28 February 2021: Clinical Research
Comparison of Combined Hemodialysis and Hemoperfusion with Hemoperfusion Alone in 106 Patients with Diabetic Ketoacidosis and Acute Renal Failure: A Retrospective Study from a Single Center in China
Guixia Wang1ACE, Zhenhe Li2AEF*, Yuliang Zhang1BCE, Yingying Pan1CDE, Longying Chen1CEFDOI: 10.12659/MSM.922753
Med Sci Monit 2021; 27:e922753
Abstract
BACKGROUND: Acute kidney injury with acute renal failure is associated with severe diabetic ketoacidosis. This retrospective study was conducted at a single center in China and aimed to compare combined hemodialysis and hemoperfusion (hemodialysis+hemoperfusion) with hemoperfusion alone in 106 patients with diabetic ketoacidosis and acute renal failure.
MATERIAL AND METHODS: The 106 patients were divided into 2 groups according to different dialysis programs, with 53 cases in each group. Hemodialysis was performed using a single-pass 4008S FX8 HeLix-One hollow fiber hemodialyzer (Fresenius Medical Care, St. Wendel, Germany). Hemoperfusion was performed using HA130 resin adsorbents.
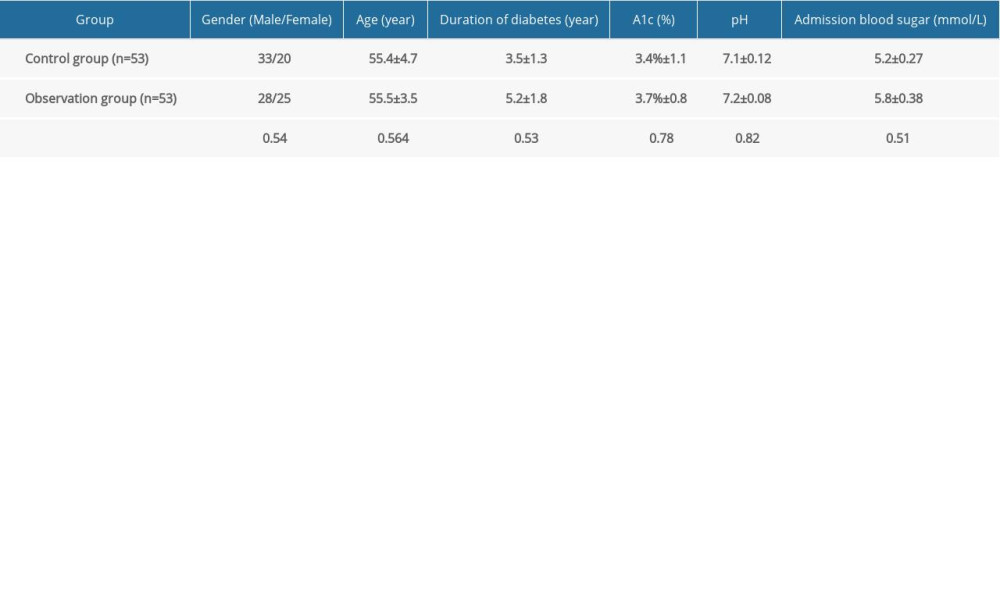
