14 August 2020: Clinical Research
A Retrospective Study of Surgical Correction for Spinal Deformity with and without Osteotomy to Compare Outcome Using Intraoperative Neurophysiological Monitoring with Evoked Potentials
Jian ChenDEF, Jing-fan YangBCF, Yao-long DengBCF, Xie-xiang ShaoBCD, Zi-fang HuangABCDE, Jun-lin YangFGDOI: 10.12659/MSM.925371
Med Sci Monit 2020; 26:e925371
Abstract
BACKGROUND: This study aimed to evaluate the effects of different combined evoked potentials monitoring modes for non-osteotomy and osteotomy surgery of spinal deformity, and to select individualized modes for various surgeries.
MATERIAL AND METHODS: We retrospectively reviewed a total of 188 consecutive cases undergoing spinal deformity correction. All patients were classified into 2 cohorts: non-osteotomy (Group A) and osteotomy (Group B). According to intraoperative evoked potential monitoring mode, Group A was divided into 2 sub-groups: A1 [spinal somatosensory evoked potential (SSEP)/motor evoked potential (MEP), n=67)] and A2 [SSEP/MEP/descending neurogenic evoked potential (DNEP), n=52]. Group B was classified as B1 (SSEP/MEP, n=27) and B2 (SSEP/MEP/DNEP, n=42). The demographics, surgical parameters, and evoked potential events of different combined monitoring modes were analyzed within each group.
RESULTS: The baselines of SSEP/MEP/DNEP in all cases were elicited successfully. Three cases with evoked potential (EP) events (2 with MEP changes and 1 with SSEP/MEP change) were noted in Group A1 and 1 with SSEP change in Group A2, with no neurological complications. Thirteen cases in Group B1 were positive for MEP intraoperatively, including 16 EP events (13 with MEP change and 3 with both SSEP+MEP changes), with no neural complications. In Group B2, 15 cases had 21 EP events, including 12 with MEP change and 2 with SSEP+MEP changes, with no complications. Postoperative neurological complications were observed in 5 of the 7 cases with SS4EP/DNEP changes.
CONCLUSIONS: Intraoperative simultaneous SSEP/MEP can effectively reflect neurological function in non-osteotomy spinal surgery patients. Simultaneous SSEP/MEP/DNEP can effectively avoid the unnecessary interference by false-positive results of MEP during osteotomy.
Keywords: Evoked Potentials, Osteotomy, Scoliosis, Adolescent, Child, Evoked Potentials, Somatosensory, Intraoperative Care, Monitoring, Physiologic, Spinal Diseases, young adult
Background
With the development of spinal surgery technology, internal fixation of the posterior pedicle screw-rod system has gradually become the criterion standard for posterior correction of spinal deformities [1,2]. Nonetheless, the complex screw placement in osteotomy and orthopedic procedures remarkably increases the risks of neurological injury. According to the literature, the incidence rate of neurological complications is 4.0~21.2% [3–6]. Intraoperative neurophysiological monitoring (IONM), which is suggested to be a good predictor of imminent spinal cord injury, helps to reduce risks of neurological complications, and it has become an important real-time monitoring technique for nerve function in spinal orthopedic surgery [7]. At present, several IONM techniques are applied in scoliosis surgery, such as motor evoked potentials (MEP), somatosensory evoked potentials (SEP), electromyogram (EMG), descending neurogenic evoked potentials (DNEP), and spinal cord evoked potentials (SCEPS) [8]. Based on these techniques, a variety of single or combined IONM models have been applied in scoliosis surgery.
MEP evaluates the functional integrity of the descending motor pathway by stimulating the motor cortex and recording from peripheral muscle [9, 10]. The effectiveness of the combined multimodality of MEP and SEP in monitoring spinal cord function has been confirmed, and this multimodal mode has been widely used in surgery to correct idiopathic scoliosis [11]. DNEP is monitored by stimulating the upper end of the operative area in the spinal cord and recording from the sciatic nerve at the popliteal fossae [12]. Although not often used, partial neuromuscular blockade can markedly improve the monitoring quality of SEP by inhibiting muscle noise without affecting MEP monitoring [13,14]. Although SEP and DNEP have been reported to be likely to monitor the same neural tract, each method records different signals via different electrodes. However, both of them are subject to technical failure, and combined application of SEP and DNEP may be a more effective monitoring system used to improve reliability, especially in high-risk surgery. However, it also increases the complexity of the operation to some extent.
Mild scoliosis surgery can be directly corrected without complicated osteotomy procedures, which thus reduces the incidence of neurological complications. However, during surgery to correct severe scoliosis, osteotomy causes massive blood loss, which easily injures the spinal cord blood supply, leading to so-called iatrogenic spinal cord ischemic injury during osteotomy [15,16]. Our previous work showed that osteotomy gap closure and osteotomy have been recognized as 2 surgical stages that have the greatest neurological risks in vertebral column resection surgeries [17]. The required monitoring mode should also be adapted to the surgical procedures. However, different intraoperative neurological monitoring methods require different anesthesia and operative conditions and it is unclear whether the same surgical monitoring method can be applied at the same time in surgery to correct various degrees of scoliosis. There are few reports on the selection of a monitoring model for different surgical strategies.
To determine the most appropriate monitoring mode of evoked potentials for different operations, this study retrospectively analyzed data from 188 patients undergoing spinal deformity correction surgery and their IONM models. Patients with scoliosis were divided into osteotomy and non-osteotomy groups, and the demographics, surgical parameters, and evoked potential events were compared between the SEP/MEP/DNEP mode group and the traditional SEP/MEP monitoring mode group in spinal deformity correction.
Material and Methods
CLINICAL DATA:
This study was approved by the Medical Ethics Review Board of Xinhua Hospital Affiliated to Shanghai Jiaotong University School of Medicine. Informed consent was acquired from all patients included in this study. We retrospectively reviewed data on 188 consecutive cases undergoing spinal deformity correction from May 2008 to February 2015. The patients in the present study met the following criteria: 1) patients receiving spinal deformities surgery with normal neurological function (Frankel grade E); 2) patients with complete IONM data and follow-up data of neurological function (>1 year); 3) patients with neural axis abnormality, or with any history of spinal surgery, were excluded from the study.
Based on surgery strategy, patients were classified into a non-osteotomy group (Group A, grade 1 or grade 2 osteotomy) and an osteotomy group (Group B, osteotomy above grade 3) (Figure 1). Patients in Group A were further divided into 2 sub-groups – A1 (SSEP/MEP monitoring, n=67) and A2 (SSEP/MEP/DNEP monitoring, n=52) – based on the different monitoring modes. Patients in Group B were further divided into B1 (SSEP/MEP monitoring, n=27) and B2 (SSEP/MEP/DNEP monitoring, n=42). Then, the effects of different combined monitoring modes were compared within each group. The long-term neurological outcomes were evaluated according to the Frankel grading method.
