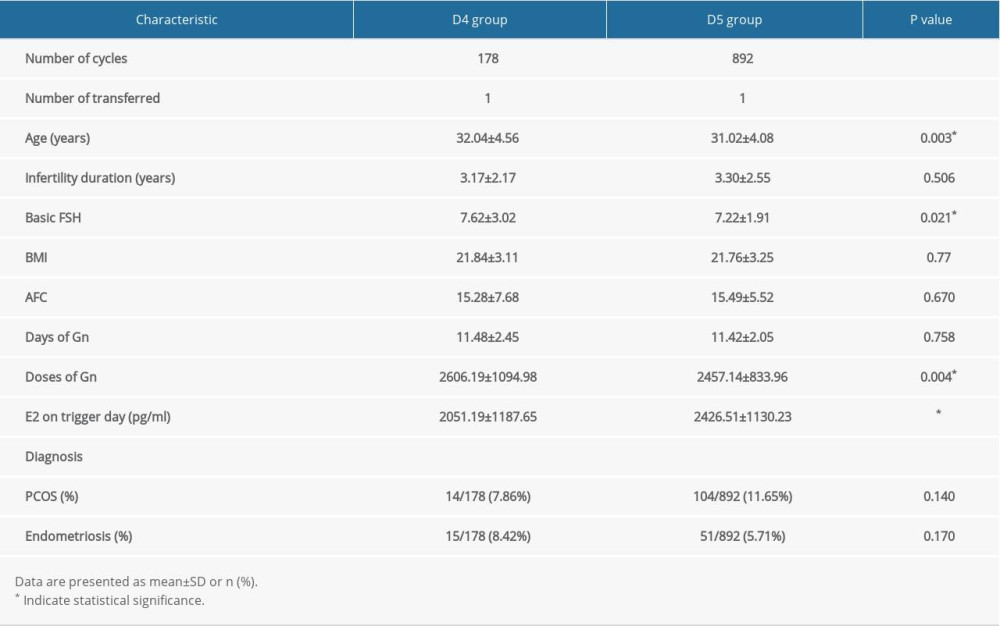 Table 2. Comparison of laboratory data between D4 and D5 group.
Table 2. Comparison of laboratory data between D4 and D5 group.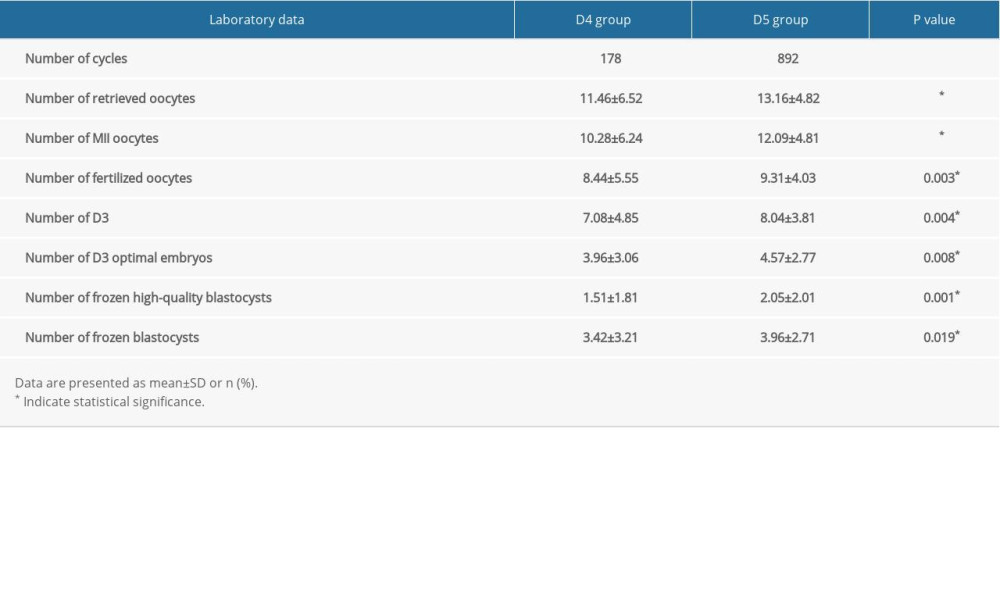 Table 3. Comparison of pregnancy outcomes between D4 and D5 groups.
