20 February 2021: Animal Study
Effects and Mechanism of Noninvasive Positive-Pressure Ventilation in a Rat Model of Heart Failure Due to Myocardial Infarction
Shan Liu1ACDEF, He Jiang2ACDEF, Chao Chang3BF, Yuhua Rui4BF, Zhigang Zuo5BF, Ting Liu1BF, Yanqiu Song1B, Fumei Zhao1BF, Qingliang Chen6ACDEFG, Jie Geng7ACDEFG*DOI: 10.12659/MSM.928476
Med Sci Monit 2021; 27:e928476
Abstract
BACKGROUND: Impaired heart function induced by myocardial infarction is a leading cause of chronic heart failure (HF). This study aimed to investigate the effects and mechanism of noninvasive positive-pressure ventilation (NIPPV) in a rat model of HF due to myocardial infarction.
MATERIAL AND METHODS: To explore the therapeutic effect and mechanism of NIPPV on acute myocardial infarction-induced HF, we established a rat model of HF by ligating the anterior descending branch of the left coronary artery and confirmed by ultrasonic cardiography and brain natriuretic peptide 45 detection.
RESULTS: The levels of heat-shock protein (HSP)-70 increased and matrix metalloproteinase (MMP)-2, MMP-9, and tumor necrosis factor (TNF)-α decreased in the group that received NIPPV treatment compared with the control group. In addition, the histopathologic results showed less severe inflammatory infiltration and a smaller area of myocardial fibrosis in the NIPPV treatment group.
CONCLUSIONS: In a rat model of HF due to myocardial infarction, NIPPV resulted in increased levels of HSP70 and reduced expression of MMP2, MMP9, and TNF-α and reduced myocardial neutrophil infiltration and fibrosis. Taken together, we showed that NIPPV is an effective treatment for HF induced by myocardial infarction by inhibiting the release of inflammatory factors and preventing microvascular embolism.
Keywords: HSP70 Heat-Shock Proteins, Positive-Pressure Respiration, Cardiomyopathies, Echocardiography, Fibrosis, Matrix Metalloproteinase 2, Matrix Metalloproteinase 9, Myocardium, Rats, Wistar, Ventricular Remodeling
Background
Heart failure (HF) is the terminal stage of various heart diseases that is caused by disorders of diastolic and systolic functions of the heart and results in pulmonary edema, ventricular filling, and dyspnea [1]. Coronary heart disease is a common cause of HF, of which 50% are secondary myocardial infarctions in China [2]. After acute myocardial infarction (AMI), myocardial cell necrosis and apoptosis due to the lack of blood and oxygen supply lead to a reduction of cardiac output, resulting in acute HF and even cardiogenic shock [3]. In addition, the failure to reperfuse in time after AMI may lead to further cardiac insufficiency and chronic HF [4]. The process of AMI to HF develops rapidly and continuous hypoxia and heart overload will cause irreversible damage to the important organs. Percutaneous coronary intervention (PCI) and intravenous thrombolysis reperfusion, which are recommended treatment strategies for patients who have acute ST-segment-elevation myocardial infarction, can rescue ischemic myocardium and reduce the myocardial infarct area [5,6]. Although early treatment of recanalization and revascularization greatly reduce myocardial necrosis, cardiac function continues to decline in most AMI patients after PCI treatment. Many patients may have myocardial infarction, angina pectoris, and HF again due to stent restenosis. Moreover, ischemia-reperfusion injury (IRI) inevitably occurs in tissues and organs after blood flow resumption. Myocardial stunning (MS), which is one of the manifestations of myocardial IRI, prevents the aggravation of myocardial ischemia by weakening myocardial contraction and lasts for days or even weeks [7,8]. Cardiac dysfunction often occurs in patients who have AMI mainly due to MS after reperfusion treatment, which is a leading cause of HF and myocardial infarction [9]. Therefore, it is crucial to alleviate the symptoms of HF so as to benefit most from PCI and reperfusion treatment.
Noninvasive positive-pressure ventilation (NIPPV), including continuous positive airway pressure, adaptive servoventilation, and bilevel positive airway pressure (BiPAP), is a method of increasing alveolar ventilation without tracheal intubation. In previous years, several studies have proved its effectiveness and economy, with reduction of complications caused by mechanical ventilation and decrease of mortality [10–12]. BiPAP ventilation has been successfully applied in the treatment of patients who have had pulmonary respiratory failure for a long time [10,11]. The clinical observation showed that hypoxemia of patients who have AMI with pulmonary edema was significantly relieved by BiPAP and the success rate of rescue left HF could be effectively improved [13].
To explore the mechanism of NIPPV in the treatment of HF induced by AMI, we established a rat model of AMI-induced HF. By detecting the serum levels of a series of inflammatory factors and histopathological examination, we showed that noninvasive ventilation is an effective treatment for AMI-induced HF. Therefore, this study aimed to investigate the effects of NIPPV in a rat model of HF due to myocardial infarction.
Material and Methods
ANIMALS AND GROUPS:
Adult male Wistar rats with body weights of 220±20 g were obtained from the Animal Experimental Center of Academy of Military Medical Sciences. This study was approved by the local Ethics Committee. Rats (120) were divided into 3 groups: the NIPPV group (n=40), in which rats received NIPPV after ligation of the coronary artery; the control group (n=40) rats received no treatment after the same operation; we performed only thoracotomy on the sham group (n=40) rats but no ligation of the coronary artery, followed by no treatment.