ANESTHESIA:
The general anesthesia protocol for spinal deformity correction was conducted according to the previous well-documented protocol [18]. To avoid the effect of inhalation anesthesia on MEP, total intravenous anesthesia was used in all operations. Typically, 1.5–2 mg/kg of propofol, 3–5 ug/kg of fentanyl, and 0.15–0.2 mg/kg of cisatracurium were routinely used for anesthesia induction. The anesthesia was maintained using remifentanil (0.2–0.5 μg/kg/min) and propofol (5–6 mg/kg/h). Moreover, non-depolarized muscle relaxants were used to assist in tracheal intubation during anesthesia induction, and then the use of muscle relaxants was avoided as far as possible during the whole course (or at the exposure stage only, if necessary), so as to reduce the effect of muscle relaxants on the evoked potentials.
IOM PROCEDURE AND ALARM CRITERIA:
The Endeavor CR monitor (Nicolet Company, USA) was used for intraoperative monitoring, and the SEP+MEP or SEP+MEP+DNEP combined multimodality was applied in all cases. MEP disappeared in unilateral or bilateral lower extremities and was not recorded under the repetitive or increased stimulation intensity after eliminating the non-operative factors such as anesthesia, blood pressure, and instruments, and the amplitude was not restored within 10 min [19]. Using the SEP prior to exposure as the monitoring baseline, the amplitude decreased by >50% and/or the latency prolonged by >10% [20]. In this study, the significance level was set at over 2 averaged trials with 80% reduction in primary DNEP amplitude or >10% extension in the response latency compared with the baseline level [21]. The specific operation steps and monitoring parameters were as follows:
STATISTICAL ANALYSIS:
Descriptive statistics were used to summarize the patient clinical and demographic data. Statistical comparisons were made by the independent
Results
HIGH RISK OF NEUROLOGIC COMPLICATIONS IN OSTEOTOMY PATIENTS:
Our results show that the incidence of evoked potential events in osteotomy patients was much higher than that in non-osteotomy patients, including MEP changes. The incidence of postoperative neurological complications was also higher in osteotomy patients than in non-osteotomy patients (Table 1). This suggests that patients with osteotomy have a higher risk of surgical neurological injury than patients without osteotomy.
CORRECTION OF SPINAL DEFORMITY:
The preoperative and postoperative outcomes of deformity correction in Group A and Group B are presented in Figure 3. As shown in Figure 3A, there was no significant difference in preoperative scoliosis (53.87±13.64° vs. 53.61±11.64°), postoperative scoliosis (12.42±7.72° vs. 8.97±7.36°), and correction rate of scoliosis (77.46±11.95% vs. 84.32±12.32%) between Group A1 and Group A2. Similarly, no significant difference was detected in the preoperative scoliosis (114.86±18.56° vs. 115.59±26.01°), postoperative scoliosis (56.14±19.62° vs. 54.07±23.66°), or correction rate of scoliosis (52.15±10.36% vs. 54.27±12.43%) between group B1 and group B2. Furthermore, differences in preoperative kyphosis (112.43±28.65° vs. 111.37±34.86°), postoperative kyphosis (52.24±19.92° vs. 47.07±24.21°), and correction rate of kyphosis (54.22±10.33% vs. 57.98±19.50%) between group B1 and Group B2 were not statistically significant (Figure 3B).
THE OCCURRENCE OF IONM POSITIVE EVENTS AND POSTOPERATIVE NEUROLOGICAL COMPLICATIONS:
SSEP/MEP and SSEP/MEP/DNEP were elicited successfully. Table 2 shows the major clinical characteristics of patients in the non-osteotomy (Group A) and osteotomy (Group B) groups. Three cases, including 2 with MEP change and 1 with SSEP+MEP change, were noted in Group A1, and 1 with SSEP change was noted in Group A2. However, no neurological complications occurred. Our results showed that there were no neurological complications and few intraoperative monitoring events in the non-osteotomy group, but the difference between SSEP/MEP monitoring and SSEP/MEP/DNEP monitoring was not significant (Table 3). A total of 13 cases had 16 EP positive events in Group B1 intraoperatively, including 13 with MEP changes and 3 with SSEP+MEP changes. All of these patients were negative in intraoperative wake-up tests, with no postoperative neural complications. In Group B2, there were 15 EP positive cases which had 21 EP events, including 12 with MEP change, 2 with SSEP+MEP changes, and 7 with SSEP+MEP+DNEP changes. Seven cases were positive for all channels (SSEP/MEP/DNEP), while 5 of them had positive results in wake-up tests and postoperative neurological complications. Regarding neurological complications, the true-positive rate in Group B2 was higher than that in Group B1, indicating that the DNEP/SSEP/TcMEP monitoring modality was superior to the SSEP/TcMEP or single SSEP and TcMEP modality in osteotomy surgery in monitoring neurological events (Table 3).
CAUSES OF INTRAOPERATIVE POSITIVE MONITORING EVENTS:
As shown in Figure 4A, 4 intraoperative positive monitoring events occurred at the stages of screw insertion (n=2) and correction (n=2) in Group A. Table 4 shows the details of intraoperative alarm and treatment in the non-osteotomy group. In Group B, >50% evoked potential monitoring events occurred during the osteotomy procedure, among them, 9 out of 16 monitoring events were monitored in Group B1, while 12 out of the 21 monitoring events were observed in Group B2 (Figure 4B). Table 5 shows the details of intraoperative alarm and treatment in the osteotomy group.
