08 March 2021: Clinical Research
Pleural Effusion Is Associated with Severe Renal Dysfunction in Patients with Acute Pancreatitis
Quan-Xiang Zeng1ABDG, Kai-Lin Jiang2ACDE, Zhen-Hua Wu1DEF, Dong-Liang Huang1B, Ye-Sheng Huang1B, Hao-Wen Zhuang2C, Hao-Jie Zhong34ACDEF*DOI: 10.12659/MSM.928118
Med Sci Monit 2021; 27:e928118
Abstract
BACKGROUND: Renal dysfunction is a leading cause of death in patients with acute pancreatitis (AP) and often occurs later than respiratory complications. Whether respiratory complications can predict renal impairment remains unclear. The aim of this study was to investigate the association between pleural effusion and renal dysfunction in AP.
MATERIAL AND METHODS: Medical records were reviewed from individuals who were hospitalized with AP from January 1, 2015 to December 31, 2019. The patients were divided into 2 groups, based on the presence or absence of pleural effusion on admission. Disease severity, renal function parameters, and outcomes were compared between the 2 groups.
RESULTS: A total of 222 patients were enrolled, 25 of whom had pleural effusion on admission and 197 who did not. Patients with AP who had pleural effusion had more serious illness (higher incidences of pancreatic inflammation, pancreatic fluid collection, and moderate-to-severe AP; worse Bedside Index for Severity in Acute Pancreatitis score; and a higher modified computed tomography severity index [all P<0.05]) plus worse outcomes (higher incidences of ventilation and vasopressor use [both P<0.05]). Moreover, patients with pleural effusion had a higher level of blood urea nitrogen and lower estimated glomerular filtration rate (both P<0.05). After adjustment for potential confounders, pleural effusion was a risk factor for renal failure in patients with AP (odds ratio 6.32, 95% confidence interval 1.08–36.78, P=0.040).
CONCLUSIONS: Pleural effusion is associated with severe renal dysfunction in AP. Therefore, efforts should be made to improve early recognition and timely treatment of renal failure by closely monitoring renal function in patients with AP and pleural effusion on admission.
Keywords: Pleural Effusion, renal insufficiency, Incidence, Kidney Diseases, Odds Ratio, Risk Factors, Severity of Illness Index, Tomography, X-Ray Computed
Background
Acute pancreatitis (AP) is the most common gastrointestinal cause of hospital admission and the fifth leading cause of in-hospital deaths; its incidence is continuously increasing [1,2]. AP-related organ failure (respiratory, cardiovascular, and renal) is a core indicator of disease severity and accounts for almost all mortality in patients with the condition [3,4]. Renal dysfunction is frequently associated with AP [5] and is a common complication of it, resulting from increased vascular permeability and hypovolemia, intravascular coagulation, and direct nephrotoxic effects, caused by the release of activated enzymes and proteases during AP [6]. The incidence of renal failure (RF) in patients with AP ranges from 14% to 44% [7,8], and although acute RF usually develops after the failure of other organs, it is associated with prolonged hospital stays and a 10-fold higher mortality rate [6,9–11]. Because renal dysfunction is not always obvious in the early stages of AP but leads to a significantly higher risk of death, it is very important to identify predictive factors for it to ensure that supportive therapies are initiated early in the disease course.
Imaging is a requirement for AP diagnosis, and with it, chest lesions including pleural effusion, pneumonia, and atelectasis can be detected in the early stages of the illness. Pleural effusion is found in up to 50% patients with AP [12,13] and is an independent predictor of AP severity [14]. In addition, pleural effusion can reduce cardiac output and produce hypoxemia, which in turn can lead to renal injury, manifested as a decreased glomerular filtration rate (GFR) and renal tubular epithelial cell damage [7]. Moreover, respiratory complications occur at an early stage of AP and are prolonged, while renal complications occur later, implying a potential role for respiratory complications in predicting subsequent renal injury [8]. Although there have been some studies of the association between pleural effusion and AP severity [14,15], whether pleural effusion can predict renal function dysfunction remains unclear.
The aim of this study was to investigate the association between pleural effusion and renal dysfunction in AP.
Material and Methods
ETHICS APPROVAL:
Ethics approval was obtained from the Institutional Review Board (IRB) of Maoming People’s Hospital, Maoming, China (No. 2020MI-141-01). Because of the retrospective design of the study, the IRB waived the need for informed consent.