RAT MODEL OF HF AND TREATMENT:
Rats were anesthetized with 3–4% isoflurane (KeyuanPharma Co., Ltd., Shandong, China) and then placed on the operating table in a supine position with tracheal intubation and attached to a ventilator (ALC-V8, Alcott Biotech Co., Ltd., Shanghai, China), anesthesia machines (VS4153, VisualSonics, Toronto, Canada), and an electrocardiogram (ECG) monitor (ECG-9130P, Nihon Kohden Corporation, Tokyo, Japan) for small animals. The concentration of oxygen used during the operation was 100%. To reduce mortality and improve repeatability, we used a modified coronary artery ligation method to establish a HF model. Specifically, tissue scissors were used to penetrate into the thorax between the left costal margin and the xiphoid process. After the heart was exposed by the nasoscope that entered the chest cavity along the direction of the tissue scissors, the anterior descending artery under the left auricle and the external myocardium were clamped with noninvasive forceps. A large area of pale myocardial surface was observed and the ventricular wall motion was obviously weakened, which was considered to reach the required level of myocardial ischemia. After the myocardial ischemia and ECG meeting the experiment requirements, the left ventricular branch of rats in the NIPPV group and the control group was ligated, whereas the rats in the sham group received no ligation. Finally, the nasoscope was removed and the chest was closed.
From 24 h after the operation, the rats in the NIPPV group were given continuous NIPPV with a small animal ventilator (SAR830-P CWE, Incorporated, Ardmore, PA, USA) for 1 h every day. The tidal volume was 2 mL/100 g (body weight) and the respiratory rate was 60/min. The airway pressure was set at 8–10 cm of H2O with 40% oxygen. Rats in the sham group and the control group received no treatments. Each group of rats was sacrificed on days 3, 5, 7, and 14 after the operation, 10 each time.
ULTRASONIC CARDIOGRAPHY (UCG):
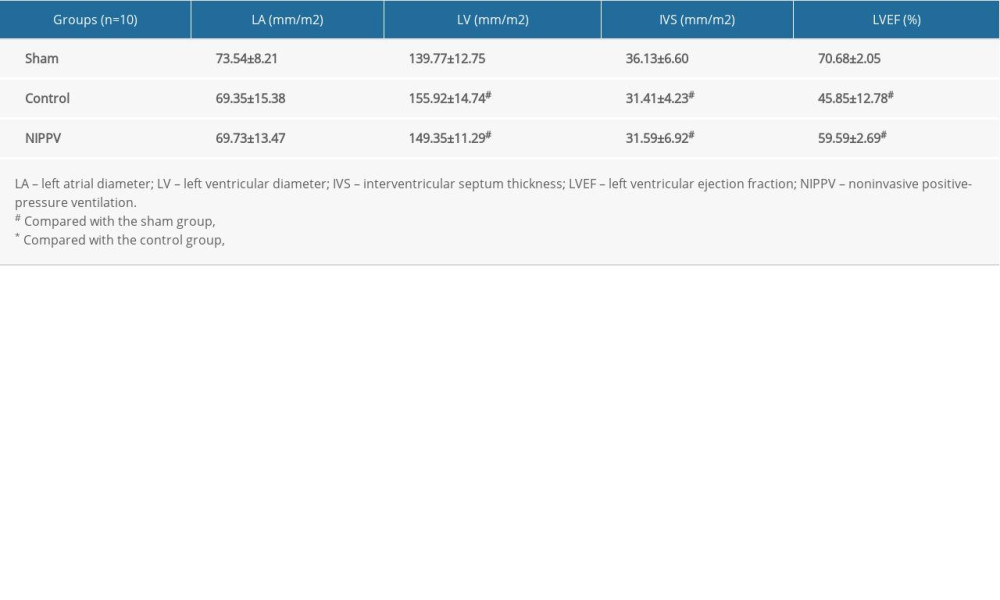
Rats in the 3 groups were anesthetized with isoflurane for UCG (Vevo2100, VisualSonics, Toronto, Canada) on the 14th day after the operation. Left atrial diameter (LA), left ventricular end-diastolic diameter (LV), and interventricular septum thickness (IVS) were measured at the left parasternal long axis section. Results were corrected with body surface area (BSA). BSA (m2)=0.09[body weight (kg)]2/3. LA index=LA/BSA; LV index=LV/BSA; IVS index=IVS/BSA. The left ventricular ejection fraction (LVEF) was measured using M-mode echocardiography. All data were measured 3 times and the average value was taken.
ENZYME-LINKED IMMUNOSORBENT ASSAY (ELISA):
Venous blood was collected on days 3, 5, 7, and 14 after the operation and serum was separated by centrifugation at 3000 revolutions per minute for 10 min. According to the instructions of the ELISA kit, 96-well plates were precoated with rat brain natriuretic peptide (BNP)45 antibody (Abcam, Shanghai, China), mouse HSP70 antibody (Abcam), mouse matrix metalloproteinase (MMP)-2 antibody (R&D Systems, Minneapolis, MN, USA), rat MMP-9 antibody (R&D Systems), and rat tumor necrosis factor (TNF)-α antibody (Abcam). The antibodies were diluted with 1× diluent to prepare 1× antibody for use in the assay procedure. Serum samples were added to the wells and subsequently horseradish peroxidase (HRP)-conjugated antibodies were added, followed by washing. Tetramethylbenzidine substrate was added and incubated at room temperature for 10 min. The absorbance was determined at 450 nm by a microplate absorbance reader (iMark, Bio-Rad Laboratories, Hercules, CA, USA).
HISTOPATHOLOGY STUDY:
Rats in each group were sacrificed on days 3, 5, 7, and 14. The left and right ventricles were opened along the longitudinal axis of the heart and fixed in 10% formalin solution (Leagene Biotechnology, Beijing, China) for 24 h. Four sections perpendicular to the longitudinal axis of the heart were fixed with 4% paraformaldehyde (pH7.3, Leagene Biotechnology). The heart tissue sections then were embedded with paraffin and stained with hematoxylin and eosin (Leagene Biotechnology).