Discussion
At present, several IONM techniques, including single or combined IONM models, have been applied in scoliosis surgery. A large number of studies show that single SEP or MEP allows for effective monitoring of spinal cord function [22–24]. However, SEP or MEP monitoring alone is associated with some drawbacks. SEP mainly monitors the sensory pathway integrity in the posterior spinal tract, but it neglects motor pathway injury in the anterior spinal tract [25]. MEP is highly sensitive to injury and ischemia of the motor pathway in the anterior spinal tract, but it is very vulnerable to anesthesia, blood pressure, and other factors during the implementation process [26,27]. Compared with total intravenous anesthesia, greater voltage amplitude is required to generate the MEP using a volatile agent-based anesthetic regimen [28]. This results in a high false-positive rate [29], which greatly interferes with the surgical process. Therefore, in view of the defect of the single evoked potential monitoring model, some researchers have applied the multimodal IONM mode during spinal surgery. The effectiveness of combined multimodality of MEP and SEP in monitoring spinal cord function has been confirmed, and such a multimodal mode has been widely used in surgery to correct idiopathic scoliosis [11]. However, the present meta-analysis suggests that the SSEP/TcMEP combined multimodality can achieve modest accuracy, and its specificity and sensitivity reached 95.1% and 76.5%, respectively, which is not adequate to meet the needs of high-risk surgery. DNEP must be utilized combined with SEP to monitor the function of the spinal cord intraoperatively when the spinal cord is at high risk [25,30]. In combination with SSEP, MEP, DNEP, and other neuroelectrophysiological tests, a electrophysiological monitoring team successfully monitored the neurological function of 99.6% patients (n=3436 in total); among them, 77 (2.2%) were detected to have neurological impairment [31]. Furthermore, the multimodality evoked potential (MEP/SEP/DNEP) monitoring method provides real-time neurological evaluation of spinal cord function and allow more aggressive surgical correction than could been undertaken previously [32]. According to our previous study, the SEP+MEP+DNEP model can effectively reduce neurological complication rates in surgery to correct spinal deformities [17]. However, this model is not extensively applied in clinical practice compared with the SEP+MEP model, which is due to its relatively complex manipulation and relatively high aseptic requirements. However, few reports are available regarding the selection of monitoring models during different surgeries for spinal deformities with or without extensive osteotomy. In our study, a total of 188 patients undergoing spinal deformity surgery were first divided into a non-osteotomy group and an osteotomy group, and the feasibility and effectiveness of the multimodal IONM modes (such as SSEP/MEP and SSEP/MEP/DNEP) were compared between these 2 groups.
Our results suggested that there were no neurological complications and few intraoperative monitoring events in the non-osteotomy group, and the difference between SSEP/MEP monitoring and SSEP/MEP/DNEP monitoring was not statistically significant. Such results might be ascribed to the shorter operative time, simpler operative procedure, less blood loss, and better status of spinal cord with non-osteotomy surgery. Our results suggest that, compared with the osteotomy group, the operation in the non-osteotomy group was simpler, with fewer neurological complications, less intraoperative confounders of EP, and lower anesthesia requirements. Therefore, we believe that SSEP/MEP combined monitoring is appropriate for non-osteotomy correction in spinal deformity surgery. We found that SSEP/MEP/DNEP combined monitoring requires more sophisticated anesthesia techniques and complex surgical procedure. Notably, the spinous process DNEP technology is associated with some drawbacks, including the accumulation of fluids in the wound that interrupt the detection of signals, as well as the larger dissection. During the surgery, the needle electrodes should be positioned near the spinous processes to the continuous cervical laminae percutaneously; alternatively, they can be positioned to the operated spinal level following laminotomy via the epidural catheter, resulting in greater dissection and massive blood loss. Blood in spinous processes can sometimes interfere with DNEP monitoring. The SSEP/TcMEP monitoring modality appears to be a reliable and convenient biomarker for early detection of spinal cord injury that may result in neurologic deficit.
Our results show that the incidence of EP events and postoperative neurological complications in osteotomy patients is much higher than that in non-osteotomy patients, suggesting that patients with osteotomy have a higher risk of surgical neurological injury than patients without osteotomy. Osteotomy has high risk and high confounding factors, which create higher demand for IONM. The neurologic deficit rate detected in our osteotomy group was 7.2% (5/69), and all of these cases suffered changes in 3 monitoring modes during the operation, and this was higher than that reported with general spinal surgery (2.2%) [31]. This also indicated that severe spinal deformity osteotomy is linked with a higher risk of neurological injury. Notably, intraoperative osteotomy and correction are the risk factors for neuroelectrophysiological monitoring events. Scoliosis osteotomy may result in massive blood loss, and it is also likely to impair blood supply to the spinal cord, leading to so-called iatrogenic spinal cord ischemic injury during osteotomy [15,16]. According to animal research, the motor pathways have higher sensitivity to ischemia and injury than the sensory pathways [33], which frequently present changes prior to the influence on the somatosensory signals [34]. Motor tracts are vulnerable to ischemia; as a result, the motor potential can serve as a highly sensitive predictor of impaired blood supply, which is partially related to the increased metabolism of gray matter in the anterior horn [34]. MEP is highly sensitive to injury and ischemia of the motor pathway in the anterior spinal tract, which is also quite vulnerable to anesthesia, blood pressure, and other intraoperative factors [26,29]. This elevated sensitivity can also result in an increased rate of false-positive results, which can thus require the otherwise unnecessary mitigation measures to lessen the optimum correction for spinal deformity [35]. Nonetheless, supporters of SSEP use have indicated that the rate of false-negative results may be increased when TcMEPs alone is used, thereby increasing the postoperative neurological deficit risk, since only the motor tracts are covered in this mode. Consequently, SSEPs appears to more comprehensively evaluate the function of spinal cord when it is used combined with TcMEPs, which is achieved through monitoring sensory tracts [7]. Interestingly, our study showed that patients with single MEP change or SSEP/MEP change in the osteotomy group had no neurological complications, which suggests a relatively mild and reversible injury; alternatively, it might indicate a false-positive outcome of MEP/SSEP, which commonly occurs during osteotomy surgery and greatly interferes with the surgical process.
DNEP, which is the third spinal cord monitoring method in addition to SSEP and MEP, has been proved to be sensitive and specific to spinal cord injury during scoliosis surgery, especially for patients with severe scoliosis and neuromuscular scoliosis. The combined application of DNEP can avoids false MEP from interrupting the operative process, and it has become an alternative monitoring modality after MEP loss. Compared with MEP, DNEP is less affected by intravenous anesthetics, blood pressure, and other intraoperative factors [29,30]. Conventional intravenous anesthetics, including opioids, propofol, and thiopental, can dose-dependently suppress MEP. Only remifentanil and propofol that are administered via the plasma level target-controlled infusion system can record MEP in the predefined range of target plasma level [29]. Furthermore, DNEP monitoring is better than the traditional SSEP monitoring in identifying injury to the spinal cord, with a sensitivity of 100%
Some limitations should be noted in our study. First, it was a single-center, retrospective study, not a prospective, randomized study. Second, it had a small sample size, and the conclusions should be validated by multi-center large-sample data. Third, the patient population was heterogeneous and the study did not compare different Lenke classifications, etiology, and operation segments. In the future, large-sample, randomized, and prospective clinical research is needed to obtain more scientific and accurate conclusions. Nonetheless, our study has strengths, including the favorable findings based on our warning criteria and protocol. Moreover, the monitoring strategy proposed based on our clinical experience and prior research could possibly guide IONM during spinal deformity surgery. Nevertheless, more well-designed, prospective research is needed to validate our findings.
Conclusions
In summary, intraoperative simultaneous monitoring of SSEP/MEP can effectively reflect the neurological function in non-osteotomy surgery of spinal deformity, which only requires a relatively simple operation and anesthesia. For osteotomy cases, simultaneous monitoring of SSEP/MEP/DNEP can effectively avoid the unnecessary interference of false alarms of MEP.