PARTICIPANTS:
In this study, all adult inpatients with AP who were treated at Maoming People’s Hospital from January 1, 2015 to December 31, 2019 were eligible for enrollment. The exclusion criteria were a history of pancreatitis, pregnancy, or lack of important medical data.
DATA COLLECTION:
The following data from enrolled patients were obtained from medical records in the hospital database: demographic information (age and sex); alcohol and smoking status; history of comorbidities; AP etiology (gallstones, alcohol, post-endoscopic retrograde cholangiopancreatography, medications, and idiopathic); physiological variables (heart rate, blood pressure, respiratory rate, temperature, and mental status); laboratory parameters (serum amylase, alanine aminotransferase, aspartate transaminase, total bilirubin, triglycerides, blood glucose, white blood cell [WBC] count, hematocrit, platelet count, blood urea nitrogen [BUN], serum creatinine, arterial pH, partial pressure of oxygen, partial pressure of carbon dioxide, serum potassium, serum sodium, and serum calcium); radiologic findings; and clinical outcomes (use of a ventilator, use of a vasopressor, Intensive Care Unit [ICU] admission, hospital stay, and mortality).
DEFINITIONS:
In accordance with the revised Atlanta classification, diagnosis of AP required at least 2 of the following 3 diagnostic features: persistent abdominal pain, serum lipase or amylase activity at least 3 times the upper limit of the normal range, and characteristic findings on abdominal imaging [3]. Pleural effusion was diagnosed as blunting of the costophrenic or cardiophrenic angle confirmed by computed tomography (CT) [12]. Alcoholism was defined as ingestion of >30 g/day of alcohol in men and >20 g/day in women. Hypocalcemia was defined as a serum calcium level <2.12 mmol/L [16]. RF was defined as creatinine ≥176.8 μmol/L (2.0 mg/dL) [17]. Severity of AP was stratified into 3 categories – mild, moderately severe, and severe – based on the revised Atlanta criteria [3]. Charlson Comorbidity Index (CCI) [18], estimated GFR (eGFR) [19], modified computed tomography severity index (CTSI) [20], Acute Physiology And Chronic Health Evaluation II (APACHE II) score [21], multiple organ dysfunction syndrome (MODS) score [22], and Bedside Index for Severity in Acute Pancreatitis (BISAP) score [23] were calculated as previously described.
STATISTICAL ANALYSIS:
Normally distributed continuous variables were presented as mean±standard deviation and those with skewed distribution as median and interquartile ranges. Categorical variables were presented as frequencies and percentages. Continuous data were compared using the t test or the Mann-Whitney U test, while categorical variables were compared using the chi-square test or Fisher exact test, as appropriate. To assess associations between pleural effusion and disease severity and RF and outcomes of AP, multiple logistic regression analysis, using the backward conditional method, was applied to adjust for potential confounders (age, sex, hematocrit, WBC count, blood glucose, serum triglycerides, and hypocalcemia) [24–27]; odds ratios (ORs) and 95% confidence interval (95%CIs) also were calculated. All data were processed using SPSS software version 22.0 (IBM Corp., Armonk, New York, United States). Results were considered significant at P<0.05.
Results
PATIENT CHARACTERISTICS:
A total of 356 patients with AP were diagnosed from January 2015 to December 2019. Of them, 134 were excluded, and 222 were finally enrolled in the present study. The patients were divided into 2 groups – pleural effusion (25) and non-pleural effusion (197) – based on their imaging results at admission. Information on demographic characteristics and AP etiology is presented in Table 1. There was a higher incidence of hypocalcemia in the pleural effusion group than in the non-pleural effusion group (44.00% vs 19.80%, P=0.007) (Table 2); however, no significant intergroup differences were observed with respect to other laboratory parameters.
DISEASE SEVERITY:
On comparing factors associated with disease severity between the 2 groups, we found that the incidence of pancreatic inflammation (92.00% vs 70.56%, P=0.023); pancreatic fluid collection (36.00% vs 13.20%, P=0.008); moderate-to-severe AP (52.00% vs 18.27%, P<0.001); BISAP score (2.00; range, 1.00–3.00 vs 1.00; range, 0.00–1.00, P<0.001); and modified CTSI scores (4.00; range, 4.00–6.00 vs 2.00; range, 0.00–2.00, P<0.001) were significantly higher in the pleural effusion than in the non-pleural effusion group (Table 3). Further, patients with pleural effusion rather without pleural effusion also had higher APACHE II scores (6.00; range, 3.50–10.00 vs 5.00; range, 3.00–7.00, P=0.182) and MODS scores (1.00; range, 1.00–3.00 vs 1.00; range, 0.00–2.00, P=0.077), but these differences were not statistically significant. There was no difference in the incidence of systemic inflammatory response syndrome between the 2 groups, and incidence of pancreatic necrosis was negligible in both groups.