APOPTOSIS ASSAY:
The tissue sections were dewaxed with xylene and subsequently 40 μg/mL of protease K was added to increase cell permeability. The sections were incubated at 37°C for 25 min, followed by washing with phosphate-buffered saline (PBS). Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labeling reaction solution was added according to the manufacturer’s description (in situ cell death detection kit, Roche Life Science, Basel, Switzerland.). The enzyme solution and the label solution in the kit were prepared at a ratio of 1: 9 and added to the samples and then incubated at 37°C for 1 h. After washing with PBS, 30 μL of HRP-labeled converter-peroxidase solution was added onto each sample and then incubated at 37°C for 25 min. Then, diaminobenzidine (DAB) was added as substrate for a color reaction. The DAB solution and the diluent were prepared at a ratio of 1: 10 and added to each sample. After washing with water, the samples were stained with hematoxylin, followed by continuously washing with water for 2 min. The samples were soaked in 95% ethanol for 1 min and then in absolute ethanol for 1 min. Neutral gum was used for sealing. Photos of the fields under the optical microscope were taken. A total of 112 high-power fields of 22 sample slices was selected to count. The percentage of positive cells was calculated by manual labeling and counting.
STATISTICS:
Statistical analysis was performed on the experimental data using SPSS 23.0 software. Measurement data were expressed as mean±standard deviation (χ±
Results
NIPPV IMPROVED THE SURVIVAL OF RATS WITH HF:
Three rats in the control group died 3 days after the operation and 1 died 5 days after the operation. One rat in the NIPPV group died on the third day and 1 died on the fifth day. Compared with the control group, the survival of the NIPPV group was significantly improved (16.67% vs 28.57%,
After the operation, rats in the NIPPV group and the control group both appeared to have symptoms of HF after AMI, such as quick respiration, loss of energy and appetite, and cyanosis of lips and toes. The rats in the sham operation group showed no obvious signs described above. Compared with the NIPPV group, rats in the control group exhibited more severe HF signs and the highest mortality occurred on the third day (8.33% vs 21.42%,
NIPPV IMPROVED CARDIAC STRUCTURE AND FUNCTION OF RATS WITH HF:
As shown in Table 1 and Figure 1A, compared with the sham group, LV of rats in the control group and the NIPPV group were significantly higher and IVS and LVEF of rats were significantly lower (P<0.05), which suggested that the rat model of HF was successful. LA was not significantly different among these 3 groups (P>0.05). Compared with the control group, LV of rats in the NIPPV group was significantly reduced and LVEF was significantly increased (P<0.05). LA and IVS were not significantly different between these 2 groups (P>0.05). BNP, which is mainly produced by ventricles, is known as a biomarker of heart injury, and its increasing concentration in plasma reflects the severity of heart failure [14]. As shown in Figure 1B, the serum BNP45 levels of rats in the control group and NIPPV group were significantly higher than that of rats in the sham group (P<0.01). BNP45 level in the NIPPV group was significantly lower than that in the control group (P<0.05), and decreased continuously on days 3, 5, 7, and 14 (P<0.01) after the operation. Combined with the results of UCG, noninvasive ventilation treatment reduced the BNP level and improved the structure and function of the heart.
EFFECTS OF NIPPV ON SERUM CYTOKINES:
To investigate the potential mechanism of noninvasive ventilation in the treatment of HF, we detected the concentrations of biomarkers in serum. Compared with the sham group, HSP70 levels in the serum of rats in the control and NIPPV groups were significantly higher (P<0.01) after the operation. HSP70 level in the NIPPV group was higher (P<0.05) than that in the control group, and increased continuously on days 3, 5, 7, and 14 (P<0.01) after the operation (Figure 2A). Meanwhile, the levels of MMP-2 (Figure 2B), MMP-9 (Figure 2C), and TNF-α (Figure 2D) in serum of rats in the control group and in the NIPPV group were significantly higher than those in the sham group (P<0.01). The levels of MMP-2 (Figure 2B), MMP-9 (Figure 2C), and TNF-α (Figure 2D) in the NIPPV group were significantly lower than those in the control group (P<0.05), and decreased continuously on days 3, 5, 7, and 14 (P<0.01) after the operation.
EFFECTS OF NIPPV ON CARDIOMYOCYTES:
The histopathology results (Figure 3) showed regular arrangement of myocardium and obvious nucleus in the sham group. There was a small number of lymphocytes and no neutrophils. The cardiomyocytes in the sham group showed no significant change on days 3, 5, 7, and 14 after the operation. In the control group, neutrophil aggregation, muscle cross-striation loss, and nuclear enlargement occurred on day 3. On day 5, the myocardium was necrotic and replaced by fibroblasts. Meanwhile, a large number of lymphocytes aggregated and the nucleus disappeared. On day 7, lymphocyte infiltration dominated in the epicardium and the inflammatory granulation tissue replaced necrotic myocardium. On day 14, myocardial fibrosis and inflammatory cell infiltration were found, dominated by lymphocytes. In the NIPPV group, the muscle cross-striations were arranged disorderly with neutrophils scattered on day 3. On day 5, the muscle cross-striations disappeared and fibroblasts appeared. On day 7, the myocardium was replaced by focal hyperplasia of connective tissue and inflammatory cells were mainly lymphocytes. On day 14, there was no obvious myocardial degeneration and a small amount of inflammatory cell infiltration scattered between the fibrosis was mainly lymphocytes. Figure 4A shows the apoptosis of cardiomyocytes on days 3, 5, 7, and 14 after the operation. The apoptosis rate of myocardial cells in the NIPPV group was significantly lower (P<0.05) compared with the control group (Figure 4B).