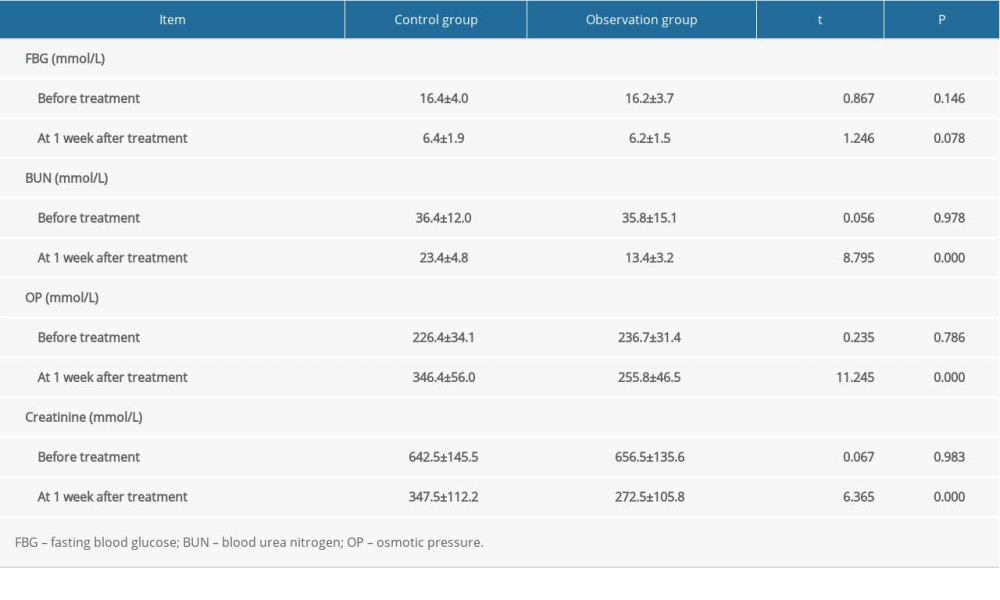
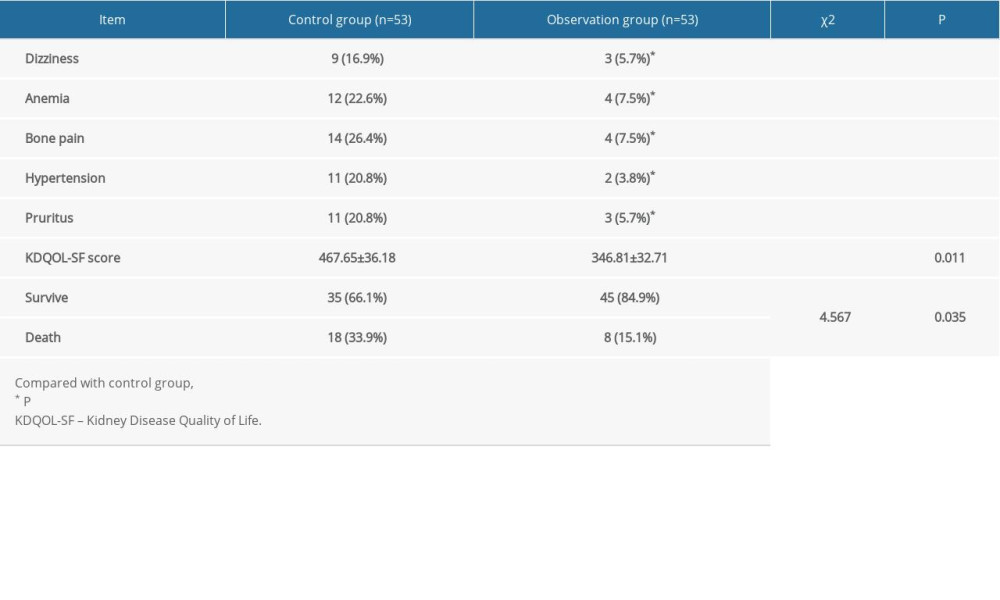
RESULTS: There were no significant differences in terms of sex, age, duration of diabetes, A1c, pH, and admission blood glucose between the 2 groups (P=0.54, 0.564, 0.53, 0.78, 0.82, 0.51). There were no significant differences in fasting blood glucose, blood urea nitrogen, osmotic pressure, and creatinine between the 2 groups before treatment (P=0.146, 0.978, 0.786, 0.983). After treatment, blood urea nitrogen and creatinine in the dual-treatment group were lower than in the control group, and the osmotic pressure was higher than that in the control group (P=0.000, 0.000, 0.000). The dual-treatment group experienced a lower prevalence of dizziness (5.7%), anemia (7.5%), bone pain (7.5%), hypertension (3.8%), and pruritus (5.7%) than the control group (P<0.05).
CONCLUSIONS: Compared with hemoperfusion alone, hemodialysis+hemoperfusion significantly reduced pruritus and anemia, improved renal function, and was associated with significantly fewer adverse events in patients with diabetic ketoacidosis and acute renal failure.