Table 3. Comparison of pregnancy outcomes between D4 and D5 groups.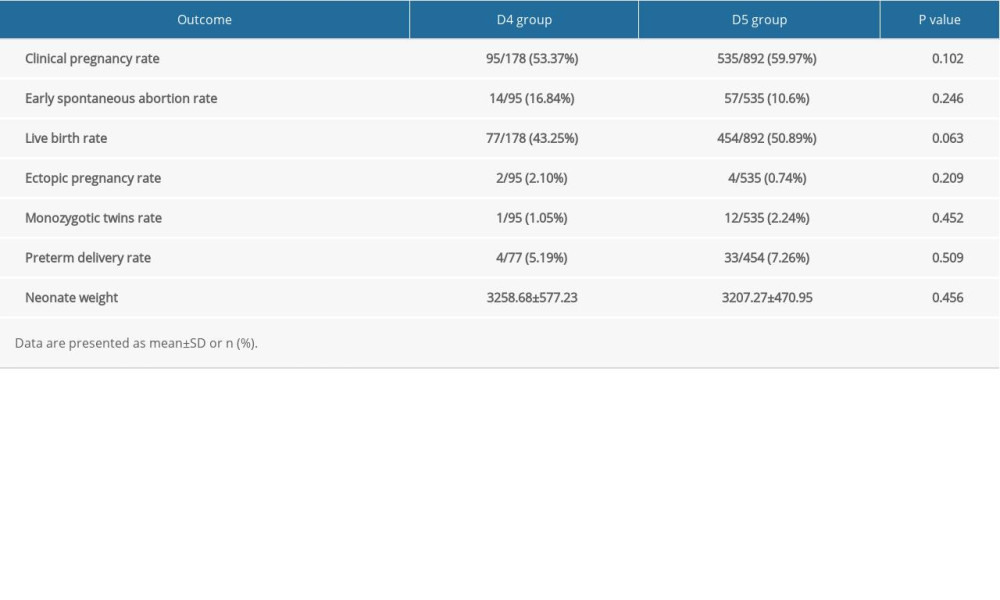 Table 4. Comparison of demographic and clinical data between group 1 and group 2.
Table 4. Comparison of demographic and clinical data between group 1 and group 2.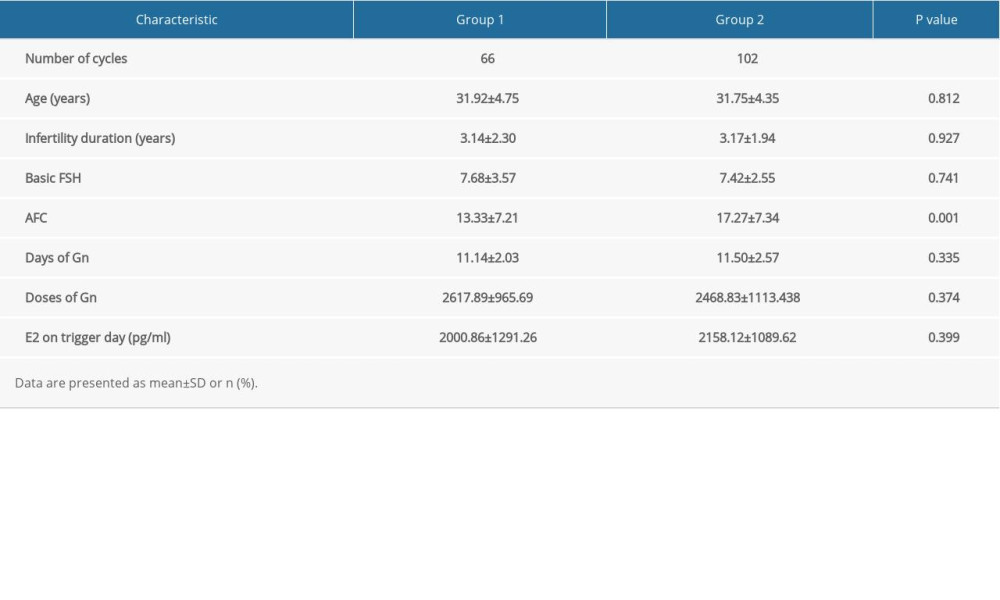 Table 5. Comparison of laboratory data between group 1 and group 2.
