11 January 2021: Clinical Research
Lightwand-Guided Insertion of Flexible Reinforced Laryngeal Mask Airway: Comparison with Standard Digital Manipulation Insertion
Dae Hee Kim1BCD, Yun Jeong Chae1ADE, Sang Kee Min1CD, Eun Ji Ha1BC, Ji Young Yoo1ABEFG*DOI: 10.12659/MSM.928538
Med Sci Monit 2021; 27:e928538
Abstract
BACKGROUND: The flexibility of the long flexometallic tube makes insertion of the flexible reinforced laryngeal mask airway (f-LMA) difficult. We compared the usefulness of rigid lightwand-guided f-LMA insertion with standard digital manipulation.
MATERIAL AND METHODS: Fifty-four patients (aged 19–70 years) were randomly divided into a control group (digital manipulation technique) or the lightwand group (lightwand-guided insertion technique). The insertion profiles, oropharyngeal leak pressure (OLP), peak inspiratory pressure (PIP), expiratory tidal volume, and ventilatory score were measured in patients with neutral, extension, rotation, flexion, and re-neutral head-neck positions in turn.
RESULTS: The success rate and ease of insertion did not differ between groups, but the insertion time was longer in the lightwand group. The fiberoptic laryngeal view was significantly better in the lightwand group than in the control group. However, the OLP, PIP, expiratory tidal volume, and ventilatory scores were not significantly different between groups according to head-neck positions. The extension posture was associated with a significant negative effect on ventilation, but ventilation returned to initial levels with the other postures.
CONCLUSIONS: Lightwand-guided f-LMA insertion showed a better fiberoptic laryngeal view than standard digital manipulation, but no improvement in the ventilatory state was observed due to position. Therefore, lightwand-guided insertion could facilitate correct placement of the f-LMA, but it has limited clinical usefulness.
Keywords: airway management, Laryngeal Masks, Ventilation, Fiber Optic Technology, Intubation, Intratracheal, Larynx, Patient Positioning, Pulmonary Ventilation, Tidal Volume
Background
The flexible reinforced laryngeal mask airway (f-LMA; Teleflex Medical, Ireland) is used during surgery and permits various head-neck positions [1–7]. The stem of the f-LMA consists of a long flexometallic tube that does not interrupt the surgical field because it is compact, freely movable, and resistant to kinks and compression [8,9]. However, this flexibility makes insertion of the f-LMA more difficult compared with the classic LMA.
Several techniques have been suggested to overcome this issue and facilitate correct anatomical placement with rigid introducers such as the modified ProSeal LMA introducer, Bosworth introducers, flexiguide introducer, spatula introducer, modified Magill forceps, and a small tracheal tube combined with a stylet [8–13]. All devices seem to be useful, but no randomized studies have been conducted to assess them. Further, most of the devices require preparation, and therefore, they are not commonly used clinically. Moreover, the final placement simply depends on the resistance perception when the f-LMA is pushed down.
A rigid lightwand (Light Way®, Luminous stylet, Ace Medical, Goyang, South Korea) could function as a rigid introducer as well as a real-time guide for correct placement through transillumination. One study assessing the classic LMA reported that a rigid lightwand was useful for correct placement and led to a higher success rate on the first attempt [14]. However, the tubes in classic LMA and f-LMA are different. Hence, we aimed to investigate the efficacy of a rigid lightwand-guided f-LMA insertion technique compared with the standard digital manipulation method in terms of oropharyngeal leak pressure (OLP) and ideal anatomical placement in adult patients with various head-neck positions.
Material and Methods
This clinical trial was approved by the Ajou University Institutional Review Board (AJIRB MED-OBS-17-108) and was registered at ClinicalTrials.gov (NCT 03224611). Written informed consent was obtained from each patient after enrollment. Fifty-four patients, aged 19–70 years, with an American Society of Anesthesiologist (ASA) physical status I or II who required elective general anesthesia with an LMA were included in the study. Patients with a recent upper airway tract infection, orofacial anomaly, a body mass index >35 kg/m2, gastroesophageal reflux, or a risk of gastric content aspiration were excluded from the study. Patients were assigned to either of the 2 groups (control group or lightwand group) using a computer-generated randomization table. The random allocation sequence was generated by an investigator who was not involved in this study. This investigator revealed the patient’s corresponding group and number by calling just before anesthesia induction. The airway was assessed using the Mallampati airway classification [15], and mouth opening, presence of buck teeth, presence of a receding mandible, and the thyromental distance were evaluated by another investigator who was unaware of patient grouping. These data were recorded in the preanesthetic period [16].