Discussion
HF is one of the most severe complications in patients with AMI. The pulmonary venous hypertension and left ventricular end-diastolic pressure increase rapidly in HF, leading to pulmonary interstitial and alveolar edema. The insufficiency of oxygen supply in myocardium further aggravates myocardial infarction [15]. NIPPV was proposed to apply to HF patients with respiratory distress in the 2018 China guidelines for diagnosis and treatment of HF [16]. By increasing the intrathoracic pressure and reducing venous return, a BiPAP ventilator improves the dyspnea and relieves the cardiac preload and pulmonary congestion so as to lower the oxygen consumption of cardiac muscle [17]. However, the improved effects of NIPPV on the structure and function of the heart and the mechanism in the treatment of HF at the molecular level still remain unclear.
The present study established a rat HF model by ligating the left ventricular branch. By selecting the incision between the left costal margin and the xiphoid process, the right thoracic cavity remained intact and the step of squeezing the heart out of the thoracic cavity could be skipped, which shortened the operation time and reduced blood loss. The LVEF of the rats in the control group and the NIPPV group was less than 45% 3 days after the operation, suggesting that the modeling was successful [18]. In addition, BNP, which is mainly secreted by the ventricle and reaches a high plasma concentration in congestive HF, is considered to be a highly sensitive and specific marker of heart injury [19]. The serum levels of BNP45 in the NIPPV group and the control group after the operation were significantly higher than that in the sham group, which also suggested that the model was successfully established. Our findings also demonstrated that BNP45 level in the NIPPV group was significantly lower than that in the control group, suggesting the therapeutic effect of NIPPV on AMI-induced HF.
Ventricular remodeling is promoted by the increased expression of inflammatory factors after myocardial infarction [20]. We hypothesized that NIPPV could reduce the injury of cardiomyocytes by affecting the release of cytokines. HSP70, which is highly expressed in human cardiovascular tissues and atherosclerotic plaques [21], can improve the tolerance of cells to stress by promoting the degradation of denatured proteins and alleviate myocardial IRI [22]. In our study, the levels of HSP70 in the NIPPV group and the control group were significantly higher than that in the sham group, which was consistent with the upregulation of HSP70 in the stress response to AMI. Higher levels of HSP70 were detected in the serum of rats in the NIPPV treatment group with a higher survival rate compared with the control group, suggesting that NIPPV can reduce the incidence and mortality of AMI-induced HF by inducing the high expression of HSP70. Moreover, HSP70 was reported to effectively prevent the damage of oxygen radicals on the membrane structure and function of cardiomyocytes by promoting the synthesis of endogenous peroxidase [23]. Therefore, inducing high expression of HSP70 could be a potential therapy for AMI-induced HF. Reperfusion injury occurs after reperfusion therapy in patients with AMI, which often aggravates tissue injury and the inflammatory response [24].
MMPs, which are released from neutrophils that aggregated in ischemic myocardium, can degrade the extracellular matrix after activation and play a key role in regulating IRI [25]. During IRI, the sudden release of oxygen molecules reactivates mitochondria and the electron transport chain, resulting in a significant increase in reactive oxygen species synthesis and activation of MMP-2 [26]. MMP-2 was proved to promote the degradation of cardiac troponin I and promote apoptosis, and inhibition of MMP-2 was helpful to prevent apoptosis [27]. Previous study also showed that MMP-2 was involved in the process of ventricular remodeling in HF, and is an independent predictive factor of death [28]. MMP-9, a key enzyme to cleave the peptide bond in the helical domain of soluble collagen, is found to be related to the instability of sclerotic plaque and the formation of atherosclerosis [29]. Overexpressed MMP-9 degrades the extracellular matrix of vascular wall cells, resulting in thinning or rupture of coronary atherosclerotic plaque [30]. Garvin et al reported that the level of MMP-9 was independently correlated with the risk for first coronary heart attack [31]. In our study, the levels of MMP-2 and MMP-9 in the NIPPV group and the control group were significantly higher than those in the sham group, which was consistent with the fact that MMP-2 and MMP-9 participate in AMI-induced HF as inflammatory factors. Compared with the control group, the levels of MMP-2 and MMP-9 in the NIPPV group were lower and decreased with time, indicating that NIPPV treatment can reduce the release of inflammatory factors by alleviating tissue hypoxia and ischemia. We believe that long-term application of noninvasive ventilation treatment is beneficial for the inhibition of MMP-2 and MMP-9 activation, so as to delay the process of ventricular remodeling and reduce mortality. TNF-α, mainly produced by activated macrophages or monocytes, is involved in the development of HF by regulating metabolism and immune function and plays roles in myocardial stunning [32]. It has been reported that a high level of TNF-α represents more severe heart failure and poor left ventricular contractility; thus, TNF-α can be applied as an indicator for the degree of HF [33]. The TNF-α levels of rats in the NIPPV group were significantly lower than those in the control group, suggesting that NIPPV treatment can block multiple target molecules in the process of HF by inhibiting the release of inflammatory factor TNF-α.