RENAL FUNCTION PARAMETERS:
A significantly higher level of BUN (5.16; range, 3.91–7.81 vs 3.98; range, 3.14–5.36 mmol/L, P=0.003) and lower eGFR (53.61; range, 46.11–70.87 vs 66.76; range, 55.51–80.34 mL/min×1.73 m2, P=0.044) were detected in the pleural effusion group than in the non-pleural effusion group. In addition, patients with AP who had pleural effusion had higher levels of serum creatinine (93.35; range, 78.85–112.73 vs 84.10; range, 72.95–98.00 μmol/L, P=0.092) and a higher incidence of RF (12.00% vs 3.55%, P=0.131) than those without pleural effusion, but these differences were not significant (Table 4).
OUTCOMES:
Outcome measures including the incidences of use of ventilators (12.00% vs 0.51%, P=0.005) and vasopressors (8.00% vs 0%, P=0.012) were significantly higher in the pleural effusion than in the non-pleural effusion group; however, the incidence of ICU admission and hospital length of stay did not differ significantly between the 2 groups. Mortality rates were very low in both groups, with only a single death in the pleural effusion group and none in the non-pleural effusion group (Table 5).
MULTIPLE LOGISTIC REGRESSION ANALYSIS:
Multiple logistic regression analysis was used to explore whether pleural effusion was a risk factor for severe AP, RF, or poor outcomes. Patients with pleural effusion had a higher risk of pancreatic inflammation (OR 4.80, 95%CI 1.05–21.95, P=0.043); pancreatic fluid collection (OR 4.15, 95%CI 1.59–10.84, P=0.004); moderate-to-severe AP (OR 5.53, 95%CI 2.15–14.24, P<0.001); RF (OR 6.32, 95%CI 1.08–36.78, P=0.040); and use of ventilation (OR 25.36, 95%CI 2.52–255.66, P=0.006) (Table 6).
Discussion
In the present study, the incidence of pleural effusion in patients with AP was 11.26% on admission, which was consistent with the previously described range of 4% to 20% [28]. In addition, similar to previous studies [14,29], our data showed that pleural effusion was a risk factor for more severe disease (pancreatic inflammation, pancreatic fluid collection, and moderate-to-severe AP) and worse outcomes (use of ventilation) in patients with AP. However, considering that pancreatic necrosis, ICU admission, and death were rare in our study, associations between pleural effusion and these variables were difficult to assess.
Complications are predictors of disease severity and worse prognosis for AP [30,31]. Some prior studies have shown that pleural effusion is associated with complications of AP. Maruti et al reported that the prevalence of respiratory failure was higher in patients with AP who had pleural effusion on admission than in those without pleural effusion [28]. In addition, Giorgio et al found that pleural effusion on admission was a risk factor for pancreatic necrosis, which is a known local and lethal complication [32]. Moreover, a recent study suggested that the volume of pleural effusion was also a specific indicator for predicting organ failure in AP [14]. Nevertheless, the association between pleural effusion and renal impairment is unclear. Given that renal dysfunction is one of the most common complications and a leading cause of death in AP and the symptoms of renal dysfunction are not obvious in early-stage illness, increased knowledge about the risk factors for renal dysfunction in AP will help clinicians select the appropriate level of care and improve the prognosis for patients with this illness [6,9,33].
Our results suggest that renal function is impaired (higher level of BUN and lower eGFR) in patients with AP who have pleural effusion. In addition, the incidence of RF was higher in patients with than without pleural effusion, although the difference was not statistically significant, which may be because of potential confounders between the 2 groups and the small sample size in the present study. Therefore, a multiple logistic regression analysis was performed to adjust for potential confounders. We found that pleural effusion was an independent risk factor for RF. Thus, to facilitate early recognition and timely treatment of renal dysfunction and even RF, renal function should be closely monitored in patients with AP who have pleural effusion on admission. To the best of our knowledge, this is the first study to assess the association between pleural effusion and impairment of renal function in patients with AP and to show the predictable effect of pleural effusion on RF in AP.