Figures
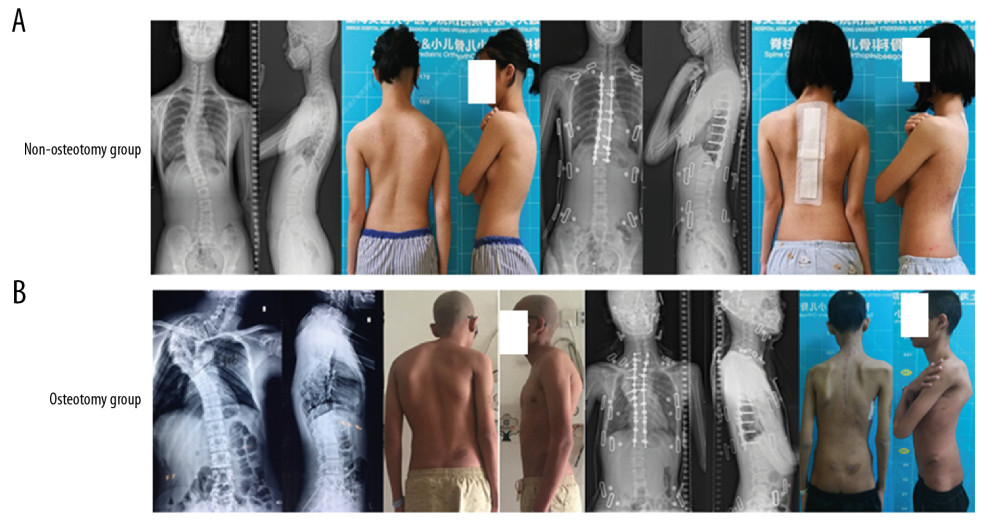 Figure 1. Two cases of the non-osteotomy group and osteotomy group. (A) A 14-year-old patient with scoliosis who was treated with a multilevel posterior correction without osteotomy (non-osteotomy group). (B) A 15-year-old patient with a severe and stiff scoliosis who was treated with a long posterior reconstruction from C7 to T12 with one-level grade 4 osteotomy at T4 (osteotomy group).
Figure 1. Two cases of the non-osteotomy group and osteotomy group. (A) A 14-year-old patient with scoliosis who was treated with a multilevel posterior correction without osteotomy (non-osteotomy group). (B) A 15-year-old patient with a severe and stiff scoliosis who was treated with a long posterior reconstruction from C7 to T12 with one-level grade 4 osteotomy at T4 (osteotomy group). 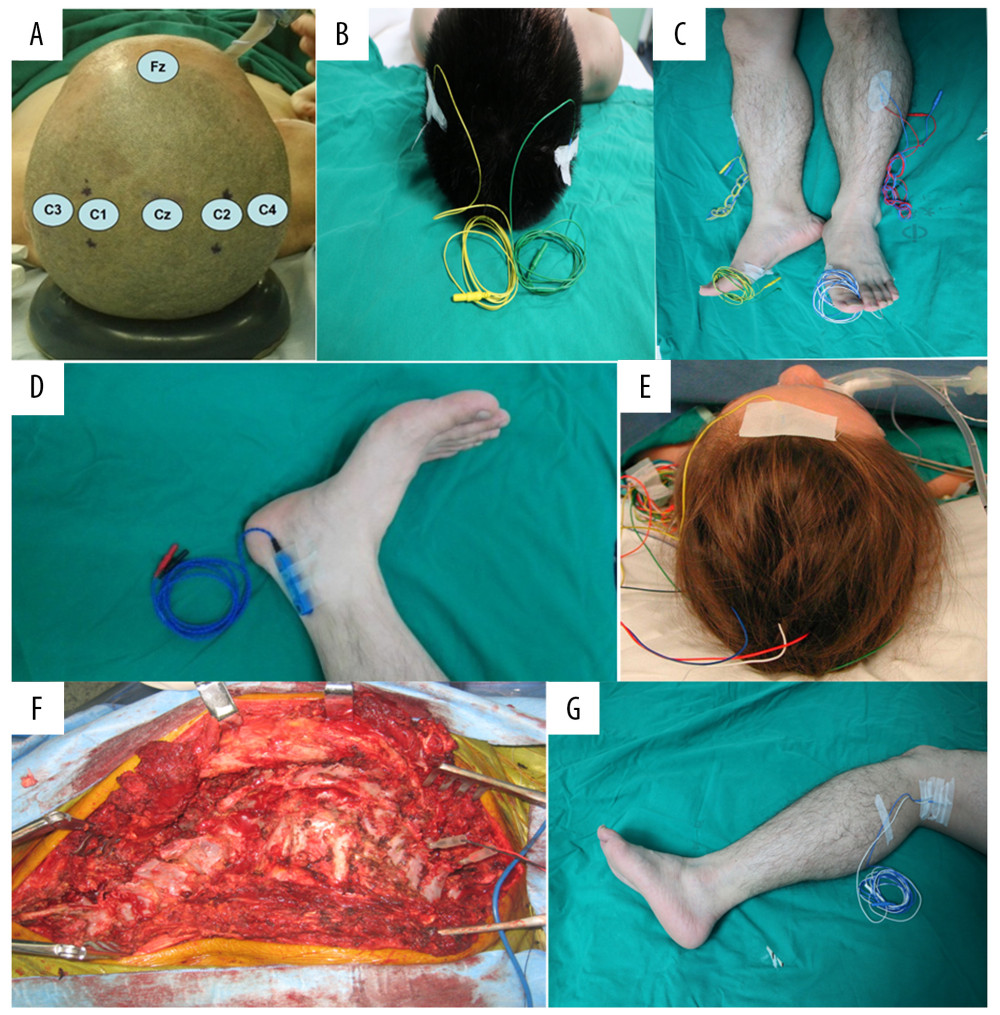 Figure 2. The position of IOM stimulation electrode and recording electrode. (A–C) MEP monitoring: The stimulation electrodes are placed on C3 and C4 of the International 10–20 system of EEG; the recording electrodes are placed on the thenar and hypothenar muscles, tibialis anterior muscle, and flexor brevis muscle. (A, D, E) SEP monitoring: The stimulation electrode is placed between the Achilles tendon and the medial malleolus; the recording electrode is placed on the Cz and Fz of the International 10–20 system of EEG. (F, G) DNEP monitoring: The stimulation electrode is placed under the spinous process, and the recording electrode is placed in the popliteal fossa.