Keywords: Acute Kidney Injury, Diabetic Ketoacidosis, Hemodialysis Units, Hospital, Hemoperfusion, Blood Urea Nitrogen, Creatinine, Pruritus, Renal Dialysis
Background
Diabetic ketoacidosis is a common clinical emergency for diabetic patients. It can be caused by multiple factors that lead to insufficient insulin and an inadequate increase in glucose-generating hormones, resulting in hyperglycemia, hyperketonemia, ketonuria, dehydration, and electrolyte and metabolic disorders [1–3]. The exchange of substances through dispersion, ultrafiltration, adsorption, and convection removes metabolic wastes in the body, maintains electrolyte and acid-base balance, and simultaneously removes excess water in the body and returns the purified blood to circulation [4–6]. As the prevalence of diabetes has continued to rise in China, diabetes has become the primary cause of chronic kidney disease, surpassing glomerulonephritis-related chronic kidney disease [7]. Acute kidney injury is an important risk factor associated with increased morbidity and mortality in diabetic patients with ketoacidosis. Multiple risk factors contribute to the development of acute kidney injury. Acute kidney injury and advanced acute kidney injury are associated with rapid progressive chronic kidney disease and mortality in patients with diabetic ketoacidosis [8]. The development of acute kidney injury, defined as acute changes in the serum creatinine level, characterizes hospitalized patients at increased risk of adverse outcomes [9]. There is no consensus definition of acute renal failure in critically ill patients. More than 30 different definitions have been used in the literature, creating much confusion and making comparisons difficult [10]. At present, drugs cannot cure uremia, which is usually treated with hemodialysis to control the progression of the disease [11]. Hemoperfusion is a dialysis treatment that introduces blood into the perfusion device and removes toxins from the body by means of dispersion, adsorption, and filtration [12]. It can effectively remove medium and macromolecular toxins in the blood [13]. This retrospective study was conducted at a single center in China and aimed to compare combined hemodialysis and hemoperfusion (hemodialysis+hemoperfusion) with hemoperfusion alone in 106 patients with diabetic ketoacidosis and acute renal failure.
Material and Methods
STUDY PARTICIPANTS:
From July 2018 to June 2019, 106 patients with diabetic ketoacidosis and acute renal failure were enrolled in this study. They were divided into 2 groups, with 53 individuals in each group. The control group (hemoperfusion alone) included 33 men and 20 women. Their ages ranged from 40 to 76 years (average 55.4±4.7 years), and the duration of diabetes was 2 to 8 years (average 3.5±1.3 years). The dual-treatment group (hemodialysis+hemoperfusion) included 28 men and 25 women aged 40–77 years (average 55.5±3.5 years old), with a diabetes duration of 2 to 9 years (average 5.2±1.8 years). The study was approved by the Ethics Committee of Linyi Central Hospital.
The clinical data of all cases were complete and were consistent with the diagnostic criteria of diabetic nephropathy complicated by ketoacidosis. All patients had a diagnosis of acute renal failure. Patients with severe heart, liver, or kidney dysfunction; ketosis caused by drinking or starvation; or cancer were excluded from the study. The diagnostic criteria for acute renal failure were: (1) the increase of serum creatinine (SCr) within 48 h of ≥0.3 mg/dL (26.5 μmol/L); (2) SCr ≥1.5 times the basic value, with a clear or inferred indication that it occurred within the previous 7 days; and (3) a urine volume of <0.5 mL/kg/h for more than 6 h. Acute renal failure was diagnosed if at least one of these conditions was met [14]. The diagnostic criteria for diabetic ketoacidosis in adults issued by the American Diabetes Association (ADA) include: (1) hyperglycemia (blood glucose >13.9 mmol/L [>250 mg/dL]); (2) arterial pH ≤7.3; (3) serum bicarbonate ≤ϖ18 mmol/L; (4) blood anion gap >10 mmol/L; and (5) positive serum or urine ketone on a semiquantitative test [15].
The inclusion criteria for the current study were the following: (1) patients with blood ketone positive or (and) urine ketone positive; (2) patients with carbon dioxide binding capacity <22 mmol/L, pH <7.35, and blood bicarbonate <22 mmol/L; (3) patients with short-term increase of creatinine >176 μmol/L and creatinine clearance >50%; (4) patients with original chronic renal dysfunction; and (5) patients with increased creatinine onset >50% or increased creatinine clearance >15%. Exclusion criteria were: (1) patients with severe dysfunction of other organs, and (2) patients with ketoacidosis caused by starvation or alcohol.