Myocardial remodeling plays a crucial role in the development of HF. In our study, NIPPV treatment improved the left ventricular systolic function by increasing LVEF. Histologic results showed myocardial degeneration, severe inflammatory infiltration, and necrosis in the control group. Neutrophils dominated in the early stage and lymphocytes dominated in the late stage, and normal myocardial tissue was replaced by fibrotic tissue. In the NIPPV treatment group, myocardial fibrosis was in the earlier stage and formed small foci, and inflammatory infiltration was less severe than that of the control group. Studies have shown that neutrophils undergo morphologic changes to form neutrophil extracellular traps (NETs) under the stimulation of lipopolysaccharide, interleukin-8, TNF, and various pathogens [34]. A thrombus formed by NETs disables movement of the perfused blood into the microcirculation, leading to myocardial stunning and even necrosis [35]. Thus, we speculated that NIPPV treatment inhibited inflammatory factor release and reduced the accumulation of neutrophils to prevent microvascular embolism and lower the possibility of myocardial stunning.
Conclusions
In conclusion, our study demonstrated that NIPPV treatment could alleviate HF after AMI by inducing the high expression of HSP70 and inhibiting the release of inflammatory mediators such as MMP2, MMP9, and TNF-α. NIPPV treatment also effectively reduced neutrophil infiltration and myocardial fibrosis size. NIPPV is an effective treatment for AMI-induced HF; however, better use of NIPPV for patients with AMI to benefit most from reperfusion treatment requires further research.
Figures
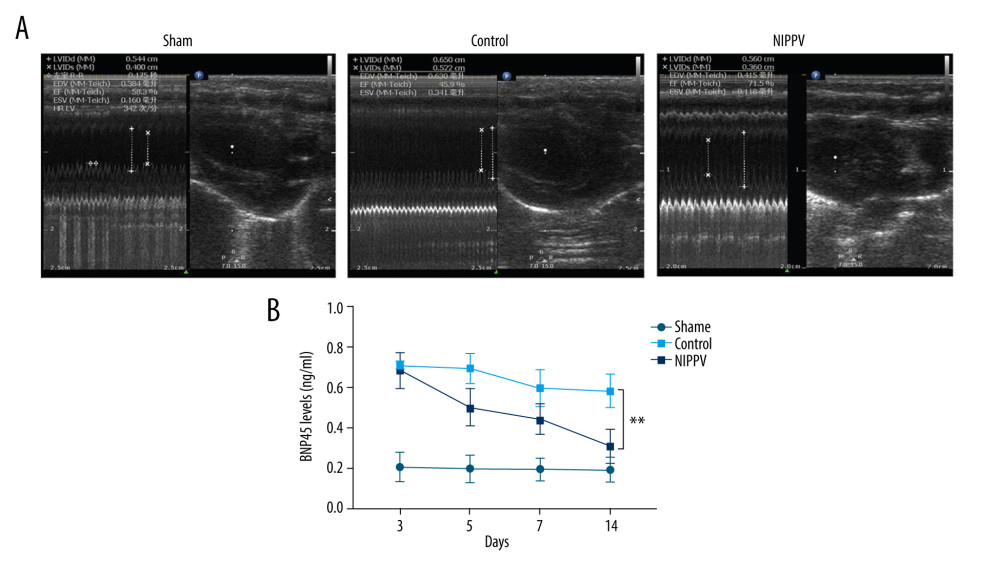 Figure 1. Rat model of heart failure induced by acute myocardial infarction was confirmed by ultrasonic cardiography (UCG) and brain natriuretic peptide (BNP)45 detection. (A) UCG of 3 rats in each group. (B) Levels of BNP45 detected in the sham group, control group, and noninvasive positive-pressure ventilation group. ** P<0.01.
Figure 1. Rat model of heart failure induced by acute myocardial infarction was confirmed by ultrasonic cardiography (UCG) and brain natriuretic peptide (BNP)45 detection. (A) UCG of 3 rats in each group. (B) Levels of BNP45 detected in the sham group, control group, and noninvasive positive-pressure ventilation group. ** P<0.01. 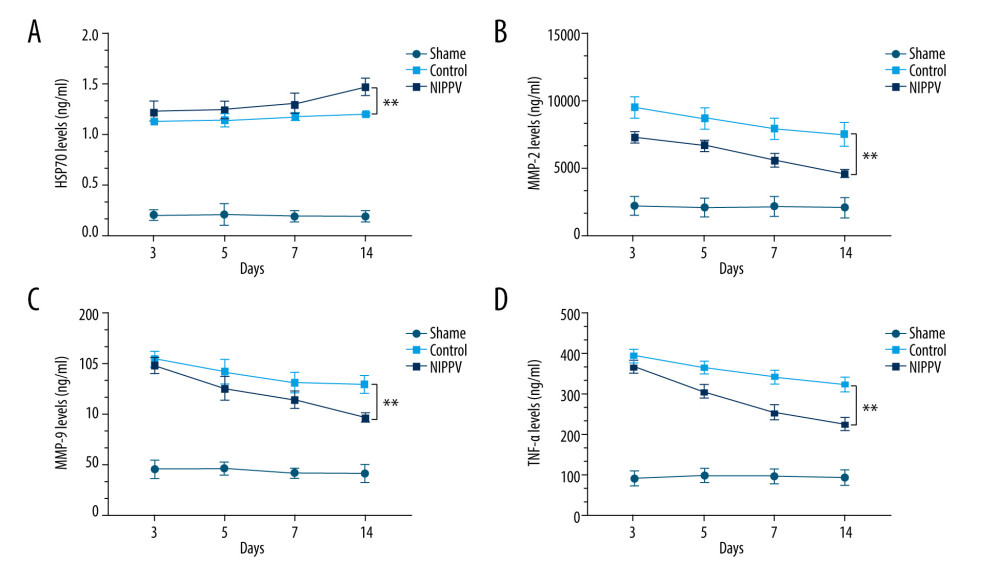 Figure 2. Serum levels of inflammatory factors detected in 10 rats of each group. (A) Heat-shock protein 70, (B) matrix metalloproteinase (MMP)2, (C) MMP9, (D) tumor necrosis factor α. ** P<0.01.