Figure 2. The position of IOM stimulation electrode and recording electrode. (A–C) MEP monitoring: The stimulation electrodes are placed on C3 and C4 of the International 10–20 system of EEG; the recording electrodes are placed on the thenar and hypothenar muscles, tibialis anterior muscle, and flexor brevis muscle. (A, D, E) SEP monitoring: The stimulation electrode is placed between the Achilles tendon and the medial malleolus; the recording electrode is placed on the Cz and Fz of the International 10–20 system of EEG. (F, G) DNEP monitoring: The stimulation electrode is placed under the spinous process, and the recording electrode is placed in the popliteal fossa. 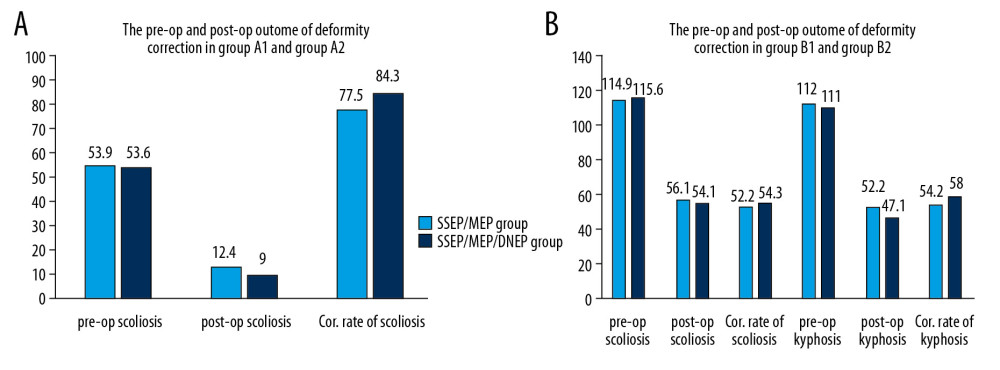 Figure 3. The preoperative and postoperative outcomes of deformity correction in Group A (A) and Group B (B). MEP – motor evoked potential; SSEP – somatosensory evoked potentials; DNEP – descending neurogenic evoked potentials
Figure 3. The preoperative and postoperative outcomes of deformity correction in Group A (A) and Group B (B). MEP – motor evoked potential; SSEP – somatosensory evoked potentials; DNEP – descending neurogenic evoked potentials 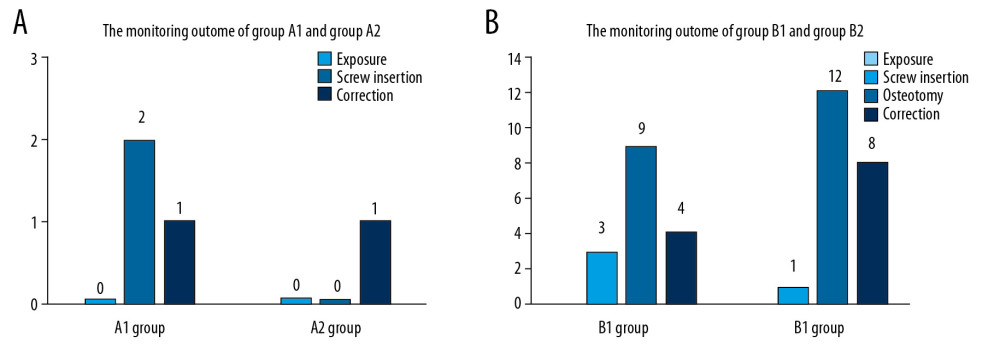 Figure 4. Causes of evoked potential events in Group A (A) and Group B (B).
Figure 4. Causes of evoked potential events in Group A (A) and Group B (B). Tables
Table 1. Intraoperative evoked potential events and postoperative neurological complications between the non-osteotomy group and osteotomy group.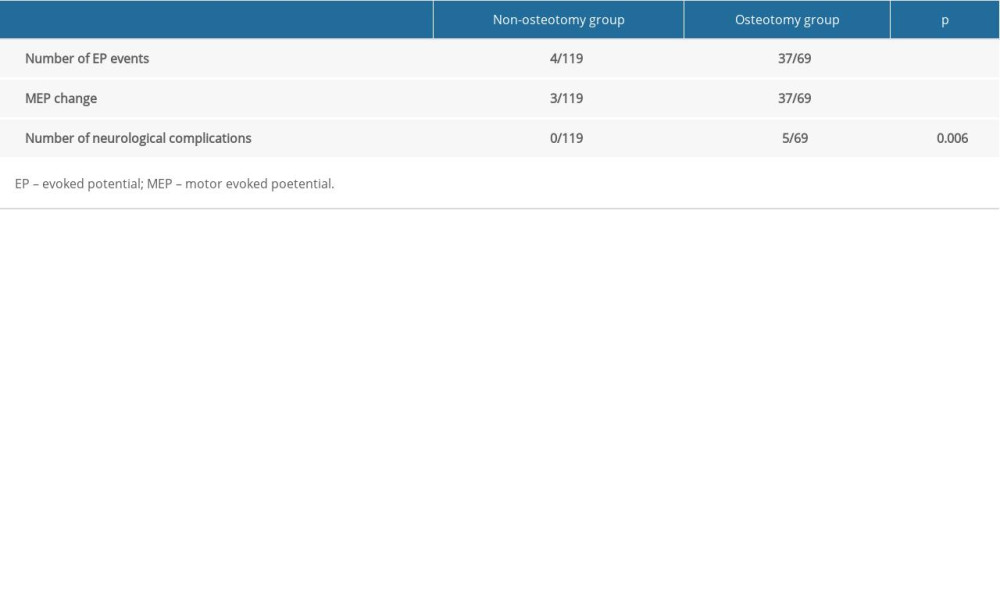 Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group.
Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group.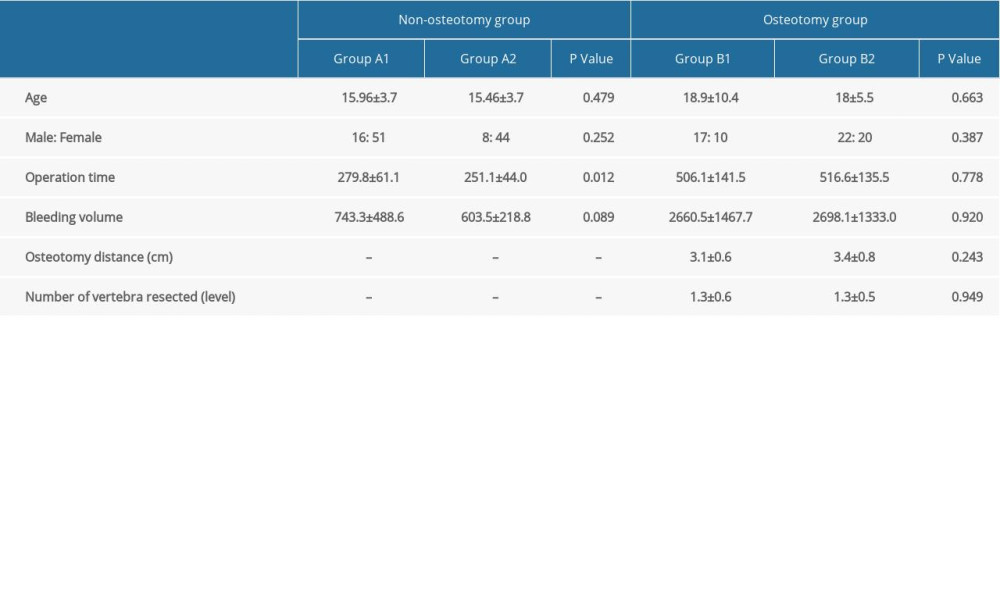 Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group.
Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group.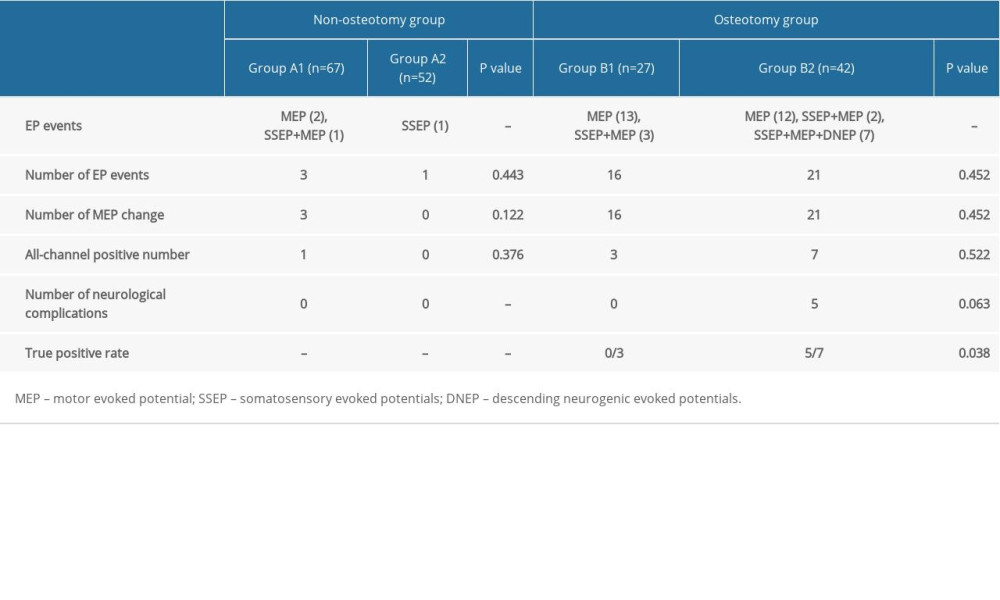 Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group.
Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group.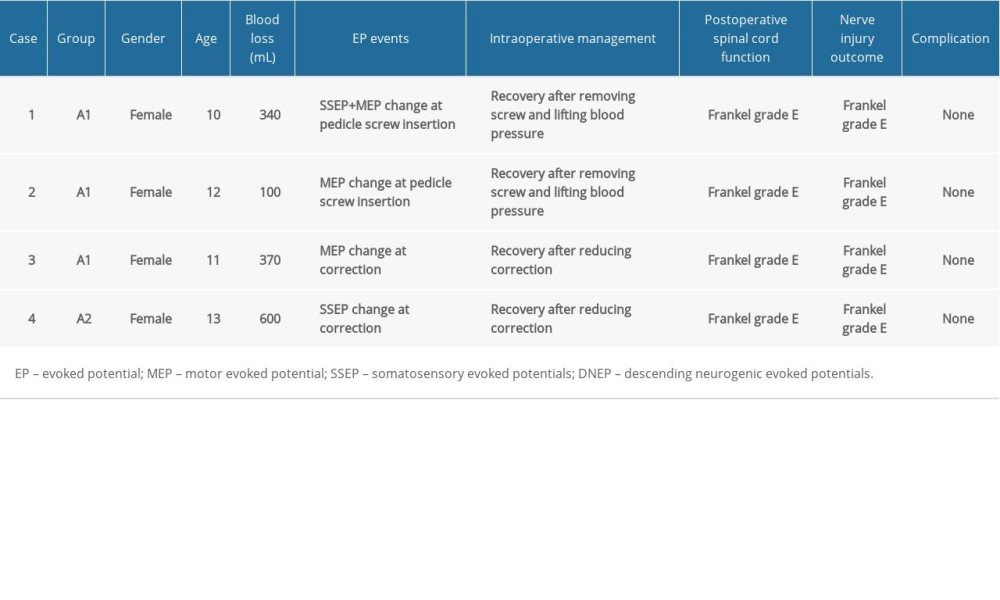 Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group.
Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group.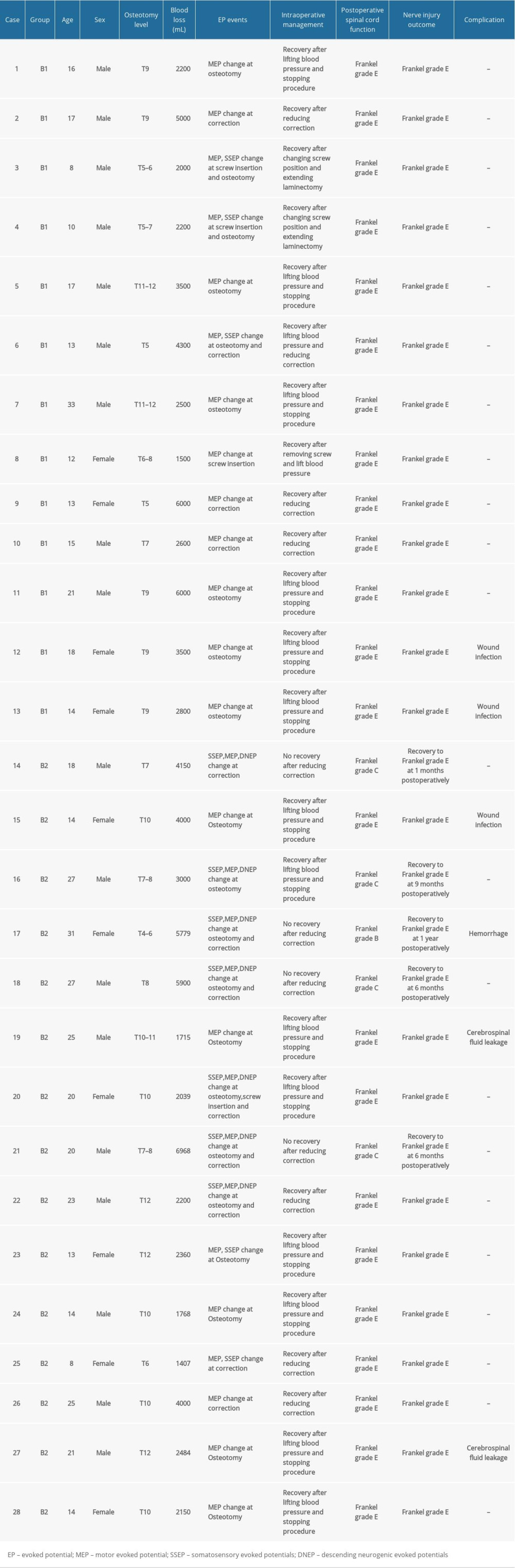
References
1. Feng J, Zhou J, Huang M, Clinical and radiological outcomes of the multilevel Ponte osteotomy with posterior selective segmental pedicle screw constructs to treat adolescent thoracic idiopathic scoliosis: J Orthop Surg Res, 2018; 13; 305
2. Wang Y, Liu Z, Du C, The radiological outcomes of one-stage posterior-only hemivertebra resection and short segmental fusion for lumbosacral hemivertebra: A minimum of 5 years of follow-up: J Orthop Surg Res, 2019; 14; 426
3. Yang JL, Huang ZF, Yin JQ, A proposed classification system for guiding surgical strategy in cases of severe spinal deformity based on spinal cord function: Eur Spine J, 2016; 25; 1821-29
4. Lenke LG, O’Leary PT, Bridwell KH, Posterior vertebral column resection for severe pediatric deformity: Minimum two-year follow-up of thirty-five consecutive patients: Spine (Phila Pa 1976), 2009; 34; 2213-21
5. Wang XB, Lenke LG, Thuet E, Deformity angular ratio describes the severity of spinal deformity and predicts the risk of neurologic deficit in posterior vertebral column resection surgery: Spine (Phila Pa 1976), 2016; 41; 1447-55
6. Li X, Zeng L, Li X, Preoperative halo-gravity traction for severe thoracic kyphoscoliosis patients from Tibet: Radiographic correction, pulmonary function improvement, nursing, and complications: Med Sci Monit, 2017; 23; 4021-27
7. Bhagat S, Durst A, Grover H, An evaluation of multimodal spinal cord monitoring in scoliosis surgery: A single centre experience of 354 operations: Eur Spine J, 2015; 24; 1399-407
8. Hadley MN, Shank CD, Rozzelle CJ, Guidelines for the use of electrophysiological monitoring for surgery of the human spinal column and spinal cord: Neurosurgery, 2017; 81; 713-32
9. Macdonald DB, Skinner S, Shils JAmerican Society of Neurophysiological Monitoring, Intraoperative motor evoked potential monitoring – a position statement by the American Society of Neurophysiological Monitoring: Clin Neurophysiol, 2013; 124; 2291-316
10. Park JH, Hyun SJ, Intraoperative neurophysiological monitoring in spinal surgery: World J Clin Cases, 2015; 3; 765-73
11. Thirumala PD, Huang J, Thiagarajan K, Diagnostic accuracy of combined multimodality somatosensory evoked potential and transcranial motor evoked potential intraoperative monitoring in patients with idiopathic scoliosis: Spine (Phila Pa 1976), 2016; 41; E1177-84
12. Owen JH, Laschinger J, Bridwell K, Sensitivity and specificity of somatosensory and neurogenic-motor evoked potentials in animals and humans: Spine (Phila Pa 1976), 1988; 13; 1111-18
13. Mendiratta A, Emerson RG, Neurophysiologic intraoperative monitoring of scoliosis surgery: J Clin Neurophysiol, 2009; 26; 62-69
14. Sloan T, Anesthesia and intraoperative neurophysiological monitoring in children: Childs Nerv Syst, 2010; 26; 227-35
15. Perese DM, Fracasso JE, Anatomical considerations in surgery of the spinal cord: A study of vessels and measurements of the cord: J Neurosurg, 1959; 16; 314-25
16. Holdefer RN, MacDonald DB, Skinner SA, Somatosensory and motor evoked potentials as biomarkers for post-operative neurological status: Clin Neurophysiol, 2015; 126; 857-65
17. Huang ZF, Chen L, Yang JF, Multimodality intraoperative neuromonitoring in severe thoracic deformity PVCR correction: World Neurosurg, 2019; 127; e416-26
18. Wang S, Zhang J, Tian Y, Intraoperative motor evoked potential monitoring to patients with preoperative spinal deficits: Judging its feasibility and analyzing the significance of rapid signal loss: Spine J, 2017; 17; 777-83
19. Cohen D, Cuffin BN, Developing a more focal magnetic stimulator. Part I: Some basic principles: J Clin Neurophysiol, 1991; 8; 102-11
20. Thirumala PD, Bodily L, Tint D, Somatosensory-evoked potential monitoring during instrumented scoliosis corrective procedures: Validity revisited: Spine J, 2014; 14; 1572-80
21. Raynor BL, Bright JD, Lenke LG, Significant change or loss of intraoperative monitoring data: A 25-year experience in 12,375 spinal surgeries: Spine (Phila Pa 1976), 2013; 38; E101-8