There are some possible explanations for the results of the present study. First, pleural effusion can cause increased intrathoracic pressure, which may subsequently lead to diminished cardiac output and reduced renal artery perfusion [7]. Decreased renal arterial blood supply is known to play a critical role in causing acute kidney injury in AP [6]. Second, pleural effusion also can lead to hypoxemia, secondary to decreased residual lung capacity. In this circumstance, renal tubular epithelial cells, which are sensitive to hypoxemia, are damaged. In addition, hypoxemia can cause renal vessel constriction, which eventually can lead to renal ischemic injury [6]. Third, pleural effusion is an indicator of disease severity in patients with AP. Hence, patients with pleural effusion may have higher levels of nephrotoxic substances, such as inflammatory cytokines, enzymes, and proteases, which can subsequently contribute to impaired renal function [6].
Our study has some limitations. First, because it was retrospective, the association between the volume of pleural effusion and impairment in renal function was difficult to assess. Second, some potential confounders, such as use of diuretics and volume of water intake, were not considered; thus, the assessment of renal function may have been somewhat affected by these factors. Third, the present study was single-center study and the sample size was limited. Therefore, our conclusions should be interpreted with caution; future studies with a larger sample size are needed to validate our findings.
Conclusions
Pleural effusion is associated with severe renal dysfunction, including high levels of BUN, low eGFR, and a high risk for RF in patients with AP. Therefore, renal function should be closely monitored in patients with AP who have pleural effusion on admission so that RF can be identified early and treated in a timely fashion.
Tables
Table 1. Patient characteristics.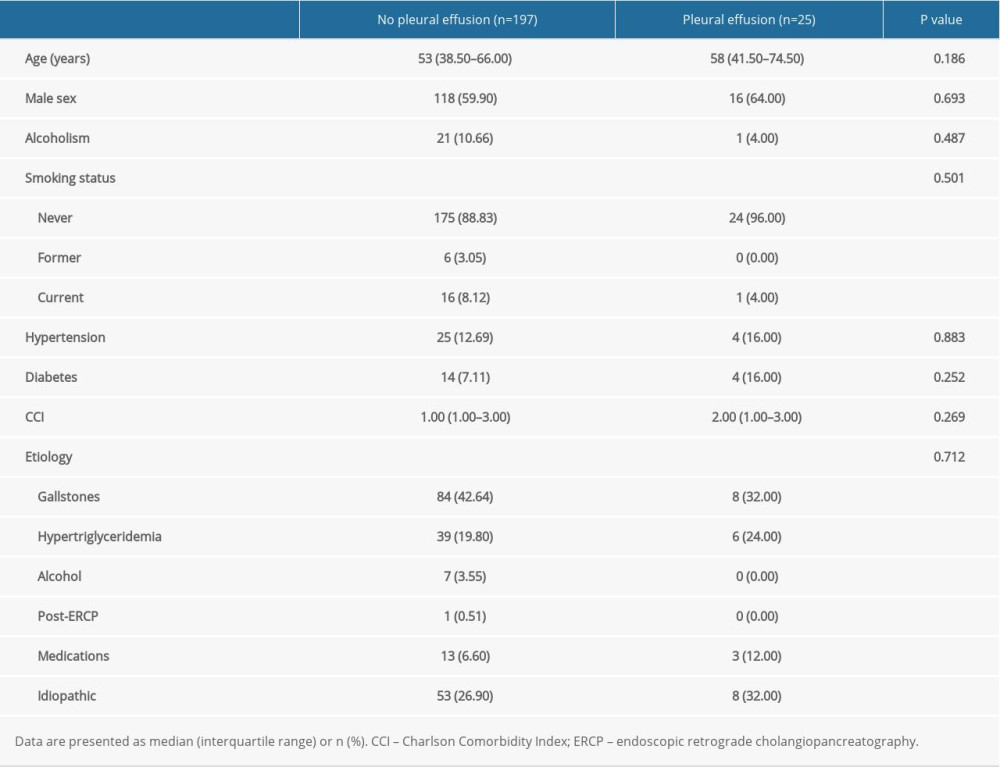 Table 2. Comparison of laboratory parameters between patients without and with pleural effusion.