No premedication was administered before surgery. Upon arrival at the operating room, all patients were subjected to an electrocardiogram, pulse oximetry, noninvasive blood pressure measurement, and bispectral index monitoring. After preoxygenation with 4 L/min of 100% O2 for 3 min, patients were administered intravenous (IV) fentanyl 0.5–1 μg/kg and propofol 1.5–2 mg/kg. After loss of consciousness, muscles were relaxed by rocuronium 0.6 mg/kg. Manual ventilation was applied with 100% O2 and sevoflurane (1.0–1.5% minimum alveolar concentration) for 90 s. Then, the appropriate-sized f-LMA was inserted. The size of the f-LMA was chosen based on the patient’s body weight (size 3 for <50 kg and size 4 for 50–70 kg). In both groups, the f-LMA was inserted by an investigator (JY Yoo) who had over 10 years of experience with the f-LMA and practiced lightwand-guided insertion of f-LMA 20 times before the study. In the control group patients, the f-LMA was inserted using the standard digital manipulation method according to the manufacturer’s guidelines, as follows. One hand was used to open the mouth, and the other hand was used to insert the f-LMA with digital pressure being applied to the proximal part of the flexometallic tube. The tip of the f-LMA was pressed against the hard palate and pushed along its midline until resistance was met. In the lightwand group, the lubricated lightwand was inserted in the flexometallic stem of the f-LMA, with the distal part of the lightwand flexed at 90° (i.e., in an L shape). The tip of the lightwand was located just behind the opening of the f-LMA. Then, one hand was used to grip the mandible for opening the mouth and the other hand was used to insert the f-LMA with the lightwand, maintaining the shape of the flexion. After the correct transillumination of the anterior neck was confirmed, the f-LMA was seated and the lightwand was removed. The cuff of the f-LMA was then inflated according to the manufacturer’s recommendations (20 mL for size 3 and 30 mL for size 4).
The investigator (JY Yoo) confirmed successful insertion based on the following criteria: (1) no signs of airway obstruction; (2) absence of any air leakage with manual ventilation; and (3) observation of chest expansion with the end-tidal CO2 curve during manual ventilation. The number of insertion attempts, ease of insertion, and insertion time were recorded. We limited the insertion attempts to 2 times before tracheal intubation was performed because the ventilation was considered inappropriate. The ease of insertion was graded as easy, fair, or difficult. The insertion time was defined from the time of opening the mouth to the time when the end-tidal CO2 curve was confirmed. If a second attempt was made, the insertion time was recorded as the sum of the times for the first and second attempts. An investigator who was blinded to the insertion technique evaluated the following parameters: OLP, peak inspiratory pressure (PIP), expiratory tidal volume, and ventilation score in 5 different head-neck positions, and the fiberoptic laryngeal score in 2 positions. These parameters were first evaluated for a neutral head and neck position (neutral position: occiput resting on the operating table), and then with an extended neck (extension position: a 15-cm pillow was placed at the level of acromion process of the scapula), right rotated neck (rotation position: fully rotated to right in natural angle), flexed neck (flexion position: a 15-cm pillow was placed at occiput), and re-neutral position in order for each patient. The fiberoptic laryngeal score was evaluated for the neutral position and the re-neutral position. For each position, the parameters were evaluated after a 60-s adjustment. The primary parameter assessed was OLP, which was defined as the airway pressure when an audible leakage sound was first detected around the patient’s mouth when the expiratory valve of the circle system was closed at a fixed gas flow rate of 3 L/min [17]. The PIP was defined as the inspiratory airway pressure at a tidal volume of 8 mL/kg of the patient’s ideal body weight and with the peak end-expiratory pressure set at 5 cmH2O. The ventilation score was measured based on 3 criteria and ranged from 0 to 3: no leakage with an airway pressure of 15 cmH2O (the gas leakage was defined as an audible leak sound detected by a stethoscope around the mouth), bilateral chest excursions with a PIP of 20 cmH2O, and a square wave capnogram. The f-LMA position was measured by the fiberoptic laryngeal scoring system using a fiberoptic bronchoscope (Karl Storz SE & Co. KR) [18]. The fiberoptic laryngeal score was categorized as follows: 1, vocal cords not visible; 2, vocal cords plus anterior epiglottis visible; 3, vocal cords plus posterior epiglottis visible; and 4, only vocal cords visible. Anesthesia was maintained with 1.5–2.5 vol% sevoflurane targeting a bispectral index between 40 and 60 and a mean blood pressure and heart rate within 20% of baseline values. Mechanical ventilation was adjusted to maintain an end-tidal CO2 between 35 and 40 mm Hg using 40% oxygen. Sore throat and hoarseness were evaluated in the recovery room after the operation by the investigator who was blinded to the study.