22. Huang SL, Qi HG, Liu JJ, Alarm value of somatosensory evoked potential in idiopathic scoliosis surgery: World Neurosurg, 2016; 92; 397-401
23. Langeloo DD, Lelivelt A, Louis Journee H, Transcranial electrical motor-evoked potential monitoring during surgery for spinal deformity: A study of 145 patients: Spine (Phila Pa 1976), 2003; 28; 1043-50
24. Chen S, Yi M, Zhou G, Abdominal aortic transplantation of bone marrow mesenchymal stem cells regulates the expression of ciliary neurotrophic factor and inflammatory cytokines in a rat model of spinal cord ischemia-reperfusion injury: Med Sci Monit, 2019; 25; 1960-69
25. Owen JH, Jenny AB, Naito M, Effects of spinal cord lesioning on somatosensory and neurogenic-motor evoked potentials: Spine (Phila Pa 1976), 1989; 14; 673-82
26. Nakatoh S, Kitagawa H, Kawaguchi Y, Change of muscle motor-evoked potentials after motor cortex stimulation caused by acute spinal cord injury in cats: J Spinal Disord, 2001; 14; 32-38
27. Ugawa R, Takigawa T, Shimomiya H, An evaluation of anesthetic fade in motor evoked potential monitoring in spinal deformity surgeries: J Orthop Surg Res, 2018; 13; 227
28. Martin DP, Bhalla T, Thung A, A preliminary study of volatile agents or total intravenous anesthesia for neurophysiological monitoring during posterior spinal fusion in adolescents with idiopathic scoliosis: Spine (Phila Pa 1976), 2014; 39; E1318-24
29. Scheufler KM, Zentner J, Total intravenous anesthesia for intraoperative monitoring of the motor pathways: An integral view combining clinical and experimental data: J Neurosurg, 2002; 96; 571-79
30. Noonan KJ, Walker T, Feinberg JR, Factors related to false-versus true-positive neuromonitoring changes in adolescent idiopathic scoliosis surgery: Spine (Phila Pa 1976), 2002; 27; 825-30
31. Thuet ED, Winscher JC, Padberg AM, Validity and reliability of intraoperative monitoring in pediatric spinal deformity surgery: A 23-year experience of 3436 surgical cases: Spine (Phila Pa 1976), 2010; 35; 1880-86
32. Laratta JL, Ha A, Shillingford JN, Neuromonitoring in spinal deformity surgery: A multimodality approach: Global Spine J, 2018; 8; 68-77
33. Hayen A, Macaskill P, Irwig L, Appropriate statistical methods are required to assess diagnostic tests for replacement, add-on, and triage: J Clin Epidemiol, 2010; 63; 883-91
34. Dawson EG, Sherman JE, Kanim LE, Spinal cord monitoring. Results of the Scoliosis Research Society and the European Spinal Deformity Society survey: Spine (Phila Pa 1976), 1991; 16; S361-64
35. Kim DH, Zaremski J, Kwon B, Risk factors for false positive transcranial motor evoked potential monitoring alerts during surgical treatment of cervical myelopathy: Spine (Phila Pa 1976), 2007; 32; 3041-46
36. Kundnani VK, Zhu L, Tak H, Multimodal intraoperative neuromonitoring in corrective surgery for adolescent idiopathic scoliosis: Evaluation of 354 consecutive cases: Indian J Orthop, 2010; 44; 64-72
37. Emerson RG, NIOM for spinal deformity surgery: there’s more than one way to skin a cat: J Clin Neurophysiol, 2012; 29; 149-50
38. Delecrin J, Nguyen The Tich S, Passuti N, Péréon YNeurogenic mixed evoked potential monitoring during scoliosis surgery: Retrospective analysis of 149 cases: Rev Chir Orthop Reparatrice Appar Mot, 2000; 86; 46-53 [in French]
39. Bernard JM, Pereon Y, Fayet G, Guiheneuc P, Effects of isoflurane and desflurane on neurogenic motor- and somatosensory-evoked potential monitoring for scoliosis surgery: Anesthesiology, 1996; 85; 1013-19
40. Owen JH, Bridwell KH, Grubb R, The clinical application of neurogenic motor evoked potentials to monitor spinal cord function during surgery: Spine (Phila Pa 1976), 1991; 16; S385-90
41. Gavaret M, Pesenti S, Diop-Sene MS, Intraoperative spinal cord monitoring: Lesional level diagnosis: Orthop Traumatol Surg Res, 2017; 103; 33-38
42. Raynor BL, Padberg AM, Lenke LG, Failure of intraoperative monitoring to detect postoperative neurologic deficits: A 25-year experience in 12,375 spinal surgeries: Spine (Phila Pa 1976), 2016; 41; 1387-93
Figures
 Figure 1. Two cases of the non-osteotomy group and osteotomy group. (A) A 14-year-old patient with scoliosis who was treated with a multilevel posterior correction without osteotomy (non-osteotomy group). (B) A 15-year-old patient with a severe and stiff scoliosis who was treated with a long posterior reconstruction from C7 to T12 with one-level grade 4 osteotomy at T4 (osteotomy group).