Table 2. Comparison of laboratory parameters between patients without and with pleural effusion.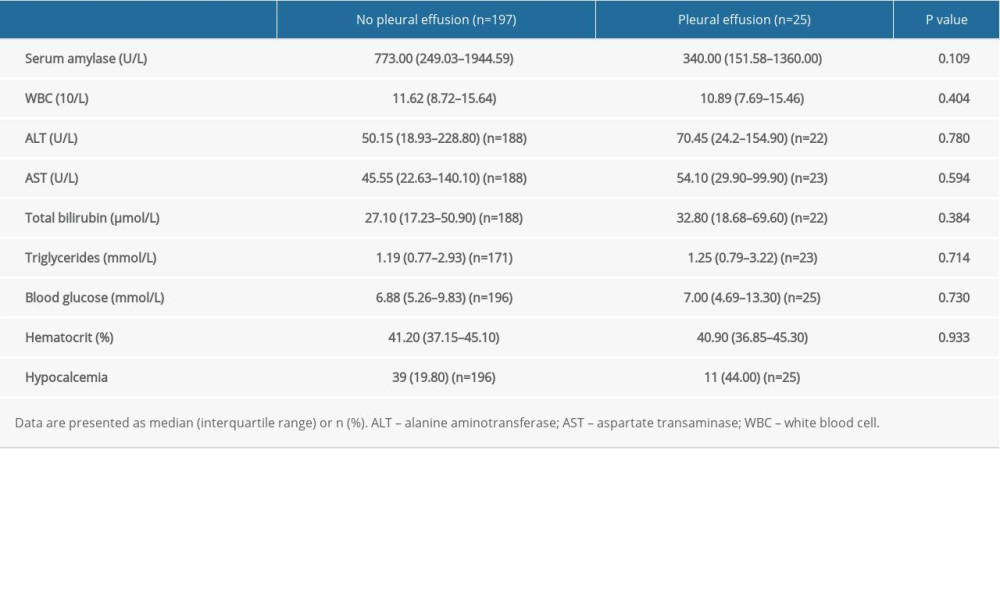 Table 3. Comparison of disease severity between patients without and with pleural effusion.
Table 3. Comparison of disease severity between patients without and with pleural effusion.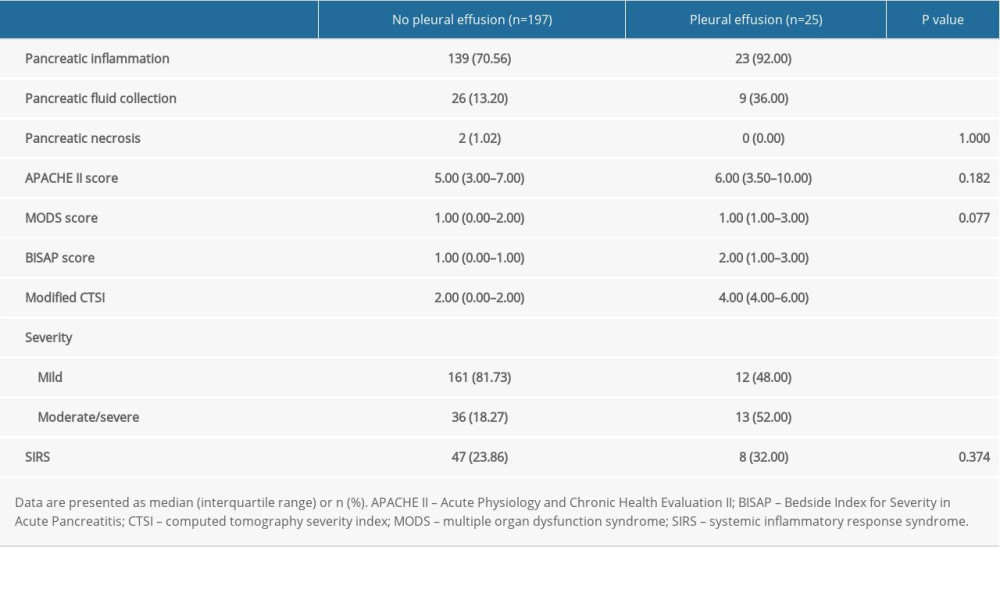 Table 4. Comparison of renal function parameters between patients without and with pleural effusion.