Table 5. Comparison of laboratory data between group 1 and group 2.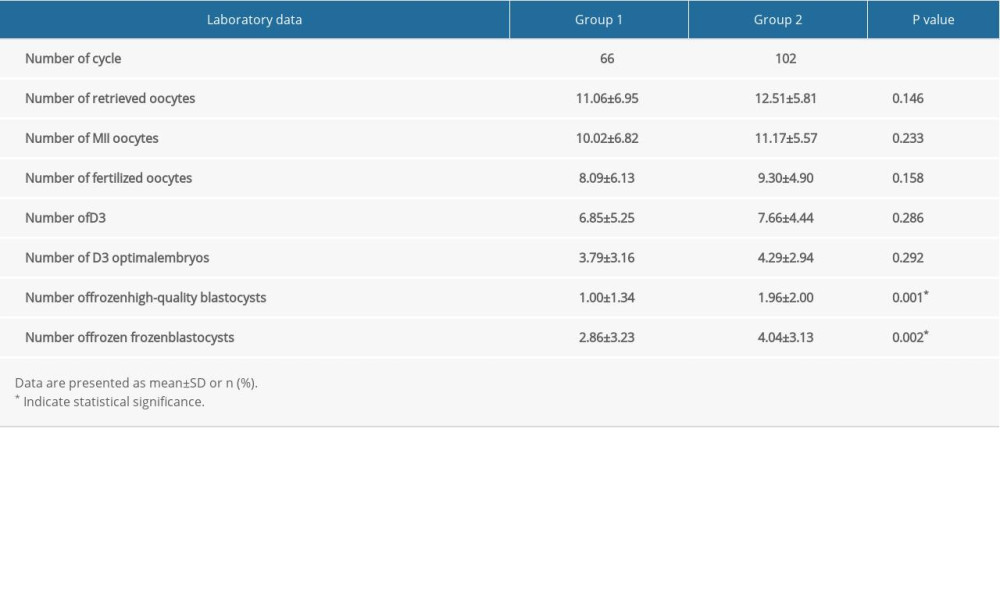 Table 6. Comparison of pregnancy outcomes between group 1 and group 2.
Table 6. Comparison of pregnancy outcomes between group 1 and group 2.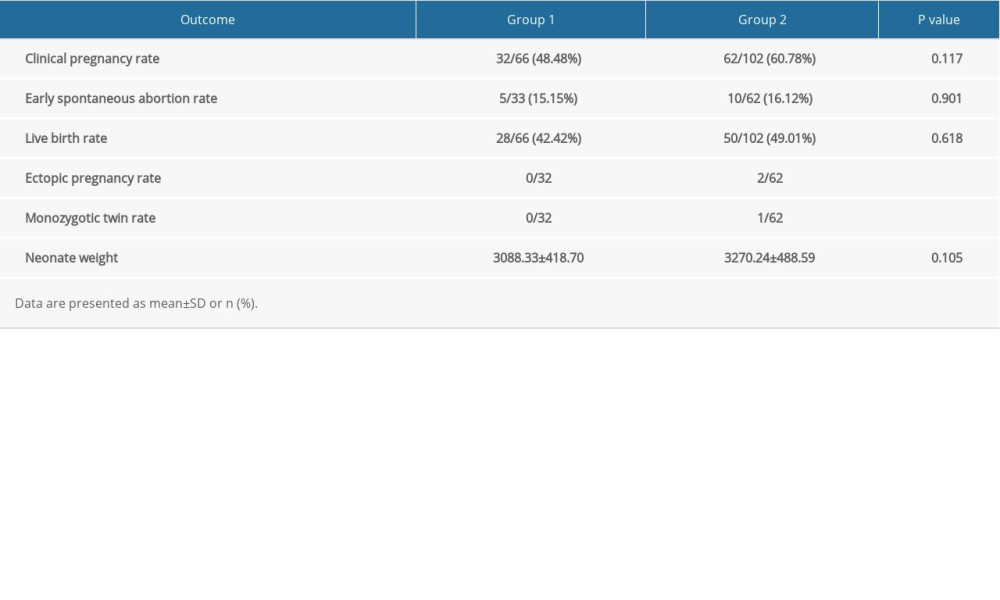
References
1. Papanikolaou EG, Camus M, Kolibianakis EM, In vitro fertilization with single-blastocyst-stage versus single cleavage-stage embryos: N Engl J Med, 2006; 354; 1139-46
2. Maheshwari A, Kalampokas T, Davidson J, Bhattacharya S, Obstetric and perinatal outcomes in singleton pregnancies resulting from the transfer of blastocyst-stage versus cleavage-stage embryos generated through in vitro fertilization treatment: A systematic review and meta-analysis: Fertil Steril, 2013; 100; 1615-21
3. Levi-Setti PE, Cirillo F, Smeraldi A, No advantage of fresh blastocyst versus cleavage stage embryo transfer in women under the age of 39: A randomized controlled study: J Assist Reprod Genet, 2018; 35; 457-65
4. National Collaborating Centre for Women’s and Children’s Health (UK): Fertility: Assessment and treatment for people with fertility problems Feb, 2013, London, Royal College of Obstetricians & Gynaecologists
5. Practice Committees of the American Society for Reproductive Medicine and the Society for Assisted Reproductive Technology, Blastocyst culture and transfer in clinical-assisted reproduction: A committee opinion: Fertil Steril, 2013; 99; 667-72
6. Phillips SJ, Dean NL, Buckett WM, Tan SL, Consecutive transfer of day 3 embryos and of day 5–6 blastocysts increases overall pregnancy rates associated with blastocyst culture: J Assist Reprod Genet, 2003; 20(11); 461-64
7. Alpha Scientists in Reproductive Medicine and ESHRE Special Interest Group of Embryology, The Istanbul consensus workshop on embryo assessment: proceedings of an expert meeting: Hum Reprod, 2011; 26(6); 1270-83
8. Li RS, Hwu YM, Lee RK, Day 4 good morula embryo transfer provided compatible live birth rate with day 5 blastocyst embryo in fresh IVF/ET cycles: Taiwan J Obstet Gynecol, 2018; 57; 52-57
9. Schoolcraft WB, Gardner DK, Lane M, Blastocyst culture and transfer: Analysis of results and parameters affecting outcome in two in vitro fertilization programs: Fertil Steril, 1999; 72(4); 604-9