Figure 1. Two cases of the non-osteotomy group and osteotomy group. (A) A 14-year-old patient with scoliosis who was treated with a multilevel posterior correction without osteotomy (non-osteotomy group). (B) A 15-year-old patient with a severe and stiff scoliosis who was treated with a long posterior reconstruction from C7 to T12 with one-level grade 4 osteotomy at T4 (osteotomy group). Figure 2. The position of IOM stimulation electrode and recording electrode. (A–C) MEP monitoring: The stimulation electrodes are placed on C3 and C4 of the International 10–20 system of EEG; the recording electrodes are placed on the thenar and hypothenar muscles, tibialis anterior muscle, and flexor brevis muscle. (A, D, E) SEP monitoring: The stimulation electrode is placed between the Achilles tendon and the medial malleolus; the recording electrode is placed on the Cz and Fz of the International 10–20 system of EEG. (F, G) DNEP monitoring: The stimulation electrode is placed under the spinous process, and the recording electrode is placed in the popliteal fossa.
Figure 2. The position of IOM stimulation electrode and recording electrode. (A–C) MEP monitoring: The stimulation electrodes are placed on C3 and C4 of the International 10–20 system of EEG; the recording electrodes are placed on the thenar and hypothenar muscles, tibialis anterior muscle, and flexor brevis muscle. (A, D, E) SEP monitoring: The stimulation electrode is placed between the Achilles tendon and the medial malleolus; the recording electrode is placed on the Cz and Fz of the International 10–20 system of EEG. (F, G) DNEP monitoring: The stimulation electrode is placed under the spinous process, and the recording electrode is placed in the popliteal fossa. Figure 3. The preoperative and postoperative outcomes of deformity correction in Group A (A) and Group B (B). MEP – motor evoked potential; SSEP – somatosensory evoked potentials; DNEP – descending neurogenic evoked potentials
Figure 3. The preoperative and postoperative outcomes of deformity correction in Group A (A) and Group B (B). MEP – motor evoked potential; SSEP – somatosensory evoked potentials; DNEP – descending neurogenic evoked potentials Figure 4. Causes of evoked potential events in Group A (A) and Group B (B).
Figure 4. Causes of evoked potential events in Group A (A) and Group B (B). Tables
 Table 1. Intraoperative evoked potential events and postoperative neurological complications between the non-osteotomy group and osteotomy group.
Table 1. Intraoperative evoked potential events and postoperative neurological complications between the non-osteotomy group and osteotomy group. Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group.
Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group. Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group.
Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group. Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group.
Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group. Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group.
Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group. Table 1. Intraoperative evoked potential events and postoperative neurological complications between the non-osteotomy group and osteotomy group.
Table 1. Intraoperative evoked potential events and postoperative neurological complications between the non-osteotomy group and osteotomy group. Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group.
Table 2. Patient preoperative demographics compared between the non-osteotomy group and osteotomy group. Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group.
Table 3. The results of intraoperative evoked potential outcomes between the non-osteotomy group and osteotomy group. Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group.
Table 4. Data of intraoperative evoked potential events and outcomes in the non-osteotomy group. Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group.
Table 5. Data of intraoperative evoked potential events and outcomes in the osteotomy group. In Press
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
11 Mar 2024 : Clinical Research
Comparison of Effects of Sugammadex and Neostigmine on Postoperative Neuromuscular Blockade Recovery in Pat...Med Sci Monit In Press; DOI: 10.12659/MSM.942773
12 Mar 2024 : Clinical Research
Comparing Neuromuscular Blockade Measurement Between Upper Arm (TOF Cuff®) and Eyelid (TOF Scan®) Using Miv...Med Sci Monit In Press; DOI: 10.12659/MSM.943630
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