Table 4. Comparison of renal function parameters between patients without and with pleural effusion.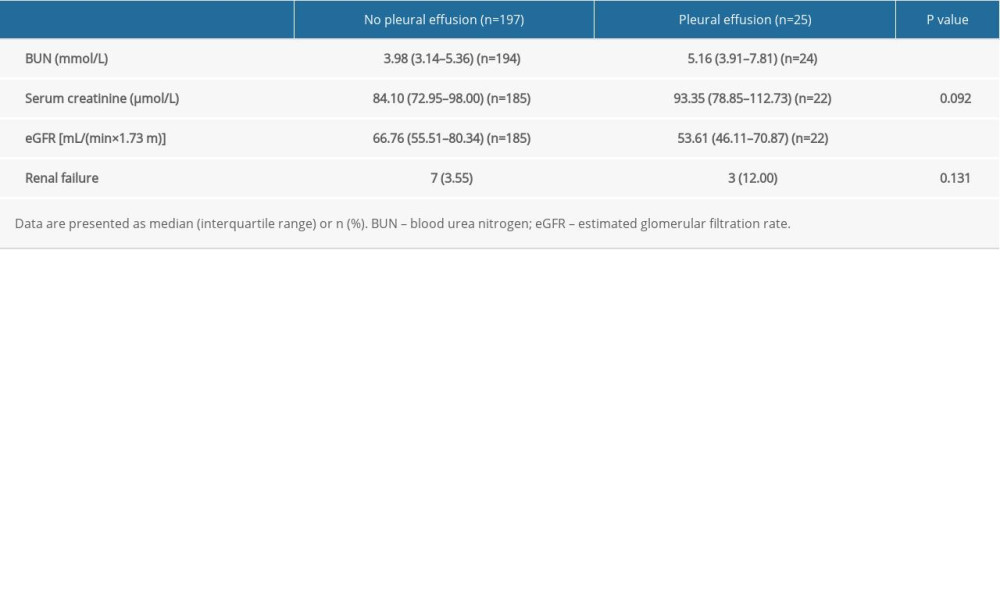 Table 5. Comparison of outcome parameters between patients without and with pleural effusion.
Table 5. Comparison of outcome parameters between patients without and with pleural effusion.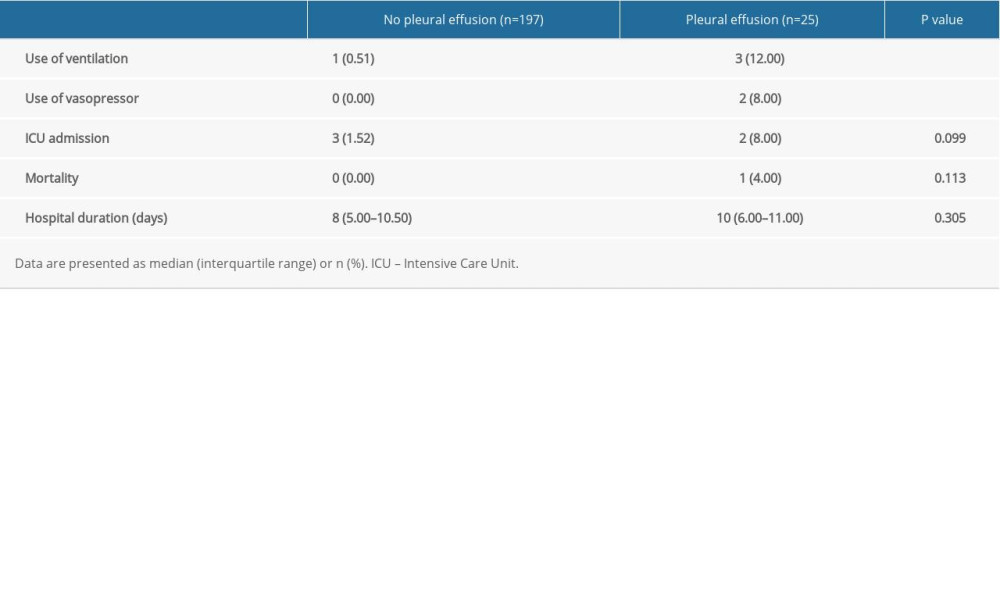 Table 6. Logistic regression analyses of pleural effusion as a risk factor for severe acute pancreatitis, renal failure, and poor outcomes.