According to a power analysis with a 5% 2-sided type I error rate and 80% power, a sample size of 22 patients per group was required to detect a projected 20% difference in OLP with an assumed standard deviation of 5 [19,20]. We recruited a total of 54 patients to compensate for possible dropouts. Statistical analyses were performed using the IBM Statistical Package for Social Sciences (SPSS ver. 20.0 for Windows). The normality of the data was assessed using the Kolmogorov-Smirnov test. Data are presented as the mean±standard deviation, median (interquartile range), or number of patients where appropriate. The normally distributed data were analyzed by
Results
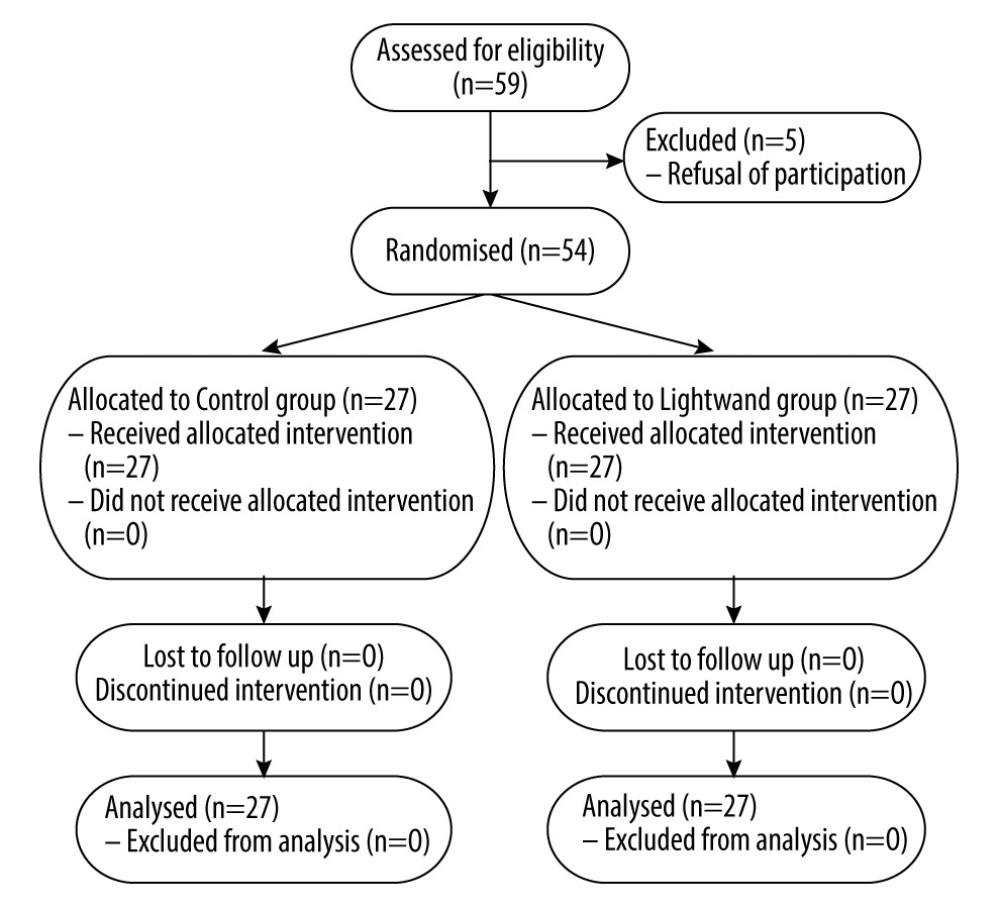
A total of 59 patients were screened for this study; 5 patients were excluded due to patient refusal, and 54 patients were finally enrolled (Figure 1). Patients in the control and lightwand groups were comparable in terms of age, sex, height, and weight (Table 1). The preanesthetic airway assessment data were also not significantly different between the groups.
The insertion profiles are presented in Table 2. Insertion was successful in 52 patients within 2 attempts. The success rate for the first attempt was 81.5% (22/27) and 70.4% (19/27) in the control and lightwand groups, respectively, and was not significantly different between groups. Excluding 2 cases, insertion was successful in the remaining failed cases on the second attempt. Finally, both groups had the same (96.3%) success rate within 2 attempts. Two patients, 1 from each group required intubation because ventilation was not effective even after the second insertion attempt. The median insertion time (first attempt plus second attempt) was 30.0 and 47.0 s in the control group and lightwand groups, respectively, and was significantly higher in the lightwand group (
Variables representing the ventilatory state for several head-neck positions are presented in Tables 3 and 4. The OLP, PIP, expiratory tidal volume, and ventilation score did not differ significantly between the 2 groups. OLP was lowest with the extension position (
The fiberoptic laryngeal score for the f-LMA placement was significantly higher in the lightwand group than in the control group (
When categorized according to the fiberoptic laryngeal score (I, II, III, IV) in the neutral position, the OLP, PIP, expiratory tidal volume, and ventilation score were not significantly different between the 2 groups (Table 5). With the extension position, almost all values were significantly worse compared with the neutral position for almost all levels of the fiberoptic laryngeal score. Furthermore, fiberoptic laryngeal score IV had a significantly better ventilatory score with the neutral position and better expiratory tidal volume with the extension position compared with fiberoptic laryngeal score I.
Complications such as sore throat and hoarseness assessed in the Postanesthesia Care Unit were similar in both groups.