METHODS:
Patients in both groups were actively treated for the primary disease, and sustained insulin therapy was given at a low dose [0.1 U/kg/h] to control blood glucose levels. At the same time, the water and electrolyte acid-base disorders, fluid replacement, and prevention of complications were actively addressed. Urinary ketones, blood ketones, and blood glucose levels were measured at defined time points. Hemodialysis was performed using a single-pass 4008S FX8 HeLix-One hollow fiber hemodialyzer (Fresenius Medical Care, St. Wendel, Germany). Hemoperfusion was performed using HA130 resin adsorbents. The control group was treated with hemoperfusion. Bicarbonate was used as the dialysate, and venous fistula was used as the puncture point. Heparin was given for anticoagulation at a dosage of 0.5–0.8 mg/kg at a rate of 6–12 mg/h. The drug was suspended 30 min before hemoperfusion, with blood flow of 150–200 mL/min and hemoperfusion flow of 500 mL/min, 4 h for each time, 3 times a week, for 2 months. The dual-treatment group underwent hemoperfusion as well as an additional hemodialysis treatment. Bicarbonate was used as the dialysate. A serial dialyzer tube was connected with the perfusion device, the tube was repeatedly cleaned with a 0.9% sodium chloride solution, air was purged from the tube, and the tube was closed with 3 L of heparin sodium normal saline for 30 min. The heparin saline was removed with 0.5 L of 0.9% sodium chloride solution, heparin was given for anticoagulation, hemodialysis+hemoperfusion was performed for 2 h, and then hemodialysis for 2 h. This process was repeated twice a month, for 2 months.
OUTCOME MEASURES:
The clinical symptoms and related indicators were observed to evaluate renal function and toxin clearance effects, including blood urea nitrogen (BUN), SCr, serum β2 microglobulin, parathyroid hormone, blood phosphorus, and calcium ion. Fasting blood glucose, BUN, osmotic pressure, and creatinine were compared between the 2 groups. Patients were monitored for adverse events such as nosocomial infections, sudden coronary heart disease, and hypotension. Quality of life in both groups was recorded. The changes in biochemical indicators before and 1 week after treatment were evaluated. Biochemical indicators included fasting blood glucose, BUN, osmotic pressure, and creatinine. Survival rates within 6 months were observed and compared between the 2 groups. The Kidney Disease Quality of Life (KDQOL-SF) assessment included 43 questions with 11 dimensions, and a higher total score was associated with a better quality of life.
STATISTICAL ANALYSIS:
SPSS 21.0 software was used to analyze the statistical data. The measurement data were expressed as mean±standard deviation (mean±SD), and the enumeration data were expressed as numerical values and percentages. Comparison between the 2 groups used the
Results
DISCUSSION:
Diabetic ketoacidosis combined with acute renal failure is a serious disease that endangers the lives of patients [16]. It is mainly characterized by hyperglycemia, hyperkalemia, dehydration, electrolyte imbalance, and acidosis. Diabetic ketoacidosis can induce tissue ischemic injury as the disease progresses, and the mortality rate is high [17].