Figure 2. Serum levels of inflammatory factors detected in 10 rats of each group. (A) Heat-shock protein 70, (B) matrix metalloproteinase (MMP)2, (C) MMP9, (D) tumor necrosis factor α. ** P<0.01. 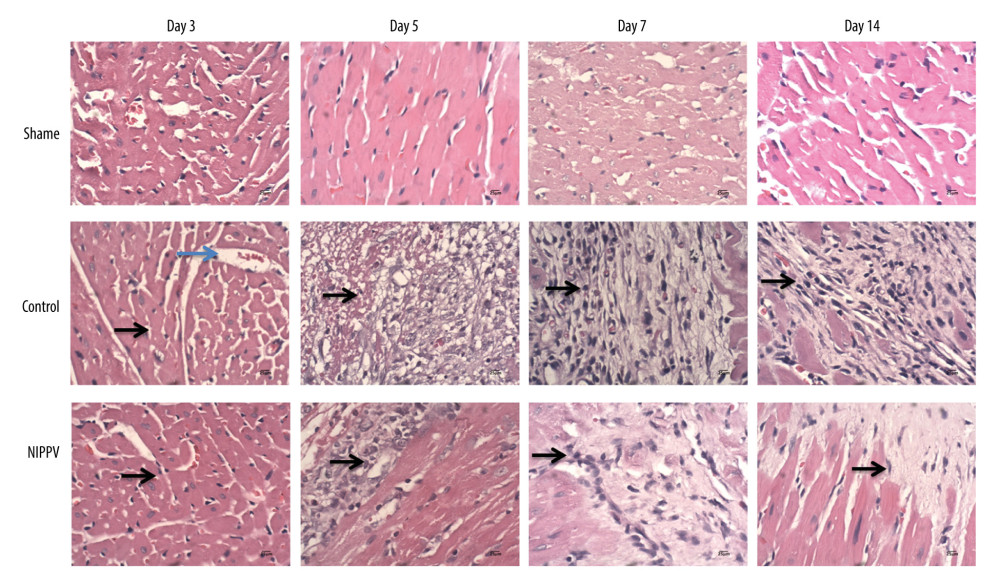 Figure 3. Hematoxylin and eosin (H&E) staining of cardiomyocytes at each time point in 3 rats of each group. No significant change in the cardiomyocytes of the sham group on days 3, 5, 7, and 14. Neutrophil aggregation and myocardial fibrosis were found in the control group. In the noninvasive positive-pressure ventilation group, the neutrophils scattered and myocardial degeneration was not obvious. H&E, ×100. Neutrophils, blue arrow; lymphocytes, black arrows.
Figure 3. Hematoxylin and eosin (H&E) staining of cardiomyocytes at each time point in 3 rats of each group. No significant change in the cardiomyocytes of the sham group on days 3, 5, 7, and 14. Neutrophil aggregation and myocardial fibrosis were found in the control group. In the noninvasive positive-pressure ventilation group, the neutrophils scattered and myocardial degeneration was not obvious. H&E, ×100. Neutrophils, blue arrow; lymphocytes, black arrows. 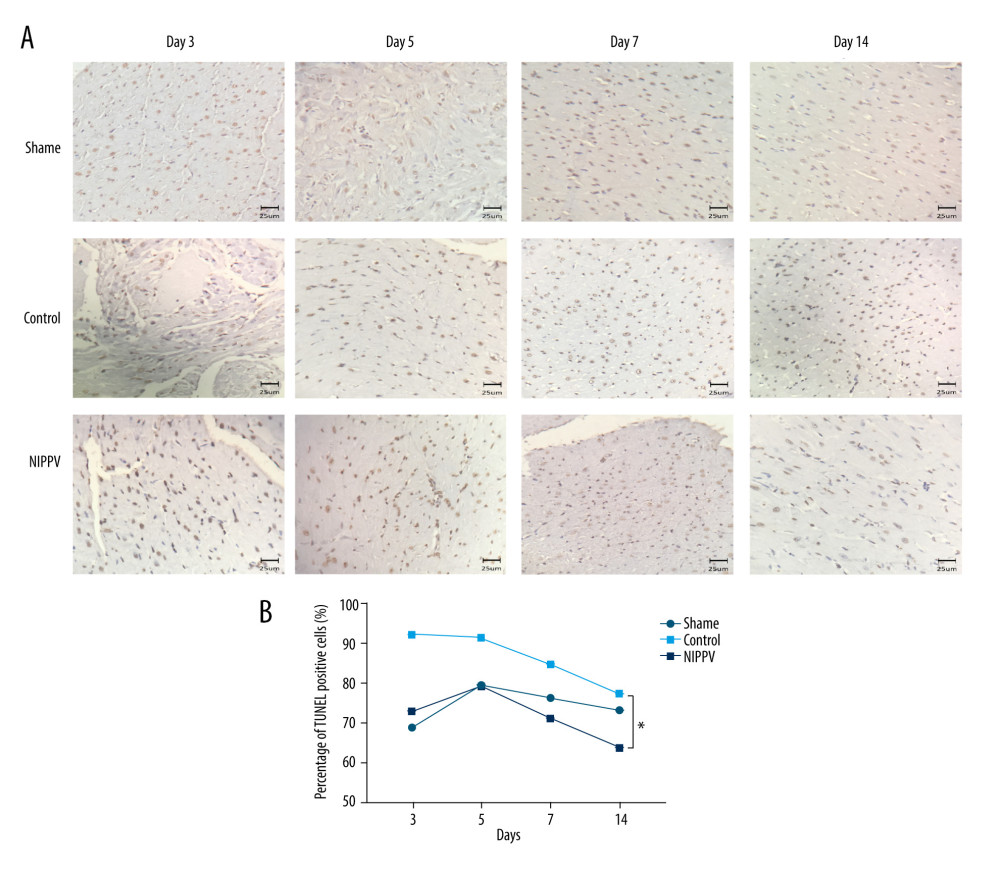 Figure 4. Effects of noninvasive positive-pressure ventilation (NIPPV) on cardiomyocytes. (A) Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labeling staining of cardiomyocytes at each time point in 3 rats of each group. (B) Apoptosis rate of cardiomyocytes in the sham group, control group, and NIPPV group. * P<0.05.