Table 6. Logistic regression analyses of pleural effusion as a risk factor for severe acute pancreatitis, renal failure, and poor outcomes.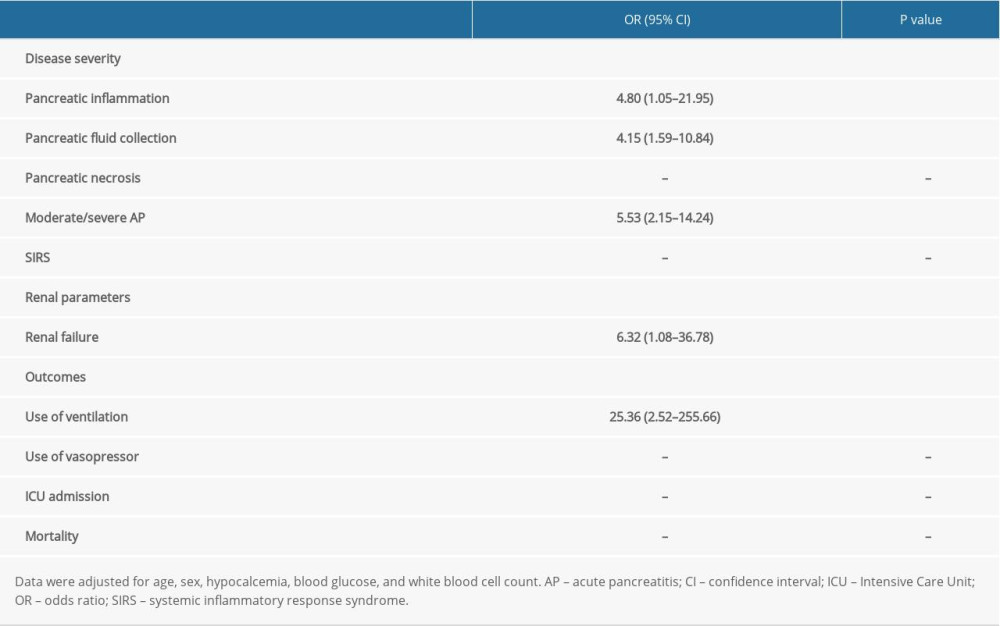
References
1. Lankisch PG, Apte M, Banks PA, Acute pancreatitis: Lancet, 2015; 386(9988); 85-96
2. Forsmark CE, Vege SS, Wilcox CM, Acute pancreatitis: N Engl J Med, 2016; 375(20); 1972-81
3. Banks PA, Bollen TL, Dervenis C, Classification of acute pancreatitis – 2012: Revision of the Atlanta classification and definitions by international consensus: Gut, 2013; 62(1); 102-11
4. Garg PK, Singh VP, Organ failure due to systemic injury in acute pancreatitis: Gastroenterology, 2019; 156(7); 2008-23
5. Puca E, Harxhi A, Pipero P, Pancreatitis in patients with hemorrhagic fever with renal syndrome: A five-year experience: J Infect Dev Ctries, 2017; 11(11); 900-3
6. Nassar TI, Qunibi WY, AKI associated with acute pancreatitis: Clin J Am Soc Nephrol, 2019; 14(7); 1106-15
7. Li H, Qian Z, Liu Z, Risk factors and outcome of acute renal failure in patients with severe acute pancreatitis: J Crit Care, 2010; 25(2); 225-29
8. Schepers NJ, Bakker OJ, Besselink MG, Impact of characteristics of organ failure and infected necrosis on mortality in necrotising pancreatitis: Gut, 2019; 68(6); 1044-51
9. Gougol A, Dugum M, Dudekula A, Clinical outcomes of isolated renal failure compared to other forms of organ failure in patients with severe acute pancreatitis: World J Gastroenterol, 2017; 23(29); 5431-37
10. Lin HY, Lai JI, Lai YC, Acute renal failure in severe pancreatitis: A population-based study: Ups J Med Sci, 2011; 116(2); 155-59
11. Kes P, Vucicevic Z, Ratkovic-Gusic I, Acute renal failure complicating severe acute pancreatitis: Ren Fail, 1996; 18(4); 621-28
12. Kumar P, Gupta P, Rana S, Thoracic complications of pancreatitis: JGH Open, 2019; 3(1); 71-79
13. Raghuwanshi S, Gupta R, Vyas MM, CT Evaluation of acute pancreatitis and its prognostic correlation with CT severity index: J Clinical Diagn Res, 2016; 10(6); TC06-11
14. Peng R, Zhang L, Zhang ZM, Chest computed tomography semi-quantitative pleural effusion and pulmonary consolidation are early predictors of acute pancreatitis severity: Quant Imaging Med Surg, 2020; 10(2); 451-63
15. Heller SJ, Noordhoek E, Tenner SM, Pleural effusion as a predictor of severity in acute pancreatitis: Pancreas, 1997; 15(3); 222-25
16. Pepe J, Colangelo L, Biamonte F, Diagnosis and management of hypocalcemia: Endocrine, 2020; 69(3); 485-95
17. Wu C, Ke L, Tong Z, Hypertriglyceridemia is a risk factor for acute kidney injury in the early phase of acute pancreatitis: Pancreas, 2014; 43(8); 1312-16
18. Charlson ME, Pompei P, Ales KL, A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation: J Chronic Dis, 1987; 40(5); 373-83
19. Ma YC, Zuo L, Chen JH, Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease: J Am Soc Nephrol, 2006; 17(10); 2937-44
20. Mortele KJ, Wiesner W, Intriere L, A modified CT severity index for evaluating acute pancreatitis: Improved correlation with patient outcome: Am J Roentgenol, 2004; 183(5); 1261-65