Discussion
This study demonstrated that the rigid lightwand-guided insertion technique for f-LMA provided a significantly better fiberoptic laryngeal view than the standard digital manipulation technique, but it did not show a significant difference in OLP based on head and neck positions. Furthermore, other ventilatory variables such as PIP, expiratory tidal volume, and ventilatory score were not significantly different between groups.
Although the digital manipulation technique is widely used, insertion of the f-LMA could be challenging in some situations when the f-LMA cannot be fully driven into position with the index finger [21]. This difficulty with positioning is due to the flexibility of the reinforced f-LMA tube which does not allow the inserting force to be effectively transmitted along the shaft [12]. Many devices have been described to facilitate correct placement [8–13] by functioning as a rigid introducer. However, the lightwand could function as a real-time guide through transillumination as well as being a rigid introducer. As a rigid introducer, the lightwand has advantages and disadvantages in our experience. The force for insertion was readily transmitted along the shaft, and the passage through the oropharyngeal area was easy. However, the mask of the f-LMA tended to rotate along its axis because the lightwand was too loose to fit to the shaft of the f-LMA. We found that the mask position needed to be adjusted to confirm the transillumination clearly even after the resistance was encountered, unlike digital manipulation in which the feeling of resistance was the final target. In this process, correction of the depth was easy, but correction of the mask direction was difficult when required. As a result, the lightwand-guided insertion technique had a longer insertion time but induced better optimal positioning of the f-LMA than the standard digital manipulation technique. The longer insertion time was not associated with the difficulty of insertion, and the ease of insertion was similar between both groups. Moreover, a 96.3% (25/26) success rate was found within 2 attempts, similar to the standard digital manipulation group. Therefore, lightwand-guided insertion can be an alternative technique for f-LMA insertion and a better alternative when an ideal anatomic placement is desirable.
The ideal anatomic placement of LMA has been found to have theoretical benefits such as minimizing the risk of airway displacement and improving airflow dynamics with less leakage [22,23]. Joshi et al. [24] reported that the fiberoptic laryngeal score showed a good correlation with the ability to generate an airway pressure of 20 cmH2O, while Berry et al. [25] reported a correlation between the view of the cords and OLP. In contrast, Brimacombe et al. [26] found no correlation between the fiberoptic score and OLP. The OLP is used to quantify the efficacy of sealing of the LMA [27]. A higher OLP is considered a good marker for providing positive ventilation effectively and protecting the airway from supra-cuff soiling [28]. In the current study, the OLP was somewhat higher in the lightwand group for the neutral, flexion, extension, and re-neutral positions, but not the rotation position. However, no significant difference was found between the 2 groups. Other ventilatory variables such as PIP, expiratory tidal volume, and ventilatory scores were somewhat more favorable in the lightwand group, but there was no statistical difference between the groups. In other words, contrary to our expectation, better anatomical placement of the f-LMA using the lightwand did not necessarily improve the ventilatory state. To further explore the effect of the anatomic placement of the f-LMA on the ventilatory state, we categorized the variables according to the fiberoptic laryngeal score (I, II, III, IV) in the neutral position. The fiberoptic laryngeal score IV tended to keep the OLP high. A significantly better ventilatory score than the fiberoptic laryngeal score I was observed with the neutral position, and the ventilatory score was maintained without deterioration in the re-neutral position. In addition, a significantly higher expiratory tidal volume than the fiberoptic laryngeal score I was observed with the extension position. Taken together, these findings imply that the ideal anatomical placement of the f-LMA was indeed slightly beneficial in the expected direction, but the benefits were not enough to yield clinically meaningful differences between the groups. Therefore, the clinical usefulness of lightwand-guided f-LMA insertion for better positioning is limited.
Head-neck movement changes the shape of the pharynx [29]. The anteroposterior diameter is decreased with the flexion position and increased with the extension position. The head rotation also increased the anteroposterior distance and cross-sectional area in the retroglossal region [20]. According to the results of previous studies assessing LMA with a less-flexible tube, such as a classic LMA, air-Q, Ambu AuraGain, or i-gel, the OLP tended to decrease with the extension position, increase with the flexion position, and was comparable with the rotated position [30–33]. In terms of the OLP, the extension position appeared to decrease mask sealing, but the flexion position appeared to promote sealing [34]. However, the effect on ventilation was varied; the ventilatory score was worse with the extension position in some cases, worse with the flexion position in other cases, or showed no difference in still other cases [30–33]. Considering the direction of change of PIP, ventilation was negatively affected due to leakage in the extension position and obstruction in the flexion position, in cases in which the head-neck position affected ventilation. In this study, the f-LMA, OLP, expiratory tidal volume, and ventilatory score were remarkably reduced with the extension position, while they remained unchanged with the flexion and rotation positions. It is unclear whether the flexibility of the reinforced tube of the f-LMA might affect these results. According to Keller et al. [20], the OLP showed little difference between the f-LMA and classic LMA, but the ventilatory score and expiratory tidal volume were not recorded. Compared with their study, we used a larger pillow (15
This study has a few limitations. First, the investigator that measured the outcomes was not blinded to the head-neck positions because it was not feasible. Second, the generalizability of our results to patients under spontaneous ventilation might be limited because a muscle relaxant was used for insertion of the f-LMA.