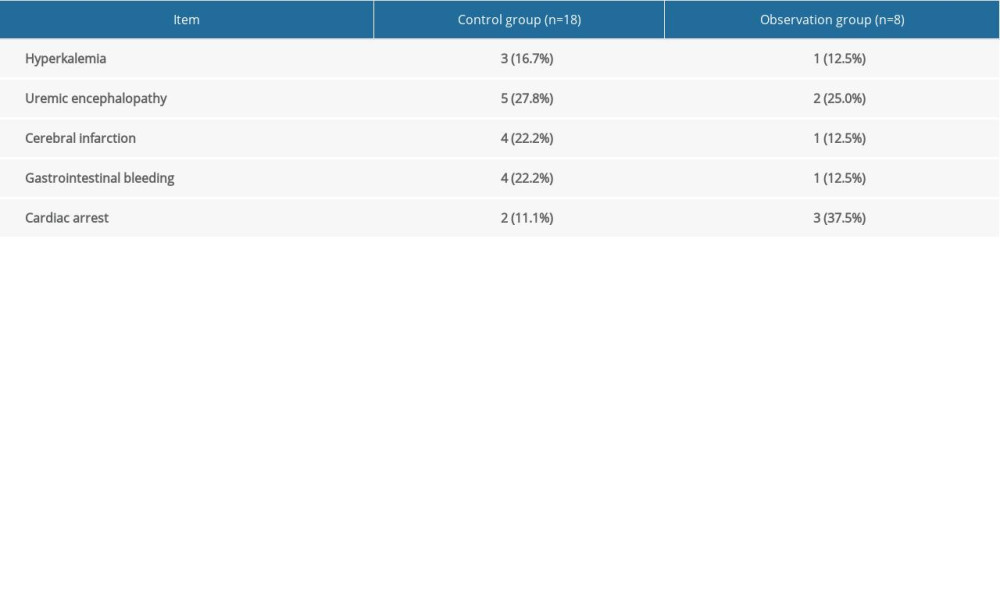
In this study, hemodialysis+hemoperfusion was performed in patients with diabetic ketoacidosis and acute renal failure. The results showed no significant differences in fasting blood glucose, BUN, osmotic pressure, and creatinine between the 2 groups before treatment. After treatment, BUN and creatinine in the dual-treatment group were lower than those in the control group, and the osmotic pressure was higher than that in the control group. The dual-treatment group had a lower incidence of dizziness (5.7%), anemia (7.5%), bone pain (7.5%), hypertension (3.8%), and pruritus (5.7%) compared with the control group, suggesting that hemodialysis+hemoperfusion is effective in the treatment of diabetic ketoacidosis and acute renal failure. This protocol could alleviate clinical symptoms, improve toxin removal, and improve the quality of life, and the results were consistent with previous findings [18]. The reason for the effectiveness may be that the blood perfusion device contains a solid adsorbent [19]. After the patient’s blood is introduced, the endogenous and exogenous drugs, toxins, and metabolic wastes that cannot be removed by hemodialysis can be removed through an adsorption effect, effectively purifying the blood [20]. However, hemoperfusion can also remove medium-size molecular substances and macromolecular substances such as uric acid and creatine. The removal of urea is not beneficial, and hemoperfusion cannot balance water and electrolytes [21]. Therefore, hemoperfusion alone is not ideal for treating diabetic ketoacidosis and acute renal failure. Hemodialysis and hemoperfusion can complement each other, however, by removing molecules ranging from small to large size, as well as inflammatory substances. Because the biocompatibility of the 2 techniques is good, it can promote the stability of the body’s water and electrolytes and reduce adverse reactions during dialysis [22]. The results of this study showed that the KDQOL-SF score (467.65±36.18) in the dual-treatment group was higher than that in the control group (346.81±32.71). The survival rate was 84.9% in the dual-treatment group and 66.0% in the control group, indicating that hemodialysis+hemoperfusion therapy has a high safety level and improves prognosis.
At present, diabetic ketoacidosis combined with acute renal failure is believed to be mainly related to the following factors: (1) infection: when the body is seriously infected, it can cause microcirculation disturbance, reduce blood flow, and then reduce the glomerular filtration rate; (2) hyperglycemia: after the onset of diabetic ketoacidosis, the patient’s blood glucose index is significantly increased, and the osmotic pressure is increased under the action of hyperglycemia, resulting in dehydration and electrolyte imbalance, combined with symptoms such as nausea and vomiting, that further reduce the circulating blood volume; (3) multiple organ failure: diabetic ketoacidosis patients are prone to multiple organ failure, and multiple organ failure and renal failure are mutually causal and can exacerbate the degree of renal function damage; and (4) acidosis: after acidosis, the myocardial contractile function of the patient is significantly decreased, resulting in peripheral vasodilation, which reduces the circulating blood volume and blood pressure [23,24]. Under the combined effect of these factors, the symptoms of poisoning in patients with diabetic ketoacidosis can be aggravated and the incidence of acute renal failure can be increased [25]. At present, diabetic ketoacidosis and acute renal failure are mainly treated by fluid replacement, low-dose insulin, and hemodialysis [26]. However, due to the unstable hemodynamic status of patients with diabetic ketoacidosis and acute renal failure, combined with the effects of metabolic acidosis and electrolyte imbalance, conventional symptomatic treatment and traditional intermittent dialysis treatment cannot achieve satisfactory results [27,28].