21. Knaus WA, Draper EA, Wagner DP, APACHE II: A severity of disease classification system: Crit Care Med, 1985; 13(10); 818-29
22. Marshall JC, Cook DJ, Christou NV, Multiple organ dysfunction score: A reliable descriptor of a complex clinical outcome: Crit Care Med, 1995; 23(10); 1638-52
23. Wu BU, Johannes RS, Sun X, The early prediction of mortality in acute pancreatitis: A large population-based study: Gut, 2008; 57(12); 1698-703
24. Wu BU, Johannes RS, Sun X, Early changes in blood urea nitrogen predict mortality in acute pancreatitis: Gastroenterology, 2009; 137(1); 129-35
25. Koutroumpakis E, Wu BU, Bakker OJ, Admission hematocrit and rise in blood urea nitrogen at 24 h outperform other laboratory markers in predicting persistent organ failure and pancreatic necrosis in acute pancreatitis: A post hoc analysis of three large prospective databases: Am J Gastroenterol, 2015; 110(12); 1707-16
26. Ruiz-Rebollo ML, Munoz-Moreno MF, Clinical relationship between serum triglycerides and acute pancreatitis: Pancreatology, 2020; 20(4); 785-86
27. Carvalho JR, Fernandes SR, Santos P, Acute pancreatitis in the elderly: A cause for increased concern?: Eur J Gastroenterol Hepatol, 2018; 30(3); 337-41
28. Raghu MG, Wig JD, Kochhar R, Lung complications in acute pancreatitis: JOP, 2007; 8(2); 177-85
29. Marchi A, Caimmi S, Caimmi D, Recurrent pleural effusion as an unusual presentation of acute pancreatitis in children: Pancreas, 2011; 40(2); 321-23
30. Hines OJ, Pandol SJ, Management of severe acute pancreatitis: BMJ, 2019; 367; l6227
31. Lee PJ, Papachristou GI, New insights into acute pancreatitis: Nat Rev Gastroenterol Hepatol, 2019; 16(8); 479-96
32. Talamini G, Uomo G, Pezzilli R, Serum creatinine and chest radiographs in the early assessment of acute pancreatitis: Am J Surg, 1999; 177(1); 7-14
33. Zhou J, Li Y, Tang Y, Effect of acute kidney injury on mortality and hospital stay in patient with severe acute pancreatitis: Nephrology (Carlton), 2015; 20(7); 485-91
Tables
 Table 1. Patient characteristics.
Table 1. Patient characteristics. Table 2. Comparison of laboratory parameters between patients without and with pleural effusion.
Table 2. Comparison of laboratory parameters between patients without and with pleural effusion. Table 3. Comparison of disease severity between patients without and with pleural effusion.
Table 3. Comparison of disease severity between patients without and with pleural effusion. Table 4. Comparison of renal function parameters between patients without and with pleural effusion.
Table 4. Comparison of renal function parameters between patients without and with pleural effusion. Table 5. Comparison of outcome parameters between patients without and with pleural effusion.
Table 5. Comparison of outcome parameters between patients without and with pleural effusion. Table 6. Logistic regression analyses of pleural effusion as a risk factor for severe acute pancreatitis, renal failure, and poor outcomes.
Table 6. Logistic regression analyses of pleural effusion as a risk factor for severe acute pancreatitis, renal failure, and poor outcomes. In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