Figure 4. Effects of noninvasive positive-pressure ventilation (NIPPV) on cardiomyocytes. (A) Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labeling staining of cardiomyocytes at each time point in 3 rats of each group. (B) Apoptosis rate of cardiomyocytes in the sham group, control group, and NIPPV group. * P<0.05. References
1. Rogers C, Bush N, Heart failure: Pathophysiology, diagnosis, medical treatment guidelines, and nursing management: Nurs Clin North Am, 2015; 50; 787-99
2. Li J, Li X, Wang Q, ST-segment elevation myocardial infarction in China from 2001 to 2011 (the China PEACE-Retrospective Acute Myocardial Infarction Study): A retrospective analysis of hospital data: Lancet, 2015; 385; 441-51
3. Dhalla NS, Rangi S, Babick AP, Cardiac remodeling and subcellular defects in heart failure due to myocardial infarction and aging: Heart Fail Rev, 2012; 17; 671-81
4. Goel K, Pinto DS, Gibson CM, Association of time to reperfusion with left ventricular function and heart failure in patients with acute myocardial infarction treated with primary percutaneous coronary intervention: A systematic review: Am Heart J, 2013; 165; 451-67
5. Weintraub WS, Spertus JA, Kolm P, Effect of PCI on quality of life in patients with stable coronary disease: N Engl J Med, 2008; 359; 677-87
6. Rentrop KP, Feit F, Reperfusion therapy for acute myocardial infarction: Concepts and controversies from inception to acceptance: Am Heart J, 2015; 170; 971-80
7. Borovnik-Lesjak V, Whitehouse K, Baetiong A, High-dose erythropoietin during cardiac resuscitation lessens postresuscitation myocardial stunning in swine: Transl Res, 2013; 162; 110-21
8. Hida S, Chikamori T, Tanaka H, Postischemic myocardial stunning is superior to transient ischemic dilation for detecting multivessel coronary artery disease: Circ J, 2012; 76; 430-38
9. Abd-Elfattah AS, Tuchy GE, Jessen ME, Hot shot induction and reperfusion with a specific blocker of the es-ENT1 nucleoside transporter before and after hypothermic cardioplegia abolishes myocardial stunning in acutely ischemic hearts despite metabolic derangement: Hot shot drug delivery before hypothermic cardioplegia: J Thorac Cardiovasc Surg, 2013; 146; 961-70.e3
10. Galli JA, Krahnke JS, James Mamary A, Home non-invasive ventilation use following acute hypercapnic respiratory failure in COPD: Respir Med, 2014; 108; 722-28
11. Chau SK, Lee SL, Successful use of BiPAP in infants with congenital myotonic dystrophy: Pediatr Int, 2013; 55; 243-45
12. Gullo CE, de Almeida Zia VA, Vilela-Martin JF, Blockade of renin angiotensin system in heart failure post-myocardial infarction: What is the best therapy?: Recent Pat Cardiovasc Drug Discov, 2014; 9; 28-37
13. Sun T, Wan Y, Kan QEfficacy of noninvasive ventilation on in-hospital mortality in patients with acute cardiogenic pulmonary edema: A meta-analysis: Zhonghua Xin Xue Guan Bing Za Zhi, 2014; 42; 161-68 [in Chinese]
14. Aburaya M, Minamino N, Hino J, Distribution and molecular forms of brain natriuretic peptide in the central nervous system, heart and peripheral tissue of rat: Biochem Biophys Res Commun, 1989; 165; 880-87
15. Gabriel-Costa D, The pathophysiology of myocardial infarction-induced heart failure: Pathophysiology, 2018; 25; 277-84
16. Chinese guidelines for the diagnosis and treatment of heart failure 2018: Zhonghua Xin Xue Guan Bing Za Zhi, 2018; 46; 760-89 [in Chinese]
17. Dursunoglu D, Dursunoglu NNon-invasive mechanical ventilation therapy in patients with heart failure: Anadolu Kardiyol Derg, 2012; 12; 261-68 [in Turkish]
18. Zhang L, Gan ZK, Han LN, Protective effect of heme oxygenase-1 on Wistar rats with heart failure through the inhibition of inflammation and amelioration of intestinal microcirculation: J Geriatr Cardiol, 2015; 12; 353-65
19. Nakagawa Y, Nishikimi T, Kuwahara K, Atrial and brain natriuretic peptides: Hormones secreted from the heart: Peptides, 2019; 111; 18-25
20. Subiela JV, Torres SH, De Sanctis JB, Cardiorespiratory responses, nitric oxide production and inflammatory factors in patients with myocardial infarction after rehabilitation: Nitric Oxide, 2018; 76; 87-96
21. Zhang X, Xu Z, Zhou L, Plasma levels of Hsp70 and anti-Hsp70 antibody predict risk of acute coronary syndrome: Cell Stress Chaperones, 2010; 15; 675-86
22. Xu J, Tang S, Song E, Hsp70 expression induced by co-enzyme Q10 protected chicken myocardial cells from damage and apoptosis under in vitro heat stress: Poult Sci, 2017; 96; 1426-37
23. Reeg S, Jung T, Castro JP, The molecular chaperone Hsp70 promotes the proteolytic removal of oxidatively damaged proteins by the proteasome: Free Radic Biol Med, 2016; 99; 153-66
24. Krzywonos-Zawadzka A, Franczak A, Sawicki G, Multidrug prevention or therapy of ischemia-reperfusion injury of the heart – mini-review: Environ Toxicol Pharmacol, 2017; 55; 55-59