10. CSRM, The Fourth Session of the committee of Chinese Society of Reproductive Medicine (CSRM) consensus on key indicators for quality control in ART clinical operation: J Reprod Med, 2018; 29; 825-35
11. Yin Y, Chen G, Li K, Propensity score-matched study and meta-analysis of cumulative outcomes of day 2/3 versus day 5/6 embryo transfers: Front Med, 2017; 11; 563-69
12. Yang L, Cai S, Zhang S, Single embryo transfer by Day 3 time-lapse selection versus Day 5 conventional morphological selection: A randomized, open-label, non-inferiority trial: Hum Reprod, 2018; 33; 869-76
13. Magli MC, Jones GM, Gras L, Chromosome mosaicism in day 3 aneuploid embryos that develop to morphologically normal blastocysts in vitro: Hum Reprod, 2000; 15(8); 1781-86
14. Braude P, Bolton V, Moore S, Human gene expression first occurs between the four-and eight-cell stages of preimplantation development: Nature, 1988; 332; 459-61
15. De Vos A, Van Landuyt L, Santos-Ribeiro S, Cumulative live birth rates after fresh and vitrified cleavage-stage versus blastocyst-stage embryo transfer in the first treatment cycle: Hum Reprod, 2016; 31; 2442-49
16. Glujovsky D, Farquhar C, Quinteiro Retamar AM, Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology: Cochrane Database Syst Rev, 2016; 30; CD002118
17. Martins WP, Nastri CO, Rienzi L: Ultrasound Obstet Gynecol, 2017; 49; 583-91
18. Behr B, Pool TB, Milki AA, Preliminary clinical experience with human blastocyst development in vitro without co-culture: Hum Reprod, 1999; 14; 454-57
19. Shen S, Rosen MP, Dobson AT, Day 2 transfer improves pregnancy outcome in in vitro fertilization cycles with few available embryos: Fertil Steril, 2006; 86; 44-50
20. Kang SM, Lee SW, Jeong HJ, Clinical outcomes of elective single morula embryo transfer versus elective single blastocyst embryo transfer in IVF-ET: J Assist Reprod Genet, 2012; 29; 423-28
21. Lee SH, Lee HS, Lim CK, Comparison of the clinical outcomes of day 4 and 5 embryo transfer cycles: Clin Exp Reprod Med, 2013; 40; 122-25
22. Holschbach V, Weigert J, Dietrich JE, Pregnancy rates of day 4 and day 5 embryos after culture in an integrated time-lapse incubator: Reprod Biol Endocrinol, 2017; 15; 37-44
23. Dar S, Lazer T, Shah PS, Librach CL, Neonatal outcomes among singleton births after blastocyst versus cleavage stage embryo transfer: A systematic review and meta-analysis: Hum Reprod Update, 2014; 20; 439-48