Hemodialysis is an effective method for the treatment of uremia [5]. Dialysis is based on the use of a dialyzer composed of myriad hollow fibers through which blood circulates outside the body, so that the blood and a similar concentration of dialysate are adsorbed and dispersed. Under the action of ultrafiltration and convection, the material exchange occurs through one hollow fiber, and the metabolic waste in the body is removed to correct and maintain balanced levels of water, electrolyte, and acid-base [4,29]. Hemodialysis is the cornerstone therapy for patients with end-stage renal disease (ESRD). However, highly protein bound or large molecular weight uremic toxins (such as phenolic and indolic compounds and homocysteine) associated with adverse outcomes (such as cardiovascular disease of patients with ESRD) are difficult to remove through hemodialysis; these toxins can be effectively eliminated by hemoperfusion [30]. At the same time, the excess water in the body is removed, and the purified blood is returned to the body. However, the biofilm holes of the hemodialysis dialyzer are limited, and although they have a good scavenging effect on small molecular metabolic waste, and removal of inflammatory substances and medium-size and macromolecular substances is difficult [31]. The use of hemodialysis alone can prolong survival, but there are many complications, such as infection, anemia, and secondary hyperparathyroidism [6].
This study also has certain limitations. First, the sample size was small; second, the study was retrospective and relied on the accuracy of medical records; and third, the study was performed at a single center. We will expand the sample size and conduct multi-center research in the future.
Conclusions
This retrospective real-world study from the experience at a single center showed that in comparison with hemoperfusion alone, hemodialysis+hemoperfusion significantly reduced pruritus and anemia, improved renal function, and was associated with significantly fewer adverse events in patients with diabetic ketoacidosis and acute renal failure.
References
1. Abdullah HMA, Elnair R, Khan UI, Rapid onset type-1 diabetes and diabetic ketoacidosis secondary to nivolumab immunotherapy: A review of existing literature: BMJ Case Rep, 2019; 12(8); e229568
2. Timilsina S, Timilsina S, Mandal A, Triad of diabetic ketoacidosis, hypertriglyceridemia, and acute pancreatitis. Severity of acute pancreatitis may correlate with the level of hypertriglyceridemia: Cureus, 2019; 11; e4930
3. McLachlan G, Keith C, Frauman A, Diabetic ketoacidosis with sodium-glucose cotransporter type 2 inhibitors: A case series: Med J Aust, 2019; 211; 237-237.e1
4. Huang M, Lv A, Wang J, Exercise training and outcomes in hemodialysis patients: Systematic review and meta-analysis: Am J Nephrol, 2019; 50; 240-54
5. Wilund KR, Viana JL, Perez LM, A critical review of exercise training in hemodialysis patients: Personalized activity prescriptions are needed: Exerc Sport Sci Rev, 2020; 48(1); 28-39
6. Marini ACB, Pimentel GD, Is body weight or muscle strength correlated with the Malnutrition Inflammation Score (MIS)? A cross-sectional study in hemodialysis patients: Clin Nutr ESPEN, 2019; 33; 276-78
7. Zhang L, Long J, Jiang W, Trends in chronic kidney disease in China: N Engl J Med, 2016; 375; 905-6
8. Chen J, Zeng H, Ouyang X, The incidence, risk factors, and long-term outcomes of acute kidney injury in hospitalized diabetic ketoacidosis patients: BMC Nephrol, 2020; 21; 48
9. Coca SG, Yusuf B, Shlipak MG, Long-term risk of mortality and other adverse outcomes after acute kidney injury: A systematic review and meta-analysis: Am J Kidney Dis, 2009; 53; 961-73
10. Bellomo R, Ronco C, Kellum JA, Acute renal failure- definition, outcome measures, animal models, fluid therapy and information technology needs: The second international consensus conference of the Acute Dialysis Quality Initiative (ADQI) group: Crit Care, 2004; 8; 204-12