Conclusions
Lightwand-guided f-LMA insertion did not show a significant difference in the ventilatory state in several positions despite a better fiberoptic laryngeal view compared with standard digital manipulation. Lightwand-guided insertion could facilitate correct placement of the f-LMA, but it has limited clinical usefulness.
Tables
Table 1. Patient characteristics.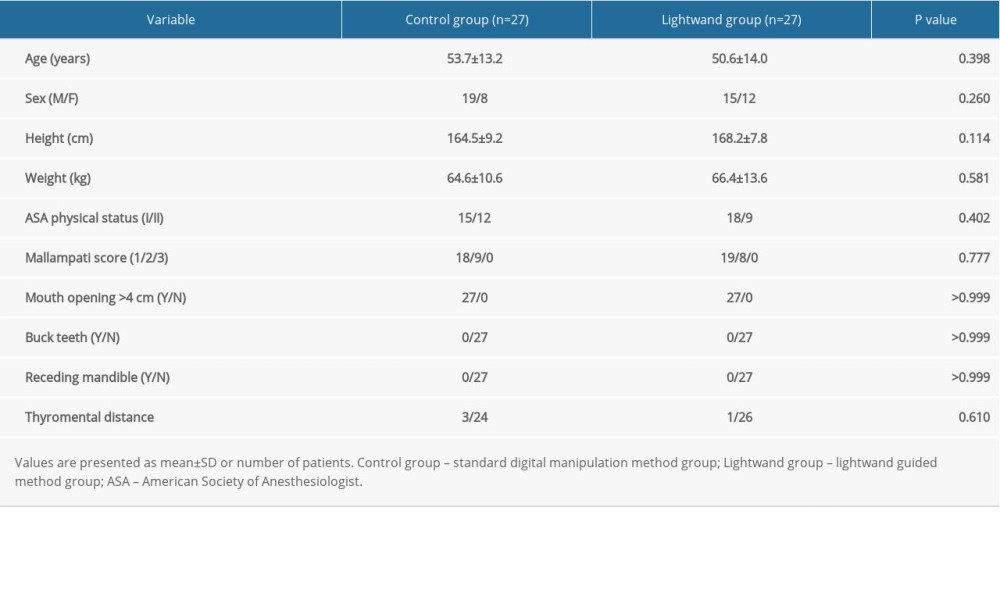 Table 2. Insertion profiles.
Table 2. Insertion profiles.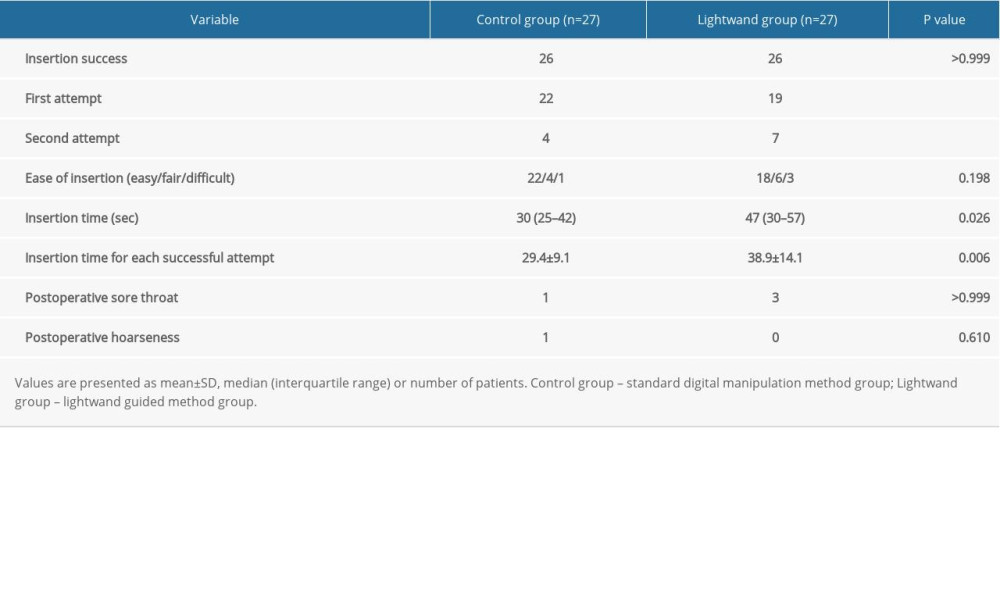 Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions.
Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions.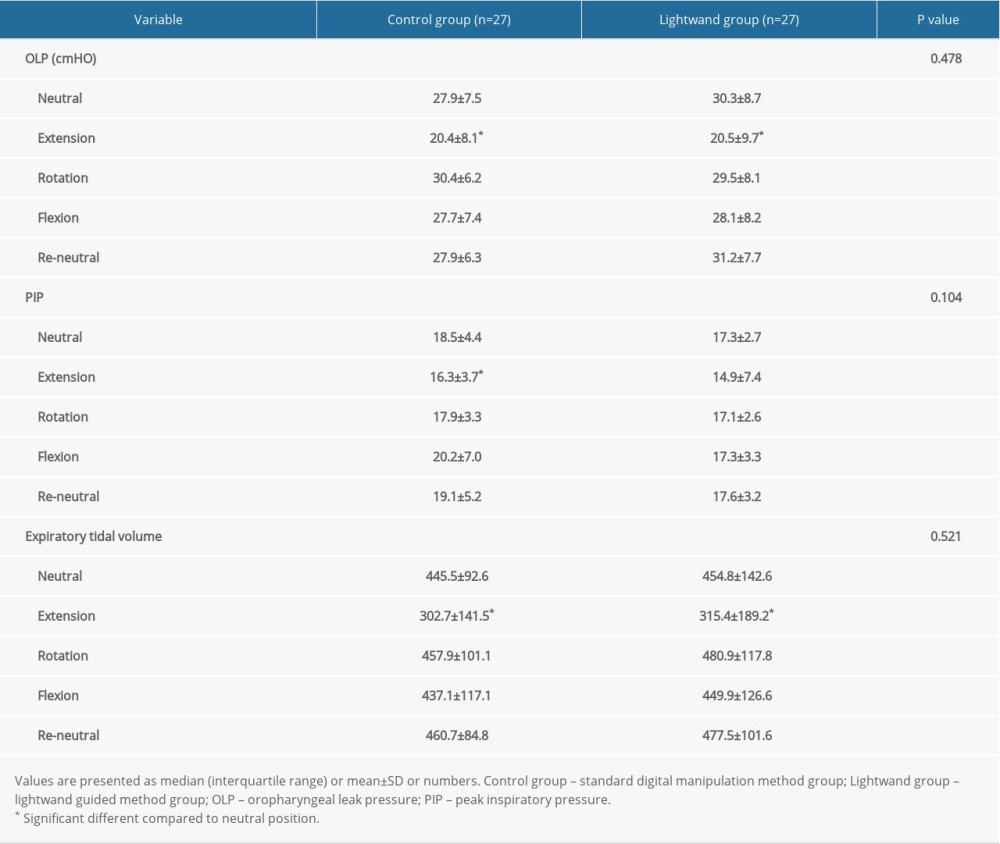 Table 4. Ventilatory score and fiberoptic laryngeal score in several positions.
Table 4. Ventilatory score and fiberoptic laryngeal score in several positions.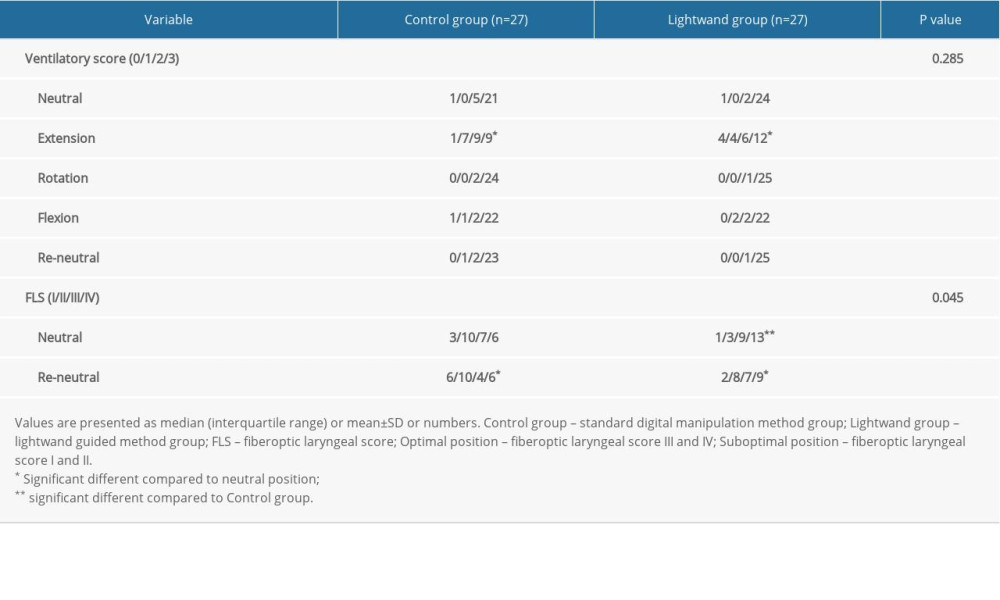 Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions.
Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions.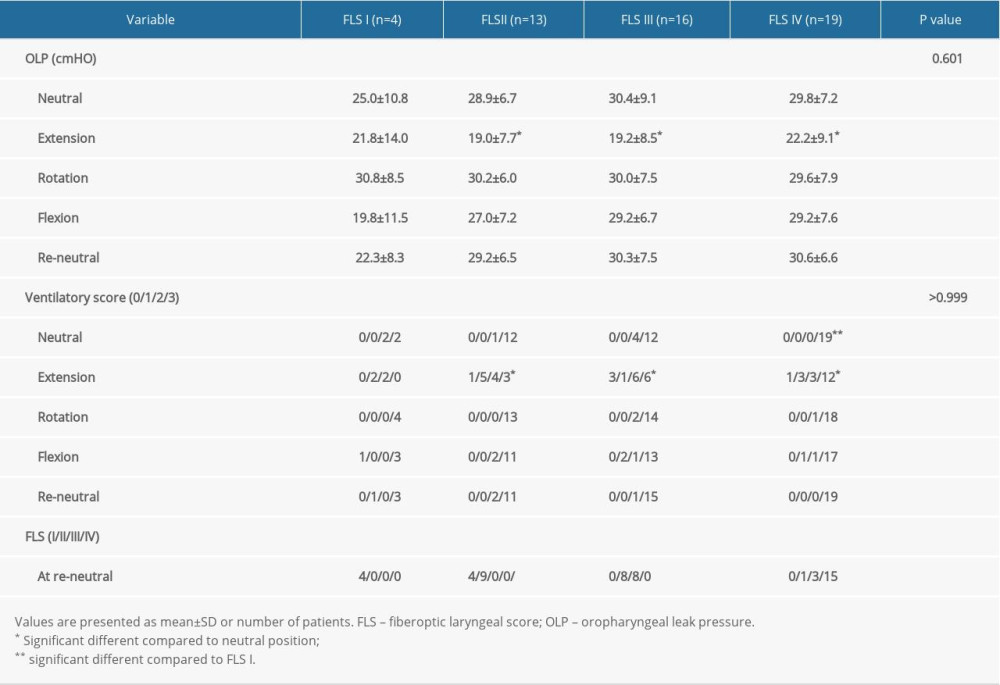
References
1. Quinn A, Samaan A, McAteer E, Moss E, Vucevic M, The reinforced laryngeal mask airway for dento-alveolar surgery: Br J Anaesth, 1996; 77(2); 185-88
2. Webster AC, Morley-Forster PK, Janzen V, Anesthesia for intranasal surgery: A comparison between tracheal intubation and the flexible reinforced laryngeal mask airway: Anesth Analg, 1999; 88(2); 421-25
3. Williams P, Bailey P, Comparison of the reinforced laryngeal mask airway and tracheal intubation for adenotonsillectomy: Br J Anaesth, 1993; 70(1); 30-33
4. Xu R, Lian Y, Li WX, Airway complications during and after general anesthesia: A comparison, systematic review and meta-analysis of using flexible laryngeal mask airways and endotracheal tubes: PLoS One, 2016; 11(7); e0158137
5. Bailey P, Brimacombe JR, Keller C, The flexible LMA: Literature considerations and practical guide: Int Anesthesiol Clin, 1998; 36(2); 111-22
6. Martin-Castro C, Montero A, Flexible laryngeal mask as an alternative to reinforced tracheal tube for upper chest, head and neck oncoplastic surgery: Eur J Anaesthesiol, 2008; 25(4); 261-66
7. Todd D, The laryngeal mask airway for general anesthesia: the case for its use: J Oral Maxillofac Surg, 2004; 62(6); 736-38
8. Kulkarni AH, Simon BP, Jose JK, A new flexible laryngeal mask airway introducer: Indian J Anaesth, 2012; 56(1); 94-95
9. Shimoda O, Yoshitake A, Stylet for reinforced laryngeal mask airway: Anaesthesia, 2002; 57(11); 1140-41
10. Bosworth A, Jago R, The Bosworth introducer for use with the flexible reinforced laryngeal mask airway: Anaesthesia, 1997; 52(3); 281-82
11. Cook T, Ford P, Craft T, An evaluation of the flexiguide introducer with the flexible laryngeal mask airway: Anaesth Intensive Care, 2003; 31(2); 193-95
12. Kil HK, Koo BN, Park JH, Kim WO, The spatula introducer for insertion of the flexible reinforced laryngeal mask airway (RLMA): Can J Anaesth, 2005; 52(1); 117-18
13. Welsh B, Use of a modified Magill’s forceps to place a flexible laryngeal mask: Anaesthesia, 1995; 50(11); 1002-3
14. Lu W, Zheng J, Gao L, Wang Y, A comparison of classic laryngeal mask airway insertion between lightwand-and standard index finger – guided techniques: J Clin Anesth, 2016; 33; 309-14
15. Mallampati SR, Gatt SP, Gugino LD, A clinical sign to predict difficult tracheal intubation; A prospective study: Can Anaesth Soc J, 1985; 32(4); 429-34
16. Wilson M, Spiegelhalter D, Robertson J, Lesser P, Predicting difficult intubation: Br J Anaesth, 1988; 61(2); 211-16
17. Keller C, Brimacombe J, Keller K, Morris R, Comparison of four methods for assessing airway sealing pressure with the laryngeal mask airway in adult patients: Br J Anaesth, 1999; 82(2); 286-87
18. Brimacombe J, Berry A, A proposed fiber-optic scoring system to standardize the assessment of laryngeal mask airway position: Anesth Analg, 1993; 76(2); 457
19. Brimacombe J, Keller C, Comparison of the flexible and standard laryngeal mask airways: Can J Anaesth, 1999; 46(6); 558-63
20. Keller C, Brimacombe J, The influence of head and neck position on oropharyngeal leak pressure and cuff position with the flexible and the standard laryngeal mask airway: Anesth Analg, 1999; 88(4); 913-16
21. Asai T, Stacey M, Barclay K, Stylet for reinforced laryngeal mask airway: Anaesthesia, 1993; 48(7); 636
22. Campbell RL, Biddle C, Assudmi N, Fiberoptic assessment of laryngeal mask airway placement: Blind insertion versus direct visual epiglottoscopy: J Oral Maxillofac Surg, 2004; 62(9); 1108-13