24. Maheshwari A, Hamilton M, Bhattacharya S, Should we be promoting embryo transfer at blastocyst stage?: Reprod Biomed Online, 2016; 32; 142-46
25. Zhu J, Lin S, Li M, Effect of in vitro culture period on birthweight of singleton newborns: Hum Reprod, 2014; 29; 448-54
26. Luke B, Brown MB, Wantman E, Stern JE, Factors associated with monozygosity in assisted reproductive technology pregnancies and the risk of recurrence using linked cycles: Fertil Steril, 2014; 101(3); 683-89
27. Ding J, Yin T, Zhang Y, The effect of blastocyst transfer on newborn sex ratio and monozygotic twinning rate: An updated systematic review and meta-analysis: Reprod Biomed Online, 2018; 37; 292-303
28. Lonergan P, Rizos D, Gutierrez-Adan A, Effect of culture environment on embryo quality and gene expression – experience from animal studies: Reprod Biomed Online, 2003; 7; 657-63
29. Tao J, Tamis R, Fink K, The neglected morula/compact stage embryo transfer: Hum Reprod, 2002; 17(6); 1513-18
30. Vassena R, Boué S, González-Roca E, Waves of early transcriptional activation and pluripotency program initiation during human preimplantation development: Development, 2011; 138(17); 3699-709
31. Lesny P, Killick SR, Tetlow RL, Uterine junctional zone contractions during assisted reproduction cycles: Hum Reprod Update, 1998; 4(4); 440-45
Tables
 Table 1. Comparison of demographic and clinical data between D4 and D5 group.
Table 1. Comparison of demographic and clinical data between D4 and D5 group. Table 2. Comparison of laboratory data between D4 and D5 group.
Table 2. Comparison of laboratory data between D4 and D5 group. Table 3. Comparison of pregnancy outcomes between D4 and D5 groups.
Table 3. Comparison of pregnancy outcomes between D4 and D5 groups. Table 4. Comparison of demographic and clinical data between group 1 and group 2.
Table 4. Comparison of demographic and clinical data between group 1 and group 2. Table 5. Comparison of laboratory data between group 1 and group 2.
Table 5. Comparison of laboratory data between group 1 and group 2. Table 6. Comparison of pregnancy outcomes between group 1 and group 2.
Table 6. Comparison of pregnancy outcomes between group 1 and group 2. In Press
05 Mar 2024 : Clinical Research
Effects of Thermal Insulation on Recovery and Comfort of Patients Undergoing Holmium Laser LithotripsyMed Sci Monit In Press; DOI: 10.12659/MSM.942836
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