11. Mujtaba MA, Al Hillan A, Shenouda D, Incidental finding of gastric schwannoma in a renal failure patient – managed by a minimally invasive procedure: Report of a rare case: Am J Case Rep, 2019; 20; 1241-44
12. Chen W, Wang ZK, Ren YQ, Silencing of keratin 1 inactivates the Notch signaling pathway to inhibit renal interstitial fibrosis and glomerular sclerosis in uremia: J Cell Physiol, 2020; 235; 1674-88
13. Church JT, Alghanem F, Deatrick KB: ASAIO J, 2017; 63; 766-73
14. Kallel S, Triki Z, Abdenadher M, Acute renal failure after cardiac surgery. Evaluation of the RIFLE criteria: Nephrol Ther, 2013; 9; 108-14
15. Kitabchi AE, Umpierrez GE, Miles JM, Fisher JN, Hyperglycemic crises in adult patients with diabetes: Diabetes Care, 2009; 32; 1335-43
16. Garrett CJ, Choudhary P, Amiel SA, Recurrent diabetic ketoacidosis and a brief history of brittle diabetes research: Contemporary and past evidence in diabetic ketoacidosis research including mortality, mental health and prevention: Diabet Med, 2019; 36; 1329-35
17. Lee K, Park IB, Yu SH, Characterization of variable presentations of diabetic ketoacidosis based on blood ketone levels and major society diagnostic criteria: A new view point on the assessment of diabetic ketoacidosis: Diabetes Metab Syndr Obes, 2019; 12; 1161-71
18. Luo SS, Yu CP, Hsieh YW, Effects of antibiotics on the pharmacokinetics of indoxyl sulfate, a nephro-cardiovascular toxin: Xenobiotica, 2020; 50(5); 588-92
19. Li M, Yan J, Zhang H, Analysis of outcome and factors correlated with maintenance peritoneal dialysis: J Int Med Res, 2019; 47; 4683-90
20. Chen J, Qin X, Li Y, Comparison of three nutritional screening tools for predicting mortality in maintenance hemodialysis patients: Nutrition, 2019; 67–68; 110532
21. Reardon MJ, Dialysis dependent renal failure and the treatment of aortic stenosis: Cardiovasc Revasc Med, 2019; 20; 831
22. Mussa FF, Horton JD, Moridzadeh R, Acute aortic dissection and intramural hematoma: A systematic review: JAMA, 2016; 316; 754-63
23. Dhatariya KK, Vellanki P, Treatment of diabetic ketoacidosis (DKA)/hyperglycemic hyperosmolar state (HHS):Novel advances in the management of hyperglycemic crises (UK versus USA): Curr Diab Rep, 2017; 17(5); 33
24. Fazeli Farsani S, Brodovicz K, Soleymanlou N, Incidence and prevalence of diabetic ketoacidosis (DKA) among adults with type 1 diabetes mellitus (T1D):A systematic literature review: BMJ Open, 2017; 7; e016587
25. Seddik AA, Bashier A, Alhadari AK, Challenges in management of diabetic ketoacidosis in hemodialysis patients, case presentation and review of literature: Diabetes Metab Syndr, 2019; 13; 2481-87
26. Ahuja W, Kumar N, Kumar S, Rizwan A, precipitating risk factors, clinical presentation, and outcome of diabetic ketoacidosis in patients with type 1 diabetes: Cureus, 2019; 11; e4789
27. Alsamman MA, Alsamman S, Moustafa A, Critical care utilization in patients with diabetic ketoacidosis, stroke, and gastrointestinal bleed: Two hospitals experience: Cureus, 2019; 11; e4698
28. Bharill SA, Hunter JD, Walsh ET, Pediatric stroke as the presenting symptom of new-onset type 1 diabetes mellitus without DKA: Case report and literature review: J Pediatr Endocrinol Metab, 2019; 32; 1035-37
29. Wang F, Wang Y, Tian Y, pattern recognition and prognostic analysis of longitudinal blood pressure records in hemodialysis treatment based on a convolutional neural network: J Biomed Inform, 2019; 98; 103271
30. Lu W, Jiang GRHD/HP versus HD trial Group: BMJ Open, 2018; 8; e022169
31. Marini ACB, Motobu RD, Freitas ATV, Total protein or leucine intakes are not associated with handgrip strength in hemodialysis patients: A pilot study: Clin Nutr ESPEN, 2019; 33; 290-93
In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952