23. Chandan SN, Sharma SM, Raveendra US, Rajendra Prasad B, Fiberoptic assessment of laryngeal mask airway placement: A comparison of blind insertion and insertion with the use of a laryngoscope: J Maxillofac Oral Surg, 2009; 8(2); 95-98
24. Joshi S, Sciacca RR, Solanki D, A prospective evaluation of clinical tests for placement of laryngeal mask airways: Anesthesiology, 1998; 89(5); 1141-46
25. Berry AM, Brimacombe JR, McManus KF, Goldblatt M, An evaluation of the factors influencing selection of the optimal size of laryngeal mask airway in normal adults: Anaesthesia, 1998; 53(6); 565-70
26. Brimacombe JR, Positive pressure ventilation with the size 5 laryngeal mask: J Clin Anesth, 1997; 9(2); 113-17
27. Shin HW, Yoo HN, Bae GE: J Int Med Res, 2016; 44(3); 405-18
28. Zhang L, Seet E, Mehta V, Oropharyngeal leak pressure with the laryngeal mask airway Supreme™ at different intracuff pressures: A randomized controlled trial: Can J Anaesth, 2011; 58(7); 624-29
29. Nandi PR, Charlesworth CH, Taylor SJ, Effect of general anaesthesia on the pharynx: Br J Anaesth, 1991; 66(2); 157-62
30. Abdel-Ghaffar HS, Abdelal FA, Osman MA, Soliman OM, Device stability and quality of ventilation of classic laryngeal mask airway versus AIR-Q and I-gel at different head and neck positions in anesthetized spontaneously breathing children: Minerva Anestesiol, 2020; 86(3); 286-94
31. Yoo S, Park SK, Kim WH, Influence of head and neck position on performance of the Ambu(R) AuraGain laryngeal mask: A randomized crossover study: Minerva Anestesiol, 2019; 85(2); 133-38
32. Lee JH, Jang YE, Kim EH, Flexion decreases the ventilation quality of the Ambu((R)) AuraGain laryngeal mask in paralysed children: A prospective randomised crossover study: Acta Anaesthesiol Scand, 2018 [Online ahead of print]
33. Kim HJ, Lee K, Bai S, Influence of head and neck position on ventilation using the air-Q(R) SP airway in anaesthetized paralysed patients: A prospective randomized crossover study: Br J Anaesth, 2017; 118(3); 452-57
34. Isserles SA, Rozenberg B, LMA-reduction of gas leak: Can J Anaesth, 1995; 42(5 Pt 1); 449
Tables
 Table 1. Patient characteristics.
Table 1. Patient characteristics. Table 2. Insertion profiles.
Table 2. Insertion profiles. Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions.
Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions. Table 4. Ventilatory score and fiberoptic laryngeal score in several positions.
Table 4. Ventilatory score and fiberoptic laryngeal score in several positions. Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions.
Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions. Table 1. Patient characteristics.
Table 1. Patient characteristics. Table 2. Insertion profiles.
Table 2. Insertion profiles. Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions.
Table 3. Oropharyngeal leak pressure, peak inspiratory pressure, and expiratory tidal volume in several positions. Table 4. Ventilatory score and fiberoptic laryngeal score in several positions.
Table 4. Ventilatory score and fiberoptic laryngeal score in several positions. Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions.
Table 5. Comparison of the data that were categorized by fiberoptic laryngeal score in the initial neutral position with various head positions. In Press
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
08 Mar 2024 : Clinical Research
Evaluation of Foot Structure in Preschool Children Based on Body MassMed Sci Monit In Press; DOI: 10.12659/MSM.943765
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952