25. Borkham-Kamphorst E, Alexi P, Tihaa L, Platelet-derived growth factor-D modulates extracellular matrix homeostasis and remodeling through TIMP-1 induction and attenuation of MMP-2 and MMP-9 gelatinase activities: Biochem Biophys Res Commun, 2015; 457; 307-13
26. Amantea D, Certo M, Russo R, Early reperfusion injury is associated to MMP2 and IL-1beta elevation in cortical neurons of rats subjected to middle cerebral artery occlusion: Neuroscience, 2014; 277; 755-63
27. Scofield SLC, Dalal S, Lim KA, Exogenous ubiquitin reduces inflammatory response and preserves myocardial function 3 days post-ischemia-reperfusion injury: Am J Physiol Heart Circ Physiol, 2019; 316; H617-28
28. Hognogi LD, Simiti LV, The cardiovascular impact of visfatin – An inflammation predictor biomarker in metabolic syndrome: Clujul Med, 2016; 89; 322-26
29. Smekal A, Vaclavik J, Adipokines and cardiovascular disease: A comprehensive review: Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub, 2017; 161; 31-40
30. Zhou F, Liu D, Ning HF, The roles of p62/SQSTM1 on regulation of matrix metalloproteinase-9 gene expression in response to oxLDL in atherosclerosis: Biochem Biophys Res Commun, 2016; 472; 451-58
31. Garvin P, Jonasson L, Nilsson L, Plasma matrix metalloproteinase-9 levels predict first-time coronary heart disease: An 8-year follow-up of a community-based middle aged population: PLoS One, 2015; 10; e0138290
32. Tian M, Yuan YC, Li JY, Tumor necrosis factor-alpha and its role as a mediator in myocardial infarction: A brief review: Chronic Dis Transl Med, 2015; 1; 18-26
33. Gombos T, Forhecz Z, Pozsonyi Z, Long-term survival and apolipoprotein A1 level in chronic heart failure: Interaction with tumor necrosis factor alpha-308 G/A polymorphism: J Card Fail, 2017; 23; 113-20
34. Baron S, Binenbaum Y, Berger Achituv S, Neutrophil elastase activity as a surrogate marker for neutrophil extracellular trap formation following hematopoietic stem cell transplantation: Biol Blood Marrow Transplant, 2019; 25; 2350-56
35. Twaddell SH, Baines KJ, Grainge C, The emerging role of neutrophil extracellular traps in respiratory disease: Chest, 2019; 156; 774-82
Figures
 Figure 1. Rat model of heart failure induced by acute myocardial infarction was confirmed by ultrasonic cardiography (UCG) and brain natriuretic peptide (BNP)45 detection. (A) UCG of 3 rats in each group. (B) Levels of BNP45 detected in the sham group, control group, and noninvasive positive-pressure ventilation group. ** P<0.01.
Figure 1. Rat model of heart failure induced by acute myocardial infarction was confirmed by ultrasonic cardiography (UCG) and brain natriuretic peptide (BNP)45 detection. (A) UCG of 3 rats in each group. (B) Levels of BNP45 detected in the sham group, control group, and noninvasive positive-pressure ventilation group. ** P<0.01. Figure 2. Serum levels of inflammatory factors detected in 10 rats of each group. (A) Heat-shock protein 70, (B) matrix metalloproteinase (MMP)2, (C) MMP9, (D) tumor necrosis factor α. ** P<0.01.
Figure 2. Serum levels of inflammatory factors detected in 10 rats of each group. (A) Heat-shock protein 70, (B) matrix metalloproteinase (MMP)2, (C) MMP9, (D) tumor necrosis factor α. ** P<0.01. Figure 3. Hematoxylin and eosin (H&E) staining of cardiomyocytes at each time point in 3 rats of each group. No significant change in the cardiomyocytes of the sham group on days 3, 5, 7, and 14. Neutrophil aggregation and myocardial fibrosis were found in the control group. In the noninvasive positive-pressure ventilation group, the neutrophils scattered and myocardial degeneration was not obvious. H&E, ×100. Neutrophils, blue arrow; lymphocytes, black arrows.
Figure 3. Hematoxylin and eosin (H&E) staining of cardiomyocytes at each time point in 3 rats of each group. No significant change in the cardiomyocytes of the sham group on days 3, 5, 7, and 14. Neutrophil aggregation and myocardial fibrosis were found in the control group. In the noninvasive positive-pressure ventilation group, the neutrophils scattered and myocardial degeneration was not obvious. H&E, ×100. Neutrophils, blue arrow; lymphocytes, black arrows. Figure 4. Effects of noninvasive positive-pressure ventilation (NIPPV) on cardiomyocytes. (A) Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labeling staining of cardiomyocytes at each time point in 3 rats of each group. (B) Apoptosis rate of cardiomyocytes in the sham group, control group, and NIPPV group. * P<0.05.
Figure 4. Effects of noninvasive positive-pressure ventilation (NIPPV) on cardiomyocytes. (A) Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick-end labeling staining of cardiomyocytes at each time point in 3 rats of each group. (B) Apoptosis rate of cardiomyocytes in the sham group, control group, and NIPPV group. * P<0.05. Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952